Chapter 7
Complications: Avoidance and Management
Aim
The aim of this chapter is to describe the management of sedation-related problems and complications.
Outcome
After reading this chapter you should be able to recognise and manage common complications associated with the administration of conscious sedation in general dental practice and other primary care settings.
Introduction
Serious complications associated with carefully administered conscious sedation are rare. Minor problems are more common. Fortunately, most minor problems are easily managed by a well-prepared dental team. Careful case selection, based on a detailed medical, dental and social history, will often allow the dental team to anticipate potential difficulties and take appropriate action. Prevention is always preferable to treatment.
Although complications may arise from the use of any sedation technique, it is a widely held misconception that intravenous sedation offers the greatest potential for difficulties. This chapter will consider only those complications which may arise from intravenous sedation using midazolam and inhalational sedation using nitrous oxide and oxygen. The reader is referred to the descriptions of alternative drugs in Chapter 6 for brief comments on the possible difficulties associated with these techniques.
Complications of Sedation and their Management
Respiratory depression
The most serious potential complication associated with intravenous sedation using midazolam is respiratory depression. The mechanisms for this are described in detail in Chapter 2. Put simply, the patient “forgets to breathe” and the normal physiological corrective mechanisms fail to respond.
It is important to understand that all patients who receive intravenous midazolam experience some reduction in both the rate and the depth of breathing. This is sometimes apparent clinically (chest movement is visibly reduced) but not always. The effect is usually most pronounced during the first 10 minutes or so of sedation. It is sometimes seen much later, particularly when there is a lull in clinical activity. The difficulty in recognising mild or even moderate respiratory depression underlines the necessity for continuous pulse oximetry in addition to careful clinical monitoring.
Management of midazolam-induced respiratory depression involves the following steps:
-
Ask the patient to take several deep breaths.
In the majority of cases, this will resolve the problem; BUT if this fails:
-
Open the airway (head tilt/chin lift or jaw thrust) and perform intermittent positive pressure ventilation using a ventilating bag, preferably with an oxygen supply attached (Fig 7-1).
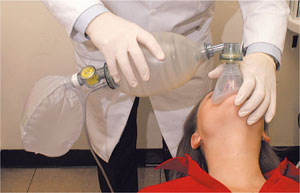
Fig 7-1 Intermittent positive pressure ventilation.
IF this fails:
-
Administer flumazenil (500 micrograms by slow intravenous injection). Continue to ventilate and encourage breathing.
Note that it is VERY rarely necessary to do anything more than encourage breathing.
Airway obstruction
Obstruction of the airway may occur during any form of sedation. Patients who have received intravenous drugs are probably less likely to notice and to complain of breathing problems. Excessive downward pressure without adequate support of the mandible during the extraction of molar teeth is a common cause, the management of which is obvious. Accumulation of water and dental debris in the oropharynx can also be a problem. This is easily managed by the use of properly positioned high-volume suction. Carrying out restorative procedures under rubber dam is a most effective way of minimising this difficulty. In the event of respiratory problems, the rubber dam must be removed immediately.
Hypotension
All intravenous sedation drugs tend to cause a decrease in the systemic arterial blood pressure. This is partly due to reduced sympathetic activity and direct depression of the brain’s cardiac control centres. Unlike respiratory depression, the fall in blood pressure is usually self-limiting and, as such, requires no active treatment. A patient with a naturally low arterial blood pressure should be moved slowly from the supine position to the sitting position to reduce the possibility of postural hypotension. A patient with a very low resting blood pressure may benefit from intermittent blood pressure monitoring.
Problems with Venepuncture
Intravenous cannulation is easily learned but, like many clinical skills, proficiency takes time and minor problems are commonplace, particularly during the early days. The similarity with learning to administer an effective inferior dental block is perhaps helpful – initial anxiety associated with a high failure rate is soon followed by an improved rate of success and confidence. With more experience, this matures into a more realistic approach which enables the confident management of occasio/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


