Chapter 4
Periodontal Microsurgery
HISTORICAL PERSPECTIVE
References to magnification date back 2,800 years, when simple glass meniscus lenses were described in ancient Egyptian writings. In 1694, Amsterdam merchant Anton van Leeuwenhook constructed the first compound-lens microscope. Magnification for microsurgical procedures was introduced to medicine during the late 1800s. In 1921, Carl Nylen, who is considered the father of microsurgery, first used the binocular microscope for ear surgery (Dohlman 1969). It was not until 1960, when Jacobsen and Suarez obtained 100% patency in suturing 1-mm-diameter blood vessels for anastomosis, that the surgical microscope gained wide acceptance in medicine (Barraquer 1980).
Apotheker & Jako (1981) first introduced the microscope to dentistry in 1978. During 1992, Carr published an article outlining the use of the surgical microscope during endodontic procedures. In 1993, Shanelec & Tibbetts (1998) presented a continuing-education course on periodontal microsurgery at the annual meeting of the American Academy of Periodontology. This led to centers devoted to teaching periodontists and other dentists periodontal microsurgery.
Belcher wrote an article in 2001 summarizing the benefits and potential usages of the surgical microscope in periodontal therapy. Although Belcher and several other periodontists view the addition of the microscope as an invaluable tool in periodontal therapy, it has been cautiously accepted by the periodontal profession as a whole.
PERIODONTAL APPLICATIONS
The operating microscope offers three distinct advantages to periodontists: illumination, magnification, and increased precision of surgical skills (Belcher 2001). The synergy of improved illumination and increased visual acuity enables the increased precision of surgical skills. Collectively, these advantages can be referred to as the microsurgical triad (Fig. 4.1).
Among many basic surgical principles, several are germane to periodontal surgery. Eliminating dead space, tissue handling, removal of necrotic tissue and foreign materials, closure with sufficient but appropriate tension, and immobilization of the wound are important surgical goals in periodontal therapy (Johnson & Johnson 1994, p. 9). The surgical operating microscope and appropriate microsurgical technique afford surgeons a more realistic chance of achieving these goals.
In periodontics, the surgical operating microscope, though useful in most areas of periodontal therapy, is particularly useful in mucogingival surgery, root preparation, and crown-lengthening procedures.
Microsurgical techniques are especially beneficial to mucogingival procedures. As mentioned, principles of wound healing require minimal dead space. The microscope enables clinicians to use smaller needles, sutures, and instruments, and precisely position tissues and stabilize the mending tissues.
Root preparation is an important modality in periodontal therapy. Lindhe & Nyman (1984) have suggested the success of periodontal therapy is due to the thoroughness of debridement of the root surface. Data show that surgical access improves the ability to remove calculus (Cobb 1996). Furthermore, research demonstrates that root preparation is enhanced when performed under illumination (Reinhardt et al. 1985). The surgical microscope provides fiber optic lighting and magnification for calculus removal.
Most published articles embracing the benefits of magnification in dentistry have been anecdotal (Campbell 1989). However, two articles do show enhanced clinical benefits of magnification. Leknius & Geissberger (1995) have shown a direct relationship between magnification and significantly enhanced performance of prosthodontic dental procedures.
A recently published article concluded that performing root-coverage techniques microsurgically versus macrosurgically substantially improved the vascularization of connective tissue grafts and the percentage of additional root coverage (Burdhardt & Lang 2005). There is a lack of studies in dentistry comparing the benefits of crown lengthening or other surgical procedures via standard versus microsurgical methods. Yet, it seems logical that if magnification is beneficial in prosthetics and root coverage, the surgical microscope, with its magnification, would aid practitioners in crown lengthening, root preparation, and other periodontal surgical procedures.
Figure 4.1. Microsurgical triad.
PERIODONTAL INSTRUMENTATION
Magnification enables dentists to use smaller instrumentation with more precision. Although the variety of microsurgical instrumentation designed for periodontal therapy is vast, the instrumentation can be divided into the following subgroups: knives, retractors, scissors, needle holders, tying forceps, and others.
The knives most commonly used in periodontal microsurgery are those used in ophthalmic surgery: blade breaker, crescent, minicrescent, spoon, lamella, and scleral knives (Fig. 4.2). Common characteristics of these knives are their extreme sharpness and small size. This enables precise incisions and maneuvers in small areas (Fig. 4.3).
The blade-breaker knife has a handle onto which a piece of an ophthalmic razor blade is affixed. This allows for infinite angulations of the blade. This knife is often used in place of a no. 15 blade.
The crescent knife can be used for intrasulcular procedures. It is available with one-piece handles or as a removable blade. It can be used in connective tissue graft procedures to obtain the donor graft, to tunnel under tissue, and to prepare the recipient site.
Figure 4.2. Periodontal microsurgical knives: 1, blade breaker; 2, crescent; 3, minicrescent; 4, 260° spoon; 5, lamella, and 6, sclera.
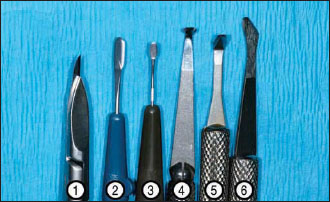
Figure 4.3. Spoon knife shown in sulcular undermining incision.
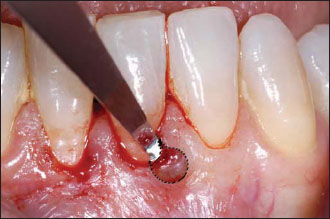
The spoon knife is beveled on one side, allowing the knife to track through the tissue adjacent to bone. It is frequently used in microsurgical procedures to undermine tissue, enhancing the placement of a connective tissue graft.
Retractors and elevators have been downsized. Scissors such as the micro–vannas tissue scissors are used for removal of small fragments of tissue. Needle holders are also downsized from sizes designed for conventional periodontal surgery. Tying forceps are an essential component of two-hand microsurgical tying. They are available in two general styles: platform and nonplatform. Several designs of both needle holders and tying forceps are available.
Microsurgical instrumentation can be made with titanium or surgical stainless steel. Titanium instruments tend to be lighter, but are more prone to deformation and are usually more expensive. Stainless-steel instruments are prone to magnetization, but there is a greater number and wider variety of them.
Needles and sutures
As mentioned earlier, basic surgical techniques are used to eliminate dead space, close a wound with sufficient but appropriate tension, and immobilize a wound (Johnson & Johnson 1994, p. 9). The appropriate combin/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


