Principles of Surgery
James R. Hupp
Human tissues have genetically determined properties that make their normal responses to injury predictable. Because of this predictability, principles of surgery that help to optimize the wound healing environment have been developed through basic and clinical research. This chapter presents the evidence-based principles of surgical practice that have been found to be most successful.
Developing a Surgical Diagnosis
Most of the important decisions concerning a surgical procedure should be made long before the administration of anesthesia. The decision to perform surgery should be the culmination of several diagnostic steps. In the critical thinking analytic approach the surgeon first identifies the various signs and symptoms and relevant historical information; then, using available patient and scientific data and logical reasoning based on experience, the surgeon establishes the relationship between the individual problems.
The initial step in the presurgical evaluation is the collection of accurate and pertinent data. This is accomplished through patient interviews; physical, laboratory, and imaging examinations; it also includes the use of consultants, when necessary. Patient interviews and physical examinations should be performed in an unhurried, thoughtful fashion. The surgeon should not be willing to accept incomplete data such as a poor-quality radiograph, especially when it is probable that additional data might change decisions concerning surgery.
For a good analysis, data must be organized into a form that allows for hypothesis testing; that is, the dentist should be able to consider a list of possible diseases and eliminate those unsupported by the patient data or evidence-based science. By using this method, along with the knowledge of disease probabilities, the surgeon is usually able to reach a decision about whether surgery is indicated.
Clinicians must also be thoughtful observers. Whenever a procedure is performed, they should reflect on all aspects of its outcome to advance their surgical knowledge and to improve future surgical results. This procedure should also be followed whenever a clinician is learning about a new technique. In addition, a clinician should practice evidence-based dentistry by evaluating the purported results of any new technique by weighing the scientific merit of studies used to investigate the technique. Frequently, scientific methods are violated by the unrecognized introduction of a placebo effect, observer bias, patient variability, or use of inadequate control groups.
Basic Necessities for Surgery
Little difference exists between the basic necessities required for oral surgery and those required for the proper performance of other aspects of dentistry. The two principal requirements are (1) adequate visibility and (2) assistance.
Although visibility may seem too obvious to mention as a requirement for performing surgery, clinicians often underestimate its importance, especially when the unexpected occurs. Adequate visibility depends on the following three factors: (1) adequate access, (2) adequate light, and (3) a surgical field free of excess blood and other fluids.
Adequate access not only requires the patient’s ability to open the mouth widely but also may require surgically created exposure. Retraction of tissues away from the operative field provides much of the necessary access. (Proper retraction also protects tissues being retracted from being accidentally injured, for example, by cutting instruments.) Improved access is gained by the creation of surgical flaps, which are discussed later in this chapter.
Adequate light is another obvious necessity for surgery. However, clinicians often forget that many surgical procedures place the surgeon or assistant in positions that block chair-based light sources. To correct this problem, the light source must continually be repositioned, or the surgeon or assistant must avoid obstructing the light, use more than one overhead light, or use a headlight.
A surgical field free of fluids is also necessary for adequate visibility. High-volume suctioning with a relatively small tip can quickly remove blood and other fluids from the field.
As in other types of dentistry, a properly trained assistant provides invaluable help during oral surgery. The assistant should be sufficiently familiar with the procedures being performed to anticipate the surgeon’s needs. Performance of good surgery is extremely difficult with no or poor assistance.
Aseptic Technique
Aseptic technique includes minimizing wound contamination by pathogenic microbes. This important surgical principle is discussed in detail in Chapter 5.
Incisions
Many oral and maxillofacial surgical procedures necessitate incisions. A few basic principles are important to remember when performing incisions.
The first principle is that a sharp blade of the proper size should be used. A sharp blade allows incisions to be made cleanly, without unnecessary damage caused by repeated strokes. The rate at which a blade dulls depends on the resistance of tissues through which the blade cuts. Bone and ligamental tissues dull blades more rapidly than does buccal mucosa. Therefore, the surgeon should change the blade whenever the scalpel does not seem to be incising easily.
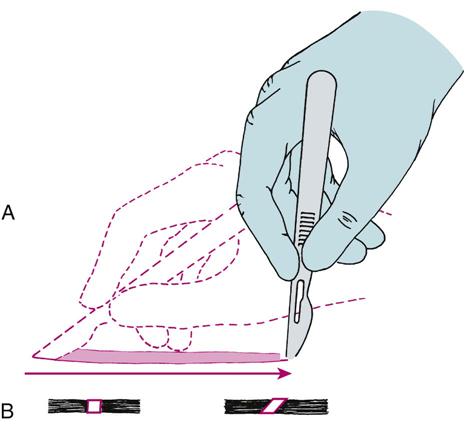
The second principle is that a firm, continuous stroke should be used when incising. Repeated, tentative strokes increase the amount of damaged tissue within a wound and the amount of bleeding, thereby impairing wound healing and visibility. Long, continuous strokes are preferable to short, interrupted ones (Fig. 3-1, A).
The third principle is that the surgeon should carefully avoid c/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses