7
Retainers
Retention is the period following active treatment when teeth need to be maintained in their new positions. In most cases, if this phase of treatment does not occur, then there is a very strong chance of relapse. This is because both bone and soft tissues take time to adapt and re-establish their pre-treatment strength.
- Explain what relapse is
- Explain the difference between relapse and maturational (or age) changes
- Understand which types of tooth movement/situations are prone to relapse
- Explain what the purpose of retention and retainers is
- Explain what retention regimes are
- Explain the need for retention with regard to interceptive treatment
- Explain some advantages and disadvantages of different types of retainer
- Describe the role of the general dental practitioner in monitoring retainers
- Describe some problems that may occur with retainers
- Understand the need to liaise with the specialist
What Is Relapse?
Consider the bone remodelling cycle: the whole cycle takes about 6 months to complete and, since when teeth are moved, bone has to be resorbed (ahead of the root) and deposited (behind the root), the whole bone remodelling cycle applies. Therefore, in order for there to be any prospect of avoiding relapse, retention needs to be for a period of at least 6 months. However, soft tissues obviously also have a role to play, and their adaptability and turnover also influence the likelihood of stability (or the lack of it).
Depending on the location, some or all of the following soft tissues may have a role to play with regard to relapse and stability: the gingivae; periodontal ligament; lips, cheeks and tongue. For all situations however, the gingivae and periodontal ligament will always have a role to play, and adaptation, particularly in the supracrestal gingival (elastic) fibres, will actually take longer than for bone. Indeed, whilst it is thought that these fibres take at least 9 months to re-adapt, it is not certain that these fibres will ever adapt fully to the new tooth positions. This means that there are a number of situations where stability will never really be possible and relapse is a strong possibility.
Many people – dentists included – will tend to term any post-active-treatment tooth movement as ‘relapse’, but this is not strictly true. Furthermore, it is important to be clear about what we actually mean by relapse, as it influences what both operators and patients can expect from treatment. Relapse should be distinguished from maturational or age changes with which it is frequently confused.
Technically and practically, relapse actually means that teeth return either to their pre-treatment position or toward this position.
Features of Relapse
- Usually occurs rapidly – within a few weeks or months.
- Often due to operator factors such as incorrect treatment mechanics, e.g. reducing an overjet by proclination of the lower incisors; correcting an incisor crossbite without ensuring there is sufficient overbite to keep the incisor corrected. Such problems may themselves be due to incorrect diagnosis in the first place.
- Occasionally patient factors may be the underlying problem, e.g. the patient fails to wear the retainer either at all or as requested.
- There are situations (noted below) that are prone to relapse unless they are ‘permanently’ retained.
What Are Maturational Changes? How Do They Differ from Relapse?
Several long-term studies have followed up untreated individuals for many years. These studies have demonstrated that teeth tend to move throughout life.
Features of Maturational Change
Common findings are:
- Inter-canine width reduces with age (more in females than males).
- Crowding tends to increase with age – this is particularly common in the lower incisor region, but other teeth, including the upper incisors, can also be affected.
- Inter-molar width however shows little change.
- Usually occurs slowly – over months or years.
- Occurs in young adults as well as older individuals.
- Can occur even in individuals who have had ‘straight teeth’ for years.
- Wisdom teeth have frequently been blamed for late lower incisor crowding, but we now know that this occurs regardless of the presence or absence of third molars.
Although other changes may also occur, such as changes in overjet or overbite, the biggest problem is that we cannot yet predict which patients will be most likely to experience such changes.
What Is the Importance of Distinguishing Relapse from Maturational Change?
The crucial point is that orthodontic treatment does not stop teeth moving throughout life; whether treatment involves extractions or not makes no difference. Teeth are not fixed in stone throughout life just because of orthodontic treatment. Therefore, this needs to be explained to all patients about to embark on treatment. Whilst retainers can help reduce the amount of relapse as the bone and soft tissues re-adapt, it is, practically-speaking, impossible to guarantee to any patient that their teeth will never move from the post-treatment position – even if they continue to wear retainers. There are several reasons for this:
- Retainers (whether removable or fixed) may break and, as a consequence, the position of the teeth will not be adequately controlled until the retainer can be repaired or a replacement can be fitted. The literature shows that fixed retainers, in particular, have high failure rates.
- Removable retainers may not always be worn as instructed and/or they may be lost.
- Clinicians may not instruct patients adequately.
- With time and use, wires tend to stretch or suffer a reduction in stiffness. Therefore, even when bonded retainers remain attached to the teeth and there is no obvious failure of any of the components, subtle changes may occur, including small spaces opening between teeth and changes in inclination of individual teeth. These have been infrequently documented in the literature to date, but this itself is probably due to the lack of long-term follow-up of patients. Furthermore, it is only comparatively recently that increasing numbers of patients are wearing retainers.
It is often assumed that bonded retainers are more effective than removable retainers. However, as noted above, this is not borne out by studies undertaken so far.
Cases That Are Particularly Prone to Relapse and Why
There are several situations that are known to be especially prone to relapse:
- Rotations
- Spacing due to small and/or developmentally absent teeth; midline diastemas
- Movements involving significant expansion
- Periodontally involved teeth.
Rotations
In the case of rotations, the issue of relapse relates directly to the soft-tissue factors noted previously. When a tooth is de-rotated, i.e. ‘untwisted’, the supracrestal gingival (elastic) fibres seem very slow to re-adapt to the new position and indeed may never adapt fully to the new tooth positions. Any residual tension in the gingival fibres is more likely to lead to some degree of relapse, even following many months of retention.
In order to reduce this tendency, a minor surgical procedure known as ‘pericision’ or ‘supracrestal fiberotomy’ has been devised. This procedure can be undertaken under local anaesthesia and involves the insertion of a thin scalpel blade down the gingival crevice (until it contacts the alveolus) and circling the blade around the neck of the tooth. The aim is to cut the gingival fibres that insert into the neck of the tooth above the alveolar bone crest, to encourage them to re-adapt to the new tooth position. However, even though this is a simple procedure to undertake, it needs to be done carefully in order to avoid causing any periodontal problems such as recession. Pericision is not really suitable for use in the lower labial segment (LLS) as the teeth are much narrower than in the upper labial segment (ULS), and so too is the gingival cuff. There is therefore a greater risk of iatrogenic periodontal damage.
Nevertheless, even if a patient agrees to pericision being performed, studies suggest that rotational relapse will still not be eliminated and relapse in the region of 20% can be expected. Also, some patients may find the idea of a surgical procedure off-putting.
Spacing Due to Small And/or Developmentally Absent Teeth: Diastemas
Here again, lack of soft-tissue adaptation is the problem. Whilst it may be possible and, indeed, quite straightforward (using fixed appliances) to close spaces of 1–2 mm, the far bigger problem is maintaining space closure. The problem seems to be even greater when attempts are made to close larger spaces. Any break in retainer wear can lead to rapid relapse even when fixed, i.e. bonded, retainers are used.
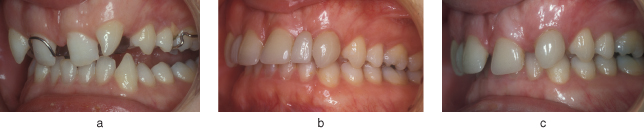
Maintaining spaces that have been increased for the placement of fixed prostheses, where teeth are developmentally missing in hypodontia cases, is an equally difficult problem. Figure 7.1 shows an example of significant relapse following orthodontic treatment for hypodontia.
Figure 7.1 Example of the strong relapse tendency of spacing – in this case associated with hypodontia. This patient underwent 2 years of fixed appliance treatment (plus a biteplane) to reduce the spaces between the centrals and open spaces for the upper laterals (a). Bonded bridges were placed (b), but unfortunately, during an hospital admission, one bridge was knocked out by an anaesthetist and within a few days UL3 had slipped forward again and UR1 and UL1 had moved apart (c). The patient had to undergo re-treatment.
In order to help with midline diastema closure, frenectomy has been suggested and performed. However, whilst this may help in some patients, the difficulty is that there is no reliable means of predicting which diastemas are caused by a ‘fleshy frenum’ and which are not. Alleged signs that a frenectomy may be indicated include: blanching of the incisive papilla when the frenum is stretched by pulling the upper lip forward, or a notch of the alveolus between the upper central incisors visible on an upper anterior occlusal radiograph. Unfortunately, neither of these signs is reliable enough to be clinically valid. Furthermore, it has been found that with time/age, diastemas tend to reduce spontaneously. The same cannot be said of spaces or spacing due to hypondontia; these spaces have no relationship to frenal attachments.
Movements Involving Significant Expansion
Some expansion can be acceptable. However, relapse occurs when teeth are tipped beyond the basal bone because this causes the teeth to flare outward and, as a consequence, there is little or no occlusal inter-digitation. Likewise, relapse is also inevitable when a crossbite of skeletal aetiology is corrected by tooth movement only. The problems of relapse in these situations are due to a combination of bone, soft-tissue and dental factors.
Periodontally Involved Teeth
Patients who experience severe periodontal disease lose bone and soft tissue from around the teeth affected. This means that the soft tissue balance is now altered: the pressures from the tongue and lips/cheeks are now less opposed than previously due to the loss of hard and soft periodontal tissues. Consequently, the teeth tend to drift to a new position of balance. However, due to the increased bone and tissue turnover (as a result of ongoing disease), a balance is not achieved and the teeth can continue to drift. In addition, tissue pressures from the periodontal ligaments are reduced due to the loss of ligament as a result of disease.
If at some stage the periodontal disease is fully controlled and the patient undergoes orthodontic treatment to re-align the teeth, the result will always be highly unstable. This is because the imbalance between hard and soft tissues around the teeth versus those around the rest of the oral cavity will always remain, as bone and soft tissue cannot be replaced. This leads to constant instability without indefinite retention.
Types of Retainers
Currently the choice of retainers divides into removable or fixed retainers. They can be made for either upper or lower arches (or both of course, as is mostly the case) and it is perfectly possible and reasonable that on occasion the two types may be used in the same patient. In contrast to (active) lower removable appliances (LRAs; which generally do not work well in the lower arch), removable retainers generally work perfectly well in the lower arch. This is because these are passive appliances; therefore, there is far less likelihood of the appliance being dislodged since there are no active forces. Active forces often lead to frequent LRA dislodgement due to the much poorer retention being available in the lower arch.
Removable Retainers
Two main types of removable retainer exist: Hawley-type (or variations thereof) (Figure 7.2) and vacuum-formed retainers (VFRs; Figure 7.3).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


