Chapter 2
Palliative Care Dentistry
Michael Wiseman
Faculty of Dentistry, McGill University, Montreal, QC, Canada; Mount Sinai Hospital, Montreal, QC, Canada
Introduction
Palliative care dentistry focuses on the treatment of terminally ill patients in which the oral cavity is affected directly or indirectly by the illness and the principle is symptom relief (Wiseman, 2000). Palliative care involves more than simply treating the patient. Care is directed both to the patient and to their loved ones (Fig. 2.1). It must be noted that the interdisciplinary palliative care team should include a dentist, as patients often suffer from oral problems that other members of the team may not realize or know how to manage.
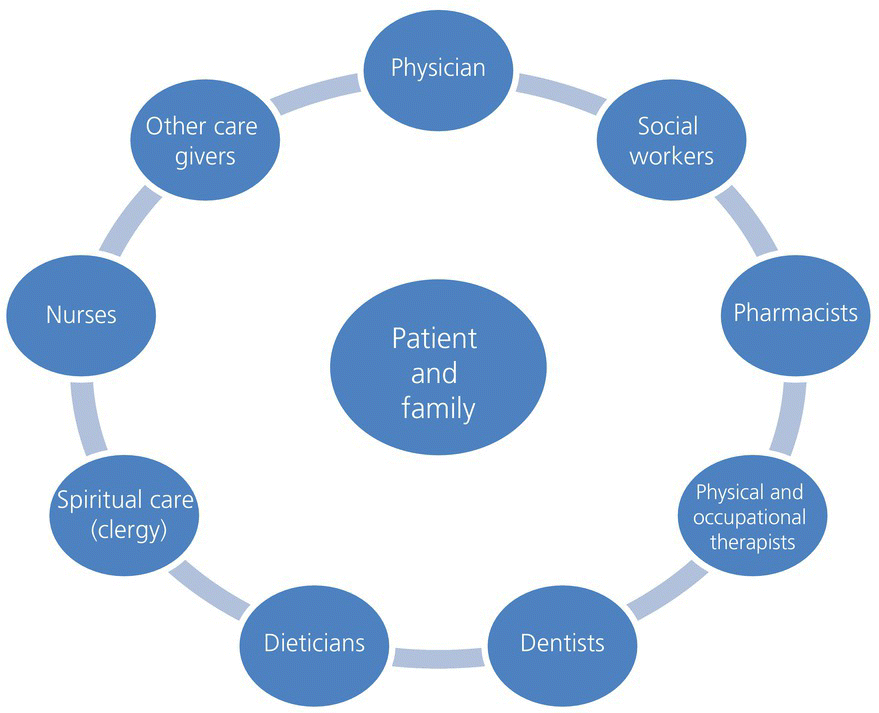
Figure 2.1 Palliative care team treating the patient and family.
The palliative care team must be careful not to become prognostic as to life expectancy, as this could influence the treatment choices for the patient, the family, and the dentist. When physicians were asked to predict life expectancy, physicians were only correct 20% of the time (Christakis & Lamont, 2000); this is important as an incorrect prognosis may lead the dentist to change from comfort-providing care to more advanced dental care. The dentist must always remember that the prime goal is comfort/pain control (“comfort care”). Although studies have indicated that palliative care patients have frequent oral problems, the inclusion of a dentist on the treating team is often overlooked. The oral cavity is vastly important to the palliative care patient. It provides an important route for nutrition, medications, speech, and affection by kissing (Table 2.1).
Table 2.1 Impact of oral problems in palliative care
| Physical impact | Social impact | Emotional impact | |
| Difficulty in eating/drinking | Difficult to speak | Emotional pain | |
| Taste disorders | Self-conscious of cancer | Fear of dying | |
| Denture instability | Embarrassed | Fear for family | |
| Xerostomia | Difficult to socialize | Depressed | |
| Fungal infections | Halitosis | Depression | |
| Viral infections Mouth ulcers Pain |
 |
Physically unable to display emotions; e.g., kiss |
|
The oral cascade of problems associated with palliative care is found in Fig. 2.2. As can be seen in this schematic, palliative care patients may have an array of problems, which will be discussed in the following sections.
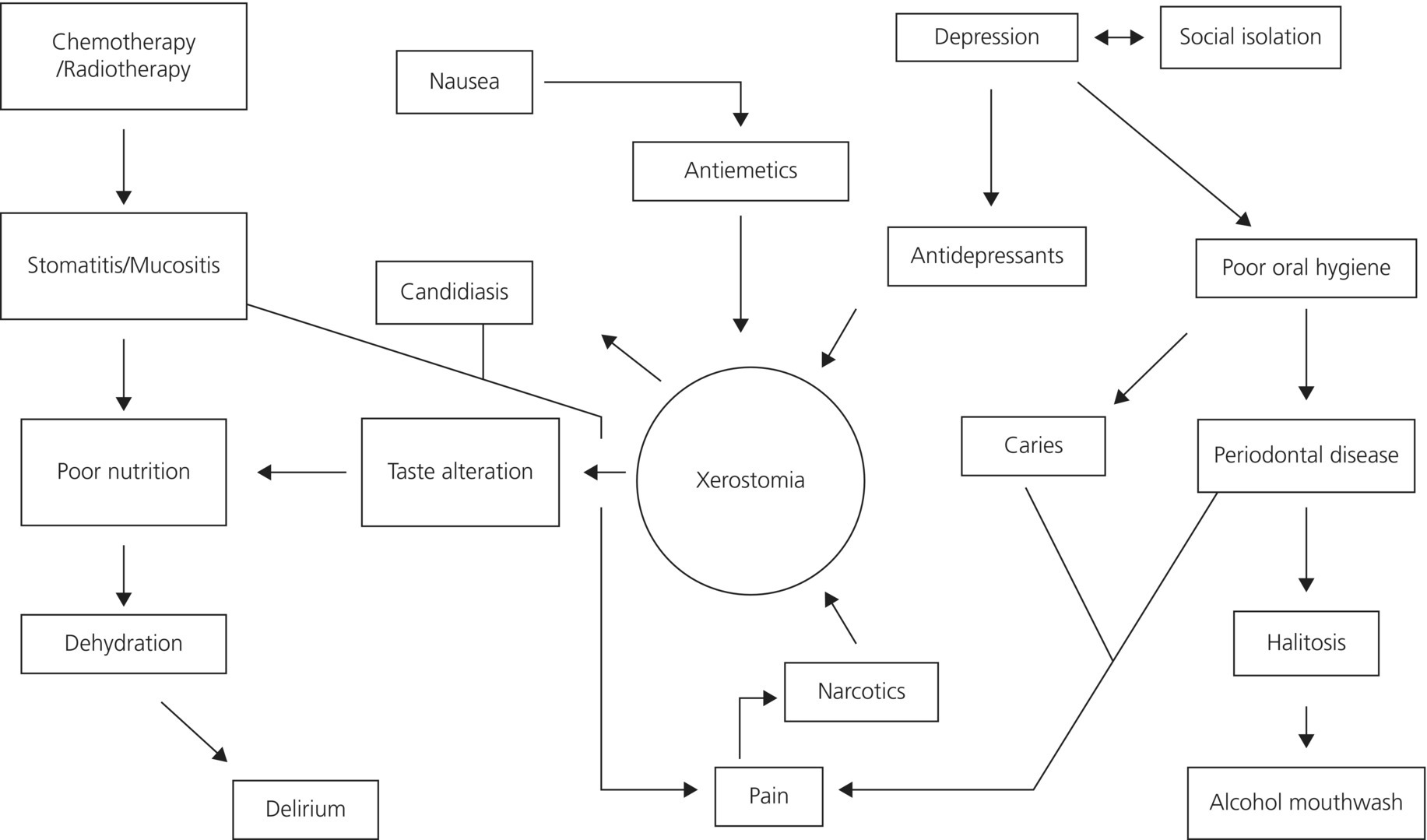
Figure 2.2 Oral problems in palliative care.
From Bruera & Neumann (1998).
Mucositis and stomatitis
As part of their treatments, patients may receive chemotherapy and/or radiotherapy. These treatments may be extended during their palliative care period in order to decrease pain or improve function. The oral cavity is affected by chemotherapy and radiotherapy at different rates. Chemotherapy affects mitotically active cells. Tissues of the oral cavity with high mitotic turnover are affected by such treatments, leading to atrophy of the tissues. Younger patients are of greater risk of atrophy of the tissues than older patients as they have a higher mitotic rate (Sonis et al., 1978). Radiotherapy affects the oral cavity by sclerosing the small vessels which vascularise the oral tissues. An index to grade the severity of mucositis exists as outlined in Box 2.1
A key element in mucositis/stomatitis prevention is to keep the mouth moist and clean. Oral care can actually decrease the rate of mucositis/stomatitis within cancer patients, probably by preventing or minimizing secondary infections (Sonis & Kunz, 1988).
Treatments for stomatitis/mucositis are primarily aimed at pain management. Failure to alleviate patient discomfort may lead to poor nutrition and hydration. This will further decrease the ability of the patient to recover. Topical anaesthetic agents are used to reduce pain. These include 2% viscous xylocaine, 10% xylocaine spray, 0.5–1.0% dyclonine hydrochloride, and 2% morphine. These agents except for morphine can be swished and swallowed. Patients must be instructed to expectorate the morphine. This can be modified by initially giving the patient saline to practice expectoration (Cerchietti, 2007).
Additional agents include sucralfate suspension, honey, benzydamine, and magic mouthwash. Sucralfate suspension as an agent in mucositis has had mixed results (Cengiz et al., 1999; Dodd et al., 2003). Its efficacy has to be evaluated on a case by case basis. Honey was found to effective in reducing mucositis; this may be due its natural bacteriostatic action (Biswal et al., 2003). Magic mouthwash is a generic term that describes a number of formulations of a palliative solution used to allay the pain and discomfort of mucositis. One study surveyed 40 institutions and found that most of the prescribed formulations included diphenhydramine, lidocaine, Maalox®/Mylanta®, nystatin, and corticosteroids (dexamethasone, hydrocortisone and prednisone). Some of the other formulations included the ingredients tetracycline, chlorhexidine, sucralfate, and Orabase®/Ulcerase® (Chan & Jenoffo, 2005). The author’s opinion is that treatment should be directed to the specific patient’s chief complaint and the patient should not be treated with ingredients not required to alleviate the oral problem. The formulation selected must be prepared specifically for the patient by a pharmacist according to the dentist’s prescription.
Nutrition
Oral problems can significantly affect a patient’s ability to eat. Furthermore as the patient functionally declines, he or she becomes more prone to an anorexia–cachexia syndrome (Yavuzsen et al., 2005). This syndrome involves the emaciation of the body of the patient. It is important that the dentist evaluates the patient’s oral cavity for any interference with mastication. Anorexia may be a result of some of the medications prescribed to the terminally ill patient; these include psychostimulents, antidepressants, and chemotherapy. Additional factors include depression, pain, stomatitis, dysphagia, nausea, and depression. It is estimated that 70% of terminally ill patients will have anorexia (Yavuzsen et al., 2005).
Suggestions that are nonpharmacologic include the provision of more frequent, small high-energy meals, attempting to make the presentation of food on the plate as appetizing as possible (use colorful foods, arrange in a visually pleasing way, accent with a piece of parsley/mint/flower), and simply asking the patient if there is anything that he or she may want to eat or drink. Pharmacologic agents to stimulate the appetite include megestrol and corticosteroids. These should be prescribed by the physician. Additionally as the patient’s mouth can be xerostomic, meals should be moist and soft so that it is easier for the patient to swallow. Using high-calorie shakes can promote nutrition, be gentle on the mucosa, and be appetizing for the patient. Some are available commercially (e.g., Ensure®) or they can be easily be prepared in a blender by family members or caregivers. The careful use of seasonings may enhance flavors and promote nutrition; some may have the potential to irritate the mucosa so use of seasonings should be monitored for patient tolerance.
Dysphagia
Dysphagia can be divided into two different phases; one being the oropharyngeal phase and the other the esophageal phase. Causes of dysphagia may involve one or both of these phases.
The oropharyngeal phase begins in the mouth. If the patient’s dentition is poor, mastication of the food bolus may not be adequate. The other components for the bolus preparation include adequate saliva production, sufficient muscular function, clear oral pathway, and freedom from pain such as ulcers, herpes, or fungi.
Inability to masticate foods can be the result of fewer teeth, poor fitting dentures, caries, or advanced periodontal disease. The palliative-care dentist should evaluate all patients for pain and function. Caries and periodontal disease should be treated. The choice of method to restore oral function should be based on prognostic longevity of the patient. For example, the patient may not be a good candidate for crowns or implants but may benefit from partial dentures.
Patients frequently do not have sufficient saliva production. This can be due to radiotherapy to the head and neck region leading to sclerosis of the salivary glands. Patients are often taking medications that cause xerostomia such as pain medications, antidepressants, and antihypertensives. (See Chapter 14 for further discussion of xerostomia.)
Muscular causes of dysphagia range from poorly functioning muscles of mastication, to poor tongue control. Causes for this include neurologic conditions such as Parkinson’s disease, cerebral vascular accident, or amyotrophic lateral sclerosis; or nerve damage (cranial nerves V, VII, or XII) due to surgical or radiation treatment of intraoral tumors. Patients with poor tongue control will lack the ability to propel the food posteriorly to the oral pharynx.
Pain from fungal, herpes, or mucositis can lead to oral pain which will affect the patient’s ability to swallow food. (See Stomatitis and mucositis section, earlier in this chapter.)
The esophageal component of swallowing can be inhibited by a physical obstruction from a tumor, or esophageal constrictions caused by radio/surgical therapy of a tumor. Additionally neurologic damage can lead to the lack of function.
Nausea and vomiting
Nausea and vomiting are common side effects of chemotherapy. Additionally, vomiting may be associated with bowel obstruction, constipation, electrolyte imbalance, autonomic failure, peptic ulcer disease, malignancy-associated gastroparesis, metabolic abnormalities, brain metastasis-associated increased intracranial pressure, and drug use such as opioids. Most patients will have at least two of these contributing factors as a causative factor. Chronic vomiting can have oral sequellae, and is discussed in greater detail later in the chapter. The acid content of vomit can erode tooth enamel and cause sensitivity. It is important to recommend the use of fluoride rinses and to prescribe fluoride varnish applications to counteract the erosive effect of the dentition’s chronic exposure to vomit in the oral cavity. Anticholinergic agents such as scopolamine are used to alleviate vomiting and nausea. It is administered transdermally (1.5 mg every 72 h), and its primary side effects are drowsiness, xerostomia, and visual disturbances (Clissold & Heel, 1985). Dexamethasone, a glucocorticoid, is a good antiemetic (0.5–9.0 mg/day in divided doses every 6–12 h). Its side effects include insomnia, mood swings, and increased energy (Basch et al., 2011). Serotonin receptor antagonists, also called 5-HT3 (type three 5-hydroxytryptamine) receptor antagonists, are excellent antiemmetics with few side effects. Agents of this class include ondansetron (Zofran®) given at a dose of 8 mg twice daily.
Nonpharmacologic agents/methods used to control nausea and vomiting include ginger and acupuncture. In a study of 576 patients undergoing chemotherapy for breast cancer, ginger reduced nausea during the first day of chemotherapy (Ryan et al., 2012). Some studies indicate that acupressure/acupuncture may be of benefit to patients (Ezzo et al., 2005). This study did not involve an appropriate control, and the authors concluded that more studies would have to be done to verify its clinical relevance.
Prolonged vomiting may also lead to dehydration. The palliative team may suggest to replace fluids by parenteral routes such as intravenous or subcutaneous routes. Once the patient is able to tolerate oral fluids, they should be encouraged to drink. It is important for the palliative team to recognize that possible causes are hypercalcemia due to bone metastasis and the use of bisphosphonates may alleviate this cause.
The major oral problem associated with vomiting and nausea is that vomiting erodes teeth and increases the severity of mucositis and stomatitis. Vomiting robs the body of vital nutrients needed for repair. Nausea can prevent patients from wearing dentures, which are important for mastication and, perhaps of greater importance, their quality of life by affecting their social interactions due to vanity with loved ones. The use of antiemetics helps prevent this pathology but has a major side effect of xerostomia and possible tardive dyskinesia. Tardive dyskinesia is the repetitive muscular movements often seen as either frequent tongue, lip, or jaw movements. The use of a fluoride varnish or rinse will help protect the teeth. Oral care must be instituted as a strict regimen even though the patient may be nauseous. The use of a smaller toothbrush (child size) may help prevent triggering the nausea as its smaller size may not illicit a gagging reflex.
Delirium
Delirium is defined as a quick-onset change in cognitive condition and is very common in palliative care patients. They will exhibit cognitive difficulties, varying levels of consciousness, and changes in their sleep/wake cycle, and have varying degrees of agitation (Pereira et al., 1997). Delirium can be caused by the accumulation of opioid metabolites and other drugs. Patients that are dehydrated due to problems in swallowing, nausea and vomiting, or inability to eat/drink from stomatitis/mucositis will experience decreased urine output and, thus, decreased drug clearance. This can lead to certain drugs to have extended half-lives and increased toxicity. Patients do not require large volumes of fluids to maintain urine output, volumes of ≤1 L/day should be sufficient to maintain urine flow and electrolyte balance (Bruera et al., 1996).
Xerostomia and salivary gland hypofunction
Xerostomia and salivary gland hypofunction are terms that are easily confused. Xerostomia is the subjective sense of oral dryness. The oral cavity may appear to be moist; however, if the patient subjectively states that his or her mouth is dry, then he or she is xerostomic. Salivary gland hypofunction is defined by a quantitative flow rate of saliva less than 0.7 ml/min (Navazesh, 2003). It is more practical in dealing with palliative care patients to utilize the xerostomia definition as the aim of care is comfort measures. Xerostomia is one of the most frequent symptoms associated with terminally ill patients (Jobbins et al., 1992). Medication usage is the most common cause of xerostomia. One study indicated that in patients taking 4–5 medications daily, the incidence of xerostomia was 50% (Sreebny et al., 1989). Medications for pain management, antidepressants, diuretics, and antiemetics frequently prescribed to palliative care patients are among the majo/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


