Chapter 11
Periodontal Disease
Saroj Gupta
Department of Periodontics, University of Maryland, Baltimore, MD, USA
Introduction
This chapter will review periodontal disease, one of the two most prevalent diseases of the oral cavity, the other being caries. We will address many of the facts and myths associated with periodontal disease.
Older people are increasingly retaining their natural teeth, but are at higher risk of oral disease accompanying increased longevity, with potential impact on quality of life. Maintenance of oral health may not have been a priority among elders for many reasons, including lack of coverage from Medicare (Medicare does not cover dental services for any elders) and Medicaid (coverage for adults varies from state to state, is limited to low-income individuals, and often provides no or minimal dental services for adults), or coverage from other third-party sources. Even private dental insurance often does not extend into retirement As a result of limited or nonexisting access to dental services, adults often resort to a hospital emergency room for their dental care, or neglect it entirely.
Throughout the life span, teeth remain at risk for the two most prevalent oral diseases – dental caries and periodontal disease. (See Chapter 10 for a discussion of root caries.) Older adults are at risk for new and recurrent decay that is untreated in approximately 30% of dentate adults. They are at increased risk for root caries because of both increased gingival (i.e., gum) recession that exposes root surfaces and increased use of medications that produce xerostomia (i.e., dry mouth). Approximately 50% of persons aged over 75 years have root caries affecting at least one tooth. Approximately 25% of older adults have loss of tooth-supporting structures because of advanced periodontal disease. Without early prevention and control interventions, these progressive conditions can necessitate extensive treatment to treat and prevent infection and restore function (CDC, 2003).
Self-ratings of health have been associated with functional ability. These associations suggest that older persons who report poorer general health are at increased risk for limited dexterity, mobility, and tolerance of stress; such factors can compromise abilities to maintain oral hygiene, visit a dental office, or tolerate treatment. These persons likely will need caregiver assistance and innovative strategies to maintain daily self-care, obtain regular oral assessments, and receive primary and secondary prevention services (CDC, 2003). Older persons usually require coordinated health care offered by different healthcare professionals due to high prevalence of complex chronic disease and psychologic disorders during aging, including depression, frailty, diabetes, cardiovascular and neurodegenerative disease (Fig. 11.1)
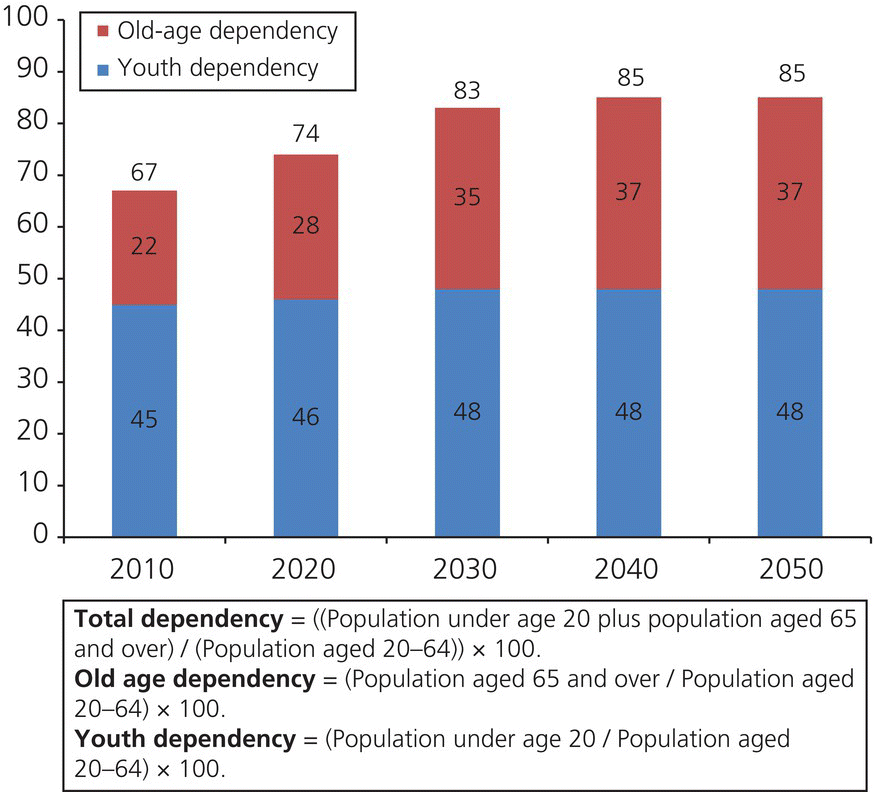
Figure 11.1 Dependency ratios for the USA, 2010–2050.
From US Census Bureau (Vincent & Velkoff, 2010).
Compared with younger persons, the current cohort of older adults likely experienced higher rates of dental caries and tooth extraction as young adults and is more likely to have lost all their teeth. Patients with a history of smoking comprise approximately half of all cases of periodontal disease in the USA. The higher prevalence of tooth loss among smokers may be closely associated with the well-recognized adverse effects of cigarette smoking (Van Dyke & Sheilesh, 2005).
Epidemiology of periodontal disease
Periodontal disease has a higher prevalence in older adults than any other age group. However, periodontal disease is not a direct result of aging. The old beliefs concerning periodontal disease were: (i) everyone was equally susceptible to periodontal disease; (ii) gingivitis progresses to periodontitis with resulting bone and tooth loss; and (iii) susceptibility to periodontitis increased with age (Burt, 2005). Epidemiologic studies of periodontitis have disproved all of these beliefs. Studies have shown that the majority of adult populations are affected by moderate periodontitis, but that only a small proportion, 5–15%, of any population suffers from severe generalized periodontitis, with these numbers holding true among both well-treated and underserved populations. The individuals most susceptible to periodontitis had signs dating back to teenage and adolescent years (Burt, 2005). The belief that gingivitis progresses to periodontitis has been disproved since the 1980s; a notable 3-year longitudinal study of patients with gingivitis showed that most of the patients were resistant to further clinical attachment loss (CAL) and development of periodontitis (Burt, 2005; Listgarten et al., 1985).
The role of periodontal disease in oral health/overall health
Periodontal disease is an inflammatory disease caused by gram-negative anaerobic bacteria from dental plaque displaying virulent properties and increasing pro-inflammatory cytokines. Periodontal disease progresses to periodontitis when the inflammation extends to the periodontal ligament and alveolar bone which lead to loss or recession of gingival tissue, decrease in alveolar bone mass, tooth mobility/tooth loss, and potentially edentulism (Chung et al., 2011).
These pro-inflammatory cytokines, notably tumor necrosis factor (TNF), interleukin-1 beta (IL-1β), and interleukin-6 (IL-6), associated with periodontal disease are noteworthy because they also have associations with many other chronic inflammatory diseases such as rheumatoid arthritis, osteoporosis, myeloma, type II diabetes and atherosclerosis; all of these diseases and conditions have been traced back to the same or similar etiologic onset of the inflammation (Chung et al., 2011). Further, Actinobacillus actinomycetemcomitans, Porphyromonas gingivalis and other bacteria originating from plaque in the oral cavity can travel to other areas of the body and have been linked to infections of the endocardium, meninges, mediastinum, vertebrae, hepatobiliary system, lungs, urinary tract, and prosthetic joints (Dumitrescu, 2010). Plaque bacteria have been associated with systemic implications in the cardiovascular and nervous systems. For the dental examiner it is important to know and understand this information in order to comprehensively treat the patient. Many of the chronic inflammatory diseases have established associations with oral inflammation and thus these associations have placed the dental examiner in an important position to identify possible systemic diseases from a routine oral exam. If other systemic diseases are suspected the dental clinician can then work with the medical profession to discuss the findings and determine the best treatment plan for the patient.
Senescence of tissue
An etiologic component attributed to the higher prevalence of periodontal disease in older adults is a result of biologic aging or senescence of the periodontium. All tissues undergo certain changes as a result of aging: reduction in vascularity, elasticity, and reparative capacity are some of the common manifestations of aging, generally noticed in tissue. Periodontal tissues are no exception to this rule and may show signs of atrophy as age advances.
Gingival fibroblasts (GF) are the main cellular component responsible for synthesizing periodontium. The influences of oral bacteria on the GF are an important factor in periodontal disease and will be discussed in more detail later in the chapter. But studies have shown that aging GFs have an increased rate of intracellular phagocytosis, throwing off the homeostasis balance between degradation and synthesis, and leading up to a fivefold decrease in collagen production. In addition, aging GFs have increased DNA methylation, which reduces mRNA levels and further decreases collagen synthesis (Huttner et al., 2009). The decreased collagen synthesis leads to dekeratinization and overall weakening of the gingiva. The oral epithelium thins and forms irregularly, which decreases the physical barrier ability of the epithelium to keep out pathogenic bacteria (Huttner et al., 2009). The periodontal ligament, anchoring tooth to alveolar bone and serving as cushion during chewing, is composed of many types of cells that differentiate to affect the entire periodontium. Aging periodontal ligaments show decreased number of cellular components and, like the gingival epithelium, its structure becomes irregular. Periodontal ligament cells differentiate into osteoblasts and osteoclasts involved in alveolar bone homeostasis. With age there is reduced osteoblast chemotaxis and osteoclast differentiation to osteoblast resulting in decreased alveolar bone density, an indicator of periodontal disease in itself (Huttner et al., 2009). Of note in aging periodontal ligaments is the large amount of cytokines produced in response to mechanical stress, such as prostaglandin E2 (PGE2), IL-1β, and plasminogen activator. As periodontal disease is an inflammatory disease in response to cytokines caused by plaque biofilm bacteria, this is a significant observation.
Healthy gingiva of younger adults has been associated with simple, supragingival plaque biofilm (1–20 cell layers), and mainly consists of gram-positive, aerobic, and facultative aerobic bacteria with very few gram-negative bacteria. In comparison, older adults with no history of gingivitis displaying overall healthy oral conditions show an increased number of gram-negative bacteria directly related to inflammatory responses (Dumitrescu, 2010). Several of these gram-negative bacteria are associated with gingivitis and periodontitis including P. gingivalis and Fusobacterium nucleatum. The presence of these anaerobes in older adults is believed to be a result of aging and the body’s natural decline in immune responses leading to a greater susceptibility to periodontal disease.
Identifying periodontal disease
Periodontal disease is an inflammatory disease with clear visual signs. When triaging the patient, the examiner needs to be able to identify visual differences between healthy versus diseased tissue. The color of normal, healthy soft tissues of the oral cavity, including the gingiva, tongue, and palate, should be coral-pink and, depending on the complexion of the individual, may contain areas of melanin pigmentation. The texture of the gingiva should be smooth or have a stippling consistency like the rind of an orange. A thorough clinical exam also includes checking for ulcers, lesions, cancers, or tumors of the oral cavity as well as the contours of the underlying bone. It is important to remember that older individuals with prior bone loss that have undergone periodontal therapy may have a significant amount of recession but maintain healthy gingiva, i.e, probing depths (PDs) of 1–3 mm, with no bleeding on probing (BOP).
Unhealthy gingiva displaying gingivitis is red, inflamed, and swollen, sensitive to touch, and bleeds on touching or probing (Figs 11.2 & 11.3). Patients presenting with periodonta/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


