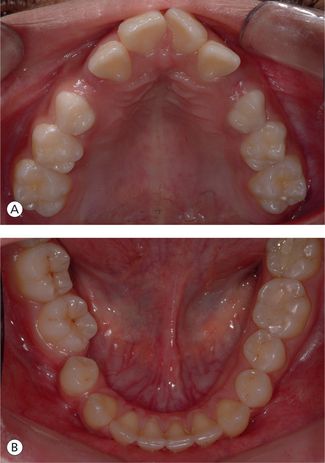
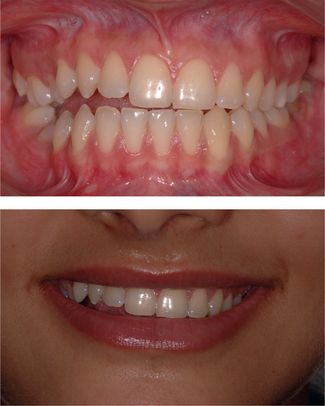
Transverse discrepancies
Transverse discrepancies warrant special consideration in orthodontic diagnosis and treatment planning. Determination of the underlying cause of the asymmetric or symmetric transverse problem must be an important ingredient in the process of formulation of an appropriate treatment plan. Depending upon the structures involved, these problems may be primarily dental, skeletal, functional in origin or may even have combination of these factors present. It is equally important to determine the relationship of the transverse discrepancy with the sagittal and vertical problems, which often have a significant impact on designing a treatment strategy. The management of transverse discrepancies has been universally recognized as one of the most challenging aspects of orthodontic therapy, and this chapter comprehensively deals with the development, differential diagnosis and treatment of such problems.
Asymmetry in craniofacial morphology can be recognized as differences in the size or relationship of the right and left sides. This may be the result of imbalances in the individual position and form of teeth, variation in the position of bones of the craniofacial complex, and it may also be limited to the overlying soft tissues. It is recognized that the human face displays bilateral symmetry exhibiting mirror image characteristics between right and left halves. Is this perfect bilateral dentofacial or craniofacial symmetry predominantly a theoretical concept that seldom exists? Due to large biological variations, either inherent in the developmental process or caused by environmental disturbances, such symmetry is rarely encountered. Certain degree of asymmetry goes unnoticed and is often considered normal; however, the point at which this mild transverse discrepancy becomes abnormal cannot be easily defined, as it is influenced by the clinician’s understanding of asymmetry and the patients’ perception of imbalance.
As patients view themselves from the frontal perspective enabling them to compare right and left sides of the face, contemporary orthodontic diagnosis and treatment planning should incorporate identification of transverse problems and achievement of symmetric results with appropriate mechanics. Though diagnosis of certain craniofacial structural variations in transverse dimension is quite simple, some underlying asymmetries may be masked by dental compensations. These undiagnosed transverse discrepancies usually become apparent as treatment progresses, often leading to increased treatment duration, change in treatment plan or compromised result. The management of transverse discrepancies has been universally recognized as one of the most challenging aspects of orthodontic therapy, and this chapter comprehensively deals with the development, differential diagnosis and treatment of such problems.
Development of a Transverse Problem
Dentofacial asymmetric relationships can result mainly from genetic alterations in the mechanism that is responsible to establish symmetry, and various environmental factors producing differences in right and left halves.1,2 Some of the most severe facial asymmetries are observed in individuals with craniofacial syndromes. Hemifacial microsomia, clefting syndromes and craniosynostoses are some of the examples characterized by significant facial asymmetries. Some clefts of the lip and/or palate are genetically influenced leading to significant facial abnormality associated with collapse of the maxillary dental arch.2 In certain situations, although some of the facial imbalance is found primarily in the soft tissue, skeletal contributions can be significant. The glenoid fossa position is determined by the growth of the cranial base, and any variation in this growth leads to asymmetrical positions of the glenoid fossae, producing rotation of the mandible with respect to the maxilla. Under these circumstances, even if the maxilla and the mandible are not asymmetric in form, the resultant occlusion exhibits a Class III relationship on the side of the anteriorly positioned fossa and a Class I relationship on the contralateral side. In the absence of dental compensations, this often produces midline deviations. Even if the glenoid fossae are symmetrically positioned, the maxilla can undergo certain degree of rotational growth change relative to the cranial base with resultant asymmetric occlusal relationship.
In addition to asymmetric mandibular positioning, morphological variations between the right and left sides of the mandible like differences in the length of the body of the mandible or height of the developing ramus, can lead to asymmetries. Moulding of the parietal and facial bones due to intrauterine pressure during pregnancy and significant pressure in the birth canal during parturition can result in facial asymmetry. These changes are usually considered as transient which undergo rapid restoration of the normal skull relationships within a few weeks to several months.3
Trauma and/or infection within the temperomandibular joint can cause ankylosis of the condyle to the temporal bone.4 The loss of muscle function and tone as a result of damage to a nerve may indirectly lead to asymmetry. Various pathological conditions, not necessarily congenital in nature, cause craniofacial asymmetries. Osteochondroma of the mandibular condyle leads to facial asymmetry, mandibular deviation and open bite on the involved side.5
Asymmetries within the maxillary or mandibular arch lead to significant differences in the interarch relationships on the right and left sides. When primary molars are ankylosed, the adjacent teeth continue to erupt as a part of dentoalveolar development and appear to tip over the crown of the ankylosed tooth. This results in a loss of space and asymmetric axial inclinations of the adjacent teeth and subsequent asymmetric molar occlusion. Since the leeway space is larger in the mandibular arch than in the maxillary arch, a combination of permanent molar drift into the leeway space and differential growth of the mandible relative to the maxilla allows spontaneous correction of the end-to-end relationship into a normal molar relationship. Any unilateral partial loss of the leeway space results in an asymmetric molar relationship. Such molar occlusion is often encountered in patients with arch length loss as a result of interproximal caries or premature loss of a primary or permanent tooth.
Congenitally missing teeth, supernumerary teeth or ectopic eruptions are common causes for developing occlusal asymmetries. Asymmetries in archform, which can also be characterized by midline discrepancies, are often produced by habits. Transverse discrepancies are also caused by functional mandibular shifts due to centric prematurities leading to a lateral mandibular displacement in habitual occlusion. Temporomandibular joint disorders like articular disc dislocation or fossae changes are often associated with asymmetries involving off-centred midline.
Diagnosis of Transverse Problems
Contemporary orthodontic diagnostic process must involve an assessment of problems in the transverse dimension. Minor asymmetries that are often neglected, or underlying asymmetries that are masked by dental compensations, if undiagnosed at the beginning of treatment, usually become apparent as treatment progresses, especially during the finishing stage. This prolongs the treatment duration, causes certain alterations or changes in treatment direction, or it will ultimately leave the patient with a compromised result. To avoid this untoward situation, every clinician should make a conscious effort to assess dentofacial abnormalities in the transverse plane.
Types of transverse discrepancies
Facial asymmetries or transverse discrepancies can be broadly grouped into following categories:
Dental asymmetries
Transverse discrepancies that are dental in nature are mainly caused by local factors like premature loss of deciduous teeth, congenitally missing single tooth or group of teeth and certain habits like thumb sucking or tongue thrusting. These dental asymmetries essentially involve midline deviations, asymmetric posterior tooth positions, asymmetric archforms and diverging occlusal planes.
Midline deviations: Quite often, most individuals presenting for orthodontic treatment do not exhibit coincident maxillary and/or mandibular dental midlines with each other or with the facial midline. This maybe because of displacement or distortation of the maxillary or mandibular dental arches, tooth rotations, tooth size discrepancies, asymmetric crowding or spacing etc.6,7 Midline deviations certainly warrant special consideration in the orthodontic diagnosis and treatment planning. However, aesthetic acceptability of dental midline discrepancies depends on individual factors, including the transverse discrepancies associated with other facial midline structures. It has been found that overjet and dental crowding or spacing were considered to be more significant factors than midline deviations in determining self-satisfaction with dental appearance.8 In contrast, another study found that symmetry was one of the most important factors in defining an attractive smile.9 Generally, a dental midline deviation of 2 mm or more is considered to be easily detectable by most individuals, and therefore, warrants its consideration in treatment planning process. Individuals with midline discrepancies present with a variety of clinical situations where maxillary midline is coincident with facial midline and the mandibular dental midline is shifted either to the left or right side; mandibular midline is normally positioned, but the maxillary midline is deviated to the left or right sides or it could be the combination of both (Fig 5.1).
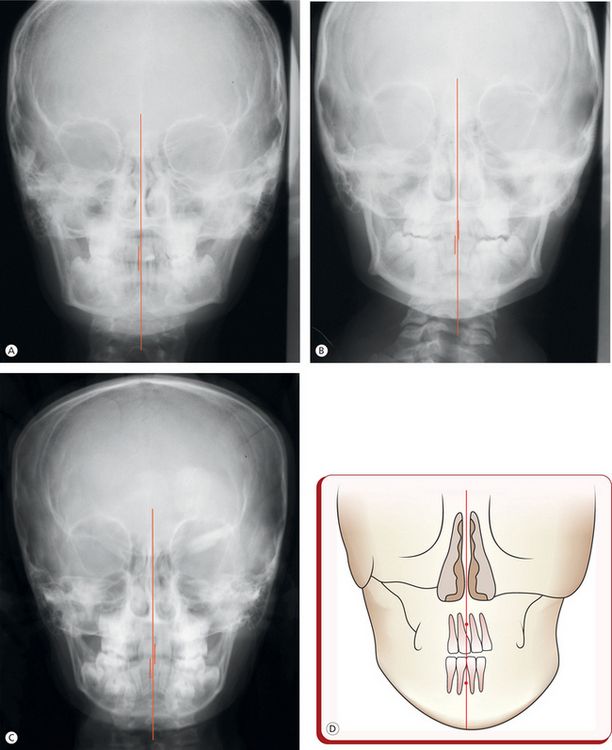
Figure 5.1 Variations in the maxillary and mandibular dental midlines. (A) Maxillary and mandibular dental midlines are coincident but are deviated to the right side when related to the midsagittal reference plane. (B) Maxillary dental midline is coincident with the midsagittal plane while the mandibular dental midline is shifted to the right side. (C) Maxillary dental midline deviated to the left and the mandibular to the right side of the midsagittal plane. (D) Maxillary dental midline deviated to the left without apical base discrepancy.
Posterior tooth position: The buccal occlusion on the right and left sides should be evaluated, and the individual tooth positions with respect to their mesiodistal and buccolingual inclinations and rotation be properly assessed to determine their contribution to the development of a problem. Although abnormal mesiodistal axial inclinations of the posterior teeth are sagittal discrepancies, but when assessed with respect to the opposite side, they result in an asymmetric buccal occlusion. In individuals with normal growth, the maxillary molars have a distal axial inclination. With continued favourable growth of the facial complex, the molar will erupt with a more mesial axial inclination.10 Abnormalities in buccolingual axial inclinations of the posterior teeth may be present in individuals with or without posterior crossbite. Their proper assessment helps the clinician to differentiate dental problems from the skeletal ones. Rotations of the posterior teeth form an important part of transverse dental problems. Mesial migration with forward tipping of the permanent molar is usually accompanied by rotation (mesialin) of the tooth, leading to a significant space loss in the posterior dental arch. This results in Class II molar relationship on the affected side.
Archform distortions: Abnormal positions of the posterior teeth, either in the buccal or the lingual side, symmetrically or asymmetrically, with or without crossbite, result in deviations from normal configuration of the arch form (Fig 5.2). These distorted archforms are either because of displacement of a single or group of teeth or because of an underlying skeletal discrepancy, and it is critical to establish differential diagnosis. Since skeletal discrepancies contributing to such problems is common, it is important to understand the role of buccolingual axial inclination compensations in the dental arch that occur naturally to mask the discrepancy. It should be recognized that natural compensation in the form of changes in the buccolingual axial inclinations of the teeth, influencing the arch width, minimizes the magnitude of a problem and makes it to appear less severe clinically. It has been observed that some malocclusions involving transverse component, presenting with a centric relation-centric occlusion discrepancy, are symmetric in centric relation and asymmetric in centric occlusion.11 Therefore, an assessment of occlusion in centric relation and centric occlusion is the key to differentially diagnose these conditions.
Occlusal plane considerations: Occlusal plane is the line along which the teeth function and is considered to be an important reference plane to achieve functional balance. Occlusal plane, when viewed from the frontal aspect, is an expression of vertical position of teeth on right and left sides of dental arch. Therefore, when vertical relationship of teeth along this plane on one side of the arch is assessed with respect to the other, it forms an integral part of transverse assessment to determine the cant of occlusal plane. As most malocclusions are often the result of a dysplasia in the vertical dimension, every clinician should make an effort to better evaluate function as relates to vertical growth. Occlusal plane changes in transverse dimension are true reflection of relative vertical heights of the segments of teeth on the left and right sides, as a result of differential vertical dentoalveolar growth, vertical eruption of teeth on one side of the arch or underlying skeletal discrepancy (Fig 5.3). Canted occlusal plane may involve both upper and lower arches; however, in majority of the patients, the problem is limited to either the upper or lower arch or isolated to anterior or posterior segment.
Skeletal transverse discrepancies: Transverse skeletal discrepancies may involve either the maxilla or the mandible or a combination of both. The maxillary problems in a transverse dimension usually result from a symmetric or an asymmetric constriction of the basal arch, with or without posterior crossbite depending upon the severity of the condition. The maxilla can undergo some rotational changes relative to the cranial base producing an asymmetric occlusal relationship (Fig 5.4A).
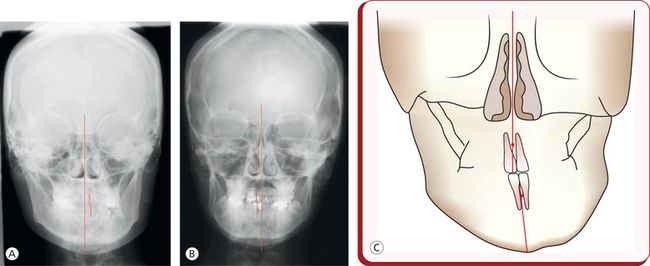
Figure 5.4 Transverse skeletal problems. (A) Maxillary and mandibular asymmetry exhibiting symphysis deviation to the left and canted occlusal plane. (B) Mandibular asymmetry without occlusal plane distortion. (C) Dental midlines coincident. Apical base discrepancy is masked by compensatory tipping of the maxillary and mandibular incisors.
Most people have some facial asymmetry, and asymmetric development of the jaws, though rare, does produce transverse problems. Severe skeletal problems in a transverse dimension are often produced by some congenital anomalies like facial clefts, and trauma or infection. Patients with cleft lip and palate pose a unique problem, requiring extensive and prolonged orthodontic care. Individuals with a lateral cleft typically exhibit lingually collapsed maxillary posterior segments and labially displaced premaxillary segment, leading to extreme distortion of the maxilla. The surgical repair of the lip and palate carried out an early stage for aesthetic and functional reasons often results into some degree of lateral constriction of the palate and constriction across anterior segment of the maxillary arch in the early and late mixed dentition.
Transverse mandibular problems result from both asymmetric positioning and asymmetric morphology of the mandible (Fig 5.4B and C). An abnormal growth of the cranial base may lead to asymmetries in the positions of the glenoid fossae and subsequent rotation of the mandible relative to the maxilla. Mandibular asymmetries significantly contribute to the facial asymmetries, and it is important for the clinician to identify whether a resultant problem is due to a congenital anomaly or a trauma.
There is an absence of tissue in the mandibular condylar region in patients with a congenital anomaly of hemifacial microsomia with a diminished growth on the affected side leading to asymmetry. An injury to the mandibular condyle often produces scarring and fibrosis of the affected area, leading to an apparently similar situation of slower growth and resultant asymmetry. Hemifacial microsomia is characterized by the absence of growth potential due to a lack of tissue; while in a posttraumatic situation, the fibrotic tissue causes restriction of condylar movement and subsequent interference with normal expression of growth, but there is potential for normal growth. In addition to deficient condylar growth, mandibulofacial asymmetries can also be caused by excessive growth of the mandibular condyle on one side. Unilateral overgrowth of the mandibular condyle may be expressed as an enlargement of the whole half of the mandible, with associated prognathism. The gonial and ramal overgrowth hypertrophy may manifest itself as a more localized enlargement of the mandible.
Certain infections and inflammations, especially the ones that originate from middle ear, often leading to ankylosis of the temporomandibular joint were earlier regarded as important factors contributing to the development of mandibulofacial transverse problems. However, such incidences have significantly reduced owing to advances in diagnostic and therapeutic medicine.
Considerable changes in mandibular function and structure as a result of destruction of the surfaces of the temporomandibular joint and the disk are commonly observed in children suffering from rheumatoid arthritis.
Muscular asymmetries
Any deviation from normal muscle function plays an important role in the development of skeletal and dental transverse discrepancies.12 Muscular asymmetry, as commonly observed in hemifacial atrophy or cerebral palsy is one of the factors responsible for facial disproportions and midline discrepancies.13 Sometime facial transverse problems are confined mainly to the soft tissues due to disproportionate muscle size as seen in masseter muscle hypertrophy.14
Functional transverse problems
Functional transverse discrepancies are often caused by deflections of the mandible due to occlusal interferences.7,12 During mandibular closure, the abnormal initial tooth contact in centric relation results in subsequent mandibular displacement laterally or anteroposteriorly, leading to asymmetric maxillomandibular relationship (Fig 5.5). The functional mandibular deviations are caused by a malposed tooth or by a symmetric or an asymmetric constricted maxillary arch.
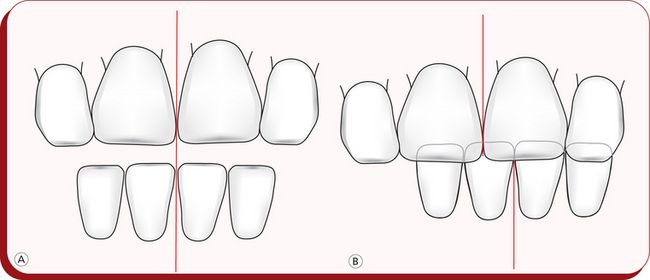
Figure 5.5 Mandibular functional shift. (A) Transverse incisor relationship at rest. (B) Incisor relationship in habitual occlusion.
Sometimes temporomandibular joint disorders, especially an anterior disc displacement without reduction, may lead to midline discrepancy during opening as the displaced disc interferes with the normal forward mandibular translation as on the unaffected side.
Assessment of transverse problems
The diagnosis of transverse discrepancies should be accomplished by a thorough clinical examination and an analysis of various diagnostic records to determine the extent of involvement of dental, skeletal, soft tissue and functional components. The goal of these diagnostic procedures is to identify the causative factor and determine the location and extent of the transverse problem. The differential diagnosis of transverse discrepancies is critical to formulate proper treatment plan.
Clinical examination: One of the challenges in treatment planning and treatment of transverse problems is the proper alignment of maxillary and mandibular dental midlines. Not only should they be coincident with each other, but they must also exhibit a definite relationship with the face. The clinical examination is of vital importance as it enables the clinician to carry out dynamic assessment of these discrepancies. To establish differential diagnosis of midline discrepancies, the dental midlines should be evaluated in different mandibular positions: mouth open; in centric relation; at initial teeth contact and in centric occlusion. Functional transverse problems due to occlusal interferences lead to a mandibular functional shift following initial tooth contact. These functional mandibular shifts may accentuate or mask the midline discrepancy depending upon the direction of shift – in the same or opposite direction of the dental or skeletal discrepancy. Maxillary and mandibular dental arches should be thoroughly examined for arch symmetry and their coordination and for a more localized factor like malposed or displaced tooth. Clinical assessment of the patient must involve the examination of temporomandibular joint and associated musculature since certain temporomandibular joint disorders causing interferences in normal mandibular translation result in mandibular deviations.
The facial midline is an important component of facial aesthetics, and its proper clinical evaluation must become an integral part of the clinical examination. A common procedure adopted by most clinicians to evaluate the facial midline is to use a dental instrument handle/shaft or a piece of dental floss to connect soft tissue points at nasion, subnasale and pogonion. The author does not consider this approach reliable, since it is difficult to accurately identify these points; and in the presence of mandibular asymmetry, these points would not correspond. For this reason, the philtrum is considered to be a reliable midline structure, and in most instances, can be used as the basis for midline assessment.15 Another approach is to observe the distance between the canine or first premolar and the corner of the mouth.12 In the presence of midline deviation, the patient will notice unequal amount of tooth exposure on the right and left side. In clinical examination, the clinician must record the extent to which the maxillary midline is deviated from the facial soft tissue midline, since the orthodontic treatment goal is to position the two midlines and the mandibular midline so they are aligned with each other.
Radiographic examination: While clinical examination is an important step in diagnostic procedures for the orthodontist to assess dynamic relationships of orofacial complex, certain radiographic projections provide valuable information to differentiate between various types of transverse discrepancies. A number of radiographic projections are available for accurate identification of the location and aetiopathology of transverse problems.
The lateral cephalometric radiograph provides little useful information on transverse discrepancies; however, it is a valuable diagnostic tool to locate and quantify associated vertical and sagittal problems in the craniofacial complex. To certain extent, this view enables the clinician to assess ramal height, gonial angle and mandibular length, but due to the inherent characteristics of this projection like superimposition of the right and left structures and variations in their magnifications as a result of their different distances from the film and X-ray source; its interpretation in diagnosing transverse problems is of limited value.
The panoramic radiograph is a useful view for an overall examination of the dental and bony structures of the maxilla and the mandible. Certain conditions like missing or supernumerary teeth, impacted teeth, the presence of gross pathology etc. can be assessed. It also provides valuable information on comparison of some structures such as mandibular ramus, condyles and configuration of inferior border of the mandible on both sides.
Posteroanterior cephalogram: For cephalometric assessment of orthodontic problems, the routinely prescribed radiograph is the lateral cephalogram. Only when a transverse problem or an asymmetry of face is detected, then the clinician asks for a frontal radiograph. It is a valuable tool in the assessment of the right and left structures of the dentofacial complex. Since these structures are located at relatively equal distances from the film and X-ray source, the unequal enlargement by the diverging rays and the distortion as in lateral cephalogram are significantly reduced. This promotes proper registration and evaluation of the facial and dental midlines and an accurate comparison between the sides to determine the extent of the asymmetry present. The use of posteroanterior cephalogram is fraught with inherent problems: difficulty in reproducing head posture; difficulty in identifying landmarks because of superimposed structures or poor radiographic technique; and concern about exposure to radiation.16
Despite these disadvantages numerous frontal cephalometric analyses have been used for several decades for surgical application as well as orthodontic use. Figure 5.6A illustrates the commonly used frontal cephalometric points. In orthodontic usage, frontal cephalometric assessment serves two primary purposes:
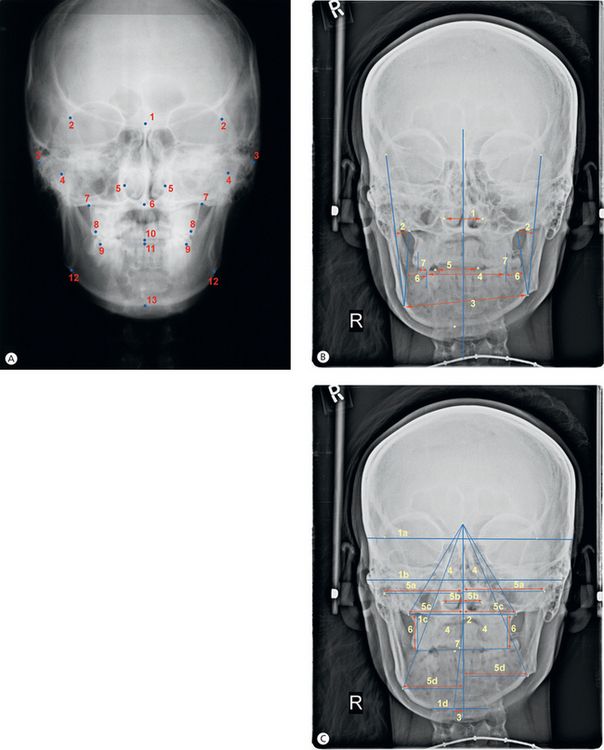
Figure 5.6 (A) Frontal cephalometric points. 1, Crista galli (Cg). 2, Point at the medial margin of the zygomatico frontal suture (left and right) (Z points). 3, Point at the most lateral border of the centre of the zygomatic arch (left and right) (ZA points). 4, Most superior point on condylar hand (left and right) – condylion (Cd). 5, Most lateral aspect of the piriform aperture (left and right) (NC). 6, Anterior nasal spine (ANS). 7, The intersection of the lateral contour of the maxillary alveolar process and the lower contour of the maxillo zygomatic (Jugal) process of the maxilla (left and right)–point Jugale (J points). 8, The most prominent lateral point on the buccal surface of the first permanent maxillary molar (left and right) (A6). 9, The most prominent lateral point on the buccal surface of the first permanent mandibular molar (left and right) (B6). 10, The mid point between the mandibular central incisors at the level of the incisal edges – incision inferior frontale (iif). 11, The midpoint between the maxillary central incisors at the level of the incisor edges – incision superior frontale (isf). 12, The highest point in the antegonial notch (left and right) – antegonion (Ag). 13, Menton (Me). (B) Frontal cephalometric assessment. 1, Nasal cavity width – distance between NC points. 2, Maxillary relation (maxillary concavity) – distance from J point to frontal facial plane (Z-Ag) on either sides. 3, Mandibular width – distance between Ag points. 4, Intermolar width – distance between buccal surfaces of mandibular first molars. 5, Intercuspid width – distance between incisal cusp tips of mandibular canines. 6, Lower molar to frontodenture plane (B6 to J-Ag) on either sides. 7, Buccal surface of upper molar to lower molar. (C) Assessment of asymmetry. 1, Four horizontal planes – a, connecting medial aspects of the zygomatico-frontal sutures (Z–Z); b, connecting the centres of the zygomatic arches (ZA-ZA); c, connecting the medial aspects of the jugal processes (J–J); d, plane parallel to Z plane at menton. 2, Distance from ANS to midsagittal plane. 3, Distance from Pog to midsagittal plane. 4, Two pairs of triangles, each pair bisected by mid sagittal plane – One pair from Cg to J to MSR on either sides, one pair from Cg to Ag to MSR on either sides. 5, Linear distances to the mid sagittal plane from bilateral points – a, condylion; b, nasal cavity; c, J point; d, antegonion. 6, Distance from the buccal cusps of the upper first molars (on the occlusal plane) along the J perpendiculars. 7, Distance between incision inferior frontale and ANS-Me plane and distance between incision superior frontale and ANS-Me plane.
The selection of a reliable vertical reference line is pivotal in carrying out frontal cephalometric assessment. Grummons and Van De Coppello suggested a midsagittal reference plane running vertically from crista galli through anterior nasal spine to the chin area. This plane will typically be nearly perpendicular to the Z plane (the plane connecting the medial aspects of the zygomaticofrontal suture).16
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses