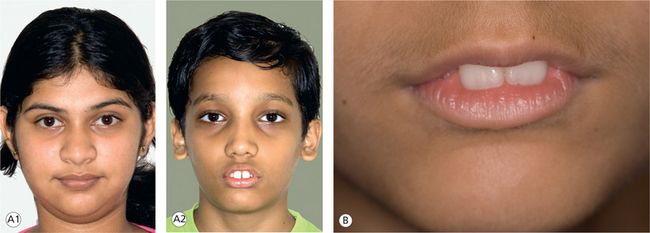
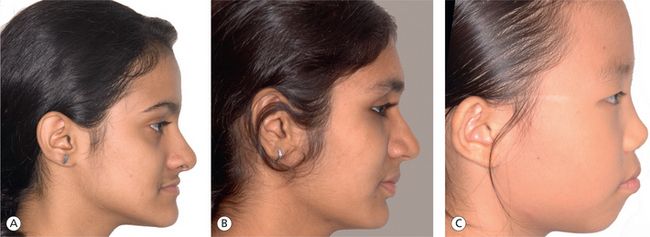
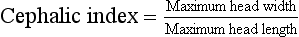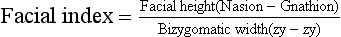Craniofacial growth, diagnosis and treatment planning
Advances in diagnostic technology, appliance design innovations and expansion of practises to include diverse patient populations have transformed the face of orthodontics over the past several years. These have resulted in ever increasing levels of well-conceived efficient and customized care, while simultaneously increasing the challenge of designing a treatment plan appropriate for each individual patient. Accurate diagnosis is a key element in the design of any successful treatment plan.
Diagnosis in orthodontics, like in other disciplines of dentistry and medicine, is the recognition of abnormal conditions, the practical synthesis of the diagnostic information that helps the clinician to plan an appropriate treatment strategy. A well-designed questionnaire for patient interview, numerous clinical observations, individual findings and analysis of relevant diagnostic records are essential to establish a correct diagnosis. It is a scientific procedure and does not offer any scope for individual opinion or judgment. The information generated must be objective, relevant and accurate.
This information is sourced from patient history – both dental and medical examinations, clinical examination and functional analysis. As a part of a routine examination, it is supplemented with the findings of the analysis of various diagnostic records like lateral cephalometric analysis. Certain cases may require further examination methods or specialized diagnostic records to generate additional information about a specific area. These various individual findings must be properly synthesized to result into a summary of the most important findings, devoid of any insignificant information having no relevance to the treatment. The clinician’s ability to interpret and synthesize the relevant data is a key to establish comprehensive diagnosis. Improper or inaccurate diagnosis is often caused by insufficient information or predetermined decisions made in an effort to adapt the case to a particular type of treatment modality.
This requires that the practitioner should also have adequate knowledge about the craniofacial growth and its clinical implications.
Craniofacial growth: a clinical perspective
Majority of the problems that are encountered by the orthodontist in a day-to-day clinical practise are related to growth. The difficulty in dealing with such problems may involve a failure on the part of the orthodontist to diagnose a growth and development problem or a poor patient cooperation in which the orthodontist is not given the chance to solve the problem, or it may be a growth pattern that is beyond the control of both the patient and the orthodontist. It is, therefore, essential that the clinician gives due importance to the significance and assessment of craniofacial growth while dealing with variety of clinical situations.
The orthodontic practitioner must realize that the facial pattern is not constant; it is changed during growth and is also changed by orthodontic treatment. The treatment planning process must involve proper prediction of future growth and response to treatment, which requires better understanding of facial growth. This helps the clinician to institute optimal treatment to the patient. When jaws grow, they move and carry the dentition with them. If the amount and the direction of the movement of both the jaws as a result of growth is the same, the occlusion remains unchanged. However, disproportionate growth leads to the development of a new relationship of jaws to each other. This change in jaw relationships is often associated with compensatory tooth movements in one or both the jaws. Differential growth can occur anteroposteriorly, vertically or transversely. As the changes in the face and dentition continue throughout life, the clinician must consider both the immediate outcome of the treatment and the long-term stability and the benefits of the treatment as important goals.
For better understanding of the craniofacial growth, it is important to know the sites or the location of the growth and the type of growth occurring at that location. The growth of the craniofacial complex that is relevant to the orthodontic professional can be divided into following areas:
Cranial base
The cranial base is essentially a midline structure in which the bones are formed initially in a cartilage and later transformed to bone by endochondral ossification. The changes in the cranial base take place primarily as a result of endochondral growth, mainly at various synchondrosis (Figs 1.1 and 1.2). As ossification proceeds, bands of cartilage called synchondroses remain between the centres of ossification, which subsequently get converted into bone. The midline cranial base contains four primary cartilaginous sutures or synchondroses: the intersphenoidal sutures close by birth, the intraoccipital synchondrosis closes around 5 years of age, the sphenoethmoidal synchondrosis closes around 6–7 years of age and the sphenooccipital synchondrosis closes by 13–15 years of age.
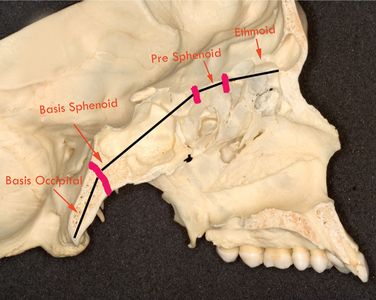
Figure 1.1 Sagittal section of the skull showing the cranial base and the approximate location of important growth sites.
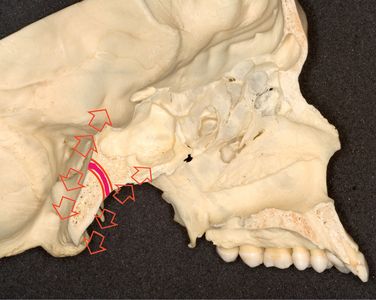
Figure 1.2 Growth at the sphenooccipital synchondrosis in which the maturing cartilage cells extend in both directions away from the centre as a part of endochondral ossification occurring at both margins. It contributes to the increase in length of this area of the cranial base.
As the sphenoethmoidal synchondrosis closes by 6–7 years of life, the segment of the anterior cranial base – designated as the planum sphenoidale – becomes relatively stable, early in life.1 Therefore, this area is usually used for cephalometric superimpositions to evaluate the changes in the face due to either growth or treatment. The sellanasion (SN) plane is frequently used as a reference plane in order to more accurately determine the changes occurring in the facial structures. The distance between sella and nasion normally increases by approximately 1 mm per year from 6 to 16 years of age. Another frequently used reference plane is nasion–basion plane. The distance between nasion and basion increases by approximately 1.7 mm per year between 6 and 16 years of age. After the closure of the sphenooccipital synchondrosis, any changes occurring either in the length or in the flexure of the cranial base are as a result of remodelling or surface deposition or resorption.2
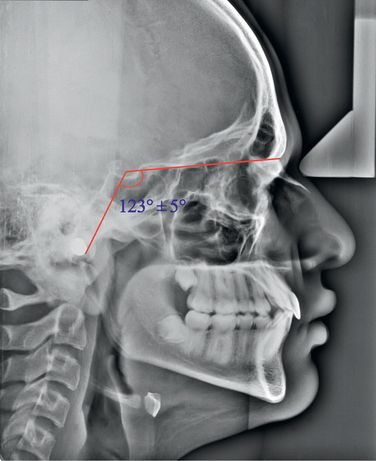
Though there are minor opening and closing movements in the cranial base angle, this angle is relatively stable for most part. The average cranial base angle is approximately 130°. Obtuse or open cranial base angles are usually associated with a more backward position of the mandible and hence a Class II type of facial pattern. A more acute or closed cranial base angle is normally associated with a more forward position of the mandible and hence a Class III type of facial pattern. The sagittal growth centre – the sphenooccipital synchondrosis – is located in the region of the posterior cranial base, and the growth changes in this area determine the position of the fossa. A large angle between the anterior and posterior cranial base, measured cephalometrically as N-S-articulare (Ar), indicates a posterior position, and a small angle indicates an anterior position of the fossa. The mean value is 123° ± 5° (Fig 1.3). This deviation in the position of the fossa is often compensated by the length of the ascending ramus. If there is no compensatory growth of the ascending ramus, this leads to either retrognathic or prognathic facial profile. Because the glenoid fossa determines the posterior/superior limit of the mandible, it holds important implications for mandibular displacement. Björk3 indicated that the distance between the fossa and the nasion increases by 7.5 mm between 12 and 20 years of age when the landmark Ar is used. As a result of the elongation of the posterior cranial base, the fossa and the temporal bone are displaced inferiorly and posteriorly.4 It was observed that the glenoid fossa was displaced between 1.8 and 2.1 mm posteriorly and between 1.0 and 1.8 mm inferiorly, and it demonstrated greater posterior and inferior displacement during adolescence than during childhood.5 Therefore, during the treatment planning process for skeletal correction, the clinician should consider posterior fossa displacements to be added to any existing anterior discrepancies and future growth deficiencies. Another important growth change that occurs in the cranial base is the remodelling that takes place in the anterior cranial fossa. This brings about a forward displacement of the frontal bone and the nasal area.6
Maxilla
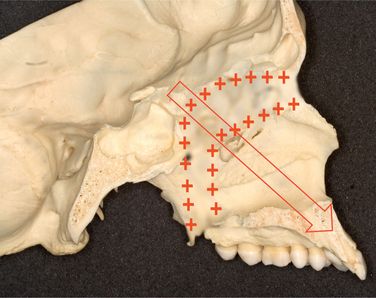
The maxillary complex is surrounded by a system of sutures such as zygomaticomaxillary, frontozygomatic, sphenopalatine and pterygomaxillary. The maxilla mainly grows by bone apposition at the sutures that connect the maxilla to the cranium and the cranial base and by surface remodelling (Fig 1.4). Björk7 in his implant study carried out to evaluate the changes in the growth direction of the nasomaxillary complex between 7 and 19 years of age and observed that the maxilla grew in a downward and forward direction at an angle of approximately 51° to the anterior cranial base (SN plane) with a very large range of 0–82° (Fig 1.5). This variation explains the fact that the maxilla would grow primarily in a horizontal direction in some patients, while it would grow primarily in a vertical direction in others. It has been observed that during the first decade of life, the maxillary growth proceeds normally in a horizontal direction, while during the second decade of life, it proceeds in a more vertical direction.7
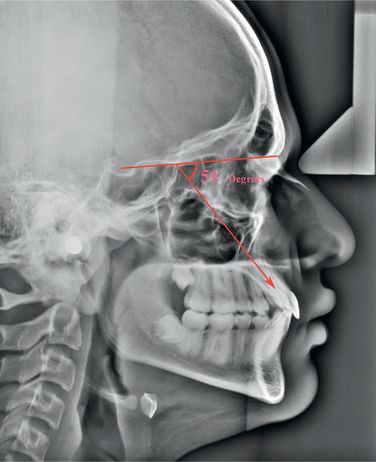
Figure 1.5 The growth of the nasomaxillary complex from 7 to 19 years of age moves it downward and forward at an average angle of 51° with the cranial base.
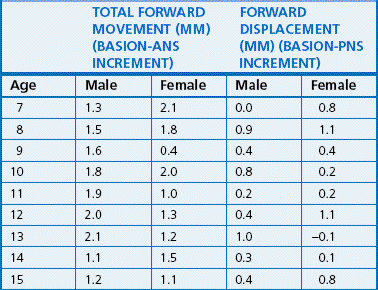
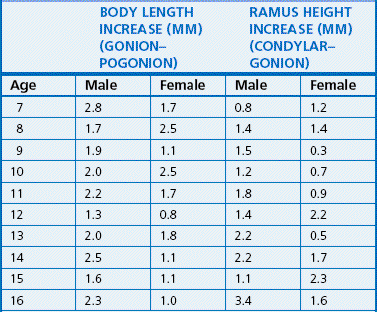
The displacement and remodelling changes play an important role in the growth of the maxilla.6 The horizontal displacement of the maxilla is primarily due to remodelling expansion within the middle cranial fossa. Also, deposition of bone on the posterior aspect of the maxilla, in the area of tuberosity, allows it to keep pace with the forward displacement of the frontal and nasal bones (as a result of expansion of the anterior cranial base) and to accommodate for the eruption of the permanent molars. The maxillary length changes are shown in Table 1.1. The vertical displacement of the maxilla occurs primarily by growth and expansion of the eyeballs and the nasal septum. The growth of the cartilaginous nasal septum, especially the vomer and the perpendicular plate of the ethmoid, carries the nasomaxillary complex downward and forward.1 At birth, the nasal septum is made up entirely of cartilage and extends down to lie within the U-shaped vomer in the vomerine groove. During the first year of life, ossification begins in the perpendicular plate of the ethmoid. By 3 years of age, ethmoid reaches the vomer, and by 10 years of age, it is in contact. After this period, the downward growth of the upper face occurs primarily by the process of apposition. On an average, the amount of this vertical displacement measured from the SN plane to the palatal plane is just over 1 mm per year.
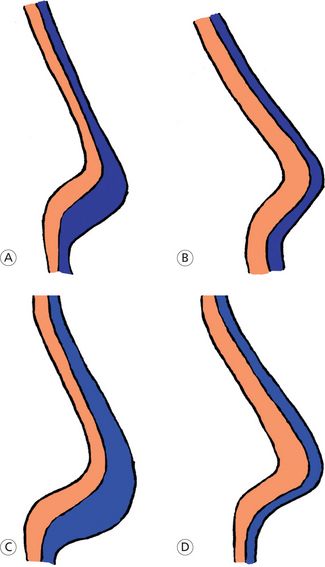
The maxilla, as a result of remodelling changes, takes on periosteal deposits of bone on all of its surfaces. The most significant amount of bone deposition occurs on the posterior aspect of the maxilla. This, in addition to the lateral deposits, allows for lengthening of the dental arch and eruption of the upper teeth. The palate receives periosteal deposits on its oral surface and is resorbed on its nasal surface. In addition to these horizontal and vertical growth changes, the maxilla can undergo rotational change (Fig 1.6). The maxilla can rotate in a downward and forward direction anteriorly, as occurs in the anterior deep bite case, or it can rotate in an upward and forward direction, as occurs in anterior open bite case. The amount and the direction of these rotational changes can be determined by the angle between the SN plane and the palatal plane or by the angle of inclination (AM Schwarz) between the Pn line (perpendicular from N’) and the palatal plane. The posterior end of the hard palate does not seem to be subjected to influence by Class III elastics.8 However, the maxillary molars may be encouraged to grow downward away from the palatal plane. Anterior end of the hard palate is easily influenced by Class II elastics and extraoral anchorage.9 Growth at the intermaxillary and interpalatine sutures, contributing mainly to the maxillary width, occurs during the first 5 years of life.
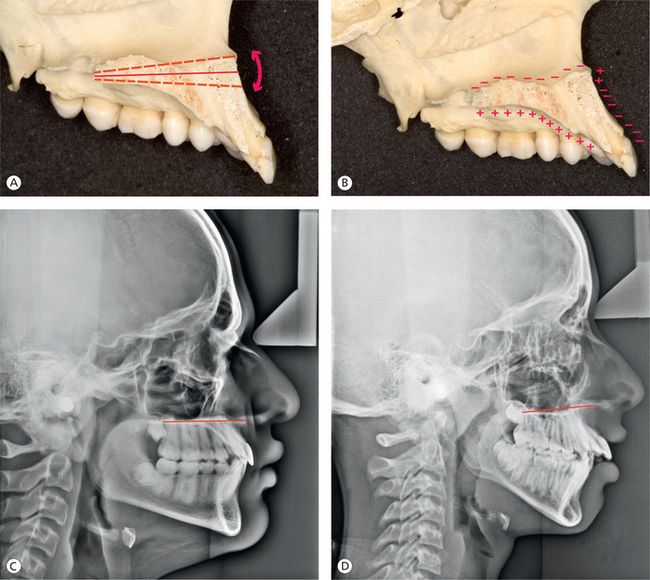
Figure 1.6 Rotational changes in the maxilla. (A) Diagrammatic representation of the rotational changes of the maxilla on the sagittal section of the skull. (B) Surface remodelling changes at the nasal floor, the roof of the mouth and the anterior surface below the anterior nasal spine. (C) Normal orientation of the palatal plane. (D) The palatal plane is tipped upward anteriorly.
Mandible
Compared with the growth of the maxilla, both endochondral and periosteal activity play an important role in growth of the mandible. For years, the condylar cartilage was considered a primary growth centre, acting in a manner similar to the epiphyseal growth plate of a long bone. However, histologically, the condylar cartilage is quite different from the cartilage of the epiphyseal growth plate. The mandible is a unique bone that grows in many different ways. It should not be considered a single growth entity but rather different entities, mainly at condyle and ramus, corpus, posterior alveolar process and anterior alveolar process. Other than condyle, all other areas of the mandible are formed and grow by direct surface apposition and remodelling.6 (Fig 1.7).
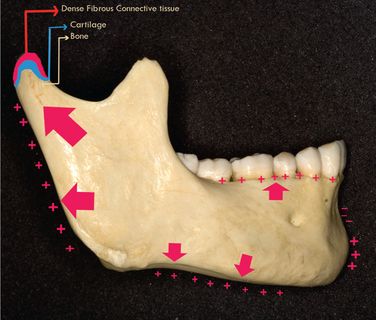
Figure 1.7 Surface remodelling changes in the mandible. Diagrammatic representation of the unique growth mechanism of the mandibular condyle showing both interstitial and appositional proliferation.
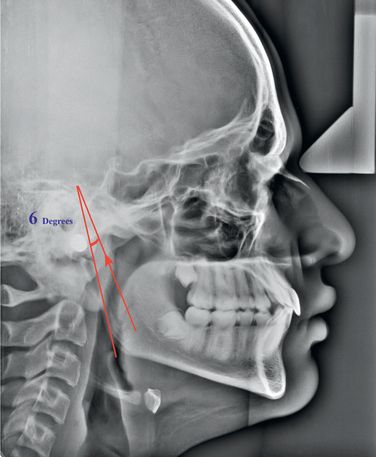
Björk10 provided an excellent information on the growth of the mandible with his implant studies. These studies revealed that average direction of condylar growth was 6° anterior to a line drawn tangent to the posterior border of the ramus (Fig 1.8). This emphasized the distinct curvature in the direction of condylar growth. He observed condylar growth of 3 mm per year during the childhood period, a slight decrease to prepubertal minimum, followed by an adolescent spurt peaking at 5.5 mm per year at approximately 14.5 years of age. Baumrind et al11 observed that condylar growth remains relatively constant between 8.5 and 15.5 years for both treated and untreated patients. The results of another study showed that the condyle grew between 0.8 and 1.3 mm posteriorly and between 9.0 and 10.7 mm superiorly over the 4-year period.5 The vertical condylar growth was approximately nine times greater than the posterior condylar growth. Boys showed significantly greater superior condylar growth during adolescence than during childhood.
The average individual experiences resorption below the ramus and deposition of bone below the symphysis. These two changes by themselves would tend to increase the gonial angle. The anterior aspect of the chin is generally unaffected and chin prominence occurred by horizontal growth and some resorption at point B. Due to extensive and variable remodelling changes on the inferior border of the mandible, it is considered unsuitable to be used as a reference plane. Björk stated that the four areas in the mandible that are most suitable for the purpose of superimposition are the tip of chin, the inner cortical surface of the inferior border of symphysis, the mandibular canal and the lower contour of the third molar germ from mineralization to root formation.
The posterior growth of the condyle and the posterior border of the ramus contribute to the elongation of the mandibular corpus and the primary displacement of the mandible. Table 1.2 shows growth changes in the mandibular length. The mandible also undergoes secondary displacement as a result of the enlargement of the middle cranial fossa. However, this is not as pronounced as that of the maxilla since the middle cranial fossa growth is mostly localized anterior to the condyles. On the average, ramus height increases by 1–2 mm per year and body length increases by 2–3 mm per year.12
The mandible also undergoes rotational change due to the rotation that occurs in the core of the jaw, called internal rotation, and due to surface bone remodelling and alterations in the rate of tooth eruption leading to external rotation13 (Fig 1.9). The internal rotation essentially consists of rotation around the condyle (matrix rotation, 25%; Fig 1.9A) and rotation centred within the body of the mandible (intramatrix rotation, 75%; Fig 1.9B). The combination of internal and external rotation results into the overall change in the orientation of the jaw. In majority of the individuals, the core of the mandible, the bone that surrounds the inferior alveolar nerve, rotates during growth in a manner that tends to decrease the mandibular plane (MP) angle (up anteriorly and down posteriorly).
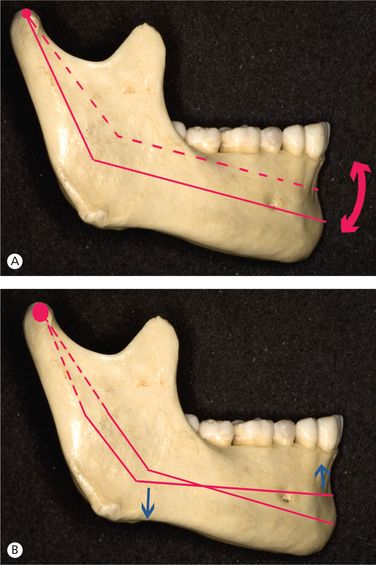
Figure 1.9 Internal rotation of the mandible. (A) Rotation around the condyle (matrix rotation). (B) Rotation within the body of the mandible (intramatrix rotation).
The compensatory surface changes (external rotation) do not allow proportionate decrease in the MP angle as a result of the forward rotation of the core of the mandible. In the average individual during childhood and adolescence, approximately 15° of internal rotation (forward rotation), as observed normally, results into just 3°–4° of decrease in MP angle due to compensatory 11°–12° of external rotation (backward rotation). This compensatory external rotational change is considered to be due to resorption at the posterior part of the lower border of the mandible and due to the apposition at the anterior part of the lower border.
Dental arches
The growth of the maxillary and mandibular alveolar bone is significantly influenced by the presence and eruption of the teeth. Alveolar processes undergo selective remodelling changes through bone deposition and resorption. The facial height is increased primarily due to the vertical growth of the maxillary and the mandibular alveolar processes, which in turn is determined by the eruption of the teeth.
As mentioned earlier, the growth of the alveolar processes is influenced by the presence and the eruption of the teeth. After the eruption of teeth, the progression of the primary dentition to the permanent dentition has an impact on dental arch length, circumference and intercanine and intermolar widths14 (Fig 1.10). In the maxillary arch, there is an increase in the intercanine width by an average of 6 mm between 3 and 13 years of age and by an average of 1.7 mm between 13 and 45 years of age.14 The intermolar width in the primary dentition increases by 2 mm between 3 and 5 years of age. The inter-first-molar width increases by 2.2 mm between 8 and 13 years of age, and by 45 years of age, it decreases by 1 mm.
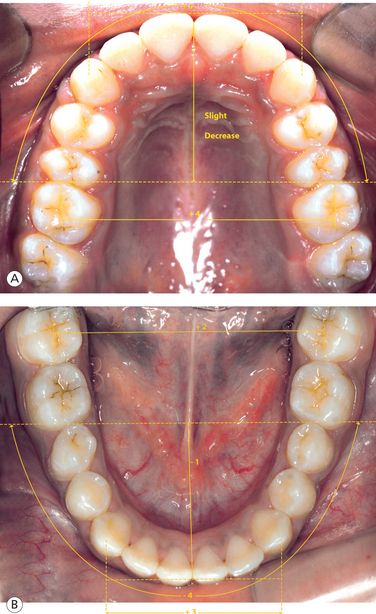
Figure 1.10 Dimensional changes (in millimetres) in dental arches between 6 and 18 years of age. (A) Maxillary arch changes. (B) Mandibular arch changes.
In the mandibular arch, the intercanine width increases by approximately 3.7 mm and then decreases by 1.2 mm between 13 and 45 years of age.14 There is an increase in intermolar width of 1.5 mm between 3 and 5 years of age. An increase in inter-first-molar width of 1 mm between 8 and 13 years of age is followed by a decrease of 1 mm by 45 years of age.14 Certain changes in the mixed and permanent dentition like uprighting of the incisors and the loss of the leeway space result in decrease in the arch length.
Horizontal and vertical growth interrelationship
It has been recognized that the growth at the mandibular condyles brings the chin forward, not downward, nor downward and forward. Then, how does the chin move downward and forward or downward and backward? It is only when the vertical growth increments of facial growth begin to influence the condylar growth through occlusal contact that a downward and forward/backward direction of the chin is produced. Therefore, the final vector of growth of the chin is a resultant of the interaction between horizontal growth (condylar growth) and vertical growth (vertical growth of molars). If the condylar growth is greater than the vertical growth in the molar region, there is counterclockwise rotation of the mandible with a resultant horizontal change in the chin position and a less increase in anterior facial height. The greater change in this relationship leads to deep bite. However, if the vertical growth in the molar region is greater than the growth at the condyles, the mandible rotates clockwise with a resultant vertical change in the chin position (less horizontal change) and an increased anterior facial height. The greater change in this relationship causes open bite.
Fred Schudy15 pointed out that the following vertical growth increments contribute to an increase in facial height:
It should be remembered that, in a patient with clockwise rotation of the mandible, an excessive vertical growth would not help to reduce the ANB angle and also the correction of Class II molar relationship. However, it does facilitate the correction and retention of overbite.15 On the other hand, counterclockwise rotation of the mandible associated with excessive condylar growth moves the pogonion forward, increases the facial angle, flattens the MP and tends to increase the overbite. In patients showing this type of growth pattern, it is difficult to correct the overbite and retain it. Therefore, molar height plays an important role in controlling the vertical position and, to some extent, the anteroposterior position of the chin.
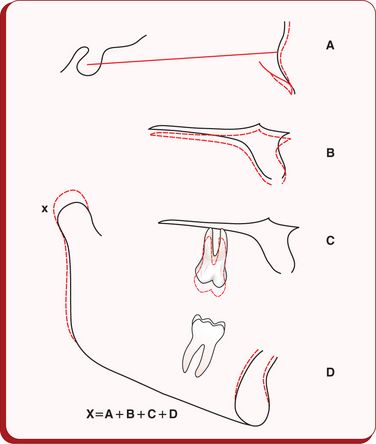
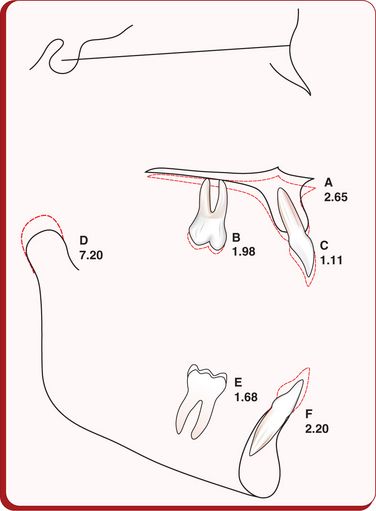
It is evident from the above discussion that the clinician must have deep understanding of these five principal growth increments – condylar growth, anteroposterior growth at nasion, the vertical growth of the corpus of the maxilla, vertical growth of the maxillary alveolar process and the vertical growth of the mandibular alveolar process –and the impact of their interaction on the chin position and outcome of the treatment. For the normal expression of the growth and the behaviour of the mandible, the condylar growth should equal the total of other four growth increments15 (Fig 1.11). The vertical growth of the anterior alveolar processes does not have a significant effect on facial height. However, it results in varying degrees of overbite. The vertical growth of the posterior alveolar process of the maxilla exceeds that of the mandible from age 8 to 14.16 Average growth (in millimetres) of maxilla, maxillary first molar, maxillary incisor, mandibular condyle, mandibular first molar and mandibular incisor in a 3-year period is shown in Figure 1.12.
Overbite changes
The growth of the jaws plays an important role in establishing varying degrees of overbite. The relationship between the condylar growth and the vertical growth of the posterior and anterior alveolar processes controls the amount of overbite. Therefore, to control deep bite or open bite, the clinician should control growth increments that determine this vertical relationship. Fred Schudy17 has called attention to the following growth increments that are relevant to the overbite relationship.
As mentioned earlier, the vertical growth of the body of the maxilla and maxillary molars has the effect of pushing the mandible downward and backward through occlusal contact, influencing the overbite. The downward growth of the maxillary molars significantly exceeds the downward growth of maxillary incisors (by almost 2:1). Of all the six growth increments, the movement of maxillary incisors downward and away from the palatal pane is the smallest, while the mandibular incisor growth is perhaps the greatest and most variable.17 The vertical growth of the mandibular molars plays a minor role among these factors.
Facial soft tissue growth
Establishing optimal facial aesthetics is the primary goal of orthodontic treatment. As the position of the underlying hard tissues influences the morphology of the overlying facial soft tissues, it is essential for the clinician to have adequate knowledge of the soft tissue components of the face. In addition to this, the soft tissues of the face undergo significant changes throughout life due to growth, maturation and ageing; this information plays an important role in orthodontic diagnosis and treatment planning.
Nasal growth
Anatomical relationships and proportions of the nose, lips and chin largely determine the configuration of the face. The balance and harmony among these components is essential for the pleasing soft tissue facial profile. This is influenced by both growth and orthodontic treatment. In addition to understanding the changes that occur due to orthodontic treatment, the clinician should have knowledge about the amount and the direction of growth of the soft tissue elements of the face.
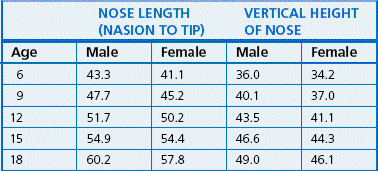
The projection of the ‘dorsal hump’ is increased due to the rotation of the upper nasal dorsum upward and forward (counterclockwise) between 6 and 14 years of age.18 The lower dorsum growth changes are related to vertical and horizontal skeletal patterns in the lower face, with clockwise rotation of the lower dorsum in vertically growing individuals. In females, the nasal projection remains virtually constant from 12 to 17 years of age, while in males, it shows a continued greater rate of growth with a resultant greater degree of nasal prominence at age 17.19 Several studies have pointed out that the nose grows downward and forward20,21(Fig 1.13). Both males and females experience proportionally more growth in the vertical dimension than the anteroposterior projection of the nose. In males, a spurt of growth occurs between 10 and 16 years of age with its peak from 13 to 14 years.20 The females show comparatively a steadier growth curve, with small percentage of subjects showing a nasal growth spurt around the age of 12 years. The majority of growth in length of the nasal bones takes place before the age of 10 years, but the soft tissues continue to grow downward and forward along with the maxillary complex.22 The growth changes in length and height of the nose are shown in Table 1.3.
Growth changes in the lip length and thickness
The upper lip rapidly increases in length from approximately 1 to 3 years of age, with a reduction in the rate of incremental growth between 3 and 6 years of age.20 From age 6 onward, a progressive increase in lip length continues till age 15. Most of the maxillary lip length is achieved by age 14 in females and by age 18 in males. The mandibular lip-length growth continues longer than the maxillary lip-length growth in females, which is complete by age 16.23 The incremental growth is greater in males than in females, which is not entirely complete by age 18. The changes in the lower anterior facial height due to vertical skeletal and dentoalveolar growth are usually concluded before completion of vertical lip growth, with comparatively more growth of the lower lip than the upper lip.24 Similar to many aspects of facial growth, the vertical growth of the lips is age and gender related.
The upper lip thickness increases in both males and females between 1 and 14 years of age, which continues in males beyond age 14.20 The upper lip thickness increases more in the vermillion region than in the part of the lip overlying point A. This change is proportional to the increase in length of the lip. In a similar manner, an increase in the thickness of the lower lip is greater in the vermillion region than at pogonion and point B. The upper lip thickness in females is at its maximum by 14 years of age and remains the same till age 16, with lip thinning afterward.23 In males, the upper lip thickness is at its maximum by 16 years of age, with lip thinning afterward. The lower lip thickness in both males and females is generally concluded by 15 years of age.23
The chin growth
The soft tissue chin thickness in females from 7 to 9 years of age is 11.7 mm, which increases by 1.6 mm up to age 17, whereas in males, it is 10.8 mm from age 7 to 9 and shows an increase of 2.4 mm up to age 17.19 This results in similar soft tissue chin thickness of 13.3 mm in both males and females at the age of 17 years.
Posttreatment craniofacial growth
In this chapter, the discussion on craniofacial growth so far has been related to actively growing individuals who constitute a large portion of the average orthodontic patient population. However, a portion of growth that usually occurs after orthodontic treatment can influence the long-term stability of a treated case. Therefore, for comprehensive and successful treatment of the growing child, every clinician should have knowledge about this ‘terminal growth’ of the craniofacial complex. George Schudy25 studied 74 orthodontically treated Caucasians to analyse the effects of post-treatment terminal growth on dentition and deeper basal structures (Fig 1.14). He suggested that the typical terminal growth is characterized by a decrease in SN-MP, SN-occlusal plane and the gonial angle. The mandible moves forward more than the maxilla, and the condylar growth proceeds in a predominantly vertical direction. The maxillary first molar moves forward more than the mandibular first molar. The upper incisors usually tip forward during the terminal phase of jaw growth. Posttreatment mandibular rotation, expressed by decreased SN-MP angle and lingual movement of lower incisor teeth, contribute to the overbite relapse and arch length reduction. The facial profile becomes progressively less convex primarily due to nasal growth and forward movement of the chin.
Ageing: skeletal and soft tissue changes
Knowledge on changes in the dentofacial complex as a result of ageing process is crucial to modern orthodontic diagnosis and treatment planning and should be of significant value to all orthodontists. The study by Behrents26 involving 113 untreated individuals from 17 to 83 years of age provided comprehensive data on the subject. In his study, the subjects from the age of 17–41 years (young adulthood) maintained their craniofacial patterns – Class II individuals grew as Class II individuals, and Class III individuals grew as Class III individuals. The subjects in the age group of 41–83 years showed vertical dimensional changes and became less protrusive. The males showed counterclockwise rotation of the mandible, and females tended to be more vertically growing. The percentage of change in the females was less than that in the males.
The soft tissue changes from age 17 to 83 included increased nasal projection and inferior movement of the nasal tip. The lips became less prominent and positioned inferiorly. Due to decreased lip prominence and lowering of the nasal tip, the nasolabial angle tended to become more acute. Dental changes included uprighting of the maxillary incisors and protrusion of the mandibular incisors in female group only. The mandibular molars uprighted in the males, and it moved forward in the females. The maxillary molars tipped mesially in the males, and it uprighted in the females.
Diagnostic information
The first step in the assessment of orthodontic patients is to generate relevant diagnostic information to establish accurate diagnosis and formulate a treatment plan. It is important to consider the improvement of patient’s physical and emotional well-being as a part of a successful orthodontic treatment outcome. A sound knowledge of normal anatomy, growth and development is essential to recognize various dentofacial deformities. The goals of diagnostic and treatment planning process are threefold:
Patient interview (Questionnaire)
The patient interview is often the first formal interaction between the patient and the orthodontist. Patient’s general personal information and demographic data should be recorded to facilitate efficient communication between the patient and the office. The patient interview essentially consists of family history and patient history. The goal is to understand the development of the problem to institute appropriate therapeutic procedures and eliminate early causative factors. The author considers the patient’s chief complaint or concern as the most important ingredient of patient interview process, as it provides valuable information on whether the patient is seeking functional improvement, aesthetic improvement or both. It also helps in designing a treatment strategy that should ideally incorporate the specific needs and desires of the patient.
A family (genetic) history is aimed at gathering some valuable information about certain malocclusions and other abnormalities present in members of the same family. A data pertaining to the history of orthodontic treatment for any siblings of the patient and either or both parents and the nature of their problems should be recorded. It should be noted that relatively a large number of craniofacial abnormalities are inherited and transmitted through a dominant gene, while in cases of cleft lip and palate, it is mostly through a recessive gene. During the course of interaction, it is common to have a patient or a parent respond that a close relative had a severe problem that required surgery.
Patient’s history should include any postnatal trauma, the manner of feeding and nutritional disturbances. Inquiries should be made with respect to the child’s general development like the initiation of walking and talking and the eruption of the first deciduous tooth. It is important to explore the possibility of having any abnormal habits like digit sucking and mouth breathing. Relevant information regarding allergies, medications, previous hospitalizations or traumatic injuries should be carefully recorded. While taking patient history, psychological aspects of orthodontic treatment should be discussed with the patient to determine motivation and attitude towards treatment, treatment result expectations, patient compliance etc. Such information is extremely useful to estimate future cooperation during treatment. Medical history of the patient forms an important part of the diagnostic information as it can indicate compromising factors that need special attention during treatment.
In patients with diabetes mellitus, it is essential to get blood glucose level under control prior to orthodontic treatment.27 Plaque control is critical in such patients as they are more prone to develop tooth decay and periodontal breakdown. Diabetes-related microangiopathy can occasionally occur in the periapical vascular supply, resulting in unexplained odontalgia, sensitivity on percussion, pulpitis or even a loss of vitality in sound teeth.28,29 The clinician should be alert to this phenomenon and should regularly check the vitality of teeth involved, especially when treatment is carried out for a prolonged duration. In adult patients with diabetes, it is important, prior to orthodontic treatment, to obtain a full-mouth periodontal examination including probing depth, plaque and gingivitis scores to determine the need for specific periodontal treatment. Deviations from appropriate diet and the scheduled insulin injections will result in distinct changes in the serum glucose level.30 Hypoglycemic reactions might occur more often in these patients. Type I diabetes mellitus is more often encountered in younger patients who frequently come for orthodontic treatment. For such patients, it is advisable to schedule long duration appointments in the morning hours, and the patient is advised to eat a usual meal and take required medication.
Orthodontic patients with bleeding disorders present two main challenges to the orthodontist: risk of viral infection (hepatitis and HIV) and risk of excessive bleeding. Treatment planning in such patients should incorporate reduction in the duration of treatment and nonextraction treatment whenever possible. Any gingival or mucosal irritation should be avoided; therefore, bonding of molar tubes is preferred over placing bands on the molars. In painful situations, it is better to prescribe acetaminophen with codeine if required and avoid aspirin. In case of gingival bleeding, 25% zinc chloride should be applied.
Patients with HIV infection are in an immunodeficient state and are more susceptible to infections. Therefore, necessary precautions should be taken to avoid cross-infections. Case history pertaining to the past and current medications should be obtained, and its relevance to the orthodontic treatment should be assessed. Low dosage of corticosteroids (1 mg/kg body wt) decreases tooth movement by suppressing osteoclastic activity.31 However, high dosage of corticosteroids (15 mg/kg body wt) increases osteoclastic activity, producing more rapid tooth movement and subsequent relapse.32 Therefore, it is advisable to avoid use of corticosteroids during orthodontic treatment.
As there are more and more adults seeking orthodontic treatment, it is important to know the impact of use of bisphosphonates, used in the treatment of osteoporosis and malignancies, on orthodontic treatment. Certain procedures like extractions and placement of miniscrews for skeletal anchorage should be avoided.33
Clinical examination
Orthodontic complications almost always arise from errors in diagnosis and not from failures in implementation of the proposed treatment plan. The clinical findings, therefore, become the basis of diagnostic procedures to establish accurate diagnosis. The goals of clinical examination are as follows:
Natural head position
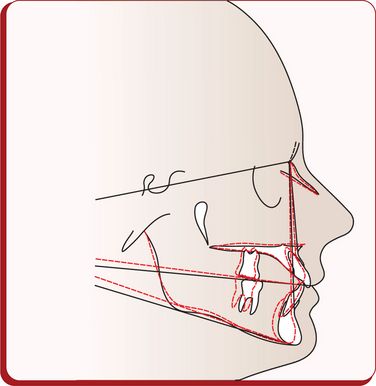
To record accurate clinical findings, the clinician should first determine the reference position of the patient in which the examination is carried out. For this purpose, it is appropriate to use the natural head position (NHP) in which the patient carries himself or herself in everyday life.34,35 In this position, the patient is instructed to sit upright and look straight ahead into the horizon or directly into a mirror mounted on the wall. This establishes a true horizontal line, parallel to the floor, where pupils of the eyes are centred in the middle of the eyes (Fig 1.15). It is based on the line of vision when the patient looks straight ahead, and it is related to the natural body posture and alignment with the cervical column.36 This position has shown reproducibility within the clinically acceptable variation of 4° as compared to the variability of 26° of FH plane and SN plane.35,37 NHP radiograph is obtained with the patient in the cephalostat looking straight ahead into a mirror and ear rods placed directly in front of the tragus with light contact with the skin to stabilize head in transverse plane. The patient should also be observed from the side to make sure that the pupil is in the middle of the eye. It should be noted that the lateral cephalostat ear rods alter the position of the head and neck during postural recordings.38 The patient should be comfortable and relaxed. The nose piece is then placed to establish third light contact with the skin, which secures the patient in NHP.
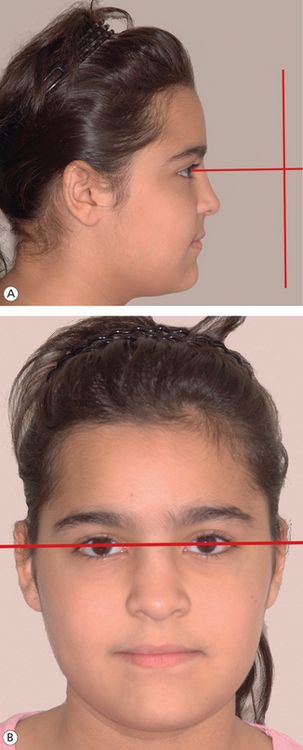
Figure 1.15 Natural head position. (A) The patient is looking straight ahead with the true horizontal coinciding with the line of vision and parallel to the floor. The pupils of the eyes are centred in the middle of the eyes. (B) The ‘true vertical’ is perpendicular to the floor and the ‘true horizontal’ (passing through the pupils).
Extraoral examination
Cephalic and facial type: Extraoral examination should be carried with the patient in NHP. This essentially consists of an assessment of the facial structures and the shape of the head. The shape of the head can be determined by the measurements derived from the cephalic index (Fig 1.16). It is based on the anthropological measurements of the width and the length of the head.
Dolichocephalic (long skull): less than 75.9
Brachycephalic (short skull): 81.0–85.4
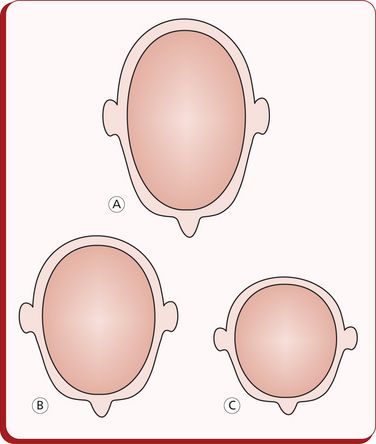
An assessment of facial frontal and profile view is essential in order to have a comprehensive understanding of the patient’s aesthetic characteristics.39 The facial type should be established from measurements derived from the proportional relationship of height and width of the face. The facial height and the width are determined by the distance between nasion and gnathion and bizygomatic width, respectively.
The average facial index in males is 88.5 ± 5.1, and in females, it is 86.2 ± 4.6. The facial index below normal is brachyfacial face type, indicating a broad and round face. The normal range facial index suggests that the face type is mesofacial, having average facial skeleton. If it is above normal, it is dolichofacial face type, indicating a long and narrow face due to high facial skeleton (Fig 1.17). This has a high significance in treatment planning as orthodontic treatment mechanics should be directed towards normalizing or at least maintaining the facial index. Also, it has been generally recognized that the form of the facial morphology has a certain relationship to the type of the archform. In a broader sense, expansion treatment modality is usually considered in borderline crowding cases of a broad facial type, while extractions are preferred in long face types.
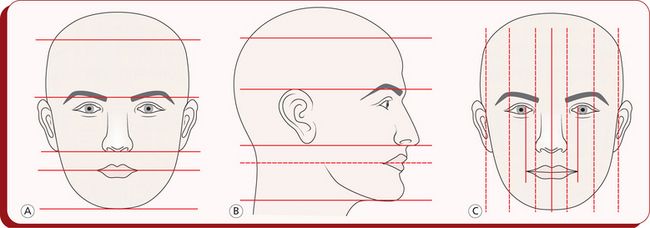
Frontal facial examination: Frontal view of the face is evaluated to determine vertical and horizontal proportions and symmetry, as any abnormality in proportion or asymmetry significantly contributes to the impaired facial aesthetics. In a patient with harmonious facial morphology, the height of the upper face determined by the distance between the hairline and the glabella (supraorbital ridges) should equal the height of the mid-face (measured between the supraorbital ridges to the base of the nose) and should also equal the height of the lower face (distance between the base of the nose and the chin)40 (Fig 1.18A). Within the lower one-third of the face, the distance between the base of the nose and the stomion should be half the distance from the stomion to the chin. Usually, the forehead is considered to be narrow or wide based on its relationship to the bizygomatic width.
In a bilateral symmetric face, the true vertical or the mid-line passes through the middle of the forehead, tip of the nose, the lips and the chin, perpendicular to the true horizontal (the line of vision) and divides the face into right and left equal halves (Fig 1.18C). Horizontally, the frontal face extending from left eye to right eye may be divided into three equal thirds: right and left eye widths and the nasal width. Also, the alar base (width of the base of the nose) should approximately equal the interinner canthal distance, and the width of the mouth should equal the distance between irises.40 At this stage of facial examination, it is important to evaluate facial and dental midlines for any deviation. A slight amount of facial asymmetry is common and may be considered ‘normal’. However, any gross facial asymmetry usually warrants further functional assessment for any deviations during various mandibular movements and also a skeletal examination with a posteroanterior cephalogram. Such evaluation provides fairly good information to the clinician for the overall facial appearance and proportionality.
Profile facial examination: Examination of the facial profile of the patient is carried out to assess the jaw relationships and soft tissue drape, both anteroposteriorly and vertically. It is imperative that the patient is relaxed with the head oriented in the NHP. Variations in the configuration of the forehead have been observed according to age and gender and are genetically and ethnically determined. The lateral contour of the forehead can be flat, protruding or oblique. Patients with steep forehead generally tend to have more prognathic dental bases than those with flat forehead.
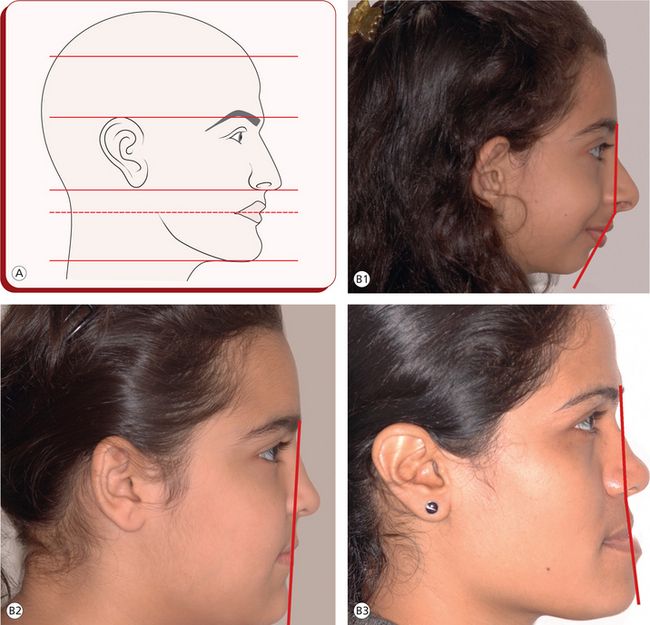
While assessing the facial profile, the clinician should consider vertical facial proportions (Fig 1.19A) and the relationship between two vertical lines – one from the glabella to the base of the upper lip and the other from the base of the upper lip to the most prominent point on the chin. This establishes whether the face is convex, straight or concave (Fig 1.19B). A convex angle indicates a Class II skeletal relationship, and a concave angle indicates a Class III skeletal relationship. The profile angle, however, only indicates the spatial relationship between the jaw bases relative to each other. Any deviation from the normal may be due to a disparity in absolute size, position or both. The facial divergence is determined by the inclination of the lower face relative to the forehead. Therefore, the possible line, normally straight and suggestive of an orthognathic profile, may slope anteriorly (anterior divergence) or posteriorly (posterior divergence). An inclination of MP should be clinically assessed by placing a scale or any instrument handle along the lower border of the mandible. A steep angulation indicates a high MP angle and usually a vertical growth direction. A nearly horizontal angulation indicates a low MP angle and generally a horizontal growth direction.
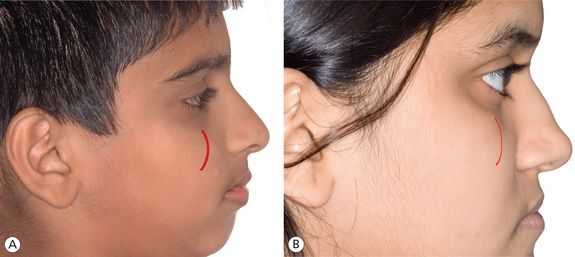
Malar sufficiency: The malar region should be observed for its optimal prominence. A direct quantification of the cheek bone prominence in millimetres is difficult. It needs to be assessed clinically as frontal and profile examination simultaneously. A prominent malar bone is a usual feature of an extreme case of horizontal grower (Fig 1.20A). Malar insufficiency is usually seen in an individual with maxillary retrognathism (Fig 1.20B).
Examination of nose: Morphological characteristics of the nose play an important role in the aesthetic appearance of the face (Fig 1.21A). To get an overall estimate of nasal proportion, the clinician should assess the ratio of the nasal width to the nasal height (GL-Sn), which should be 70%.41 Various anatomical parts of the nose, their analysis, interaction and role in nasal aesthetics and their contribution to an overall facial profile appearance may be evaluated with soft tissue cephalometric analysis. However, clinical examination should assess contour of the bridge and tip of the nose. The size, shape and width of the nostrils and position of the nasal septum should be assessed to determine an impairment of nasal breathing.
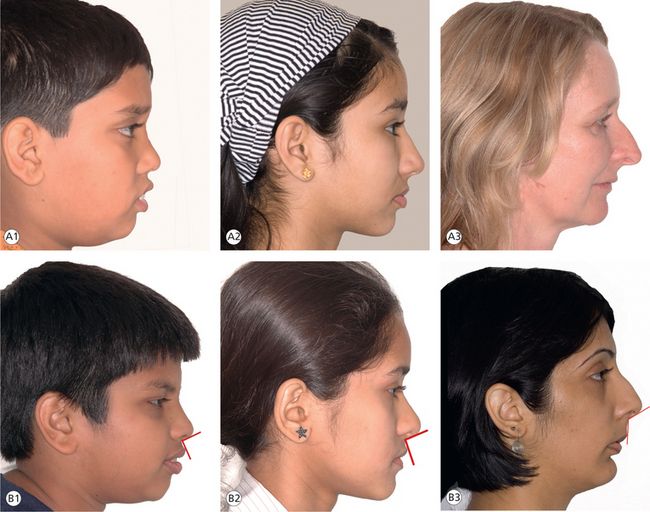
Figure 1.21 Examination of nose. (A) Nose size: (1) small nose, (2) average nose and (3) large nose. (B) Nasiolabial angle: (1) acute nasiolabial angle, (2) normal nasiolabial angle and (3) obtuse nasiolabial angle.
The nasolabial angle, formed by intersection of columella and upper lip tangent, should be in the range of 90°–120° (Fig 1.21B). Its morphology is a function of several anatomic features. An acute nasolabial angle is an indication of procumbency of maxilla, while obtuse nasolabial angle is produced by maxillary retrusion. When facial profiles are compared between males and females, female profiles with smaller noses are more aesthetically pleasing, and it is ideal for females to have less prominent noses and for males to have more prominent ones in relation to their chins.39
Examination of lips: The purpose of this clinical examination is to assess the configuration of the lips, which includes lip length, thickness, competence and posture. It is performed when the patient is in a relaxed position and the lips are in repose. The distance between the upper and lower lips when in repose should ideally be 2–3 mm. If this distance is increased, the lips are considered to be incompetent (Fig 1.22A). Under normal circumstances, the length of the upper lip measures one-third, and the lower lip and the chin measure two-thirds of the lower facial height. Incompetent lips could be due to either short upper lip or lips of normal length but everted as a result of incisor protrusion. The average upper lip length is 22 ± 2 in males and 20 ± 2 in females. A short upper lip results in incompetence of lips in the absence of incisor procumbancy. Ethnic characteristics do influence the lip protrusion. However, apart from this, lip protrusion is influenced by the configuration of underlying bony structures, thickness of the soft tissues, position of the anterior teeth and the tone of the orbicularis oris muscle. At rest, in patients with increased overjet, the lower lip is positioned behind the upper incisors. This situation causes lower lip dysfunction and is self-aggravating as the trapped lower lip pushes the upper teeth forward, increasing the overjet further (Fig 1.22B). The vertical position of the lips in relation to the upper incisors should be assessed when the patient is in repose (at rest) and on smiling. Ideally, the incisor display at rest should be 2–4 mm. On smiling, a gingival display of 1–3 mm is considered to be more aesthetic. It should be noted that with increasing age, the incisal display tends to reduce.
Examination of chin: The configuration of the chin plays an important role in facial aesthetics. It should be assessed in patient’s NHP and relaxed facial musculature. The chin contour is evaluated with respect to the lower lip position and the configuration of the mentolabial fold (Fig 1.23). It is influenced by underlying bony structure and thickness and tone of the mentalis muscle. The chin position, both anteroposterior and vertical, is determined by the growth of the condyle, the displacement of the glenoid fossa and the vertical growth of the molar teeth.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses