3
Cases Suitable for Treatment with Removable Appliances
Historically in the UK, removable appliances were used to treat a wide range of malocclusions, often to an acceptable standard when used by an experienced and skilled operator. However, it is now recognised that fixed appliances are able to achieve far superior results when used by operators trained in their use, and these have superseded removable appliances in many cases.
That said, the use of removable appliances is an extremely effective and efficient method of treatment in specific situations. These situations mostly relate to mixed dentition/interceptive orthodontics. They are very seldom indicated for definitive treatment of a malocclusion.
The majority of examples in this chapter will relate to upper removable appliances (URAs), although two examples of the use of a lower removable appliance (LRA) will be included. LRAs are less well tolerated by the patient than URAs because they encroach on tongue space. Also, it is more difficult to achieve good retention of a LRA because the undercuts on the lower molars are on the lingual side of the teeth, rather than the buccal side as for the upper molars. Often, the arrowheads of Adams’ clasps on lower molars and premolars do not have any undercuts into which to engage, significantly reducing the retentive ability of the clasps.
- Have knowledge of the types of malocclusion that may be successfully treated with removable appliances
- Be able to design removable appliances for treatment of a number of specific malocclusions
- Understand the rationale behind specific design features
- Be able to write out a laboratory prescription for your technician
Expansion
In general terms, transverse expansion of the upper arch may be undertaken to correct unilateral or bilateral posterior crossbites in the following circumstances:
- There is a lateral displacement of the mandible on closure.
- Space is required in the upper arch to relieve crowding or aid in overjet reduction.
- The teeth that are to be moved are tipped palatally, i.e. bodily movement is not needed.
It is not always necessary to correct a posterior crossbite under other circumstances. However, when it is decided that crossbite correction is needed, it is always essential to assess:
- How much expansion is required to correct a crossbite
- Whether these tooth movements may be achieved
- The stability of the result.
Relapse of a posterior crossbite correction may leave the patient with a cusp-to-cusp relationship of the buccal teeth and, hence, induce a lateral mandibular displacement on closure. This is the reason why URAs should only be used to correct posterior crossbites in specific situations.
Design 1: Midline Expansion Screw (Figure 3.1)
Figure 3.1 Laboratory prescription for a URA that will provide symmetrical expansion of the upper arch.
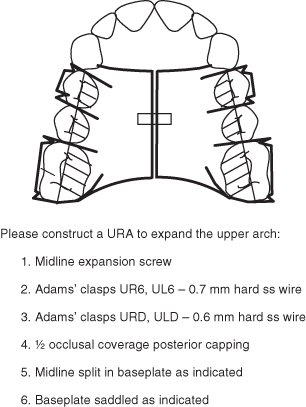
Indications
- Bilateral narrowing of the maxillary arch in which the teeth are tipped palatally
This is often associated with a cusp-to-cusp buccal segment transverse relationship in the retruded contact position (RCP), leading to a lateral mandibular displacement into the inter-cuspal position (ICP) on closure. This could occur as a result of a digit-sucking habit.
- When a mandibular displacement on closure is present, clinically the patient presents with a unilateral posterior cross-bite on the side to which the mandible is displacing and a lower centre-line shift to the same side.
- The aim of the treatment is to expand the upper arch so that the cusp-to-cusp relationship is removed and the mandibular displacement eliminated.
- The points above illustrate why it is not always appropriate to correct a unilateral crossbite with ‘unilateral’ or asymmetric expansion (see Design 2 below and Figure 3.2). Therefore, it is essential that the presence of any mandibular displacement is detected prior to the design of the appliance.
Figure 3.2 Laboratory prescription for a URA that will provide asymmetrical expansion of the upper arch.
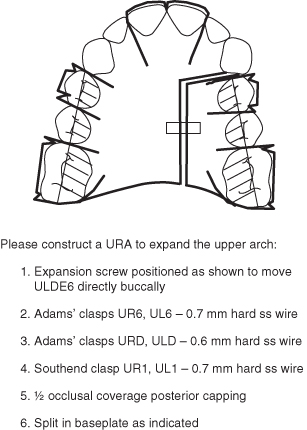
Rationale: Correcting a posterior crossbite may help relieve crowding. Also, correcting a posterior crossbite that has been caused by a mandibular displacement during the early mixed dentition hopefully will enable subsequent permanent teeth to erupt into the RCP, so ensuring that any future orthodontic treatment is more straightforward. Other suggested adverse consequences of a lateral mandibular displacement on closure include tooth wear and the possibility of a young patient’s mandible and hence dentition growing in an asymmetric pattern.
Contra-Indications
- The buccal teeth are already buccally tipped (flared)
Rationale:
- The action of the removable appliance is to tip the teeth buccally to correct the transverse discrepancy. If the teeth are already tipped buccally, then only a limited amount of tooth movement is possible.
- As the teeth are tipped buccally, it causes the palatal cusp to ‘drop down’ and this has the effect of propping the bite open. This should be avoided especially in patients who have increased vertical dimensions.
- If the teeth are already buccally tipped, the presence of a posterior crossbite indicates a significant skeletal discrepancy between the maxilla and the mandible in the transverse dimension, and a removable appliance is not capable of correcting significant skeletal discrepancies.
- A bilateral posterior crossbite also indicates a significant transverse skeletal discrepancy and removable appliances should not be used for expansion in such cases.
Design Features (Figure 3.1)
Active:
Midline expansion screw.
Retention:
Adams’ clasps on upper first permanent molars (0.7 mm hard ss wire) and upper first premolars (0.7 mm wire) or upper first primary molars (0.6 mm wire).
Anchorage:
Reciprocal: both sides of the arch will move by the same amount in a buccal direction.
Baseplate:
Midline split to allow expansion.
1/2 occlusal coverage posterior capping to disengage occlusion and allow free movement of upper teeth.
- Because of occlusal interferences between the maxillary and mandibular teeth, failure to disclude the teeth in a well-inter-digitated occlusion often results in concomitant expansion of the lower arch, with no correction of the transverse discrepancy between the two
- Posterior capping will encourage the incisors to erupt and so will increase the overbite. If the overbite is already increased and a further increase is contra-indicated, then a flat anterior biteplane (FABP) may be included instead of posterior capping
Fitting and Activation:
See Chapter 4.
Design 2: Asymmetric Expansion Screw (Figure 3.2)
Indications
- Expansion of the upper arch where it is apparent that the narrowing of the maxillary arch is unilateral and there is a displacement of the mandible on closure
Once again, expansion may help relieve crowding and will hopefully enable subsequent permanent teeth to erupt into the RCP, so ensuring that any future orthodontic treatment is more straightforward (Figure 3.3).
Figure 3.3 Intra-oral views, pre-treatment (a–c) and post-treatment (d-f), of a patient who underwent expansion of the upper arch with a URA in order to correct the crossbite of URCDE6. A Z-spring was used to correct the crossbite of UR2. Note the improvement in lower centre-line discrepancy. Also note that the patient requires no further orthodontic intervention as the permanent teeth have now erupted into a very acceptable position.
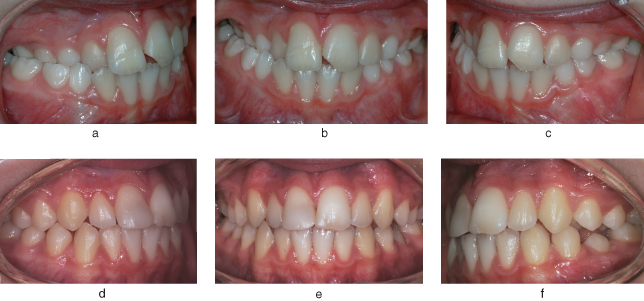
Contra-Indications
As above.
Design Features (See Figure 3.2)
Active:
Expansion screw, offset toward the side that requires expansion.
Retention:
Adams’ clasps on upper first permanent molars (0.7 mm hard ss wire) and upper first premolars (0.7 mm hard ss wire) or upper first primary molars (0.6 mm hard ss wire).
Southend clasp on upper central incisors (0.7 mm hard ss wire).
Anchorage:
Because more teeth are included in the anchor unit, i.e. the teeth that do not need to be moved, there will be more expansion of the smaller unit – the teeth that do need moving. However, it is inevitable that some expansion of the teeth in the anchor unit will occur.
Baseplate:
Split in baseplate to separate the teeth that need to be moved from the anchor unit.
1/2 posterior capping to disengage occlusion and allow free movement of upper teeth (see above).
Fitting and Activation:
See Chapter 4.
Moving Teeth Around the Arch
Before use of fixed appliances became more common, removable appliances were often used to retract canines into the space created by the extraction of the first premolars as part of the treatment of Class II division 1 malocclusions. These days, because fixed appliances give such superior results, removable appliances are more commonly used simply to re-open space for the eruption of teeth by moving adjacent teeth around the arch, often in the mixed dentition.
Teeth can be moved mesially or, more commonly, distally, depending on requirements, but often space will need to be created first by the extraction of teeth, e.g. primary canine teeth.
Design 1: Use of Palatal Finger Springs (Figure 3.4)
Figure 3.4 Laboratory prescription for a URA to retract UR2, UL1 and UL2 to recreate space to allow the eruption of UR1.
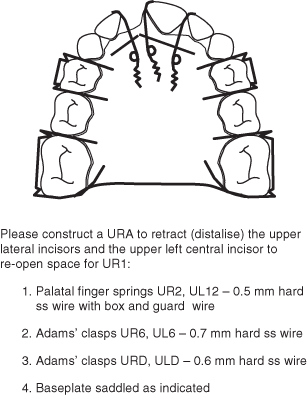
Indications
- Re-creation/redistribution of space, e.g. following loss of space for the eruption of a central incisor whose eruption has been impeded by a supernumerary tooth, and where the contra-lateral central incisor and the lateral incisors have tipped mesially into the unerupted central incisor space
Rationale: An unerupted tooth will only erupt if there is enough room for it to do so and once two-thirds to three-quarters of its root is formed. The teeth adjacent to a space will always tip into it. Therefore, the erupted incisors in this type of case are usually mesially tipped. The distal tipping caused by the springs serves to upright the teeth again, so achieving a more normal angulation at the same time as recreating the space. In this situation, it is often necessary to extract the primary canine teeth bilaterally to provide space into which to move the lateral incisor teeth. - Retraction (distal movement) of canines that are in the line of the arch
This should only be undertaken in rare and very specific cases where there is a small amount of space distal to the permanent canine teeth once they have erupted (up to 2–3 mm) and the canines are mesially tipped.
Rationale: This situation may be seen in cases where the upper permanent lateral incisors are microdont and the canines have tipped forward into the space. Tipping them distally again will create space distal to the upper laterals to allow composite build-ups on these teeth and so improve aesthetics.
Contra-Indications
- Retraction of canines following the extraction of first premolar teeth
Rationale: In general, canines should not be retracted into the space created by the extraction of the first premolar teeth using a URA, as this causes the crown of the canine to become distally angulated. This is unaesthetic and the root apex is left in its original position, leading to relapse. These cases should be treated using fixed appliances, which can control the crown angulation and root position. - Retraction of teeth that are upright or distally angulated prior to treatment
Rationale: The same principles apply as for retracting canines following extraction of premolar teeth. - Retraction of buccally displaced canines
Rationale: Palatal finger springs will push the tooth further from the line of the arch.
Design Features of a URA to Recreate Space for the Unerupted UR1 (See Figure 3.4)
Active:
Palatal finger springs on the erupted central incisor and lateral incisors (0.5 mm wire) with box and guard wire (see Chapter 2).
Retention:
Adams’ clasps on the upper first permanent molars (0.7 mm hard ss wire) and upper first premolars (0.7 mm hard ss wire) or upper first primary molars (0.6 mm hard ss wire).
Anchorage:
Care needs to be taken with the anchorage in this case. The reaction to the force applied to the incisor teeth to move them distally will be movement of the anchor teeth and the appliance mesially. Activating all three finger springs simultaneously will run the risk of losing anchorage and so disrupting the buccal segment relationship (it will become more Class II, i.e. move forward) and increasing the overjet.
Baseplate:
The acrylic on the fit surface, around the finger springs, should be boxed out to ensure uninhibited activation of the springs (see Chapter 2). The collets distal to the incisors should be removed to allow distal movement of these teeth. If the overbite is increased, then an FABP may be included as appropriate.
Fitting and Activation:
See Chapter 4.
Design 2: Use of Buccal Canine Retractors (Figure 3.5)
Figure 3.5 Laboratory prescription for a URA to retract buccally placed upper permanent canine teeth.
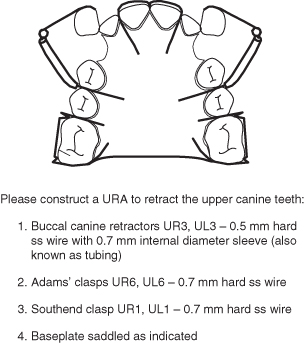
Indications
- Retraction of buccally displaced canines that are mesially tipped
Buccal canine retractors are rarely used now, as canines usually erupt buccally only if the arch is crowded. If the arch is crowded, then space will need to be created prior to alignment of the canines. As the canines erupt around the same time as the second premolars, the patient is likely to be in the permanent dentition and, therefore, fixed appliances following the extraction of first premolars is the preferred option in most cases.
Contra-Indications
- Patients with a decreased buccal sulcus depth
Rationale: The design of the spring means that it sits in the buccal sulcus. If there is inadequate sulcus depth the spring is more likely to cause ulceration in the buccal sulcus and, consequently, discomfort for the patient leading to an understandable lack of compliance. - Canines are upright or are already distally tipped
See above comments in relation to palatal finger springs.
Design Features (See Figure 3.5)
Active:
Buccal canine retractors on the upper permanent canine teeth (0.5 mm wire sleeved in ss tubing with an interior diameter of 0.7 mm).
Retention:
Adams’ clasps on upper first permanent molars (0.7 mm hard ss wire) and a Southend clasp on upper permanent central incisors (0.7 mm hard ss wire).
Anchorage:
Care needs to be taken with the anchorage in this case. The reaction to the force applied to the canine teeth to move them distally will be movement of the anchor teeth and the appliance mesially. Canines are large teeth and need more force to move them than the incisors. Therefore, anchorage must be monitored carefully to ensure that it is not lost.
Baseplate:
If the overbite is increased, then an FABP may be included as appropriate in order to decrease it.
Colleting distal to the upper lateral incisors and mesial to the upper first premolars needs to remain in place to prevent any unwanted drifting of these teeth.
Fitting and Activation:
See Chapter 4.
Design 3: Use of Orthodontic Screws (Figure 3.6)
Figure 3.6 Laboratory prescription for a URA to distalise UL6.
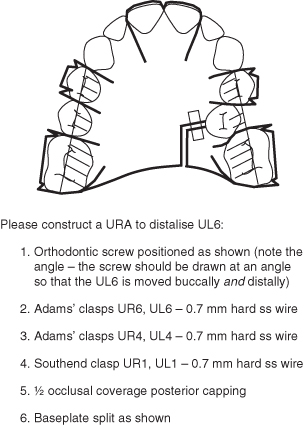
Indications
- For distal movement of blocks of teeth
For example, slight shortage of space (2–3 mm) for alignment of an upper or lower second premolar tooth due to mesial migration of the first molar on that side following early loss of the second primary molar.
Rationale: The advantage of using a screw in this situation is that the teeth that are being moved can also be included as part of the retention for the appliance.
Contra-Indications
- More than 2–3 mm of space is required
- Space is required bilaterally
Rationale: Both the above situations will put too much stress on the anchorage, usually resulting in an increase in overjet (if used in the upper arch). This may be overcome by mov/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


