6
Use of CAD/CAM Technology in Custom Abutment Manufacturing
1Department of Restorative Dentistry, Division of Graduate and Post Graduate Prosthodontics, Tufts University School of Dental Medicine, Boston, MA
2Private Practice, Boston, MA
History of Cad/Cam Technology in Prosthetic Dentistry
Computer-aided design (CAD)/computer-aided milling (CAM) technology first appeared in prosthetic dentistry with the introduction of the first CEREC scanning and milling system in 1985 (Siemens AG, Germany) (Calamia 1994; Isenberg and Garber 1994). CEREC is an acronym for “chairside economical restoration of esthetic ceramics.” The first CEREC system photographed the cavity preparation and stored the photograph as a 3-dimensional (3D) digital model. Next, the proprietary software approximated the restoration shape using biogeneric comparisons with the surrounding teeth. The clinician could then refine that model using 3D CAD software, after which an optical scanner controlled a milling machine that carved the actual restoration out of a ceramic block using diamond head cutters. The milled ceramic restoration was then bonded into the tooth using a resin cement.
Another early CAD/CAM system was the CELAY system (Mikrona Technologie AG, Switzerland) (Eidenbenz et al. 1994; McLaren and Sorensen 1994). The CELAY system had some advantages over the early CEREC system as it could create all surfaces of a restoration, whereas the earliest CEREC system could not fabricate the occlusal surface. Another advantage was that the CELAY system had the potential to fabricate crowns and short-span bridges utilizing the In-Ceram system (Vita Zahnfabrik, Bad Säckingen, Switzerland) (Eidenbenz et al. 1994). Both the CEREC and CELAY systems could be used for direct and indirect restoration fabrication so the clinician could opt for completing a milled ceramic restoration in a single patient appointment. This is still an attribute of the current day CEREC 3D system.
Through most of the 1980s and 1990s, CEREC outpaced CELAY with production advances and became the predominant CAD/CAM chairside milling system in clinical use. Both its software and milling hardware have undergone numerous changes and CEREC can now offer clinicians sophisticated ideal tooth morphology design and milling capability. A second generation scanning and milling unit was developed in 1994, which was followed 8 years later in 2002 by the CEREC 3D system (the first Windows®-based CEREC product) (Figure 6.1).
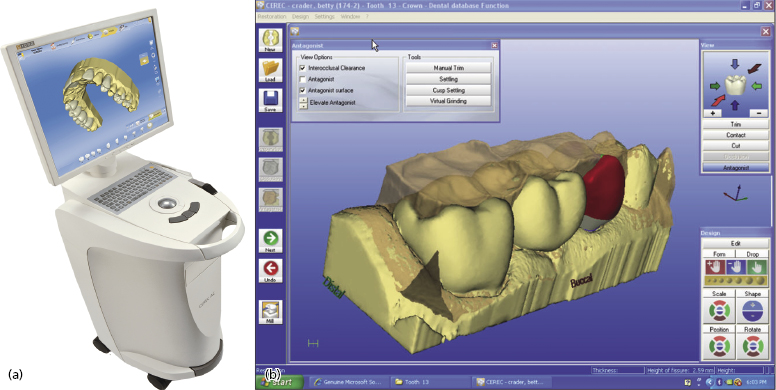
The CEREC technology spawned an entire speciality of prosthetic dentistry that, at present, comprises over 100 milling systems that produce implant abutments, copings, removable partial denture frameworks, fixed bridge frameworks, fixed implant frameworks, crowns, inlays, onlays, and porcelain veneers.
History of Cad/Cam Technology in Implant Abutment Manufacturing
CAD/CAM custom manufacturing technology developed at a time when custom abutment options for implants were mostly created manually by technicians utilizing a UCLA wax-up sleeve (Branemark Implants, Gothenberg, Sweden) that fitted over an external hex platform design (Nishimura et al. 1999). The UCLA plastic sleeve acted as scaffold to hold a technician-created wax-up that shaped the custom abutment form. The wax-up was invested with the abutment connection, so that after burn-out, cast gold formed the abutment, which was mechanically adhered to the connection. The abutment then screwed over an external hex onto the implant body. Later UCLA plastic designs incorporated the external hex into the plastic waxing sleeve so that the entire waxed abutment was a one-piece abutment. This could then be secured onto the hex with an abutment screw.
Adaptations to the UCLA design came from other implant manufacturers (e.g. Core-Vent, Van Nuys, CA, USA), who created preformed plastic waxing components that fitted inside the implant. These plastic burn-out components could be trimmed and waxed onto so as to form ideal tooth preparation forms that, after casting in gold, would fit back into the implant body. The cast abutments were internally cemented to the implant instead of being screwed into place like the traditional UCLA abutment. Recurrent clinical problems were observed with these internally cemented, castable abutments. One was dislodgement due to problems with the cementation. Another was fracture of the internally cemented post (which rendered the internal compartment of the implant body useless). Such problems resulted in cementable abutments losing clinical acceptance to the internally hexed, screw-retained custom abutments.
The first manufactured CAD/CAM abutment technology utilized in implant–abutment prosthodontics was described in 2000 as the Atlantis Custom Abutment Technology (Atlantis Components, Cambridge, MA, USA) (Figure 6.2) (Kerstein et al. 2000). Osorio, in collaboration with Atlantis Components, secured the first patents on computer-aided virtual design technology for implant abutments (Osorio 1997; Osorio et al. 1999, 2001).
The earliest Atlantis abutment design capability eliminated the need for a technician-created wax-up by employing design software that contained numerous virtual tools to create the abutment virtually (VAD™, Atlantis Components). First, a master cast was made from an intra-oral transfer impression that located: (i) the intra-arch position of the implant to be restored; (ii) the soft tissue contours around the implant; (iii) the neighboring teeth; and (iv) the opposing occlusal clearance. This master cast and its opposing cast were scanned individually (Figure 6.3), and then virtually articulated within the design software.

The virtual abutment design templates of the incisors (Figure 6.4a), canines, premolars, and molars could then be modified using numerous measurement and design tools, to create a virtual patient-specific abutment (Figure 6.4b).
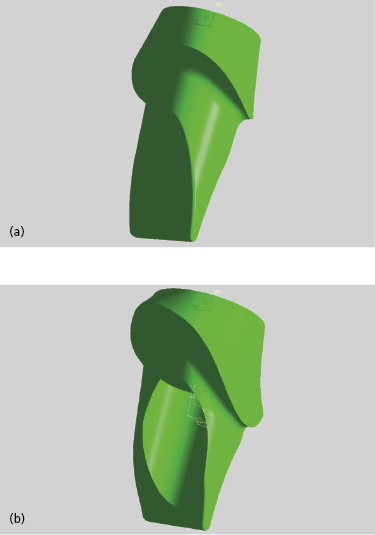
When the virtual design was complete, the digital abutment files were exported to a milling machine where commercially available pure titanium blanks were milled into the final abutment (see Figure 6.2). The milling of the blanks included: (i) the abutment screw access; (ii) differing abutment connections to accommodate many different implant systems; (iii) the hex (either internal or external); (iv) the cuspal contours and occlusal morphology; (v) a shoulder or chamfer margin; and (vi) the abutment base, which was shaped to maximize an ideal tooth preparation form despite screw access (Figure 6.5).
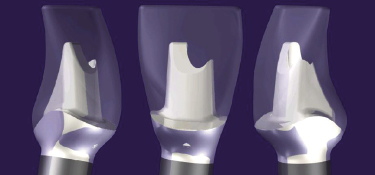
Because the abutments were milled from computer files, a single abutment could be duplicated multiple times. A patient could wear a provisional restoration, while the lab technician had a duplicate one to create the final crown (Kerstein and Osorio 2003). Today, the Atlantis virtual design and custom abutment milling technology is used to manufacture titanium, gold hue, and zirconia custom abutments (Figure 6.6).

Prior to Atlantis, the Procera® technology was developed in the mid-1990s (Nobel Biocare Procera LLC, Mahwah, NJ, USA) (Andersson et al. 1998). Procera technology was initially capable of fabricating all-ceramic crowns. Later, the Procera system expanded to include the fabrication of custom abutments. These abutments were initially formed from a technician-created wax-up made on a plastic waxing sleeve that inserted into an implant analog. When the wax-up was complete, it was scanned and then milled out of blocks of ceramic materials. Today, the wax-up sleeve is still required to create Procera abutments. However, after being manually inserted into an implant analog, the wax-up sleeve and master cast are scanned into design software so that the abutment shape can be then virtually waxed-up.
The most notable differences between the early Atlantis abutment and the Procera abutment manufacturing processes were:
- The Procera abutment contours were the result of a technician’s waxed-up morphology.
- The Procera milled abutment was (and still is today) attached to the implant via a metal connecting element that is screwed through when inserting the abutment into the implant. This separate metallic connection incorporates an additional location within the implant–abutment system where the solidity of the screw anchorage can be compromised under occlusal function. This can result in increased risk of abutment dislodgements and zirconia fractures.
- The Procera system is a “closed system” that can only be utilized with Nobel Biocare implants (Nobel Biocare LLC, Yorba Linda, CA, USA).
- Atlantis titanium abutments did not rely on a technician-created wax-up for abutment contour.
- Atlantis titanium abutments did not require a separate metallic connection component to engage the implant. This was because they were virtually designed and milled from the implant connection all the way up to the cuspal contours. The connection to the implant was milled in one piece in titanium without additional locations within the implant–abutment system where the solidity of the screw anchorage could be compromised under occlusal function. This is still the case today for titanium and zirconia Atlantis abutments.
- Atlantis technology is not a “closed system.” It can be employed with over 50 different implant connections, including the connections from but not limited to Astratech (Astratech/Atlantis, Waltham, MA, USA), Nobel Biocare (Nobel Biocare LLC), Biomet 3i (Biomet 3i, Palm Beach Gardens, FL, USA), Zimmer (Zimmer Dental, Carlsbad, CA, USA), Straumann (Straumann USA LLC, Andover, MA, USA), Dentsply/Friadent (Friadent GmbH, Manheim, Germany), and BioHorizons (BioHorizons, Birmingham, AL, USA). The Atlantis VAD software incorporates the connection size and shape parameters of various implants, and mills the custom abutment for these different connection designs. This flexibility allows the restorative dentist to use a single custom abutment system even if his/her surgical team utilizes many different types of implants.
The next early CAD/CAM abutment system was the Encode System™ (Biomet 3i) (Drago and Peterson 2007). The Encode System scanned a cast made from an intra-oral impression that measured the position of different-sized healing caps that contained orientating surface lines. The different-sized healing caps fit specific underlying implant sizes, and the surface orientating lines predicted the rotational position of the underlying implant. From these combinations of scanned measurements, in combination with a technician-created wax-up, the Encode software could create a custom abutment for the underlying implant, which was milled for intra-oral use. Encode is available today as a closed system and can only be used with 3i implants.
This chapter will discuss the Atlantis patient-specific custom abutment manufacturing technology, which spawned the entire custom abutment manufacturing segment of implant prosthodontics. At present, most other major implant companies have developed their own custom abutment manufacturing processes. However, these alternative systems follow the original Procera model by employing a wax–scan–mill approach that is technician driven and not software driven. Only the Atlantis process completely creates the abutment within a virtual environment before it is manufactured.
Table 6.1 describes some of the advantages and disadvantages of a number of commercially available manufactured custom abutment solutions.
Table 6.1 Comparison Chart of Some of the Commercially Available Custom Abutment Systems
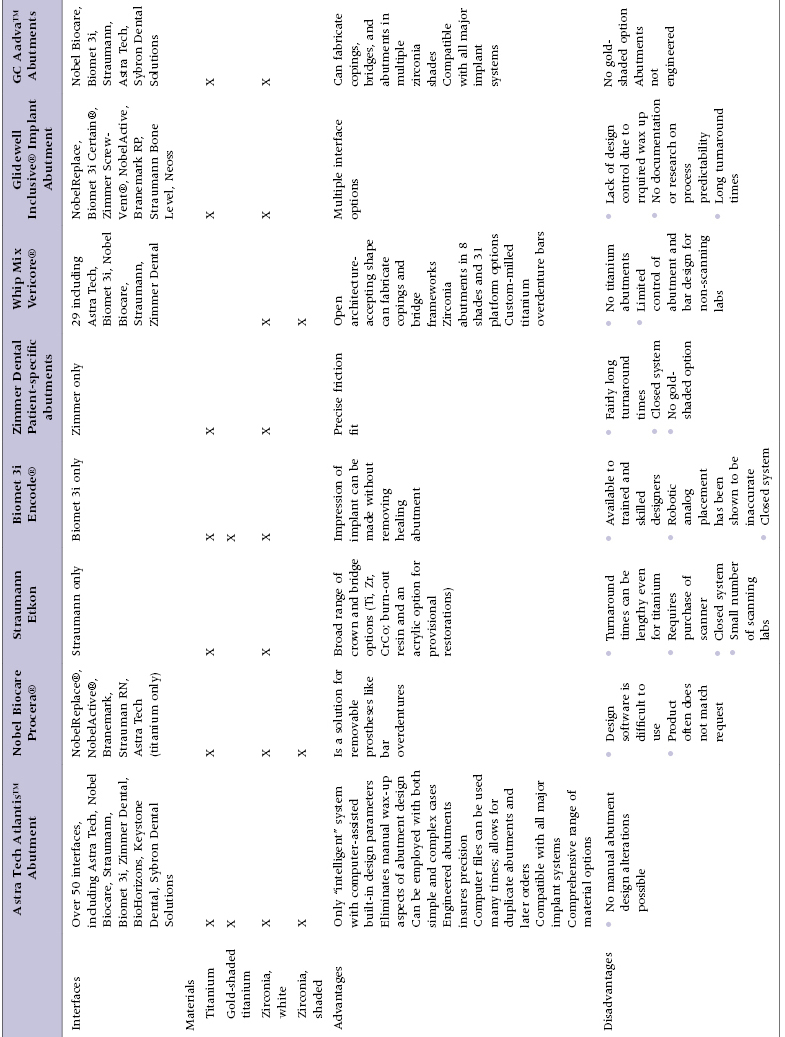
Virtual Design and Manufacture of Abutments
Design Process Prior to Machining Custom Abutments
The Atlantis custom abutment manufacturing process, which utilizes virtual abutment design software (Atlantis VAD, Astratech/Atlantis,Waltham, MA, USA), is an ISO 13485 certified and Food and Drug Administration (FDA) Quality System Regulation (QSR) compliant process. A manufactured custom abutment is first virtually created within the design software by virtual tools before it is machine milled. Before the virtual design process can start, a non-virtual implant master cast must be fabricated. The master cast contains all the implant analogs (that reproduce the intra-oral implant placements) surrounded by a removable soft tissue reproduction. Soft tissue removability allows for fit and placement evaluations of the final custom abutments; the abutment bases are fabricated anatomically wider than the implant body and the intra-oral peri-implant sulci.
Laboratory Steps in the Scanning and Fabrication of Custom Abutments
The steps in the scanning and fabrication of a custom abutment are shown in Figure 6.7. Master cast fabrication begins with the intra-oral placement of all the impression copings.
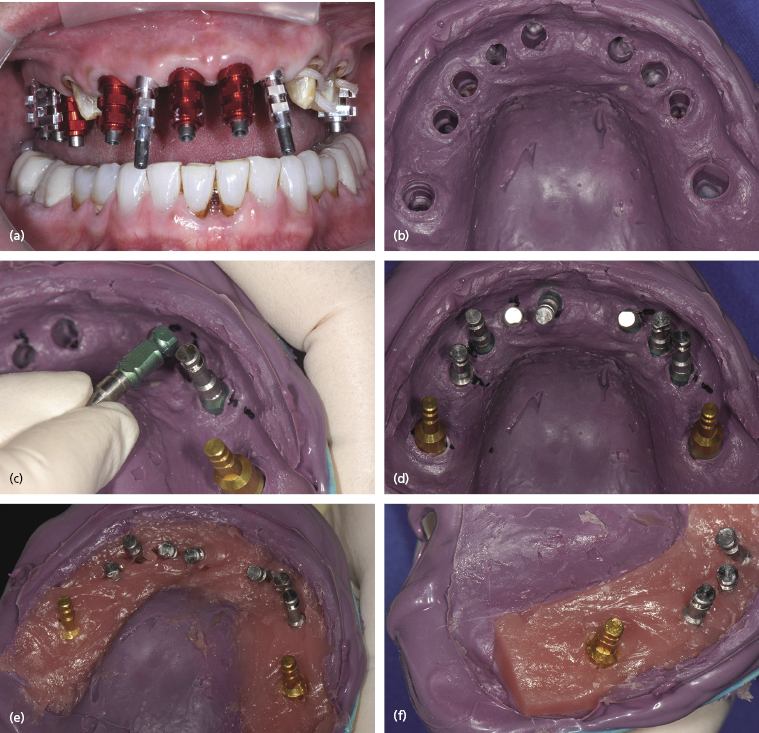
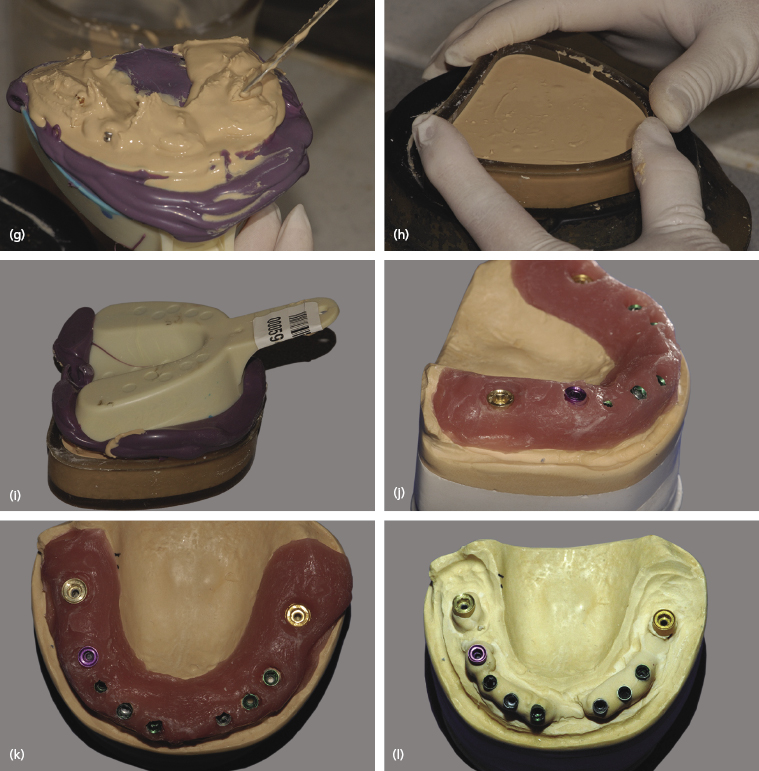
After radiographic confirmation that the impression copings are properly seated, the master impression can be made with an elastomeric impression material (Impregum, 3M Espe, Seefeld, Germany). The recovered impression is cleaned of blood and saliva, and then disinfected appropriately. The impression copings are removed from each implant, and the matched analogs placed onto each impression coping. They inserted back into their respective location within the impression guided by the individual copings’ axial wall shape.
Once all the impression copings are in place, the peri-implant tissues can be reproduced within the impression. A soft denture reline material (Zhermack Occludefast, River Edge, NJ, USA) is mixed and spatulated around the analogs. The occlusal third of the analog body is covered with the soft tissue material, leaving the apical two-thirds exposed. This allows the analog’s retentive elements to engage the die stone when it is poured. When the soft tissue is completely set, it is trimmed with a blade into a block-like shape that facilitates its easy removal and accurate replacement back into the final master cast. The removal and replacement of the soft tissue is crucial for the technician to be able to evaluate the seating of any oversized and fully anatomically designed abutments.
The die stone pour is accomplished in two stages. First, the impression is held inverted and vacuum-mixed die stone (Fuji Rock EP, GC America, Alsip, IL, USA) is vibrated into the impression. This is done until the intaglio surface and the retentive elements of each analog are completely covered with stone. Then, a rubber model base former is filled, after which the first pour is inverted onto the former so both pours together set completely.
The master cast is retrieved, trimmed, articulated, and smoothed externally. Because of the block cut of the soft tissue made prior to the die stone pour, the entire soft tissue element can be removed to simplify the seating of any oversized and fully anatomical abutments.
The master cast is then ready for optical scanning to begin the virtual abutment design.
Virtual Abutment Design of Custom Abutments
The sequence of steps involved in virtual abutment design can be seen in Figure 6.8. The procedure shows a mandibular right posterior quadrant that is to be restored with a single PFM crown (tooth no. 28) and two implant-supported splinted crowns in the no. 29 and no. 30 sites.
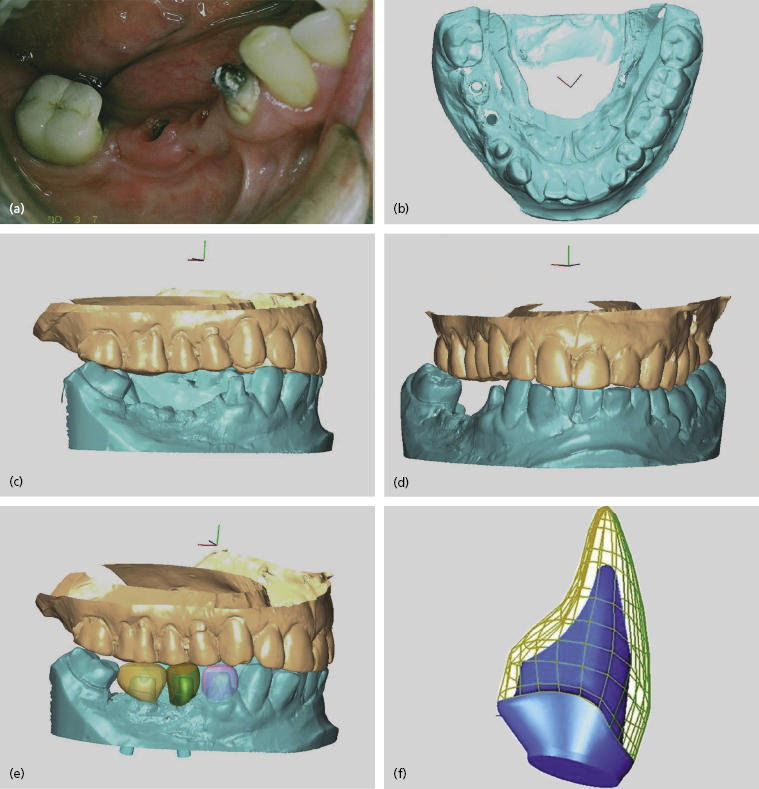
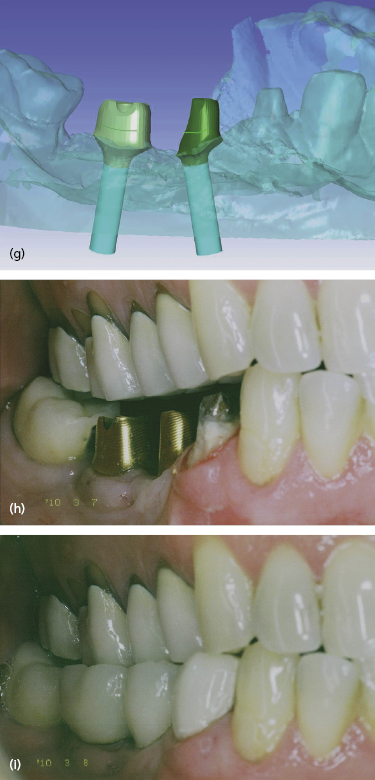
The stone master cast and its opposing cast are scanned and imported into the design software where they are reassembled and virtually occluded. Note in Figure 6.8d that there are two “holes” within the edentulous area where the implants have been “located” within the scanned cast. To facilitate ease of cast viewing during the design process, the occluded casts can be virtually rotated 360 degrees within the design software.
Next, virtual crowns are placed upon each implant (and any neighboring teeth that are being restored as well) and properly stretched into opposing occlusal contact. They are then virtually contoured to match the anatomic requirements of the neighboring teeth. In Figure 6.8e tooth no. 28 is virtually crowned in a pink-colored translucent restoration (denoting the presence of a neighboring non-implant restoration), while the implant virtual crowns in the no. 29 and no. 30 sites are represented in translucent green.
These virtual crown shapes will guide the future form of the underlying abutment to be designed in the same manner that a full contour wax-up and clear plastic template overlay would guide the manual creation of a cast custom abutment. The design software allows for easy removal (and replacement) of the implants, virtual crowns, and opposing cast so that all the case elements can be viewed with varying transparencies. Virtual crowns can also be displayed as a meshwork should the abutment designer prefers this to a transparent view.
All these desktop display features enhance the designer’s ability to visualize all anatomic aspects of the case. Under these optimally shaped virtual crowns, the ideal abutment morphology is generated from the external crown contours. The abutment morphology is therefore designed to properly fit underneath the individual final restoration. Figure 6.8g shows the implant angulations being corrected with the ideal abutment morphology within the virtual cast, in the same way that the final abutments will sit intra-orally to facilitate ideal restoration of the patient’s edentulous region.
Once the ideal abutment morphology has been virtually designed, the digital files are exported to the milling machinery for the manufacture of the final abutments. In this example, note how both abutments follow the opposing occlusal plane for future final crown fabrication. The final abutment form is a definitive match to the virtually designed abutments and will support the crown morphology that was also virtually designed.
Machine Milling of Custom Abutments
Although custom abutments began as traditional cast gold abutments, today the most frequent materials to be used are titanium, zirconium dioxide, and plastic (for provisional abutments). Custom abutments are milled from titanium or ceramic rods once the virtual design of the abutment is completed. The digital abutment files guide the cutting tools of the milling machines in 6 degrees of freedom through the differing abutment material(s) to manufacture a finished custom abutment.
Milling machines range in size, rate of abutment production, and cutting degrees of freedom. A typical milling machine can be seen in Figure 6.9. This machine mills long rods of commercially pure titanium within its milling chamber (rod materials milled are FDA 510K cleared) (Figure 6.10). Approximately 12 different abutments can be cut out of each foot-length of a titanium rod.


The milling takes place under copious amounts of cooling water spray (Figure 6.11).

When milling tools require replacement due to production wear, the milling machine self-manages the automated tool replacement. Depending on the product to be milled, the individual machines have their own “self-check” system in place, which monitors preprogrammed machining parameters while the milling process continually produces abutments. When the cutting tools fail to produce abutments that meet these machining parameters, the milling machine warns the operator of the need for component tool replacement. This approach ensures that the highest level of machining precision is consistently maintained for each milled abutment.
Milling Zirconia
Today, more abutments are being manufactured out zirconia than ever before. This is due to the fact that when zirconium is stabilized with yttrium trioxide (Y2O3) it has excellent mechanical properties for intra-oral use. It behaves very similarly to stainless steel, while its color can be modified to mimic the colors of teeth. Stabilized zirconia has a flexural strength of around 1200–1300 MPa, which compares well with PFM’s flexural strength of around 1400 MPa. It also resists cyclical loading stresses very well (Piconi and Maccauro 1999). Zirconia has been shown to be kinder to the peri-implant tissues than titanium as it creates less of an inflammatory reaction (Warashina et al. 2003; Degidi et al. 2006). This combination of strength characteristics, tooth color compatibility, and soft tissue acceptance, makes zirconia a very desirable material for custom abutment fabrication.
Milling of zirconium is similar to that of titanium; long dime-sized rods of non-sintered zirconia are employed (Figure 6.12).

Zirconia is best milled in a non-sintered state (known as the green state) as fully sintered Zirconia is so hard, making milling difficult and detrimental to the mechanical properties of the finished abutment. Alternatively, when zirconia is milled before full sintering, the useful mechanical properties of the material are preserved. The sintering process induces a 20% sintering shrinkage which must be allowed for in the abutment design to obtain a properly fitting abutment (Manicone et al. 2007). Zirconia abutments are therefore designed 20% larger than the desired final abutment (Figures 6.13 and 6.14).


A green-state milled abutment is sintered beginning at 500°C up through a range of temperatures to 1200–1500°C. This temperature range increases crystalline formation for maximum density without creating an excess of porosity formation. Sintering temperatures above 1500°C cause the porosity of the grains to increase so that it becomes impossible to produce a high-density abutment (Karaulov and Kudyak 1975). Once sintered, a zirconia abutment is finished and ready for intra-oral use.
Finishing Metallic Custom Abutments
Depending upon the system employed, finishing procedures of the various abutment manufacturing processes differ considerably. Metal finishing can range from hand polishing and contouring the raw titanium, to where abutments are milled into a finished state with retentive grooves and surface anatomy (requiring no surface smoothness corrections). Computer-guided surface finishing procedures can create superior surface characteristics to those obtainable with hand polishing methods. Figures 6.15 and 6.16 illustrate a comparison of a finished machined abutment surface to a manually polished abutment surface. Titanium can be coated with titanium nitride (TiN) to convert a sliver-colored abutment to a gold hue. TiN is a ceramic material that adheres to a titanium abutment by a vapor deposition process.

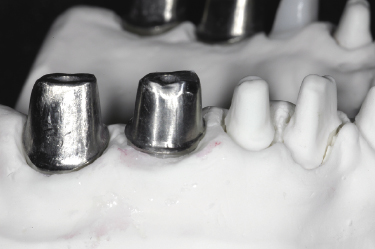
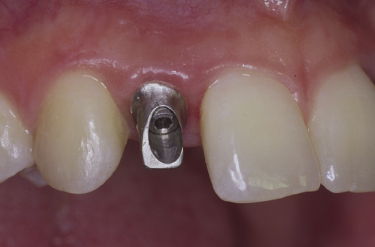
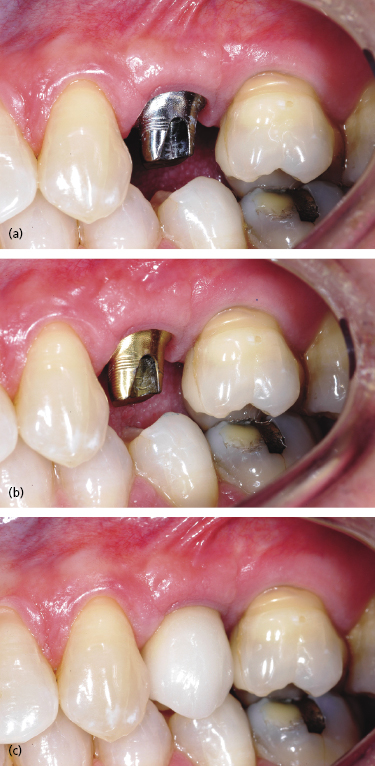
One advantage of using a gold hue surface application can be seen in the esthetic zone when there is thin tissue and the clinician employs a titanium abutment. A silver-colored titanium abutment can discolor the gingival margin, thus compromising the esthetic results of a visible implant restoration (Figure 6.17a). With the gold hue this problem is markedly improved as its yellow color does not discolor the gingival tissues (Figure 6.17b). Additionally, gold hue abutments can be used underneath all-ceramic crowns so that the underlying silver-colored metallic abutment does not lower the intrinsic value of the overlying crown (Figure 6.17c).
Another advantage of coating an abutment with TiN is that the coating withstands surface damage from routine intra-oral hygiene procedures better than uncoated abutments (Mengel et al. 2004). Mechanical abrasion by sharp dental hygiene instruments can leave more pronounced indentations and roughness on non-coated abutments when they are compared to silver nitride-coated abutments. These data suggest that TiN-coated abutment bases would be a better long-term plaque resister through the life of the implant prosthesis (due to better surface smoothness preservation), than would uncoated abutment bases.
Zirconium abutments are “finished” by the sintering process. Surface treatments and mechanical abrasion techniques to polish, smooth, or reshape the finished abutment can weaken the physical properties of the material and, therefore, are contraindicated.
Custom Abutment Inspection
Abutment I/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


