Chapter 6
Clinical Techniques
Aim
This chapter describes the techniques commonly used to sedate patients for treatment in primary care settings.
Outcome
After reading this chapter you should have an understanding of the clinical procedures used during conscious sedation in primary care settings.
Introduction
Inhalation sedation using nitrous oxide and oxygen and intravenous midazolam are by far the most commonly used and useful techniques. Since some appropriately trained and experienced practitioners may use other drugs and routes of administration for selected dental patients, an outline of some alternative techniques is also provided.
There are advantages of having a variety of techniques at one’s disposal.
-
It allows optimal management of each patient, taking into account medical, psychological and social status. Examples might include a recent history of myocardial infarction, potential interactions with antidepressant medication or domestic or business responsibilities.
-
Consideration of the type of dentistry and the length of the intended procedure.
-
A combination of techniques may sometimes be appropriate – for example, in a needle-phobic patient for whom nitrous oxide sedation is used to facilitate cannulation for intravenous sedation.
Presedation Preparation
Meticulous preparation will increase the likelihood of success. It is particularly important that the patient is fully prepared for both the sedation and the planned dental procedure. Anxiety is likely to increase if an anxious patient has to wait whilst missing items are found or faulty equipment replaced. All necessary equipment and drugs must be prepared and checked in advance. When the patient enters the surgery, the dental team must be able to concentrate fully on putting the patient at ease. After the induction of adequate sedation, the dentist must be ready to proceed with treatment without delay. A checklist (Fig 6-1) is a useful aid for training members of the dental team.
Fig 6-1 Presedation checklist.
Conscious Sedation Techniques
In regular use in primary dental care in the UK
Inhalation sedation (nitrous oxide and oxygen) – Relative analgesia
Intravenous midazolamAdvanced techniques which may only be used by appropriately trained and experienced practitioners
Intravenous propofol (by infusion)
Intravenous midazolam plus an opioid
Oral or intranasal benzodiazepines
The practice environment is also important in putting patients at ease. A quiet, calm environment with minimum interruption provides the best setting for conscious sedation. It is important to avoid having alarming or explicit cardiopulmonary resuscitation posters in full view of anxious patients. This also includes graphic illustrations of florid dental disease or procedures which may increase the level of anxiety in dental phobics. Threatening equipment should also be kept out of site or covered.
Before starting any clinical procedure, it is essential to check the patient’s name, medical history and bloodpressure. Written consent should have been obtained in advance of the treatment appointment for both the procedure and the sedation. It is also necessary to confirm that the patient has a responsible adult escort who is able and willing to look after the patient for the rest of the day. A patient who does not have a suitable escort should not be sedated. Be wary of patients who say they will “phone a friend” or have arranged a taxi to travel home and then have a neighbour keep an eye on them. These arrangements are never satisfactory, may place the patient at risk and leave the dentist open to criticism if anything goes wrong. If there is any doubt about the quality of aftercare, conscious sedation should NOT be used. A final check should be made to ensure that the appropriate preoperative instructions have been followed and that the patient has been to the lavatory.
Inhalational Sedation with Nitrous Oxide and Oxygen
Nitrous oxide has excellent anxiolytic, sedative and analgesic properties with little or no depression of myocardial function or ventilation. Induction and recovery are rapid. As described in Chapter 3, nitrous oxide has a wide margin of safety.
The response to nitrous oxide sedation varies considerably and unpredictably between patients. One person may be adequately sedated with 20% nitrous oxide, others may require in excess of 50%. A titration technique is therefore employed to avoid the risk of under- or oversedation.
Modern inhalational sedation machines are similar to traditional Boyle’s anaesthetic machines, but modified so as to make them safe for use by a sedationist (see Chapter 5). The inhalational sedation machine must be carefully checked before use. The safety features and ease of operation of purpose-designed inhalation sedation machines make them ideal for a clinician acting as both operator and sedationist (Fig 6-2). Demand-flow devices and equipment designed for general anaesthesia are not suitable for the administration of inhalation sedation by an operator-sedationist. The advantages of inhalational sedation include:
-
no needles
-
level of sedation easily altered
-
minimal impairment of reflexes
-
rapid induction and recovery
-
some analgesia
-
suitable for patients of all ages.
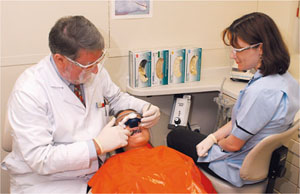
Fig 6-2 Operator-sedationist working with Relative Analgesia.
The disadvantages are:
-
sedation depends on good psychological support
-
postoperative amnesia is variable
-
nitrous oxide pollution.
Contraindications of inhalational sedation are:
-
nasal obstruction, e.g. cold, polyps, deviated septum
-
cyanosis at rest
-
poor cooperation
-
first trimester (12 weeks) of pregnancy
-
fear of masks.
Administration of nitrous oxide
After checking that the Relative Analgesia machine is working and that extra gas cylinders are available (or that piped gases are flowing), the patient is laid supine in the chair and the procedure explained. The machine is then adjusted to administer 100% oxygen at a flow rate of 6 litres/min and the correct size nasal mask selected. Patients often prefer to place the mask over their own nose rather than have someone else do it (Fig 6-3). It is important to maintain a steady flow of conversation and encouragement during the induction of sedation. The oxygen flow rate (minute volume) may be checked by observing the movement of the reservoir bag. If there is under-or overinflation of the bag, the gas flow must be increased or decreased respectively (Figs 6-4 and 6-5).
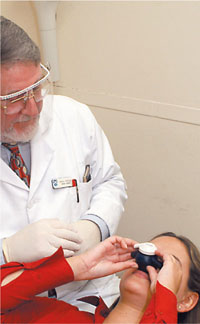
Fig 6-3 Patient trying mask.

Fig 6-4 Overinflated reservoir bag.

Fig 6-5 Underinflated reservoir bag.
Regular observation of the reservoir bag combined with clinical vital signs provides all the necessary monitoring for fit patients. Pulse oximetry is NOT indicated for ASA I and II patients (see Chapter 4) undergoing inhalation sedation. Patients are receiving a high inspired oxygen concentration continuously and, therefore, arterial oxygen estimations are artificially high. Some practitioners, however, find the continuous heart rate monitoring provided by a pulse oximeter a useful indicator of anxiety.
Ten per cent nitrous oxide is then added (90% oxygen) and the patient informed that he/she may feel:
-
lightheaded
-
changes in visual/auditory sensation
-
tingling of hands and feet
-
suffusing warmth
-
remote from the immediate environment.
This concentration is maintained for one minute during which verbal encouragement and reassurance are given continuously. The concentration of nitrous oxide is then increased by 10% for a further minute to a total of 20% nitrous oxide. After this, if more sedation is required, increments of 5% nitrous oxide are added per minute until the patient appears and feels sufficiently relaxed.
Nitrous oxide concentrations of between 20% and 50% normally produce a state of detached sedation and analgesia without any loss of consciousness or potential impairment of laryngeal reflexes. At these levels patients are aware of operative procedures and cooperate without being fearful. If, after a period of effective sedation, the patient becomes restless or apprehensive, it is usually the result of disinhibition due to the concentration of nitrous oxide being too high.
Local anaesthesia (LA) should be administered once the patient is sedated. Topical local anaesthesia preparations can be placed during the induction period. The most common cause of apparent failure of nitrous oxide sedation is the assumption that the analgesic properties of nitrous oxide render the use of local anaesthesia unnecessary. This is not the case – nitrous oxide does not provide sufficient analgesia for the majority of dental procedures in either adults or children.
Nitrous oxide has limited solubility in blood and body tissues (see Chapter 3). When the incoming flow of nitrous oxide is stopped there is a rapid outflow of the gas across the alveolar membrane. This may dilute the percentage of alveolar oxygen available for uptake by up to 50%. This phenomenon is called diffusion hypoxia and is prevented by giving 100% oxygen for at least two minutes at the end of the procedure. The patient may then be brought slowly up to the sitting position. Recovery is variable but most patients should be able to walk (with supervision) to a recovery area within five minutes.
All patients, when sufficiently recovered, should be discharged into the care of an escort who must be given written and verbal post-sedation instructions (see Chapter 4). Patients should not be discharged until sufficiently recovered so as to be able to stand and walk without assistance. Recovery is variable and each patient should be individually assessed on every occasion for fitness for discharge. The discharge of patients who have been sedated is the responsibility of the operating dentist.
Nitrous oxide pollution and scavenging
Long-term exposure to nitrous oxide may result in an increased incidence of liver, renal and neurological disease. There is also some evidence of bone marrow toxicity and interference with Vitamin B12 synthesis which may lead to signs and symptoms similar to those of pernicious anaemia. In the UK, the Health and Safety Executive specifies a maximum level of 100 ppm of nitrous oxide, time-weighted over eight hours. Scavenging must be employed to safeguard both patients and staff.
Other inhalation sedation methods
In recent years various combinations of isoflurane, desflurane, sevoflurane and oxygen have been investigated. The lack of a suitable delivery system for use by a dental operator-sedationist has slowed development in this area. Sevoflurane shows most promise.
Intravenous Sedation with Midazolam
Midazolam is well suited to conscious sedation for dentistry (Figs 6-6 and 6-7). It is presented in a 5 ml ampoule in a concentration of 2 mg/ml and in a 2 ml ampoule in a concentration of 5 mg/ml. The more dilute presentation (2 mg/ml) is preferred as it is easier to titrate – that is, administer in small increments, whilst obse/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


