Chapter 6
Geriatric Patient Assessment
Mary R. Truhlar
Department of General Dentistry, School of Dental Medicine, Stony Brook University, Stony Brook, NY, USA
Introduction
The value of the geriatric assessment is that it provides a basis for treatment decisions and the prediction of treatment tolerance in the frail elderly patient.
This chapter is designed for the reader to develop an understanding of how to assess the older adult patient, why a focus on function is important, which tools are useful for incorporating into the dental office visit, and strategies to enhance communication and understanding with older patients. The importance of a “geriatric” assessment has long been recognized and classically described as “a multidisciplinary evaluation in which the multiple problems of older patients are uncovered, described, and explained, if possible, and in which the resources and strengths of the person are cataloged, need for services assessed, and a coordinated care plan developed to focus interventions on the person’s problems” (AGS Public Policy Committee, 1989). The value of a “geriatric” assessment versus a traditional patient assessment lies in the recognition that many times “usual” care may not meet an elderly patient’s needs. Despite the fact that the majority of elderly live independently, disability and dependency rises steadily with increasing age and must be part of the equation when developing any course of patient care.
A geriatric assessment is essential to the establishment of a realistic, well-planned, and beneficial course of dental treatment. The development of the tools and an approach to the individual assessment is base on the findings of measures of oral health status in older adult population assessments. The Geriatric Oral Health Assessment Index (GOHAI), a self-reported oral health assessment index, developed by Atchinson and Dolan (1990), gave the dental profession one of its first tools to measure oral health in the geriatric population. Ongoing population assessments give insight into changing population characteristics, the accuracy of developing diagnostic tools, as well as assess the effectiveness of implemented treatment modalities. Despite progress in the development of generally applicable assessment tools, the discipline of geriatrics is confounded by the innate population characteristic of increasing individual variability that naturally occurs with aging. The older adult/geriatric population is heterogeneous – ranging from physically fit, healthy, active, engaged elders to medically complex, frail, isolated individuals living either independently or with assistance in their own homes or in long-term care facilities. Age is only a number; it does not reflect ability or functionality. Therefore, a geriatric assessment should be an essential part of every older patient examination with the goal of efficiently and effectively collecting information that facilitates diagnosis, suggests interventions, is a predictor of outcomes and future needs, and takes into consideration the concerns and desires of the patient and/or caregiver. The key is to identify and become familiar with a select group of short screening assessments and communication strategies that will assist in establishing not only the patient desires and dental diagnosis, but will provide an appraisal of the patient’s capacity to tolerate as well as the prognosis of a selected course of dental treatment.
Common geriatric conditions that must be considered in the head, neck, and oral examination of the older adult are covered in Section 4. As for the domains of general medical health, psychologic, social, and physical function, a number of geriatric assessment models and definitions exist to evaluate status and are discussed in other sections of this book. When utilizing any assessment in the older population it needs to include evaluation of the caregiver and environmental concerns with an emphasis on the optimization of independent function supporting an increase in “active” life expectancy. In assessing functional health and dental service utilization in community-dwelling elderly, Dolan et al. (1998) concluded that even in a well-educated older population, impaired functional status is associated with lower levels of dental service utilization. To summarize, the geriatric assessment represents a “shift in focus” from a disease specific evaluation to a function-oriented evaluation, with the understanding that small changes in function can make a big difference in quality of life for patients and their caregivers.
This chapter presents the components of a “function-oriented assessment” as they apply to the older adult in the dental office setting. These components facilitate the establishment of a realistic dental treatment plan relative to the patients overall well-being and capacity. The following components will be addressed in order listed.
- Communication status: Ability to express, see, hear, and/or understand the provider or information presented.
- Physical status: Independence in Activities of Daily Living (ADLs) and Instrumental Activities of Daily Living (IADLs).
- Mobility status: Fine and gross motor abilities.
- Mental status: Memory and cognitive ability.
- Nutritional status: Malnutrition and dehydration.
- Social support: Ability to engage assistance needed.
- Medical status and consultation: Ability to medically tolerate the procedure.
Communication status
Communication is assessed when a patient first encounters the staff and strategies to establish and maintain effective communication are essential in developing a productive doctor–patient relationship. The older patient benefits tremendously from an environment that supports communication. This includes well-lit rooms, minimal extraneous noise, and minimal interruptions during conversation. The technique of establishing the initial relationship is intuitive and straightforward, but not always put into practice. Introduce yourself by name, address the patient by last name (until invited to do otherwise), and avoid “terms of endearment”such as “dear” or “sweetheart.” Sit at eye level facing the patient directly, speak slowly in a deep tone, ask open-ended questions, such as “What would you like me to do for you?” and allow ample time for the patient to answer. Whenever possible, try to communicate with the patient without your mask on. The mask muffles sounds, and also precludes the patient being able to see and/or read your lips. Rephrase and summarize to ensure the patient and provider have a similar understanding of the information exchanged. It should not be assumed that the geriatric patient needs sensory accommodations; however, they should be offered. Inquire about visual deficits and be prepared to offer and have available larger print material, including business cards, brochures, care instructions, and educational as well as reception room leisure material. For the hearing impaired individual, increase voice volume according to need and ensure extraneous noise is monitored. Generally, the hearing in one ear is better than the other. Ask the patient in which ear they have better hearing, and speak into that ear. Do not shout. Patients with hearing impairments often perceive speech sounds as muffled; shouting only makes the muffled sounds louder, not clearer. Also, facilitate and encourage the use of assistive devices, such as hearing aides and corrective eyewear, and be prepared to provide written copies of important discussions with contact information on a routine basis. (See Chapter 5 for additional discussion of sensory impairments.)
Physical status
Evaluation of the independence in homecare is evaluated with a review of the patient’s ability to perform ADLs and IADLs. There are six basic ADLs: dressing, eating, ambulation, toileting, transferring (being able to move from the bed to a chair), and hygiene (grooming and bathing). The higher function IADLs consist of the community interactions of shopping, housekeeping, accounting/managing finances (writing checks, balancing a checkbook), food preparation, telephone use, medication dosing, and transportation. Some type of disability is reported by approximately 40% of adults aged 65 and older, and, as shown in Fig. 6.1, the rate of limitations in activities among persons aged 85 and older is much higher than those for individuals aged 65–74 (US Department of Health and Human Services, 2011).
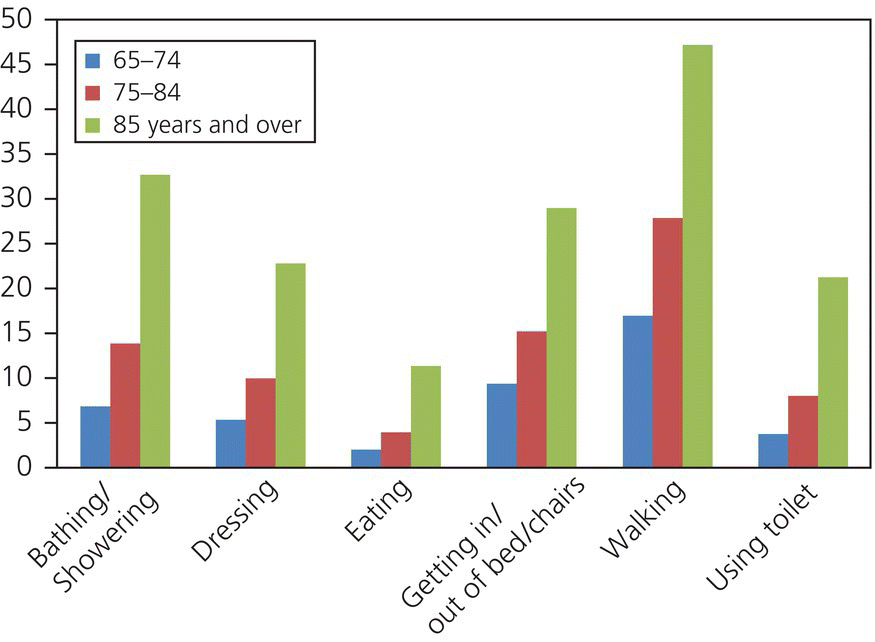
Figure 6.1 Percentage of persons with limitations in activities of daily living by age group: 2009.
From US Department of Health and Human Services (2011), p. 15.
A person’s ability to perform ADLs is very indicative of the prognosis for the progression of oral disease and the ability to maintain oral health. In addition to the impact of disabilities on social, psychologic, and interpersonal factors, diminishing ADLs impact a person’s ability to comply with treatment instructions and oral home care. Technical procedures may require in-office evaluation and modification due to physical and medical conditions and personal assistance may need to be identified to complete tasks. Patients can be assessed for “preclinical disabilities” (developing, but not “clinically evident” disability) by asking about perceived difficulties (Fried et al., 2001). Fried and colleagues concluded from their cross-sectional study that there appears to be a preclinical stage of physical disability which precedes onset of task difficulty (disability) (Fried et al., 2001). In a cross-sectional study of community-dwelling elderly women, these authors concluded that there appears to be a preclinical stage of physical disability that precedes the onset of task difficulty. Recognition of this stage provides a basis for identifying older adults at risk of becoming disabled and provides the practitioner with a window of opportunity to introduce devices and techniques, giving the patient the opportunity to accommodate before the onset of the disability. Limitations in the higher level IADLs can be used to identify subtle functional losses in otherwise high functioning patients. These subtle losses are frequently overlooked and undervalued in the complete geriatric assessment, but can provide valuable information on patient capacity and give indication of the overall treatment prognosis.
Mobility status
Evaluation of a person’s mobility is integral to the geriatric assessment and is assessed in the review of ADLs. However, falls and gait disorders, which are so common among the elderly, should be reviewed and monitored separately because they are closely related to greater functional impairment and are a major cause of patient morbidity and mortality (Centers for Disease Control):
- Approximately one-third of elderly fall each year representing a major cause of nursing home placement.
- One out of three adults aged 65 and older falls each year but less than half talk to their healthcare providers about it.
- Among older adults (those aged 65 and older), falls are the leading cause of injury death. They are also the most common cause of nonfatal injuries and hospital admissions for trauma.
- In 2010, 2.3 million nonfatal f/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


