Chapter 3
Periodontal diagnosis
Systemic factors
It is well-recognized that taking a full medical history from a patient is an important part of diagnosis and assessment. Taking a medical history requires a systematic approach to obtaining information about the patient’s past medical history. This can be carried out using a standard pro forma. If preferred, the patient can be asked to complete the pro forma him- or herself, and this can be checked by the clinician. The relevance of the medical history in periodontal diagnosis and treatment is mainly due to the following:
• The medical history may affect the management of the patient in some way.
• The medical history may affect the susceptibility, presentation, and progression of periodontal disease.
• The medical history may identify a condition that can directly manifest itself in the periodontal tissues.
Conditions that may affect periodontal management
Conditions that may affect the management of the patient include those that might adversely affect the ability to successfully carry out treatment, including surgical procedures. The major examples of such conditions include bleeding disorders and other blood dyscrasias where there is an obvious risk of uncontrolled bleeding following any type of periodontal treatment. In addition, any patient who is severely immunocompromised may be at increased risk of infection postoperatively.
It has long been suggested that patients with valvular heart disease, prosthetic cardiac valves, and those with a previous history of infective endocarditis may be at risk of infective endocarditis following the bacteraemia that is inevitably caused by any periodontal procedure, including both nonsurgical and surgical instrumentation. This has resulted in the suggestion that these patients should be provided with antibiotic prophylaxis prior to carrying out any invasive procedure. However, current guidelines for the United Kingdom have failed to find sufficient evidence that dental procedures are a cause of infective endocarditis or that the routine use of antibiotic prophylaxis regimes is helpful. As such, antibiotic prophylaxis prior to invasive dental procedures is not currently recommended.
Bisphosphonates are anti-bone resorptive drugs that are widely used for the management of osteoporosis, but they are also used in less common conditions such as neoplastic bone disease (e.g., the presence of bony secondary metastases from carcinomas). These drugs include alendronate, zoledronate, and pamidronate. Most patients take these drugs orally, but some patients, particularly those with neoplastic bone disease, may be given intravenous bisphosphonates. It is now recognized that bisphosphonate therapy results in the risk of the very serious complication of osteonecrosis of the jaw, which may occur, for example, following tooth extractions. This is particularly the case for those who are being treated with intravenous bisphosphonate therapy. Therefore, although people taking oral bisphosphonates can be managed normally, in those with a history of intravenous bisphosphonate therapy, tooth extractions are best avoided if possible, and where necessary, it may be appropriate to refer to a specialist centre for management.
Medical conditions may also affect periodontal management in many other ways. For example, they may have an important influence on a patient’s ability to regularly attend periodontal treatment, may impair manual dexterity and the ability to carry out oral hygiene procedures (e.g., in those with severe rheumatoid arthritis), and in some cases may also influence goals and expectations of periodontal treatment outcomes. In addition, knowledge of a patient’s past medical history may be invaluable during dental treatment if a medical emergency should arise.
Many medical conditions can occasionally manifest themselves in the gingival or periodontal tissues. The ability to distinguish between periodontal disease and the periodontal manifestations of another disease is discussed in < ?xml:namespace prefix = "mbp" />
Systemic aetiological factors in periodontal disease
From the epidemiology of periodontal disease, it is clear that susceptibility to periodontal disease varies considerably among patients, independent of the level of plaque control. Systemic factors have often been called secondary modifying factors of disease because in the presence of plaque, they may modify the host response, resulting in increased susceptibility to destructive disease or altered inflammatory response to the plaque. In general, these systemic factors can be categorized as those that predominantly affect the presentation of gingival inflammation and those that affect disease progression and susceptibility to periodontitis. Some of these conditions, such as type 2 diabetes mellitus, are extremely common, whereas there are a number of very rare, typically genetically inherited conditions that may also have profound effects on the presentation of periodontal disease.
Systemic factors predominantly affecting the gingival tissues
Pregnancy
It is well-recognized that the gingivae may show increased bleeding during pregnancy. Pregnancy gingivitis is an increase in gingivitis seen during pregnancy, which is thought to be due largely to the increased vascular blood flow associated with elevated progesterone levels. Pregnancy gingivitis in its mild form may simply be manifest as profuse gingival bleeding on minor trauma such as tooth brushing and even when eating. More typically, the gingivae show increased swelling, redness, and are extremely haemorrhagic (
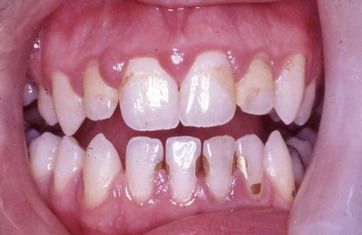
Fig 3.1 Swollen and inflamed gingivae, most marked here in the upper incisor regions, in pregnancy gingivitis. (Corsodyl staining of composite restorations in lower incisors is also evident.)
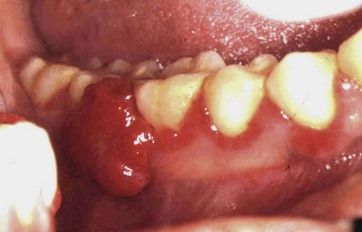
Occasionally, the inflammation may be sufficiently severe as to result in the formation of a localized pyogenic granuloma known as a pregnancy epulis. The pregnancy epulis is a localized inflammatory swelling that is extremely haemorrhagic and can often become quite large—for example, growing sufficiently to interfere with the occlusion (
Other hormonal factors
Less marked increased gingival bleeding, similar to pregnancy gingivitis, may be seen in patients taking the contraceptive pill and in girls at puberty, and occasionally patients report marked variations in gingival bleeding during their menstrual cycle. Again, the emphasis is on establishment and maintenance of good plaque control measures together with professional cleaning and careful oral hygiene instruction.
There is little evidence that pregnancy gingivitis or other hormonally related gingival inflammation results directly in increased periodontal breakdown. However, the establishment of poor periodontal health, such as may occur during pregnancy, may well be associated with risk of future periodontitis. Once it has become established, gingival inflammation is much more difficult to resolve than if there has been maintenance of good gingival health from the outset.
Drug-induced gingival enlargement
Drug-induced gingival enlargement, also known as drug-induced gingival overgrowth, is caused by three distinct classes of drugs:
The general feature of drug-induced gingival enlargement is a variable degree of enlargement of the gingivae, particularly focused at the dental papillae, which is associated with the dose of the drug and the level of plaque and inflammation present. The mechanisms of action of these drugs to cause gingival enlargement are not fully understood, and it is not clear whether the same mechanisms account for the gingival response in each class of drug.
 Phenytoin-induced gingival enlargement
Phenytoin-induced gingival enlargement
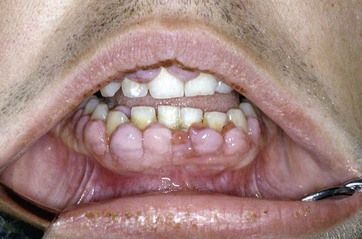
Phenytoin is an anticonvulsant drug used mainly for the treatment of epilepsy. Many patients with epilepsy take phenytoin, but it is not usually the first drug of choice for epilepsy management. Although there are sporadic cases of gingival enlargement reported with the use of other anticonvulsant drugs, notably lamotrigine, these cases appear to be very rare and the gingival enlargement is mainly a specific side effect of phenytoin. The clinical features of phenytoin-induced gingival enlargement are principally fibrous swelling of the gingivae, particularly emanating from the dental papillae, which may have a fibrous, pink, and uninflamed appearance (
Although there are many reports of marked spontaneous improvement following withdrawal of the drug and replacement with a different anticonvulsant therapy, considerable caution needs to be exercised when considering this treatment given the serious implications of loss of control of seizures in the patient whose epilepsy is currently well controlled. In severe cases, the dental practitioner may need to liaise closely with the attending neurologist in order to discuss whether substitution of the drug with another anticonvulsant would be appropriate and beneficial.
 Ciclosporin
Ciclosporin
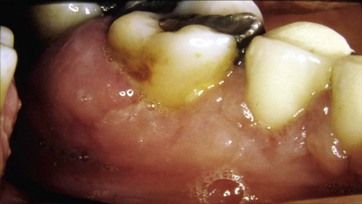
Ciclosporin is an immunosuppressant drug that is particularly widely used for the suppression of graft rejection following transplantation of organs, most notably kidneys but also any other organ transplant procedure. The gingival enlargement seen with ciclosporin is often less notably fibrous than that of phenytoin-induced gingival enlargement and is reportedly responsible for the most severe gingival overgrowth of all three classes of drugs implicated (
 Calcium channel blocking drugs
Calcium channel blocking drugs
The calcium channel blocking drugs are very widely used medications for the control of hypertension and also in the management of coronary artery disease. Their primary action is to cause vasodilation. In recent years, calcium channel blockers (including nifedipine, amlodipine, felodipine, verapamil, and diltiazem) have become one of the most widely prescribed classes of drugs for the primary management of hypertension. The reported prevalence of gingival enlargement associated with the calcium channel blockers is highly variable, ranging between 5 and 40% of patients being affected in different studies according to the different criteria used for diagnosis. The appearance of the enlarged gingivae is often less fibrous and more vascular than that involving phenytoin, and it is also often of less severity (
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses