Chapter 7 The Head by Regions
The Head by Regions
1 The Face and Scalp
REGIONS OF THE FACE
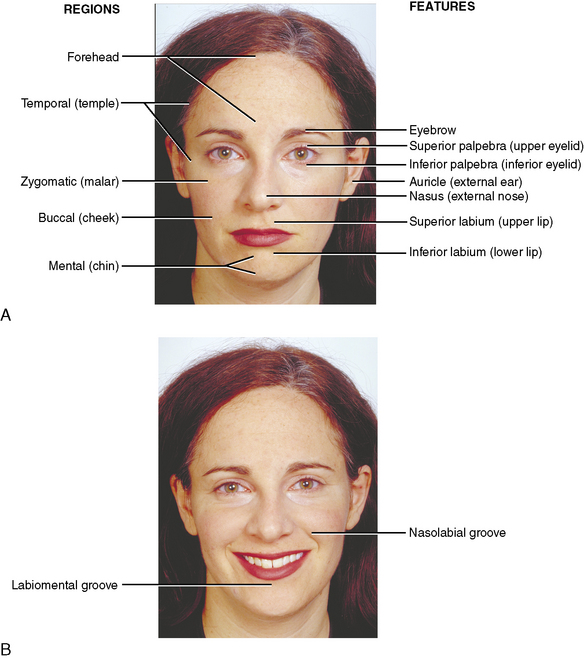
The facial region may be subdivided into a number of areas (Figure 7-1): (1) the forehead, extending from the eyebrows to the hairline; (2) the temples or temporal area anterior to the ears; (3) the orbital area containing the eye and covered by the eyelids; (4) the external nose; (5) the zygomatic (malar) area (prominence of the cheek); (6) the mouth and lips; (7) the cheeks; (8) the chin; and (9) the external ear.
SKELETON
The anterior, superior, lateral, and posterior aspects of the skull are discussed in Chapter 6.
SENSORY (CUTANEOUS) NERVES OF THE FACE
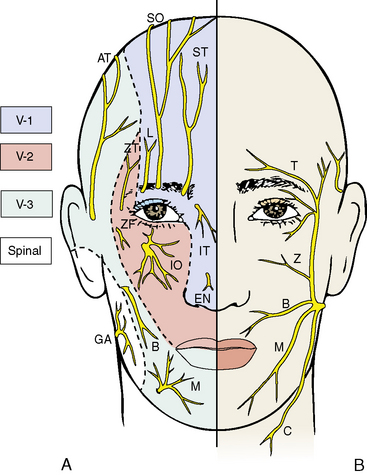
The facial cutaneous nerve supply is principally derived from the trigeminal nerve (cranial nerve V) (Figure 7-2). Within the skull, the trigeminal nerve divides into three parts: (1) the ophthalmic nerve (cranial nerve V-1), a sensory nerve associated mainly with the orbit and its contents; (2) the maxillary nerve (cranial nerve V-2), a sensory nerve associated with the nasomaxillary complex; and (3) the mandibular nerve (cranial nerve V-3), a sensory and motor nerve associated with the lower jaw and the muscles of mastication. Only the mandibular nerve contains motor as well as sensory fibers. Each division of the trigeminal nerve contributes sensory cutaneous branches to the face.
Facial Branches of the Ophthalmic Nerve
Facial Branches of the Maxillary Nerve
Infraorbital Nerve
ARTERIES OF THE FACE
The face is richly supplied with blood from various arteries, and the terminal branches of these various arteries anastomose freely (Figure 7-3). The entire blood supply is derived from either the internal or the external carotid arteries. Their facial branches travel as companion arteries to the sensory facial nerves described previously and, in general, carry the same names as the facial sensory nerves.
Facial Branches of the Ophthalmic Artery
VEINS OF THE FACE
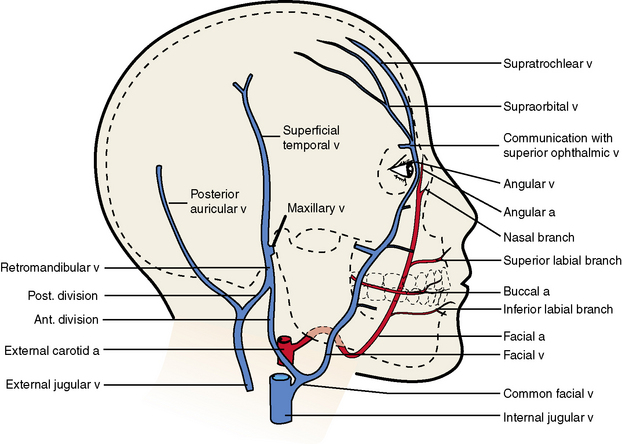
The veins of the face follow somewhat the same pattern of distribution as the arterial supply, except for a few small but important differences (see Figures 7-3 and 7-4). Veins generally show more variability in their distribution than do arteries.
Veins that Accompany Cutaneous Nerves and Arteries
The Facial Vein
Venous Communications
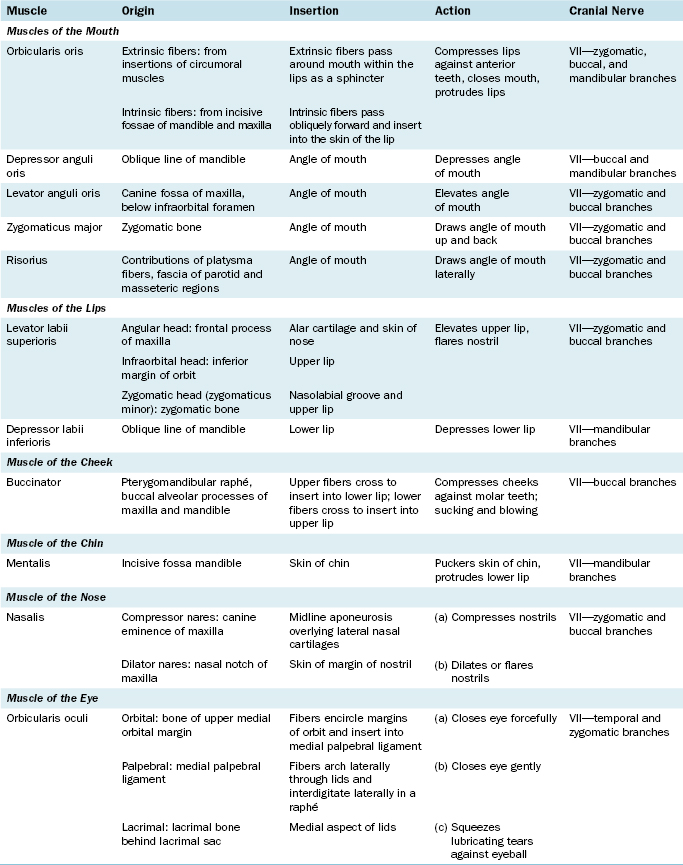
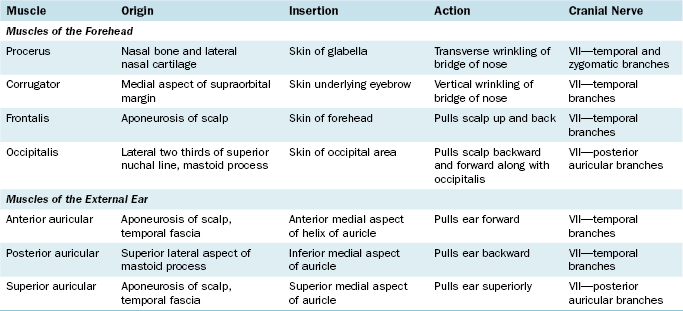
MUSCLES OF THE FACE
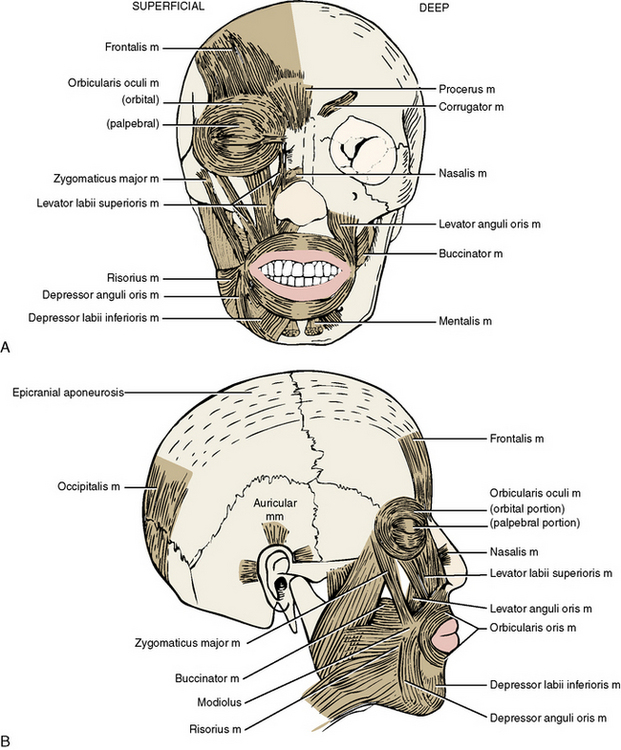
The muscles of the face, or muscles of facial expression, are derived from the second branchial arch and are supplied by the cranial nerve of the second arch, the facial nerve (cranial nerve VII) (Figure 7-5 and Table 7-1). The muscles of the scalp and the platysma muscle of the neck belong to the same muscle group.
Lips
Cheek
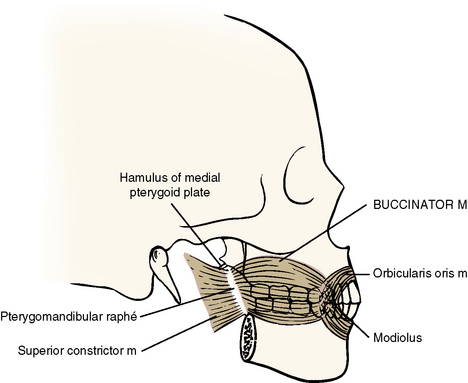
Buccinator
Origin
The buccinator muscle arises from three areas (Figure 7-6).
Nose: Nasalis
The nasalis muscle is the main muscle of the nose, and it arises as two parts.
MOTOR NERVES OF THE FACE: THE FACIAL NERVE
The facial nerve exits from the skull through the stylomastoid foramen at the base of the skull (see Figure 7-2). It passes inferiorly and anteriorly for several millimeters, enters the substance of the parotid gland, and here breaks up into five main groups of branches that radiate from the anterior margin of the gland and travel to various areas of the face.
Superficial Branches
Many facial muscles are supplied by more than one of the five branches of the facial nerve.
Sensory Nerve Communications
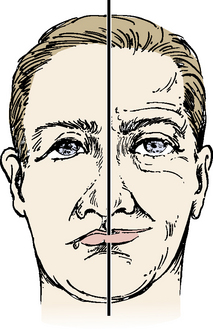
Facial Paralysis
Damage to the facial nerve results in some form of facial paralysis (Figure 7-7). The type of paralysis is dependent upon where the lesion (damage) occurs.
Lesions of the lower motor neuron
A local anesthetic mistakenly injected into the parotid gland anesthetizes the facial nerve within the gland and results in a temporary facial paralysis. (See page 269.)
FEATURES OF THE FACE
Lips (Labia)
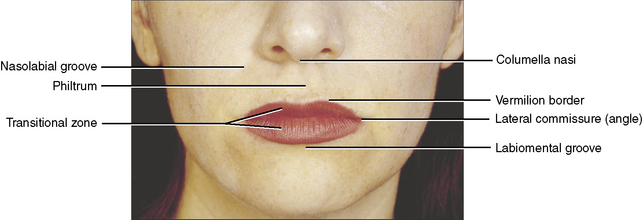
The upper and lower lips surround the mouth, or entrance to the oral cavity (Figure 7-8). The upper lip lies between the nose above and the opening of the mouth below. Laterally, the lips are separated from the cheeks by the nasolabial groove, a furrow extending from the ala of the nose to approximately 1 cm lateral to the angle of the mouth. The philtrum is a wide (6 to 7 mm), shallow trough extending from the nose to the red (vermilion) border of the upper lip. Superiorly, the philtrum ends at the columella, the fleshy external partition between the nostrils.
Layers
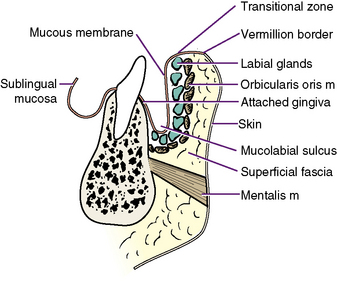
The lip consists of several layers sandwiched between the skin externally and oral mucous membrane internally (Figure 7-9).
Mucous Membrane
The transitional zone sweeps into the mouth and is transformed into true, moist, nonkeratinizing mucous membrane. The mucous membrane coats the intraoral vestibular portion of the lip and then reflects down from the upper lip or up from the lower lip onto the alveolar process. The fold is the vestibular, or mucolabial, fold. The mucous membrane ascends on the alveolar process and turns abruptly to gingiva (gums). The demarcation is abrupt, with the gingiva assuming a lighter color and a stippled surface. The gingiva is firmly attached to the underlying alveolar bone. The gingiva is described in greater detail in section 8 of this chapter.
Cheeks (Buccae)
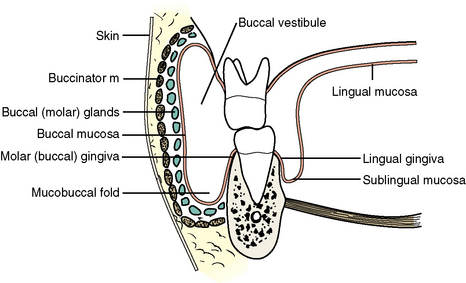
The cheeks form the lateral movable walls of the oral cavity (Figure 7-10). Externally, the cheek includes not only the movable portion but also the prominence of the cheek over the zygomatic arch. This terminology, however, is from common usage, and our definition of cheek is confined to the movable portion.
External Nose
Framework
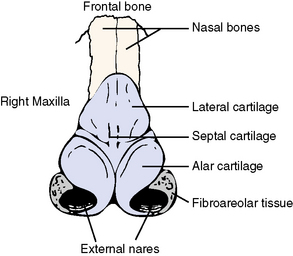
The framework of the external nose consists of the paired nasal bones superiorly and a movable hyaline cartilage and fibroareolar portion below (Figure 7-11).
Muscles
The muscle of the nose is the nasalis muscle, consisting of two sets of fibers: (1) the dilator nares, which flare the nostrils, and (2) the compressor nares, which flatten the nostrils (see Figure 7-5).
External Ear (Auricle)
Cartilage
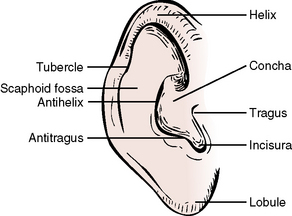
A single elastic cartilage provides support for the external ear (Figure 7-12). The pendulous lower portion, or earlobe, contains no cartilage but does contain fibroareolar tissue. The cartilage of the ear is continuous with the cartilage of the external auditory meatus (canal), leading within the petrous temporal bone to the middle ear.
Muscles
The muscles of the ear are the superior, anterior, and posterior auricular muscles, which wiggle the ear (see Figure 7-5).
Features
The cartilage and skin of the ear are thrown into several folds. The names of these resulting ridges and depressions are found in Figure 7-12.
Eyelids (Palpebrae)
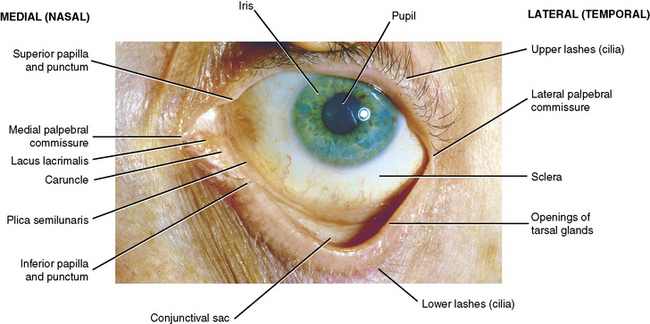
External Features (Figure 7-13)
Layers
Skin
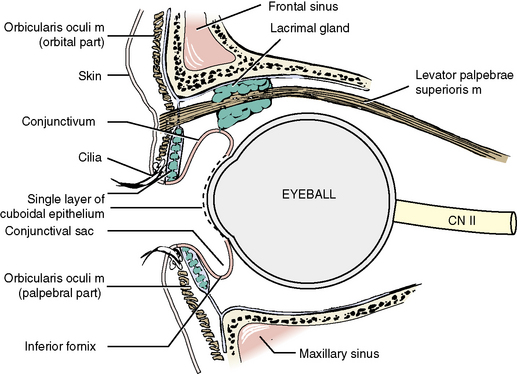
Extremely thin skin covers the lids of the eye (Figure 7-14). At the margins of the eye, prominent hairs, or cilia, form two or three irregular rows along the lateral five sixths of the margin. Associated with the cilia are large sebaceous glands, or ciliary glands (glands of Zeis). Infected ciliary glands result in the common stye.
Orbital Septum and Tarsi
The orbital septum and tarsi form the “skeleton” of the eyelid (see Figure 7-14 and also Figure 7-34 later in this chapter). The orbital septum is a membranous connective tissue sheet that attaches to the periphery of the orbital margin. Medially, it attaches to the posterior lacrimal crest. The septum forms a curtain with an elliptical transverse opening, the palpebral fissure.
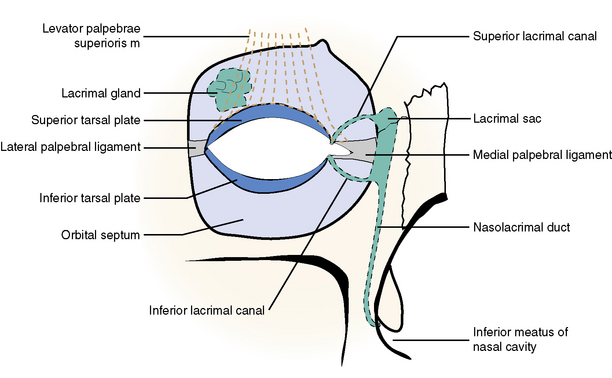
Lacrimal Apparatus
The lacrimal gland, which produces tears, and the duct system, which conveys excess tears away from the conjunctival sac, are discussed with the orbit and its contents in section 3 of this chapter.
The Scalp
Layers
Blood and Nerve Supply
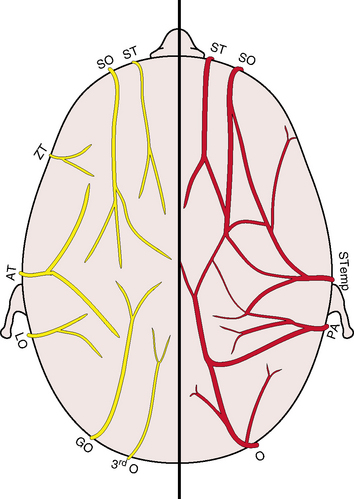
The blood supply to the scalp arises from various sources but basically arises from branches of the ophthalmic and external carotid arteries (Figure 7-15). The arteries ascend to the scalp from the face below in a semicircle.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses