Chapter 17
Assessing the patient for implant placement
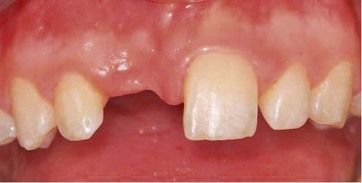
A patient presents having lost the upper right central incisor as a result of trauma (< ?xml:namespace prefix = "mbp" />
This chapter discusses the general factors in the assessment of patients for treatment with dental implants (
Table 17.1 Questions that need to be addressed in a general assessment for possible implant treatment
What are the patient’s expectations and can they be safely met?
The goal of assessment is to provide the information required to formulate a detailed individually tailored treatment plan that is likely to safely meet the realistic expectations of the patient. Both implant and nonimplant options for tooth replacement should be considered and presented to the patient. All treatment options must be evaluated and discussed in light of the general oral and systemic health of the patient. To make these decisions, it is necessary to undertake a thorough assessment that involves taking a detailed history, performing a thorough examination, and carrying out or requesting and then interpreting the results of appropriate investigations.
Does the treating team have the ability to meet the expectations of the patient?
 What training has been undertaken?
What training has been undertaken?
Implant dentistry is usually introduced during undergraduate dental training but often only in theory with little or no practical experience. This situation is changing as implant dentistry becomes more commonplace. Where regulation of dentistry exists, implant dentistry is regarded as an area of practice that requires additional appropriate postgraduate training both for the dentist and for the other members of the dental team.
 Is the appropriate equipment available and are the practice premises suitable to carry out implant dentistry?
Is the appropriate equipment available and are the practice premises suitable to carry out implant dentistry?
In addition to the high standards required for an effective, safe general dental practice, there are a number of additional requirements in order to undertake implant dentistry. For example, it is necessary to have the appropriate product-specific instruments such as screwdrivers available. If surgical implant dentistry is being carried out, additional instruments and equipment are required, such as a speed-reducing motor control unit, effective suction (with backup equipment to manage any malfunctions), and a range of implants and matched drills. The room used for operating must have effective lighting; enough space for layout of sterile instruments; and facility for proper surgical scrub, gowning, and gloving procedures. The ability to obtain detailed images of the jaw anatomy may require that computed tomography (CT) be used. CT should be easily accessible either in the practice or through a local referral. Intravenous sedation is a useful patient management adjunct in implant dentistry, and its use according to published standards requires dedicated equipment, premises, and training.
Is the patient able to give valid informed consent?
In order for the patient to make a decision about whether to proceed with implant treatment (or not), a number of key aspects of care need to be made clear, and these must be documented in the patient’s record. To assist this process, written information with images and/or accredited website addresses about implants are helpful, along with a detailed costed treatment plan and terms and conditions. Patients should also be informed about what the evidence base reveals about likely success rates of similar treatment carried out under similar conditions and by dentists with comparable levels of experience.
 What are the time-scales for the completion of treatment?
What are the time-scales for the completion of treatment?
Implant treatments tend to take longer than conventional dentistry. Patients need to be made aware of the likely number, frequency, and duration of appointments. They need to be advised that some treatments require periods of extended healing to allow for tissue maturation. Patients need this kind of information to plan how treatment can fit with occupational and lifestyle commitments.
 Will the patient be able to attend for maintenance?
Will the patient be able to attend for maintenance?
Prosthesis designs with a high anticipated maintenance requirement need to be planned with consideration of whether there is access to the appropriate level of dental follow-up care.
 Can the patient afford the treatment and maintenance?
Can the patient afford the treatment and maintenance?
Implant treatment is often costly. A clear statement of total changes, invoicing arrangements, and any fees for possible unexpected events is essential at the outset. In addition, financial arrangements and responsibilities for ongoing follow-up and maintenance as well as any warranty period must be made transparent. Some types of implant restoration, such as removable overdentures, predictably require ongoing adjustment or replacement of parts; patients need to understand this and the likely cost before committing to treatment.
 Might there be periods during treatment without tooth replacement and how might teeth be replaced temporarily?
Might there be periods during treatment without tooth replacement and how might teeth be replaced temporarily?
Although it is sometimes possible to restore implants with dental restorations at the time of implant placement, it is frequently necessary to use other means of tooth replacement for a period following extraction, bone grafting, or implant placement. The motivation for seeking implant treatment is often to avoid or do away with a removable denture, so patients need to be fully informed about any need to use removable prosthesis during treatment. This information is particularly pertinent for patients with no removable denture experience who aspire to make the transition from a failing dentition to fixed implant restorations. There are also circumstances in which the patient may be advised not to use any form of tooth replacement. This is typically for short periods following preparatory grafting or implant placement, with consequent aesthetic and functional compromise.
 What side effects from surgery are to be expected, and what are the more unusual but significant risks?
What side effects from surgery are to be expected, and what are the more unusual but significant risks?
The side effects experienced after dental implant surgery are highly dependent on the details of the surgery and the tolerance and healing capacity of the patient. The perception of pain, for example, is not solely related to the degree of physical trauma but also the result of complex subjective and objective interactions. However, patients should be warned to expect some pain and swelling. Additional warnings about common side effects may include skin or mucosal bruising due to haematoma and also the possibility of postoperative bleeding (
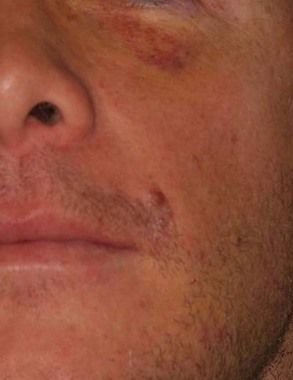
Fig 17.2 Infraorbital bruising 1 week following single implant placement with guided bone regeneration in the anterior maxilla.
There may be instances in which implant surgery carries a risk of more significa/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses