Chapter 1
Periodontal assessment
Introduction
Periodontal diseases manifest themselves in the majority of the adult population. Therefore, it is mandatory that all patients presenting to a general practitioner, regardless of the first impressions made of their periodontal health, are screened to identify those at risk of periodontal disease who will need a more comprehensive assessment prior to making an appropriate diagnosis. A failure to assess the periodontal health of a patient in any routine dental examination is potentially a negligent omission.
An assessment of the clinical signs and symptoms along with the medical history generally form the basis for establishing the diagnosis and assessing the severity of periodontal disease. From the first visit, the clinician should make an overall appraisal of the patient, including taking a full history. This will subsequently need updating at every visit, and certain historical information is crucial for both the diagnosis and to form the background for developing the most appropriate treatment plan for the individual patient.
What factors in the dental history might indicate periodontal disease is present?
Often, patients are unaware that they have periodontal problems, which may cause significant symptoms only at a relatively late stage when teeth become loose or painful. It is common for patients to complain that their gums bleed, particularly on brushing or flossing; however, many patients accept this as being a normal occurrence and not an indicator that more significant disease is present. As disease progresses, particular concerns may be conveyed that teeth are becoming loose, gaps are opening up, and the teeth are becoming uneven or the gum is receding. This may make the patient particularly anxious about losing teeth or about their appearance.
The patient may also have pain, which can present in a variety of ways, from a dull pain after eating or on chewing to a more acute pain of short duration particularly after cold food or drinks.
A dental history should aim to address the following areas:
• How long has the patient been aware of the problem? Has the nature of the symptoms changed and does anything either relieve these symptoms or make them worse?
• Has the patient been a regular attendee, and has he or she received regular hygiene as part of this? In particular, if the patient has been having regular periodontal treatment, it is important to elicit if this has been comprehensive (i.e., subgingival debridement over several visits and if local anaesthesia was used), when it was last performed, and whether the patient felt any improvement as a result of the treatment. This may allow a more accurate picture to be formed of how the individual has responded to previous regimes when considering the possible treatment options.
• The patient’s oral hygiene should be noted, including toothbrushing frequency and type of brush (powered or manual), if interdental brushes or floss are used daily, and type of toothpaste or any other oral hygiene aids (e.g., mouthwash type, interdental brushes, or water jet).
• If the patient had previous fixed or removable orthodontic treatment, the approximate dates of this should be noted. This might be of particular relevance if there are areas of gingival recession because certain tooth movement in the presence of thin bony and gingival architecture may need to be considered.
• If bleeding gums were one of the initial complaints, specific questions should be asked regarding if this is an occasional problem or whether it happens during each brushing, while eating, or even spontaneously.
• Is there a family history of periodontal problems? Specifically ask the patient whether he or she is aware of any immediate family members who have lost teeth through gum disease or have received regular periodontal treatment (rather than a routine scale and polish) at a young age (<40 years).
What is the relevance of a patient’s medical history to his or her periodontal care?
Many aspects of a patient’s medical history may be particularly relevant to his or her periodontal care. These are discussed further in subsequent chapters but may include the following:
• Medical problems can increase susceptibility to periodontal diseases (e.g., diabetes and HIV) and may, in whole or in part, explain the particular clinical presentation and disease severity.
• Medical problems can have periodontal and other oral manifestations (e.g., leukaemia and mucocutaneous disorders).
• Prescribed and nonprescribed medications can have oral and periodontal side effects (e.g., calcium channel blocker or phenytoin).
• Is periodontal infection a risk factor for systemic diseases or conditions that affect overall health? There is emerging scientific data on the association of periodontal disease with common systemic medical problems such as cardiovascular disease, stroke, diabetes, osteoporosis, and low-birth-weight infants. Future targeted anti-inflammatory therapies for patients with periodontal disease may modulate inflammation and, hence, lower risk for systemic conditions.
• Particular existing or previous medical conditions or medications may need specific precautions to be taken to avoid complications during or after treatment (e.g., antibiotic prophylaxis and patients on certain medications such as anticoagulants or bisphosphonates).
• Treating certain conditions may present additional risk to the dental team (e.g., communicable diseases) and may alter the way treatment is provided (e.g., not using ultrasonic instrumentation to avoid producing aerosol).
Why is it necessary to take a social history?
A social history should include details of habits such as tobacco use, including smokeless tobacco (see < ?xml:namespace prefix = "mbp" />
Table 1.1 Effects of smoking on periodontal health
A social history may also give information about the patient’s occupation that is both useful for interacting with the patient and may indicate specific dental issues (e.g., wind instrument player and importance of aesthetics in a job). It can also provide information about the patient’s ability to attend appointments regularly and identify issues such as stress in a patient’s life.
Clinical periodontal examination
The examination should start with a general extra- and intraoral examination of the soft tissues, temporomandibular joint (TMJ), and lymph nodes to look at the mouth and surrounding tissues as a whole.
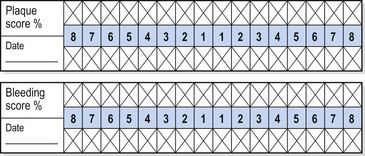
The periodontal tissue examination should be systematic, starting with an appraisal of gingival colour and contour, oral hygiene, and aesthetics. Oral hygiene and gingival inflammation can be measured in a number of ways using both full mouth scoring systems and partial scoring systems (
Table 1.2 Examples of partial and full mouth plaque scoring indices
| Full plaque recording system | Partial plaque scoring system |
|---|---|
| Plaque score (O’Leary) | Plaque index (Löe and Silness) |
| Debris index (Grace and Smales) | |
| Turesky plaque index |
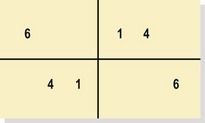
Fig 1.2 Ramfjord teeth are used as a representation of the full mouth for evaluation of plaque (FDI notation: 16, 21, 24, 36, 41, 44).
What are the methods for screening for periodontal disease?
Periodontal screening for epidemiological study of the treatment needs of populations was developed and introduced in 1978 by the World Health Organization as the Community Periodontal Index of Treatment Needs (CPITN). Subsequent modification and development of CPITN for use as a periodontal screening method in general dental practice to identify “risk patients” has occurred. The Basic Periodontal Examination (BPE), developed in the United Kingdom and widely used throughout Europe, is an example of this and is very similar to the Community Periodontal Index and Periodontal Screening and Recording indices used worldwide. The BPE is a simple and rapid screening tool that is used to indicate the level of examination needed and to provide basic guidance on treatment need.
Employing a screening tool for periodontal disease is useful because with experience it can be carried out very rapidly (1 or 2 min) and therefore implemented for all patients. Because the majority of patients seen in a general practice setting may not have established periodontitis, a screening method allows the rapid identification of those with periodontal disease who will require more detailed periodontal assessment.
What do I need to carry out a BPE and how often should it be recorded?
A special probe called the WHO probe is required, and the key features are described in
• For patients with codes 0, 1, or 2, the BPE should be recorded at least annually.
• For patients with BPE codes of 3 or 4, more detailed periodontal charting is required.
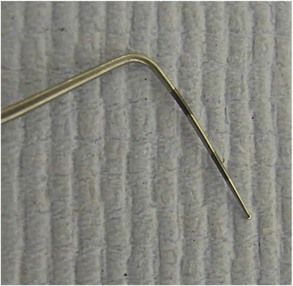
Fig 1.3 The WHO-C (clinical) probe. The key elements of this probe are a ball end with a 0.5-mm diameter, a black band at 3.5–5.5 mm, and a second black band at 8.5–11.5 mm.
BPE cannot be used to assess the response to periodontal therapy because it does not provide information about how sites within a sextant change after treatment. To assess the response to treatment, probing depths should be recorded at six sites per tooth pre- and post-treatment.
How do I record a BPE screening examination?
• The dentition is divided into six sextants: upper right (17 to 14), upper anterior (13 to 23), upper left (24 to 27), lower right (47 to 44), lower anterior (43 to 33), and lower left (33 to 37). NB third molars are not included for scoring.
• All teeth in each sextant are examined (with the exception of third molars) in adults.
• For a sextant to qualify for recording, it must contain at least two teeth. (If only one tooth is present in a sextant, the score for that tooth is included in the recording for the adjoining sextant.)
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses