Chapter 5
Is it periodontal disease?
Other conditions affecting the periodontal tissues
Introduction
Periodontal diseases are a group of inflammatory conditions of the periodontal tissues that are initiated by the accumulation of dental plaque at the gingival margin. As noted previously, collectively, these are extremely common conditions that will be encountered regularly on a day-to-day basis during routine practice. However, many other conditions can also affect the periodontal tissues, including conditions affecting the superficial gingival tissues and those that can cause destruction of the deeper periodontal tissues including the alveolar bone. These conditions all tend to be far less common than periodontal disease, but many of them may either reflect a serious underlying illness or have serious consequences in their own right. Thus, arguably the most important diagnostic decision to be made when assessing any periodontal pathology is “Is it periodontal disease?” In addition, because of its high prevalence, periodontal disease may often coexist with another, less common, condition of the periodontal tissues.
No clinician is expected to be intimately familiar with all of the possible conditions that may affect the periodontal tissues to allow an instant diagnosis. From a clinical standpoint, it is much more important that a clinician be able to identify the signs to arouse suspicion so that lesions may be investigated further, typically following referral to an appropriate specialist. Further investigation will involve clinical assessment together with additional investigation that, depending on the nature of the condition and the possible diagnoses considered, may require haematological assessment and/or biopsy.
A (noncomprehensive) list of many conditions that can affect the periodontal tissues is given in < ?xml:namespace prefix = "mbp" />
Table 5.1 Summary of conditions that may present in or affect the periodontal tissues
| Condition | Features | Basis of diagnosis |
|---|---|---|
| Diseases affecting mainly the gingival tissues | ||
| Viral infections, acute herpetic gingivostomatitis | Painful ulcerated gingivae and other mucosa tissues, pyrexia, malaise | Clinical features |
| Trauma (mechanical or chemical) | Ulceration, soreness | |
| Lichen planus | Persisting soreness, redness (desquamative gingivitis), white striae or erosive lesions affecting other mucosal tissues | |
| Vesiculobullous lesions (pemphigus, benign mucous membrane pemphigoid, etc.) | Sore mouth and ulcerating lesions; desquamative gingivitis; irregular ulcers, vesicles, and bullae on other mucosal tissues | |
| Leukaemia | Gingival redness and swelling, persisting bleeding (oozing) from the gingivae, ulceration, other signs of bruising, malaise, anaemia, and breathlessness | |
| Granulomatous diseases (sarcoidosis, Crohn’s disease, gingival tuberculosis) | Granular diffuse firm swelling of the attached gingivae, other mucosal lesions | |
| Wegener’s granulomatosis | Characteristic bright red swollen, granular “strawberry” gingivitis, pain ulceration; extraoral lesions; pulmonary symptoms | |
| Diseases affecting mainly the deeper periodontal tissues | ||
| Endodontic lesions | Periapical or furcation lesions, pain, swelling | |
| Central giant cell granuloma | Localized periodontal destruction, gingival swelling | Biopsy |
| Malignancy (primary carcinoma of the gingivae, secondary metastases of a distant carcinoma) | Periodontal destruction, pain, redness, and swelling of associated gingivae | |
| Langerhans cell histiocytosis | Single or multiple destructive bony lesions, often with periodontal pocketing | |
| Hyperparathyroidism | Multiple intrabony lesions | |
Table 5.2 Clinical features that may suggest that a periodontal condition is not the result of periodontal disease
Case 1
A 27-year-old male visited the dentist and complained of very sore gums, particularly in the upper teeth around the palatal region. He reported that this had started suddenly approximately 4 days earlier and that he had also felt slightly unwell and had a slightly raised body temperature. He was medically well and a smoker of approximately 15 cigarettes a day since he was 16 years old. He visited the dentist irregularly but had not previously noticed any problems from his gums, such as bleeding or pain.
On examination, he had generalized lymphadenopathy, and his gingivae appeared red and swollen. Some ulceration with a greyish slough was evident, particularly in the palatal gingivae in the upper teeth (
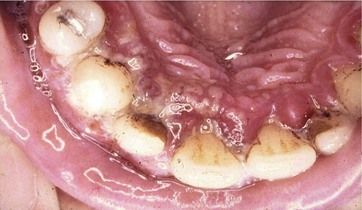
Fig 5.1 Suspected acute herpetic gingivostomatitis. The gingivae are red and inflamed, with diffuse ulceration seen at the gingival margins of the palatal aspects of the upper teeth.
After careful consideration of the clinical findings and history, a working diagnosis of acute herpetic gingivostomatitis was made. The patient was advised to take anti-inflammatory drugs, maintain fluid intake, and rest, and a follow-up appointment was scheduled in 2 weeks to assess the progress or resolution of the condition. At the 2-week follow-up, the patient reported that the condition had resolved within 3 days of his initial visit and that he was now well again and had no further oral symptoms. His plaque control was much improved, and although there were some signs of mild chronic gingivitis, there was no residual damage evident from the condition.
Distinguishing between acute herpetic gingivostomatitis and acute necrotizing ulcerative gingivitis (ANUG) can sometimes be a difficult challenge. Acute herpetic gingivostomatitis is extremely common, but ANUG is increasingly uncommon in those who are systemically healthy. Typically, with primary herpetic infection there will be other lesions affecting other parts of the oral mucosa, such as labial, buccal, and palatal mucosa, and even the dorsum of the tongue (
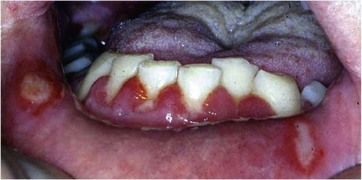
Fig 5.2 More typical appearance of acute herpetic gingivostomatitis. Gross redness and swelling of the gingivae, with discrete ulcers noted at the gingival margins of the lower central incisors, combined with characteristic ulcerative lesions on the labial mucosa.
In this case, the diagnosis was made by weighing the different features outlined, but it was prudent to arrange an early follow-up, which helped to confirm the diagnosis and allowed implementation of any periodontal care that might be required following the acute condition. Although it is also possible for other acute viral infections to present with similar features, these are also self-limiting, and it would not be appropriate to carry out any laboratory testing (e.g., serum antibody titres to herpes simplex virus or direct viral identification), which would not affect clinical management.
Case 2
A 57-year-old woman was referred to the periodontist with persisting red and sore gums around the lower teeth, particularly for the past year. She had had repeated visits with a dental hygienist for scaling and oral hygiene instruction but had not noticed any improvement in her condition. Her medical history revealed that she was hypertensive and had been taking propranolol to control her blood pressure for the past 7 years. She was otherwise fit and well and a nonsmoker.
The clinical appearance of the lower gingivae is shown in
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


