Pain Perception Control
Local Anesthesia
Mechanisms of Action
Pain perception may be altered at the peripheral level by blocking propagation of nerve impulses using local anesthesia. The initial process of pain perception involves production of nerve impulses by a noxious stimulus that activates specialized nerve fibers, termed nociceptors and classified as A-delta and C fibers, that transmit pain information to the CNS. The nerve impulses travel along the nerve fibers via a physiochemical process involving ion transport across the neuronal membrane. The primary effect of local anesthetic agents is to penetrate the nerve cell membrane and block receptor sites that control the influx of sodium ions associated with membrane depolarization.4 Current thinking holds that the sequence of events involved in a local anesthetic block consists of (1) intraneuronal penetration of the local anesthetic and subsequent binding to a receptor site that exists on the inside of the cell membrane, (2) blockade of the sodium channels through which the sodium ions would normally enter during depolarization, (3) decrease in sodium conductance, (4) depression of the rate of electrical depolarization, (5) failure to achieve threshold potential, and (6) lack of development of a propagated action potential and thus blockade of conduction of the nerve impulse.2 In general, small nerve fibers are more susceptible to the onset of action of local anesthetics than large fibers. Accordingly, the sensation of pain is one of the first modalities blocked, followed by cold, warmth, touch, and at times, pressure.
Local Anesthetic Properties
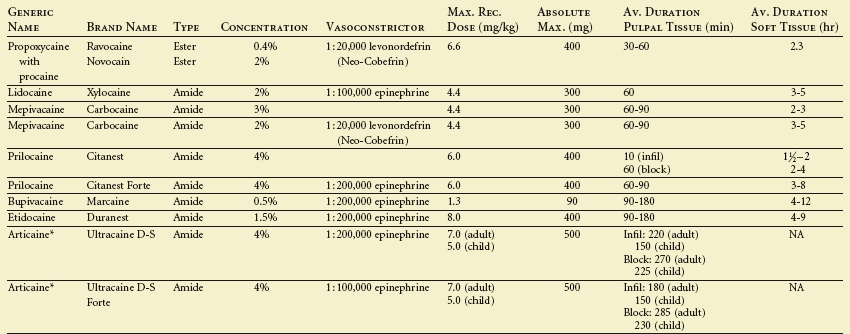
Individual local anesthetic agents differ from each other in their pharmacologic profiles (Table 7-1). They vary in their potency, toxicity, onset time, and duration. All these characteristics may be clinically important, and all vary as a function of the intrinsic properties of the anesthetic agent itself and the regional anesthetic procedure employed. Furthermore, these characteristics may be modified by the addition of vasoconstrictors.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


 Outline
Outline TABLE 7-1
TABLE 7-1