Orthodontic Treatment Planning
From Problem List to Specific Plan
TREATMENT PLANNING CONCEPTS AND GOALS
MAJOR ISSUES IN PLANNING TREATMENT
PLANNING TREATMENT FOR MAXIMAL ESTHETIC IMPROVEMENT
Macro-Esthetic Considerations: Correcting Facial Disproportions
Mini-Esthetic Considerations: Improving the Smile Framework
Micro-Esthetic Considerations: Enhancing the Appearance of the Teeth
Treatment Planning Concepts and Goals
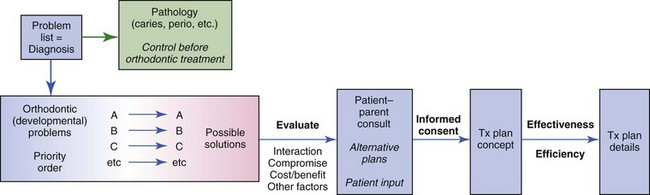
When a group of dentists and dental specialists meet to plan treatment for a patient with complex problems, questions for the orthodontist often are along the lines of “Could you retract the incisors enough to correct the overjet?” or “Could you develop incisal guidance for this patient?” To a question phrased as, “Could you …?” the answer often is yes, given an unlimited commitment to treatment. The more appropriate question is not “Could you …?” but “Should you …?” or “Would it be best for the patient to …?” Cost-benefit and risk-benefit analyses (Figure 7-1) are introduced appropriately when the question is rephrased that way.
At this point, before we talk in detail about the steps in going from the problem list to the final treatment plan that are outlined in Figure 7-1, let us examine some important concepts that underlie orthodontic treatment planning more generally.
Major Issues in Planning Treatment
Predictability and Complexity of Treatment
If alternative methods of treatment are available, as usually is the case, which one should be chosen? Data gradually are accumulating to allow choices to be based on evidence of outcomes rather than anecdotal reports and the claims of advocates of particular approaches. The quality of evidence for clinical decisions and how to evaluate the data as reports of treatment outcomes become available are emphasized in Chapter 1.
The complexity of the proposed treatment affects treatment planning, especially in the context of who should do the treatment. The focus of this chapter is on planning comprehensive orthodontic treatment. In orthodontics as in all areas of dentistry, it makes sense that the less complex cases would be selected for treatment in general or family practice, while the more complex cases would be referred to a specialist. In family practice, an important issue is how you rationally select patients for treatment or referral. A formal scheme is presented in Chapter 11 for separating child patients most appropriate for orthodontic treatment in family practice from those more likely to require complex treatment, and a similar scheme for adults appears in Chapter 18.
Treatment Possibilities
Dental Crowding: To Expand or Extract?
Esthetic Considerations
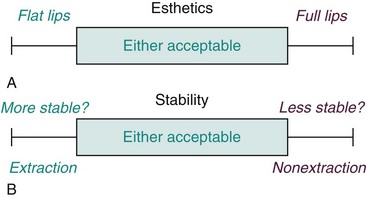
If the major factors in extraction decisions are stability and esthetics, it is worthwhile to review existing data that relate these factors to expansion and extraction. Consider esthetics first. The conceptual relationship between expansion/extraction and esthetics is illustrated in Figure 7-2. All other things being equal, expansion of the arches moves the patient in the direction of more prominent teeth, while extraction tends to reduce the prominence of the teeth. Facial esthetics can become unacceptable on either the too-protrusive or too-retrusive side.
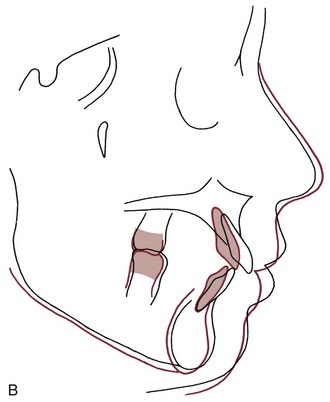
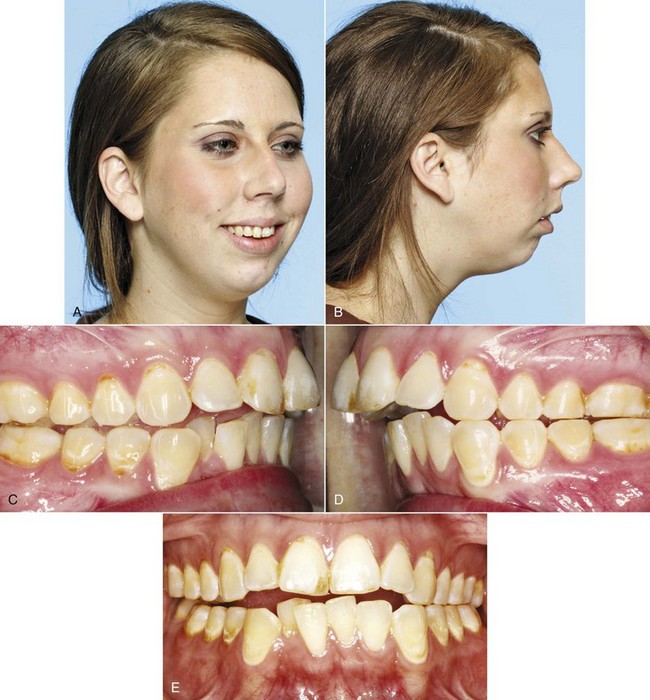
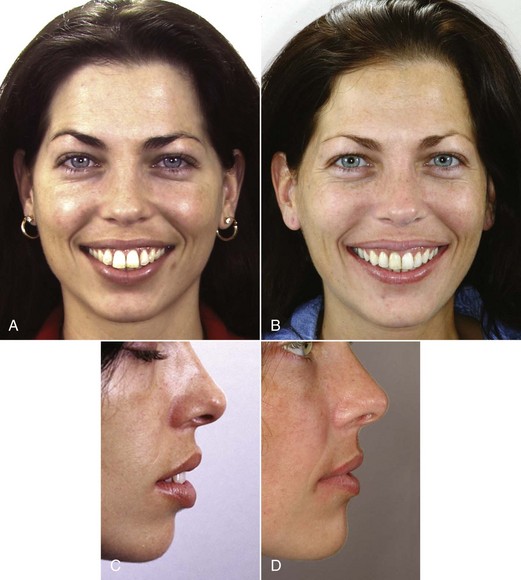
At what point have the incisors been moved too far forward so that facial appearance is compromised? The answer is found in soft tissue not hard tissue relationships: When the prominence of the incisors creates excessive lip separation at rest so that the patient must strain to bring the lips together, the teeth are too protrusive and retracting the incisors improves the facial appearance (Figure 7-3). Note that this has remarkably little to do with the prominence of the teeth relative to the supporting bone as seen in a profile view. An individual with thick, full lips looks good with incisor prominence that would not be acceptable in someone with thin, tight lips. You simply cannot determine the esthetic limit of expansion from tooth–bone relationships on a cephalometric radiograph.
At what point are the incisors retracted to the point of adversely affecting facial esthetics? This too depends largely on the soft tissues. The size of the nose and chin has a profound effect on relative lip prominence. For a patient with a large nose and/or a large chin, if the choices are to treat without extraction and move the incisors forward or to extract and retract the incisors at least somewhat, moving the incisors forward is better, provided it does not separate the lips too much. The upper incisors are too far lingually if the upper lip inclines backward—it should be slightly forward from its base at soft tissue point A (Figure 7-4, A). For best esthetics, the lower lip should be at least as prominent as the chin (Figure 7-4, B). Variations in chin morphology may put the proper incisor–chin relationship beyond the control of orthodontics alone, in which case chin surgery perhaps should be considered (see the sections in this chapter on Class II camouflage and maximizing esthetic changes in treatment and Chapter 19).
Stability Considerations
For stable results, how much can arches be expanded? The lower arch is more constrained than the upper, and so its limitations for stable expansion may be somewhat tighter than the upper arch. Current guidelines for the limits of expansion of the lower arch, admittedly based on limited data, are presented in Figure 7-5. The 2 mm limitation for forward movement of the lower incisors obviously is subject to considerable individual variation but makes sense in light of the observation that lip pressure increases sharply 2 mm out into space usually occupied by the lip (see Chapter 5). If lip pressure is the limiting factor in forward movement, as it probably is, the initial position of the incisors relative to the lip would be a consideration in how much movement could be tolerated. This suggests and clinical observation seems to confirm (again, limited data!) that incisors tipped lingually away from the lip can be moved farther forward than upright incisors. Incisors tipped labially and crowded probably represent the equivalent of a titrated end point in a chemical reaction, in that they have already become as protrusive as the musculature will allow. Moving them any further forward carries great risk of instability (see Figure 7-2).
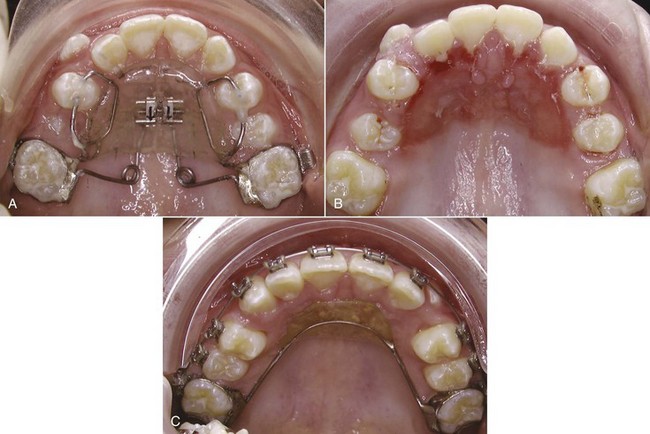
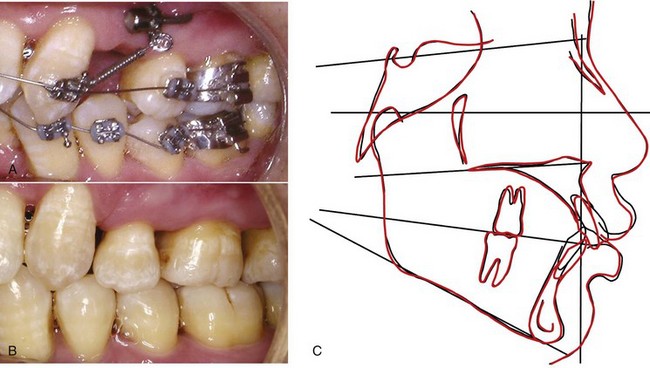
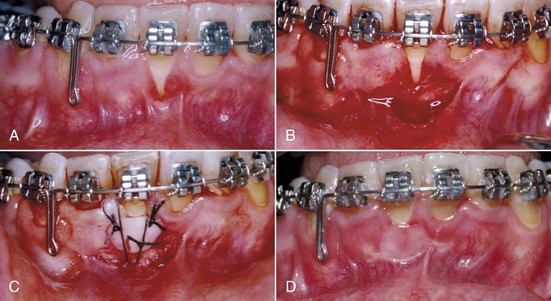
There also is a soft tissue limitation in how far the incisors, especially the lower incisors, can be moved facially. Fenestration of the alveolar bone and stripping of the gingiva become increasingly likely as the incisors are advanced. The amount of attached gingiva is a critical variable. It is important to carefully monitor patients who have a marginal amount of attached gingiva so that they can be treated promptly if a problem arises (Figure 7-6). Pretreatment consultation with a periodontist often is advisable, and depending on the amount and direction of planned tooth movement, placing a gingival graft before orthodontic treatment begins may be the best option for these patients.
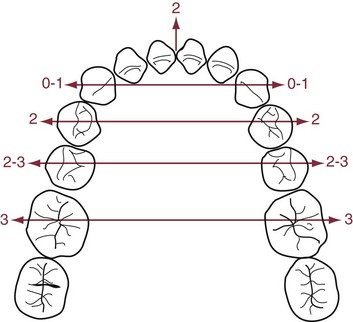
Figure 7-5 suggests that there is more opportunity to expand transversely than anteroposteriorly—but only posterior to the canines. Numerous reports show that transverse expansion across the canines is almost never maintained, especially in the lower arch. In fact, intercanine dimensions typically decrease as patients mature, whether or not they had orthodontic treatment, probably because of lip pressures at the corners of the mouth. Expansion across the premolars and molars is much more likely to be maintained, presumably because of the relatively low cheek pressures.
One approach to arch expansion is to expand the upper arch by opening the midpalatal suture. If the maxillary base is narrow, this is appropriate treatment (see the discussion of transverse maxillary deficiency below). Some clinicians theorize (with no supporting evidence) that generously expanding the upper arch by opening the suture, temporarily creating a buccal crossbite, allows the lower arch then to be expanded more than otherwise would have been possible. If the limiting factor is cheek pressure, it seems unlikely that the method of expansion would make any difference. Excessive expansion carries the risk of fenestration of premolar and molar roots through the alveolar bone. There is an increasing risk of fenestration beyond 3 mm of transverse tooth movement.1
Contemporary Extraction Guidelines
• Less than 4 mm arch length discrepancy: Extraction rarely indicated (only if there is severe incisor protrusion or in a few instances, a severe vertical discrepancy). In some cases, this amount of crowding can be managed without arch expansion by slightly reducing the width of selected teeth, being careful to coordinate the amount of reduction in the upper and lower arch.
• Arch length discrepancy 5 to 9 mm: Nonextraction or extraction treatment possible. The decision depends on both the hard- and soft-tissue characteristics of the patient and on how the final position of the incisors will be controlled; any of several different teeth could be chosen for extraction. Nonextraction treatment usually requires transverse expansion across the molars and premolars, and additional treatment time if the posterior teeth are to be moved distally, to increase arch length.
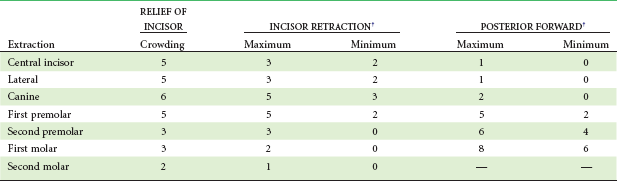
• Arch length discrepancy 10 mm or more: Extraction almost always required. For these patients, the amount of crowding virtually equals the amount of tooth mass being removed, and there would be little or no effect on lip support and facial appearance. The extraction choice is four first premolars or perhaps upper first premolars and mandibular lateral incisors. Second premolar or molar extraction rarely is satisfactory because it does not provide enough space near crowded anterior teeth or options to correct midline discrepancies (Table 7-1).
It is interesting but not surprising that retrospective studies of changes in dental arch dimensions and facial appearance in extraction versus nonextraction cases show highly variable changes in both groups. The idea that extraction leads to incisor retraction and narrower arches and that nonextraction leads to incisor protrusion and wider arches is not well supported.2,3 The amount of change in both groups, of course, would be related to the amount of crowding and protrusion that was present initially and to the clinician’s decision as to how to manage arch expansion or closure of extraction spaces. Perhaps a final set of guidelines could be as follows:
• The more you can expand without moving the incisors forward, the more patients you can treat satisfactorily (from the perspective of both esthetics and stability) without extraction.
• The more you can close extraction spaces without overretracting the incisors, the more patients you can treat satisfactorily (again, from the perspective of both esthetics and stability) with extraction.
• For oral health, excessive expansion increases the risk of mucogingival problems.
• For masticatory function, expansion or extraction makes no difference.
Skeletal Problems: Growth Modification versus Camouflage
If it were possible, the best way to correct a jaw discrepancy would be to get the patient to grow out of it. Because the pattern of facial growth is established early in life and rarely changes significantly (see Chapter 2), this is unlikely without treatment. The important questions in planning treatment are the extent to which growth can be modified, and how advantageous it is to start treatment prior to adolescence. Now that data from randomized clinical trials are available for Class II treatment outcomes, there is less reason for controversy about the best way to treat those patients (discussed in detail below), but skeletal problems in other planes of space remain controversial. Additional information on methods for early treatment of skeletal problems is presented in Chapter 12.
Transverse Maxillary Deficiency
It is appropriate to discuss maxillary deficiency at the beginning of this discussion of skeletal problems because of its relationship to the extraction–nonextraction decision that was just reviewed. In a child with crowded teeth, a diagnosis of deficient maxillary width can become a convenient rationale for enough transverse expansion to align the teeth. If the maxilla is narrow relative to the rest of the face, a diagnosis of transverse maxillary deficiency is justified and skeletal expansion probably is appropriate. Both the width of the maxillary premolar teeth (via Pont’s index, an old and now-discredited approach)4 and the width of the palate compared to population norms have been advocated as methods to diagnose maxillary deficiency. As we have emphasized in Chapter 6, the appropriate comparison of maxillary width should be to other transverse proportions in the same patient (for example, bizygomatic width), not to population averages.
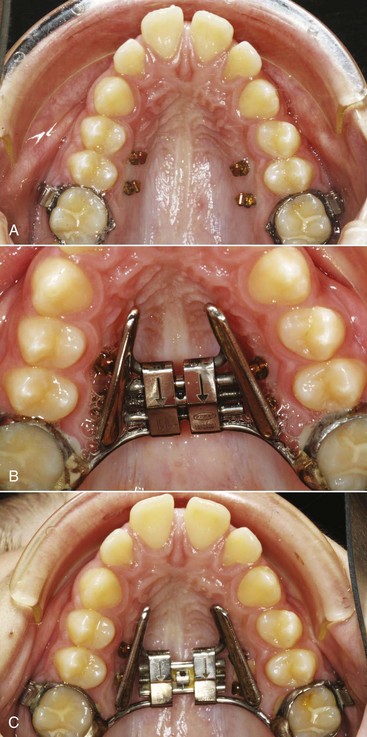
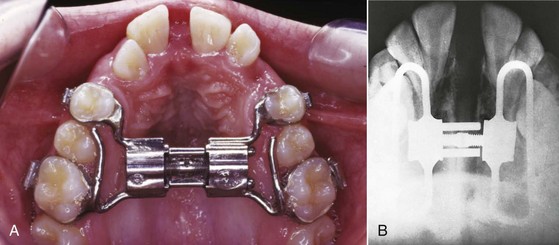
Like all craniofacial sutures, the midpalatal suture becomes more tortuous and interdigitated with increasing age (see Figure 8-30). Almost any expansion device (a lingual arch, for example) will tend to separate the midpalatal suture in addition to moving the molar teeth in a child up to age 9 or 10. By adolescence, relatively heavy force from a rigid jackscrew device (Figure 7-7) is needed to separate the partially interlocked suture, which must be microfractured. The maxilla opens as if on a hinge superiorly at the base of the nose and also opens more anteriorly than posteriorly.
It is important to realize that heavy force and rapid expansion should not be used in preschool children because of the risk of producing undesirable changes in the nose at that age (Figure 7-8). After adolescence, there is an increasing chance with advancing age that bone spicules will have interlocked the suture to such an extent that it cannot be forced open, and at that point surgery to reduce the resistance to expansion is the only way to widen the palate (see Chapter 18).
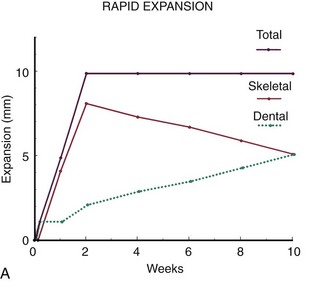
Rapid Palatal Expansion: A major goal of growth modification always is to maximize the skeletal changes and minimize the dental changes produced by treatment. The object of maxillary expansion is to widen the maxilla, not just expand the dental arch by moving the teeth relative to the bone. Originally, rapid expansion of the midpalatal suture (rapid palatal expansion [RPE]) was recommended to help meet this goal. The theory was that with rapid force application to the posterior teeth, there would not be enough time for tooth movement, the force would be transferred to the suture, and the suture would open up while the teeth moved only minimally relative to their supporting bone.
If the changes were represented graphically, the plot for rapid expansion would look like Figure 7-9, A. Note that when the expansion was completed, 10 mm of total expansion would have been produced by 8 mm of skeletal expansion and only 2 mm of tooth movement. At 4 months, the same 10 mm of dental expansion would still be present, but at that point there would be only 5 mm of skeletal expansion, and tooth movement would account for the other 5 mm of the total expansion. Rapid activation of the jackscrew, therefore, is not an effective way to minimize tooth movement.
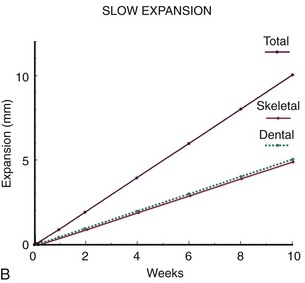
Slow Palatal Expansion: Approximately 0.5 mm per week is the maximum rate at which the tissues of the midpalatal suture can adapt. If a jackscrew device attached to the teeth is activated at the rate of one-quarter turn of the screw (0.25 mm) every other day, the ratio of dental to skeletal expansion is about 1 to 1, tissue damage and hemorrhage at the suture are minimized, and a large midline diastema never appears. Ten mm of expansion over a 10-week period, at the rate of 1 mm per week, would consist of 5 mm of dental and 5 mm of skeletal expansion (Figure 7-9, B). The situation at the completion of active expansion is approximately analogous to RPE 2 to 3 months after expansion is completed, when bone fill-in has occurred. Thus the overall result of rapid versus slow expansion is similar,5 but with slower expansion a more physiologic response is obtained.
Implant-Supported Expansion: Now that bone screws can be placed in the maxilla to serve as temporary skeletal attachments, force can be applied directly to the maxilla instead of using the teeth to transfer force to the bone. This provides a way to expand the maxilla even if no teeth are present (Figure 7-10) and would avoid tooth movement and should produce almost total skeletal change in patients with lingual crossbite. With a jackscrew attached to skeletal anchors, minimum disruption of the suture would be desired, so slow rather than rapid expansion would be indicated.
Maxillary expansion is discussed further in Chapters 13 and 14.
Class II Problems
Changing Views of Class II Treatment: In the early years of the twentieth century, it was all but taken for granted that pressure against the growing face could change the way it grew. Extraoral force to the maxilla (headgear) was utilized by the pioneer American orthodontists of the late 1800s (Figure 7-11), who found it reasonably effective. This method of treatment was later abandoned, not because it did not work, but because Angle and his contemporaries thought that Class II elastics (from the lower molars to the upper incisors) would cause the mandible to grow forward and that this would produce an easier and better correction. At a later stage in the United States, guide planes consisting of a wire framework extending down from an upper lingual arch were used to force patients to advance the mandible upon closure, also with the idea of stimulating mandibular growth.
Although headgear was reintroduced into American orthodontics in the 1940s and came to be widely used in Class II treatment, it was seen primarily as a tooth-moving device until cephalometric studies in the late 1950s clearly demonstrated not only retraction of upper teeth but also effects on maxillary growth (Figure 7-12). By the 1980s, clinical success with functional appliances, including impressive amounts of mandibular growth in some cases, had been clearly demonstrated on both sides of the Atlantic, but questions remained as to whether these appliances could really stimulate mandibular growth.
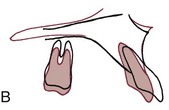
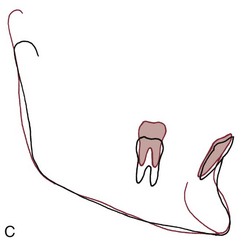
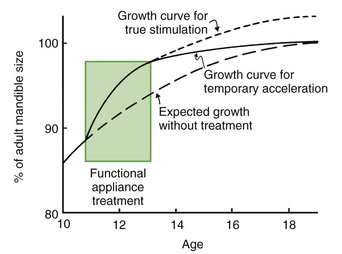
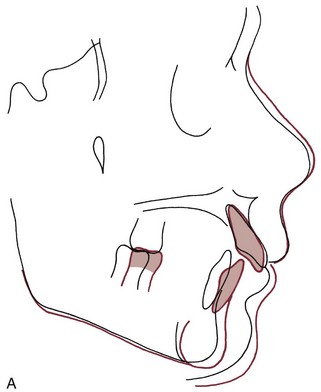
This depends on how you look at it. Growth stimulation can be defined in two ways: (1) as the attainment of a final size larger than would have occurred without treatment or (2) as the occurrence of more growth during a given period than would have been expected without treatment. Figure 7-13 is a hypothetical plot of the response to functional appliance treatment, illustrating the difference between (1) absolute stimulation (larger as an adult) and (2) temporal stimulation (acceleration of growth). As the figure suggests, an acceleration of growth often occurs when a functional appliance is used to treat mandibular deficiency, but the final size of the mandible is little if any larger than it would have been without the treatment.6 Cephalometric superimposition often shows more mandibular growth in the first months of functional appliance treatment than would have been expected (Figure 7-14). This is likely to be followed by a decrease in growth later, so that although the mandible grew faster than normal for a while, later growth was slower than would have been expected and the ultimate size of the mandible in treated and untreated patients is similar.
If that view of their effect on mandibular growth is correct, functional appliances must do something else besides accelerate mandibular growth. Otherwise, the Class II malocclusion would never be corrected or would not stay corrected. In fact, these appliances also can affect the maxilla and the teeth in both arches. When the mandible is held forward, the elastic stretch of soft tissues produces a reactive effect on the structures that hold it forward. If the appliance contacts the teeth, this reactive force produces an effect like Class II elastics, moving the lower teeth forward and the upper teeth back, and rotating the occlusal plane. In addition, even if contact with the teeth is minimized, soft tissue elasticity can create a restraining force on forward growth of the maxilla, so that a “headgear effect” is observed (see Figure 7-14). Any combination of these effects can be observed after functional appliance treatment.
Randomized Clinical Trials of Early versus Later Class II Treatment: In the 1990s, two major projects using randomized clinical trial methodology and supported by the National Institute of Dental and Craniofacial Research were carried out at the University of North Carolina and University of Florida.7,8 More recently, an important trial at the University of Manchester that was supported by the Medical Research Council of the United Kingdom has been reported.9 The results provide by far the best data that ever have been available for the response to Class II growth modification treatment.
The data from all the trials show three important things: (1) on average, children treated prior to adolescence with either headgear or a functional appliance had a small but statistically significant improvement in their jaw relationship, while the untreated control children did not; (2) changes in skeletal relationships created during early treatment were at least partially reversed by later compensatory growth, in both the headgear and functional appliance groups; and (3) at the end of comprehensive treatment during adolescence, there were no significant differences between the early treatment patients and the previously untreated controls. In short, it seems to make remarkably little difference whether growth modification is done with headgear or a functional appliance, and it is equally effective and more efficient to do it during the adolescent growth spurt rather than prior to adolescence. Further data from the trials and data from well-designed and controlled retrospective studies are discussed in more detail in Chapter 13.
Camouflage by Tooth Movement: Tooth movement alone cannot correct a skeletal malocclusion, but if the malocclusion is corrected and the facial appearance is acceptable, the overall treatment outcome can be quite satisfactory. This is called orthodontic camouflage for the simplest of reasons: camouflage means that the jaw discrepancy is no longer apparent. Of course, treatment with tooth movement is successful only if both the facial appearance and dental occlusion are satisfactory.
The following three patterns of tooth movement can be used to correct a Class II malocclusion:
• A combination of retraction of the upper teeth and forward movement of the lower teeth, without tooth extractions
• Retraction of maxillary incisors into a premolar extraction space
• Distal movement of maxillary molars and eventually the entire upper dental arch.
Nonextraction treatment with Class II elastics: If forward movement of the lower arch can be accepted, a Class II malocclusion can be corrected just with the use of Class II elastics (or their equivalent in the form of fixed connectors). The correction is achieved, however, much more by forward movement of the lower arch than by moving the upper teeth back. Rarely, excess overjet and Class II buccal segments are due to a lower arch that is distally positioned on the mandible, and then moving the lower teeth forward is exactly what is needed. Almost always, however, Class II patients have the lower teeth normally positioned on the mandible or proclined to some extent. For these patients, the result of Class II elastics or their equivalent in the form of a fixed functional appliance is likely to be a convex profile with protrusive lower incisors and a prominent lower lip. This is best described as relapse waiting to occur (Figure 7-15). After treatment, lip pressure that moves the lower incisors lingually leads to incisor crowding, return of overjet, and return of overbite as the incisors tend to erupt back into occlusal contact from their lingual position.
Retraction of the upper incisors into a premolar extraction space: A straightforward way to correct excessive overjet is to retract the protruding incisors into space created by extracting the maxillary first premolars. Without lower extractions, the patient would have a Class II molar relationship but normal overjet and canine relationships at the end of treatment. Temporary skeletal anchorage is very useful when maximum incisor retraction is desired or if the maxillary molars have little anchorage value because of bone loss. If mandibular first or second premolars also are extracted, Class II elastics can be used to bring the lower molars forward and retract the upper incisors, correcting both the molar relationship and the overjet.
Although premolar extraction for Class II correction can produce excellent occlusion and an acceptable dentofacial appearance,10 there are potential problems with this approach. If the patient’s Class II malocclusion is primarily due to mandibular deficiency, retracting the maxillary incisors would create a maxillary deformity to go with the mandibular one, which is difficult to justify as correct treatment (see the discussion of Class II camouflage in adults in Chapter 18). Extractions in the lower arch allow the molars to come forward into a Class I relationship, but it would be important to close the lower space without retracting the lower incisors. If Class II elastics are used, the upper incisors are elongated as well as retracted, which can produce an undesirable “gummy smile.”
Maxillary premolar extraction for Class II correction has been criticized as a risk factor for future TM dysfunction (TMD). No relationships between symptoms of TMD and the type of orthodontic treatment were noted in any of a considerable series of reports in the early 1990s. The best data come from a study in which a careful compilation of retrospective data was used to create two groups of patients whose “borderline” Class II malocclusions could have been treated equally plausibly with or without premolar extraction. One group had extractions, the other did not. Both groups had low scores for signs or symptoms of dysfunction, and there was no difference between them in any aspect of TM joint function.11 There is simply no evidence to support the allegation that maxillary premolar extraction causes TMD.
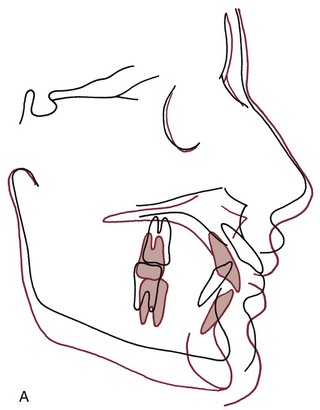
Distal movement of the upper teeth: If the upper molars could be moved posteriorly, this would correct a Class II molar relationship and provide space into which the other maxillary teeth could be retracted. If the maxillary first molars are rotated mesiolingually, as they often are when a Class II molar relationship exists, correcting the rotation moves the buccal cusps posteriorly and provides at least a small space mesial to the molar (Figure 7-16). Tipping the crowns distally to gain space is more difficult, and bodily distal movement is more difficult still. There are two problems: (1) it is difficult to maintain the first molar in a distal position while the premolars and anterior teeth are moved back, so it must be moved back a considerable distance, especially if it is tipped distally; and (2) the farther it must be moved, the more the second and third molars are in the way.
From this perspective, it is easy to understand that the most successful way to move a maxillary first molar distally is to extract the second molar, which creates space for the tooth movement. Until quite recently, the anchorage created by a transpalatal lingual arch was accepted as the best way to undertake distalization of the maxillary dentition. Although it is at least theoretically possible to do this with headgear, this type of treatment is time-consuming and requires excellent patient cooperation. Palatal anchorage for the molar movement can be created by splinting the maxillary premolars and including an acrylic pad in the splint so that it contacts the palatal mucosa. In theory, the palatal mucosa resists displacement; in clinical use, tissue irritation is likely. Even with the more elaborate appliances of this type (Figure 7-17), only about two-thirds of the space that opens between the molars and premolars is from distal movement of the molars, even when the molars are tipped distally. They tend to come forward again when the other maxillary teeth are retracted (see Chapter 15 for more details), so more than a half-cusp molar correction cannot be expected. The ideal patient for treatment with this approach, therefore, is one with minimal growth potential, a reasonably good jaw relationship (not severely mandibular deficient) and a half-cusp Class II molar relationship.
Using temporary skeletal anchorage greatly improves the amount of true distal movement of the maxillary dentition that can be achieved, and makes it possible to distalize both the second and first molars. It still is necessary to create some space in the tuberosity region, so removal of third molars is likely to be required later if it is not done immediately. In typical treatment, bone anchors are placed bilaterally in the vicinity of the base of the zygomatic arch (Edward Angle’s “key ridge”) or in the palate, and a nickel-titanium spring generates the force needed for distalization (Figure 7-18). For this purpose, bone screws between the teeth prevent the necessary distal movement of roots mesial to the screw. Although good data for typical treatment outcomes still do not exist, in some patients it has been possible to produce up to 6 mm of distal movement of first and second molars.12 In addition, the premolars migrate distally as the molars are moved back (which is due to the supercrestal fiber network). This makes the premolar retraction less complicated, and there also is no reaction force against the incisors to move them facially.
Summary: In the absence of favorable growth, treating a Class II relationship in adolescents is difficult. Compromises may have to be accepted in order to correct the occlusion. Fortunately, even though growth modification cannot be expected to totally correct an adolescent Class II problem, some forward movement of the mandible relative to the maxilla does contribute to successful treatment of the average patient. The rest of the correction must occur from some combination of retraction of the upper incisors and forward movement of the lower arch. When little or no growth can be expected, orthognathic surgery to advance the mandible may be necessary to achieve a satisfactory result (see Chapter 19).
Class III Problems
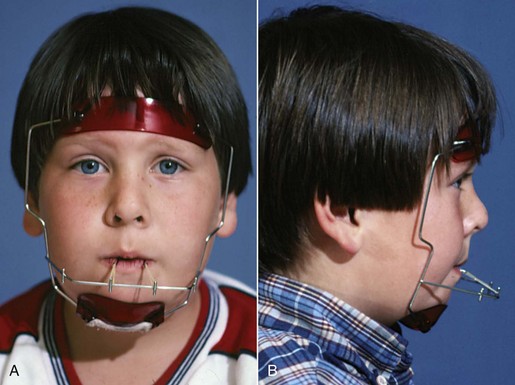
Horizontal-Vertical Maxillary Deficiency: If headgear force compressing the maxillary sutures can inhibit forward growth of the maxilla, reverse (forward-pull) headgear separating the sutures should stimulate growth. Until Delaire and coworkers in France showed that forward positioning of the maxilla could be achieved with reverse headgear, if treatment was begun at an early age, reverse pull headgear (Figure 7-19) was remarkably unsuccessful in producing anything but movement of the upper teeth. The French results suggested that successful forward repositioning of the maxilla can be accomplished before age 8, but after that, orthodontic tooth movement began to overwhelm skeletal change, and more recent studies comparing untreated Class III children to those treated with maxillary protrusion have confirmed greater skeletal change at earlier ages.13 Long-term follow-up suggests that for a good chance of success, treatment should begin by age 10 at the latest.14 The chance of successful forward movement is essentially zero by the time sexual maturity is achieved.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


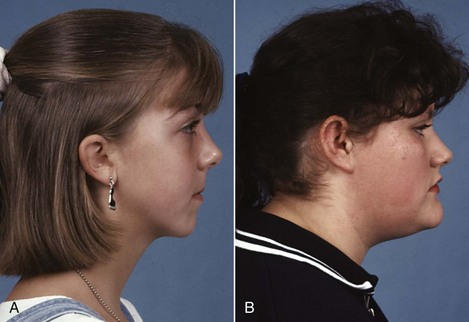
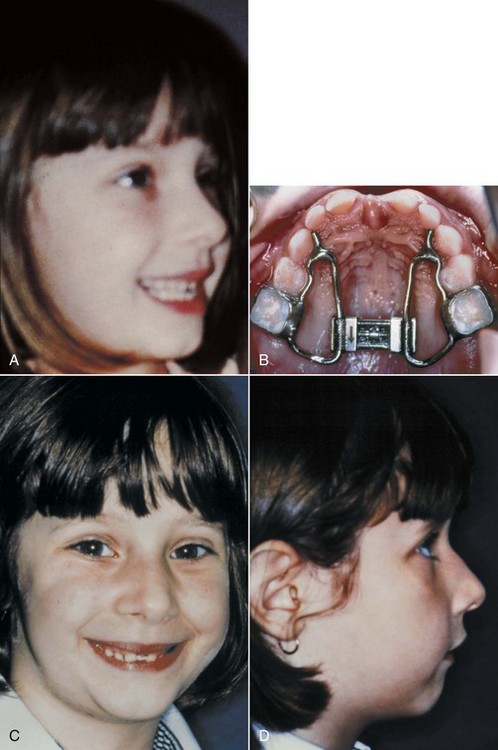
 mm/day (2 turns/day of the jackscrew). A, Nasal contours before treatment. B, Jackscrew appliance after activation over a 10-day period. C and D, Nasal hump and paranasal swelling, which developed after the child complained of discomfort related to the expansion.
mm/day (2 turns/day of the jackscrew). A, Nasal contours before treatment. B, Jackscrew appliance after activation over a 10-day period. C and D, Nasal hump and paranasal swelling, which developed after the child complained of discomfort related to the expansion.