Temporomandibular Joint Abnormalities
Susanne Perschbacher
Disease Mechanism
Disorders of the temporomandibular joint (TMJ) include all abnormalities that interfere with the normal form or function of the TMJ. These disorders include developmental abnormalities that can result in an abnormal form of the osseous or soft tissue structures of the joint. Other disorders are acquired, such as dysfunction of the articular disc and associated ligaments and muscles, joint arthritides, inflammatory lesions, trauma, and neoplasms.
Clinical Features
A wide variety of conditions can cause TMJ disorders that manifest with an extensive assortment of clinical features. Dysfunction of the joint is the most common disorder and is most likely to manifest with pain in the TMJ or ear or both, headache, muscle tenderness, joint stiffness, clicking or other joint noises, reduced range of motion, locking, and subluxation. Careful clinical assessment can help identify which structures are likely contributing to the joint dysfunction. For instance, pain to palpation of the muscles of mastication and headaches suggest a myofascial pain disorder, clicking or popping sounds in the joint and locking or reduced range of motion are often associated with disc abnormalities, and crepitus and pain over the joint itself commonly indicate arthritic involvement. A higher incidence of joint dysfunction has been reported in females, especially in their reproductive years, although the reason for this preponderance is unclear. In most cases, the clinical signs and symptoms are transitory, and often treatment is not indicated beyond patient reassurance and education. However, a small percentage (5%) of patients has severe dysfunction (e.g., severe pain, marked functional impairment, or both), which requires a thorough diagnostic workup, including diagnostic imaging, before treatment.
Other disorders of the TMJ are less common. A neoplasm may manifest with swelling of the joint region, whereas redness and heat over the joint may indicate an inflammatory lesion. Developmental abnormalities are most likely to be unilateral and manifest with facial asymmetry. Changes in occlusion may also be a sign of an abnormality in one or both of the TMJs.
Imaging Anatomy of the Temporomandibular Joint
A thorough understanding of the anatomy and morphology of the TMJ is essential so that a normal variant is not mistaken for an abnormality. Each joint is formed by articulating components of the mandible and temporal bones. The TMJs are unique because although they constitute two separate joints anatomically, they function together as a single unit as the mandibular components are part of one bone. An articular disc composed of fibrocartilage is interposed between the osseous structures of each joint. Retrodiscal tissues help maintain the normal position of the disc. A fibrous capsule lined with synovial membrane surrounds and encloses the joint. The synovial tissue is present on non–force-bearing surfaces and secretes synovial fluid, which lubricates the joint. The muscles of mastication allow movement of the condyle, whereas ligaments limit the extent of movement.
Mandibular Component
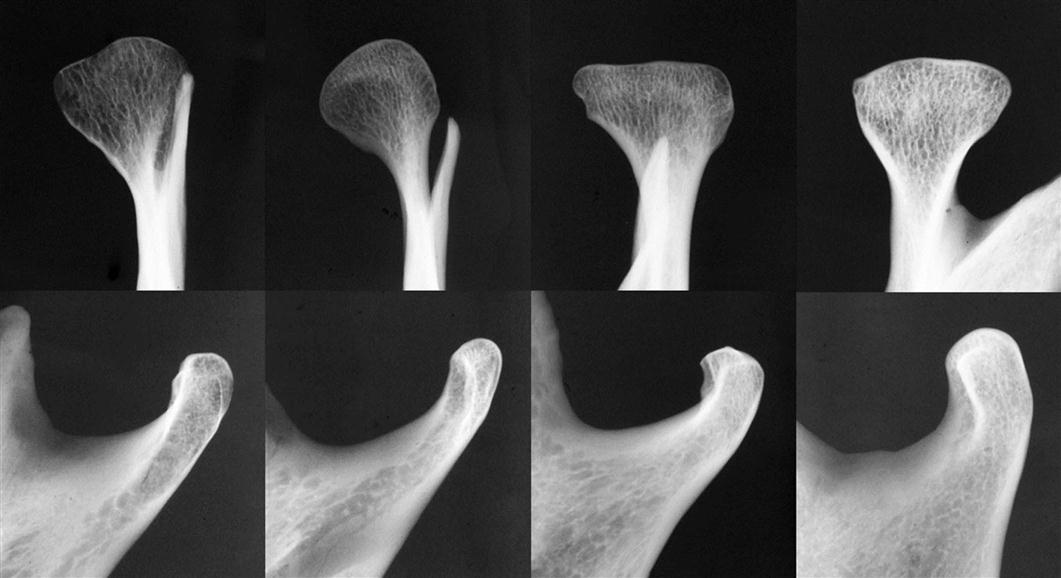
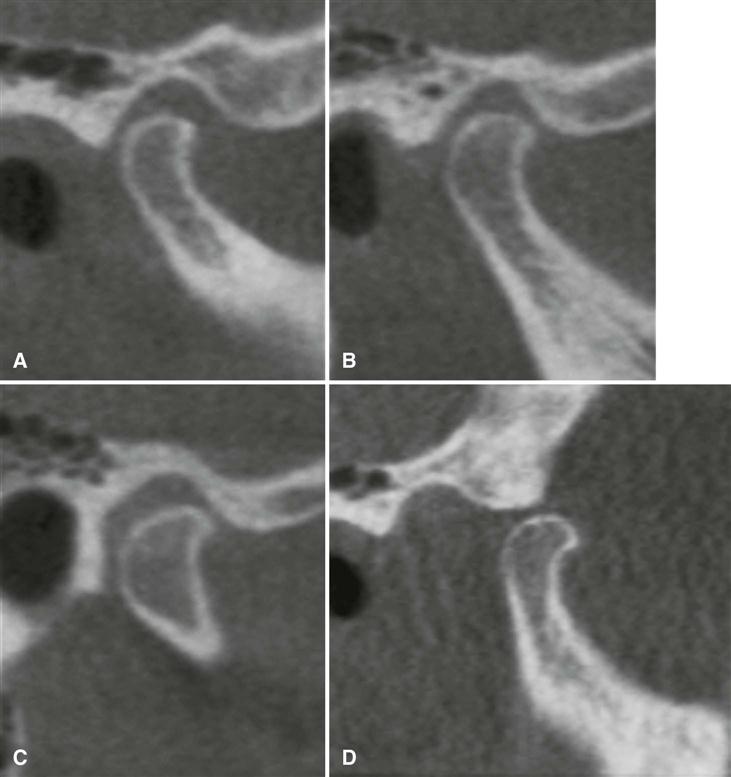
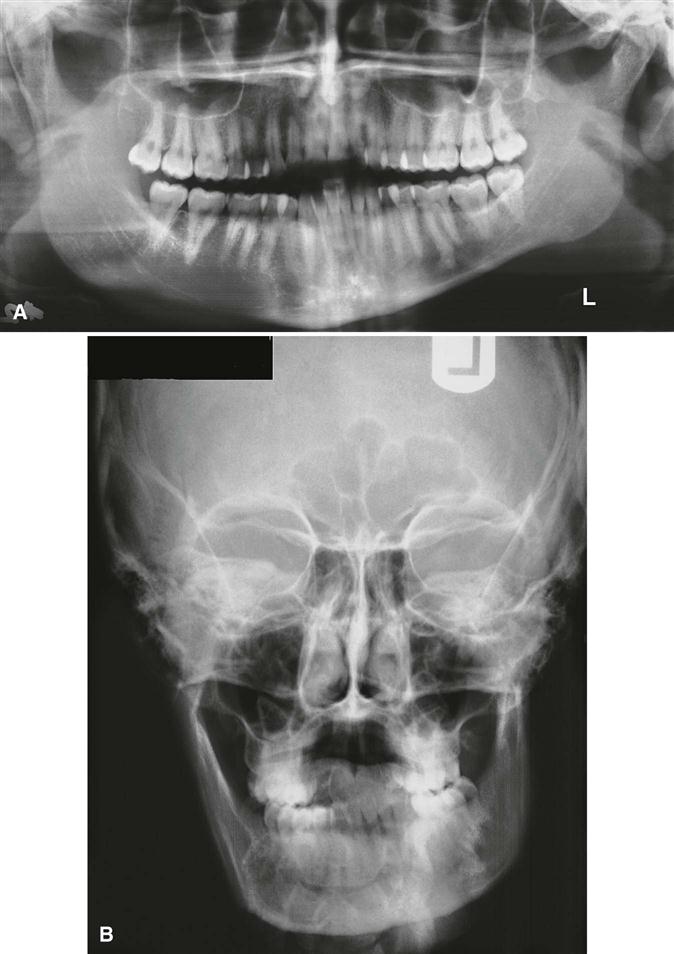
The mandibular condyle forms the mandibular component of the TMJ. The condyle is a bony ellipsoid structure connected to the mandibular ramus by a narrow neck (Fig. 27-1). The condyle is approximately 20 mm long mediolaterally and 8 to 10 mm thick anteroposteriorly. The shape of the condyle varies considerably; the superior aspect may be flattened, rounded, or markedly convex, whereas the mediolateral contour usually is slightly convex. These variations in shape may cause difficulty with radiographic interpretation; this underlines the importance of understanding the range of normal appearance (Fig. 27-2). The extreme ends of the condyle are called the medial and lateral poles. The long axis of the condyle is formed between these poles and is slightly rotated on the condylar neck so that the medial pole is angled posteriorly, forming an angle of 15 to 33 degrees with the sagittal plane. The two condylar axes typically intersect near the anterior border of the foramen magnum in the axial or horizontal plane of the skull.
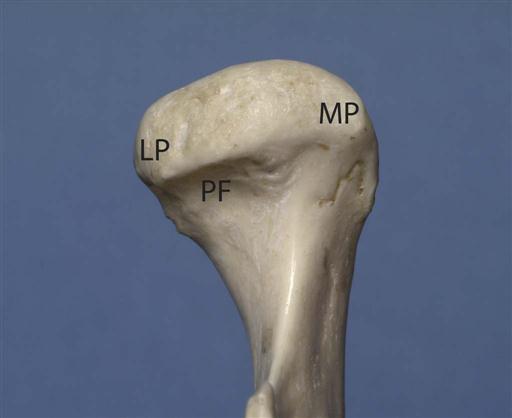
Most condyles have a pronounced ridge oriented mediolaterally on the anterior surface, marking the anteroinferior limit of the articulating area. This ridge is the upper limit of the pterygoid fovea, a small depression on the anterior surface at the junction of the condyle and condylar neck, which is the attachment site of the superior head of the lateral pterygoid muscle. The ridge should not be mistaken for an osteophyte (spur), which is a sign of degenerative joint disease (DJD).
Although the mandibular and temporal components of the TMJ are calcified by 6 months of age, complete calcification of cortical borders may not be completed until 20 years of age. As a result, radiographs of condyles in children may show little or no evidence of a cortical border. In the absence of disease, the cortical borders in adults are visible in the diagnostic image. However, a layer of fibrocartilage covering the condyle is not visible.
Temporal Component
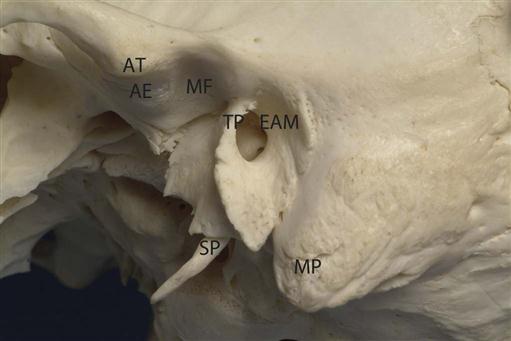
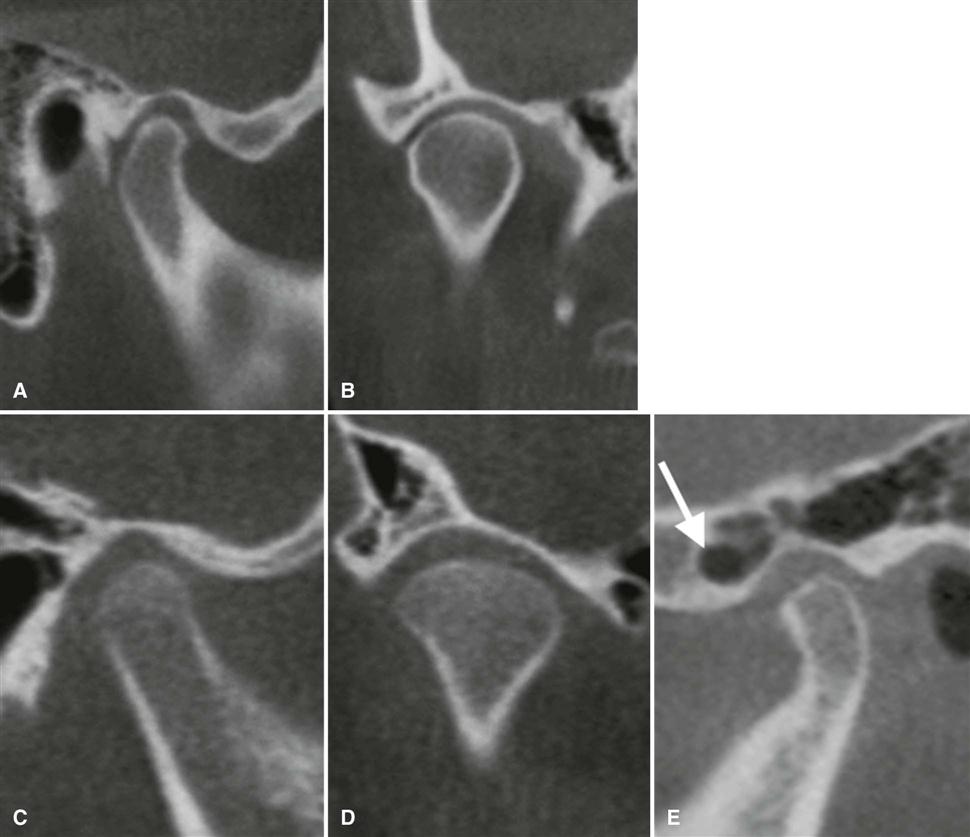
The articular component of the temporal bone is formed by the inferior aspect of the squamous process. It is composed of the glenoid or mandibular fossa posteriorly and the articular eminence and tubercle anteriorly (Fig. 27-3). Similar to the condyle, the mandibular fossa is covered with a thin layer of fibrocartilage. The posterior surface of the articular eminence is convex in shape, and its most inferior aspect is called the summit or apex. In a normal TMJ, the roof of the fossa, the posterior slope of the articular eminence, and the summit of the eminence form an “S” shape when viewed in the sagittal plane. The squamotympanic fissure and its medial extension, the petrotympanic fissure, form the posterior limit of the fossa. The middle portion of the roof of the fossa forms a small portion of the floor of the middle cranial fossa, and only a thin layer of cortical bone separates the joint cavity from the intracranial subdural space. The spine of the sphenoid forms the medial limit of the fossa. Fossa depth varies, and the development of the articular eminence relies on functional stimulus from the condyle. For example, the mandibular fossa is very flat and underdeveloped in patients with micrognathia or condylar agenesis. Young infants also lack a definite fossa and articular eminence; the fossa and articular eminence develop during the first 3 years and reach a mature shape by age 4 years, although the cortices may remain indistinct until adulthood (Fig. 27-4, C and D).
All aspects of the temporal component may be pneumatized with small air cells derived from the mastoid air cell complex (Fig. 27-4, E). Pneumatization of the articular eminence is seen radiographically in approximately 2% of patients.
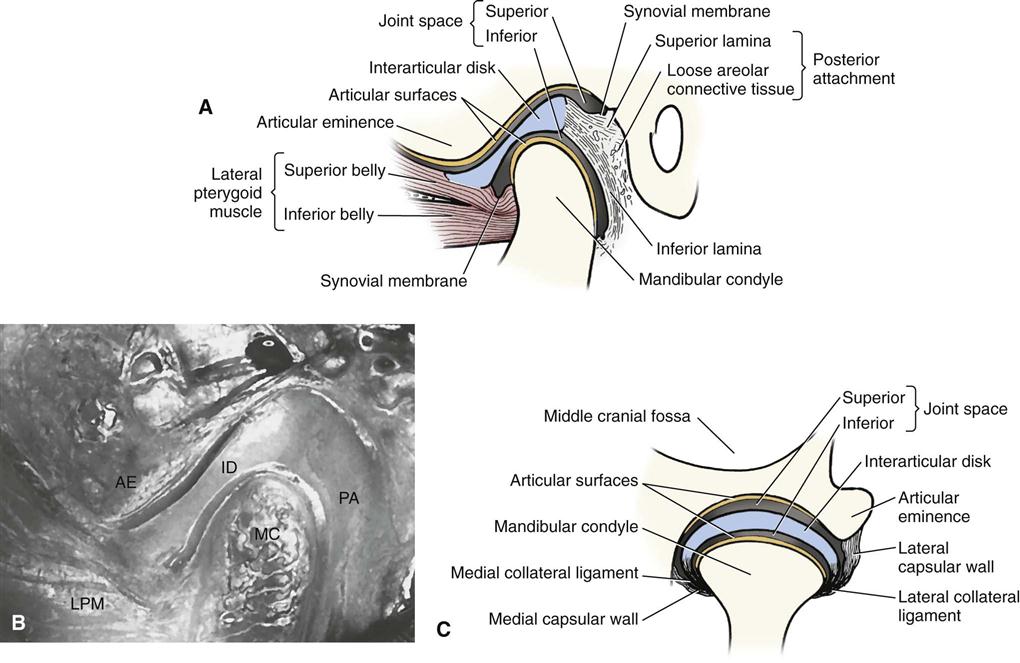
Interarticular Disc
The interarticular disc (meniscus) is composed of avascular fibrous connective tissue and is positioned between the condylar and temporal components. The disc divides the joint cavity into two compartments, called the inferior (lower) and superior (upper) joint spaces, which are located below and above the disc, respectively (Fig. 27-5). A normal disc has a biconcave shape with a thick anterior band, thicker posterior band, and a thin middle part. The disc is also thicker medially than laterally. In a normal joint, the thin central portion serves as the articulating portion of the disc, acting as a cushion between the convex articulating surfaces of the condyle and articular eminence. The posterior band sits at the superior aspect of the condyle, or slightly anterior to it, in the 11 o’clock position. The periphery of the disc attaches to the inner surface of the joint capsule. The anterior band is also thought to be attached to some fibers of the superior head of the lateral pterygoid muscle. The posterior band attaches to the retrodiscal tissues. The disc and retrodiscal tissues are collectively called the soft tissue components of the TMJ.
During mandibular opening, as the condyle rotates and translates downward and forward, the disc also moves forward and rotates so that its thin central portion remains between the articulating convexities of the condylar head and articular eminence. The disc attaches to the condylar poles laterally and medially, helping to ensure passive movement of the disc with the condyle. On mandibular closing, this process reverses, with the disc moving back with the condyle into the mandibular fossa.
Retrodiscal Tissues (Posterior Disc Attachment)
The retrodiscal tissues consist of superior and inferior lamellae enclosing a region of loose vascular tissue, which is often referred to as the bilaminar zone. The superior lamina, which is rich in elastin, inserts into the posterior wall of the mandibular fossa. The superior lamina stretches and allows the disc to move forward with condylar translation and then allows for the smooth recoil of the disc posteriorly as the mandible closes. The inferior lamina attaches more tightly to the posterior surface of the condyle. As the condyle moves forward, the retrodiscal tissues expand in volume, primarily as a result of venous distention, to fill the space created behind the condyle. The retrodiscal tissues are well innervated and may be the source of pain when the posterior attachment becomes trapped between the condyle and articular eminence in cases of anterior disc displacement.
Temporomandibular Joint Bony Relationships
Joint space is a general term used to describe the radiolucent area between the condyle and temporal component seen in diagnostic images. This term should not be confused with the terms superior joint space and inferior joint space described earlier, which refer to soft tissue spaces above and below the disc. The radiographic joint space contains the soft tissue components of the joint. The condylar position within the fossa can be determined by examining the dimensions of the radiographic joint space viewed on corrected lateral images. A condyle is positioned concentrically when the anterior and posterior aspects of the radiolucent joint space are uniform in width; the condyle is retruded when the posterior joint space width is less than the anterior; and it is protruded when the posterior joint space is wider than the anterior. However, because the radiographic outline of the glenoid fossa and the condyle do not match similar to a smooth ball-and-socket joint, the dimensions of the joint space often vary from medial to lateral aspects of the normal joint (Fig. 27-6).
The diagnostic significance of mild or moderate condylar eccentricity is unclear; condylar eccentricity is seen in one third to one half of asymptomatic individuals and is not a reliable indicator of the soft tissue status of the joint, particularly because the shape of the condylar head is not concentric to the shape of the fossa. Markedly eccentric condylar positioning usually represents an abnormality. For example, inferior condylar positioning (widened joint space) may be seen in cases involving fluid or blood within the joint, and superior condylar positioning (decreased joint space or no joint space, with contact of osseous components) may indicate loss, displacement, or perforation of the disc or its attachments. Marked posterior condylar positioning is seen in some cases of anterior disc displacement, and pronounced anterior condylar positioning may be seen when there has been destruction of the articular eminence, such as in juvenile idiopathic arthritis (JIA).
Condylar Movement
The condyle undergoes complex movement during mandibular opening. Downward and forward translation (sliding) of the condyle occurs where the superior surface of the disc slides against the articular eminence; at the same time, a hingelike, rotatory movement occurs with the superior surface of the condyle against the inferior surface of the disc. The extent of normal condylar translation varies considerably. In most individuals, at maximal opening, the condyle moves down and forward to the summit of the articular eminence or slightly anterior to it (see Fig. 27-6). The condyle typically is found within a range of 2 to 5 mm posterior and 5 to 8 mm anterior to the crest of the eminence. Reduced condylar translation, in which the condyle has little or no downward and forward movement and does not leave the mandibular fossa, is seen in patients who clinically have a reduced degree of mouth opening. Hypermobility of the joint may be suspected if the condyle translates more than 5 mm anterior to the eminence. If a superior movement also occurs anterior to the articular eminence, anterior locking or dislocation of the condyle may occur.
Application of Diagnostic Imaging
Imaging of the TMJ may be necessary to supplement information obtained from the clinical examination, particularly when an osseous abnormality or infection is suspected, conservative treatment has failed, or symptoms are worsening. Diagnostic imaging also should be considered for patients with a history of trauma, significant dysfunction, alteration in range of motion, sensory or motor abnormalities, or significant changes in occlusion. TMJ imaging is not indicated for joint sounds if other signs or symptoms are absent or for asymptomatic children and adolescents before orthodontic treatment. The purposes of TMJ imaging are to evaluate the integrity and relationships of the hard and soft tissues, confirm the extent or stage of progression of known disease, and evaluate the effects of treatment. There is often poor correlation between the severity of findings on TMJ imaging and the severity of the patient’s symptoms or dysfunction. For instance, severe degenerative changes may be noted on an imaging study, but the patient has only mild discomfort, or vice versa. The clinician must correlate the imaging information with the patient’s history and clinical findings to arrive at a final diagnosis and plan the management of the underlying disease process.
Temporomandibular Joint Imaging Modalities
Several variables must be considered when selecting the type of imaging technique to use, including the specific clinical problem to be addressed, whether imaging of hard or soft tissues is desired, the strengths and limitations of the modalities being considered, the cost of the examination, and the radiation dose. Both joints should be imaged during the examination for comparison. Images of the osseous structures of the joints may be obtained using panoramic radiography, cone-beam computed tomographic (CBCT) imaging, or multidetector computed tomographic (MDCT) imaging. The soft tissues of the joints are best imaged with magnetic resonance imaging (MRI). The application of these techniques to TMJ diagnosis is discussed further in the following sections.
Osseous Structures
Panoramic Projection
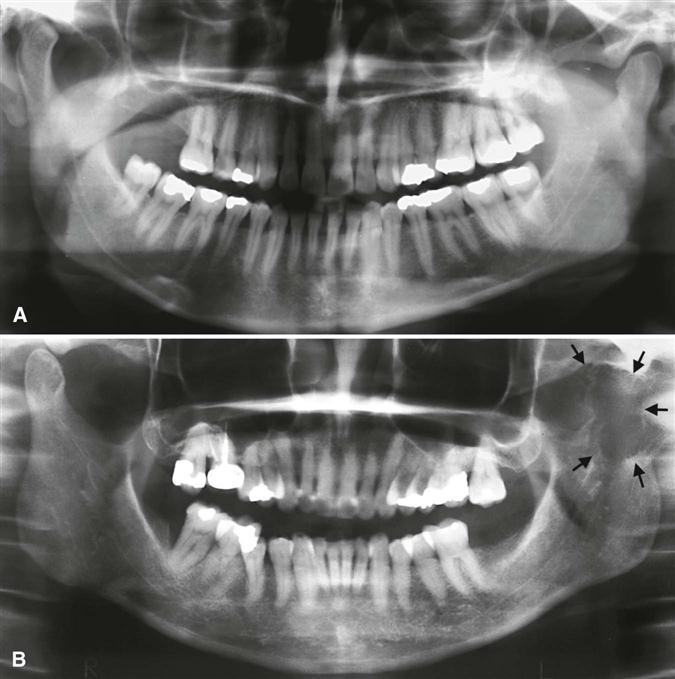
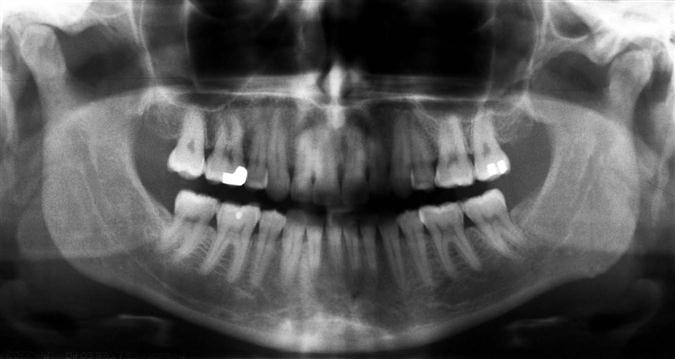
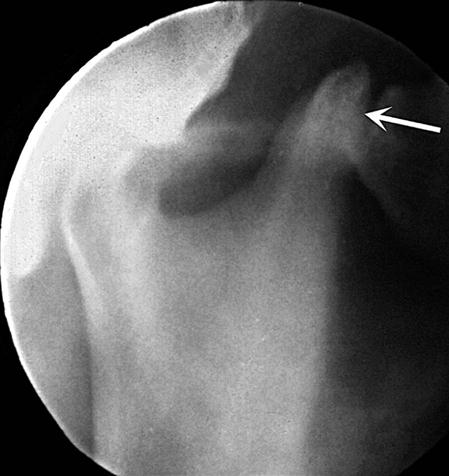
The panoramic image is a useful tool for providing a broad overview of the TMJ and surrounding structures. It serves the purpose of allowing the clinician to rule out gross disease, and for some patients, it is the only imaging required before conservative therapy is initiated. Gross osseous changes in the condyles may be identified, such as asymmetries, extensive erosions, large osteophytes, tumors, or fractures (Fig. 27-7). The panoramic projection also provides a means of comparing left and right sides of the mandible and can reveal odontogenic diseases and other disorders that may be the source of TMJ symptoms. However, no information about condylar position or function is provided because the mandible is partly opened and protruded when this image is exposed. Also, mild osseous changes may be obscured, and only marked changes in articular eminence morphology can be seen as a result of superimposition by the skull base and zygomatic arch. For these reasons, when a detailed assessment of the joint structures is desired, the panoramic view should be supplemented. The TMJ programs available on some panoramic machines do not provide the views required because of thick image layers and oblique, distorted views, and more advanced modalities are indicated.
Cone-Beam Computed Tomographic Imaging
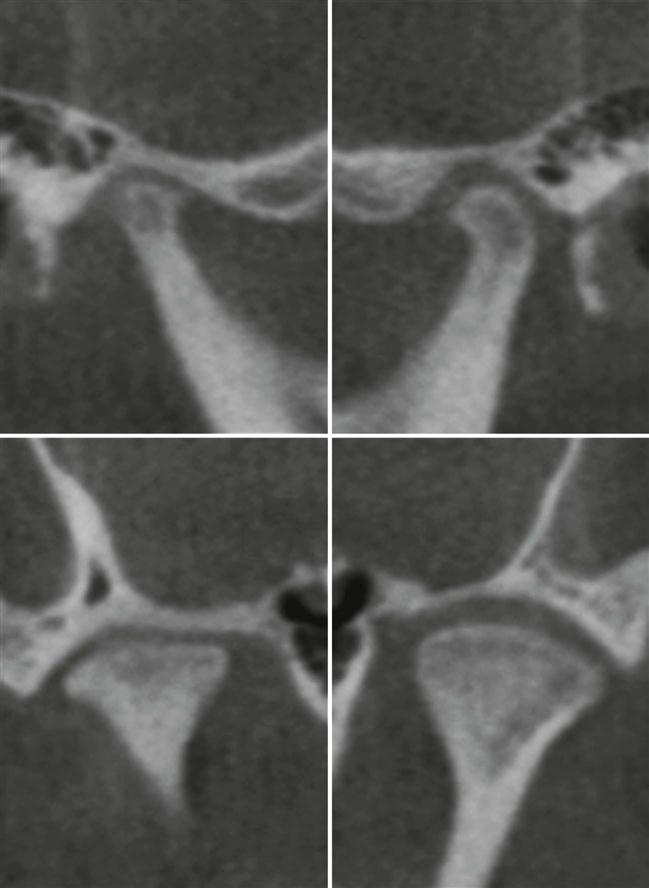
CBCT imaging produces volumetric imaging that allows reconstruction of thin section views in multiple, customizable planes. Thin sections allow the structures of the joints to be assessed without superimposition of surrounding anatomy. Classically, the joints are viewed in coronal and sagittal planes, corrected along the long axes of the condylar heads (Fig. 27-8). These views provide the least distorted representation of the condylar and temporal components and their relationship to each other. Panoramic and three-dimensional reformats also can be created, which are useful for assessing skeletal asymmetries or other osseous deformities. A CBCT scan is usually acquired with the patient’s mouth in the closed position. Some machines allow low-resolution scans to be done in open mouth or other positions (see Chapter 12) to evaluate range of motion. CBCT imaging has the advantage of reduced radiation dose to the patient compared with MDCT. This reduced dose makes CBCT imaging ideal for imaging of osseous changes associated with DJD. CBCT imaging is also useful for determining the presence and extent of ankylosis and neoplasms, imaging fractures, evaluating complications from the use of polytetrafluoroethylene or silicon sheet implants, and examining for heterotopic bone growth. Soft tissue components including the discs cannot be adequately visualized with CBCT imaging. Metallic implants in or around the joints may create streak artifacts, which can obscure the joint structures.
Multidetector Computed Tomographic Imaging
MDCT imaging (see Chapter 14) is capable of providing the same information as CBCT imaging but additionally allows some visualization of the soft tissues. This additional visualization is required only in a few situations, such as when a neoplasm is suspected to extend beyond the osseous structures. The articular disc is not adequately visualized with this modality. Also, MDCT imaging exposes the patient to higher radiation doses than CBCT imaging.
Soft Tissue Structures
The most common indication for soft tissue imaging is when clinical findings suggest disc displacement with symptoms such as TMJ pain and dysfunction and when symptoms do not respond to conservative therapy. Soft tissue imaging may also be required to supplement osseous imaging in rare cases where infection or a neoplasm is suspected. As with any other modality, imaging should be prescribed only when the anticipated results are expected to influence the treatment plan. MR imaging is the modality of choice for visualizing the disc and other soft tissues of the TMJ.
Magnetic Resonance Imaging
MRI uses a magnetic field and radiofrequency pulses rather than ionizing radiation to produce multiple digital image slices (see Chapter 14). This imaging modality does not subject the patient to any ionizing radiation dose. Because MRI can provide a contrast between different soft tissues, this technique can be used for imaging the articular disc and other soft tissue components of the joint. Joint effusions can also be detected with MRI. MRI imaging displays the osseous structures of the TMJ but not in detail comparable to CBCT or MDCT imaging.
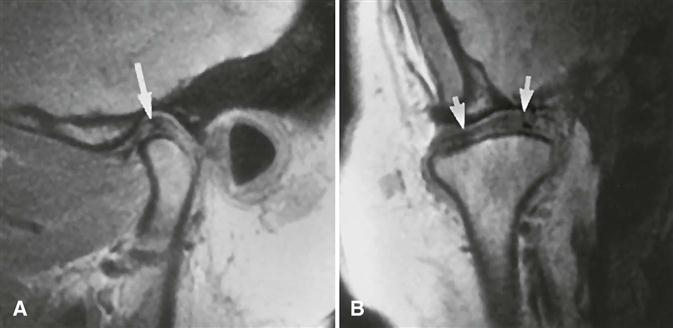
MRI allows construction of images in the sagittal and coronal planes without repositioning the patient (Fig. 27-9). These images usually are acquired in open and closed mandibular positions with use of surface coils to improve image resolution. Sagittal slices should be oriented perpendicular to the condylar long axis. The examinations usually are performed with use of T1-weighted, proton density–weighted, or T2-weighted pulse sequences. Proton density–weighted images are slightly superior to T1-weighted images in demonstrating osseous and discal tissues, whereas T2-weighted images demonstrate inflammation and joint effusion. Motion MRI studies during opening and closing can be obtained by having the patient open the jaw in a series of incremental distances and using rapid image acquisition (“fast scan”) techniques.
MRI is contraindicated in patients who have pacemakers or some other implanted devices, intracranial vascular clips, or metal particles in vital structures. Orthodontic hardware may create artifacts over the dental region but are not a contraindication to imaging the joints. Some patients may be unable to tolerate the procedure because of claustrophobia or an inability to remain motionless.
Abnormalities of the Temporomandibular Joint
Developmental Abnormalities
Disease Mechanism
Developmental abnormalities are the result of disturbance in the normal growth and development of the TMJ. The end result is abnormalities in the form or size of the joint components, most commonly the mandibular condyle. Because the condylar articular cartilage is considered the growth center for the mandible, disturbances involving this cartilage can result in altered growth of the mandibular condyle, ramus, body, and alveolar process on the affected side.
Condylar Hyperplasia
Disease Mechanism.
Condylar hyperplasia is a developmental abnormality that results in enlargement and occasionally deformity of the condylar head; this may have a secondary effect on the mandibular fossa as it remodels to accommodate the abnormal condyle. Proposed etiologic factors include hormonal influences, trauma, infection, heredity, intrauterine factors, and hypervascularity. The mechanism may be overactive cartilage or persistent cartilaginous rests; the thickness of the entire cartilaginous and precartilaginous layers is increased. This condition usually is unilateral and may be accompanied by varying degrees of hyperplasia of the ipsilateral mandible.
Clinical Features.
Condylar hyperplasia is more common in females and is most frequently discovered before age 20 years. The condition is self-limiting and tends to arrest with termination of skeletal growth, although a few cases continue to grow, and adult onset has been reported. The condition may progress slowly or rapidly. Patients have a mandibular asymmetry that varies in severity, depending on the degree of condylar enlargement. The chin may be deviated to the unaffected side, or it may remain unchanged but with an increase in the vertical dimension of the ramus, mandibular body, or alveolar process of the affected side. As a result of this growth pattern, patients may have a posterior open bite on the affected side or a crossbite on the contralateral side with resultant problems with mastication or speech. Patients may also have symptoms related to TMJ dysfunction and may complain of limited or deviated mandibular opening, caused by restricted mobility of the enlarged condyle.
Imaging Features.
The hyperplastic condyle may have a relatively normal shape but be enlarged, or its form could be altered (e.g., conical, spherical, elongated, lobulated) or irregular. It may appear to be more radiopaque in plain images because of the additional bone volume present. However, the cortical thickness and trabecular pattern of the enlarged condyle usually are normal, which helps to distinguish this condition from a condylar neoplasm. The glenoid fossa may be enlarged to compensate for the larger condylar head, usually as a result of remodeling of the posterior slope of the articular eminence. Secondary degenerative changes may be present because of the altered forces on the joint. The condylar neck may also be longer and thickened. Forward bending of the elongated condylar head and neck, to compensate for the increased bone volume, may result in an inverted “L” shape to these structures. The condylar neck may also bend laterally when viewed in the coronal (anteroposterior) plane (Fig. 27-10). Secondary enlargement of the ramus and mandibular body also may result in a characteristic downward bowing of the inferior mandibular border on the affected side. The ramus may have increased vertical and anteroposterior dimensions.
Differential Diagnosis.
A condylar tumor, most notably an osteochondroma, is included in the differential diagnosis. An osteochondroma usually results in a condyle with a more irregular shape compared with a hyperplastic condyle because this tumor creates a more localized protruding growth. Surface irregularities and continued growth after cessation of skeletal growth should increase suspicion of this tumor. Occasionally, a condylar osteoma or large osteophyte that occurs in chronic DJD may simulate condylar hyperplasia. Associated ipsilateral hyperplasia of the mandible would not be seen in these other conditions.
Treatment.
Treatment consists of a combination of condylectomy, orthognathic surgery, and orthodontics. Condylectomy removes the source of abnormal growth, whereas orthognathic surgery and orthodontics aim to correct any resultant functional and esthetic deficits. Initiation of treatment before condylar growth is complete helps limit the severity of mandibular deformation and compensatory changes in the maxilla and dentoalveolar structures. Treatment may also be delayed until growth is completed to avoid relapse and the need for additional interventions. A technetium bone scan may be helpful in determining if condylar growth is still active or not but may be misleading if there is increased activity secondary to concurrent remodeling or degenerative changes.
Condylar Hypoplasia
Disease Mechanism.
Condylar hypoplasia is an undersized mandibular condyle, which may be the result of congenital, developmental, or acquired diseases that affect condylar growth. Severe congenital malformations may result in complete lack of formation of the condyle (aplasia). Rare congenital conditions causing hypoplasia of the condyle often also present with abnormalities of other structures of the face, such as the ear, eye, and zygomatic arch (see Chapter 32). Trauma, infection, and therapeutic radiation exposure to the condyle during growth are potential acquired causes of hypoplasia.
Clinical Features.
Condylar hypoplasia is more commonly unilateral, unless it is a feature of a syndrome (e.g., Treacher Collins syndrome, Pierre Robin sequence). The condyle is a mandibular growth center; therefore, condylar hypoplasia is usually associated with some degree of unilateral mandibular hypoplasia and facial asymmetry. Deviation of the mandibular midline to the affected side and accentuation of this deviation on mandibular opening and malocclusion may develop. The amount of growth disturbance of the mandible is related to how early the onset of the disturbance to condylar growth occurs; earlier onset results in more severe underdevelopment of the ramus and mandibular body. Patients with condylar hypoplasia may develop symptoms of TMJ dysfunction.
Imaging Features.
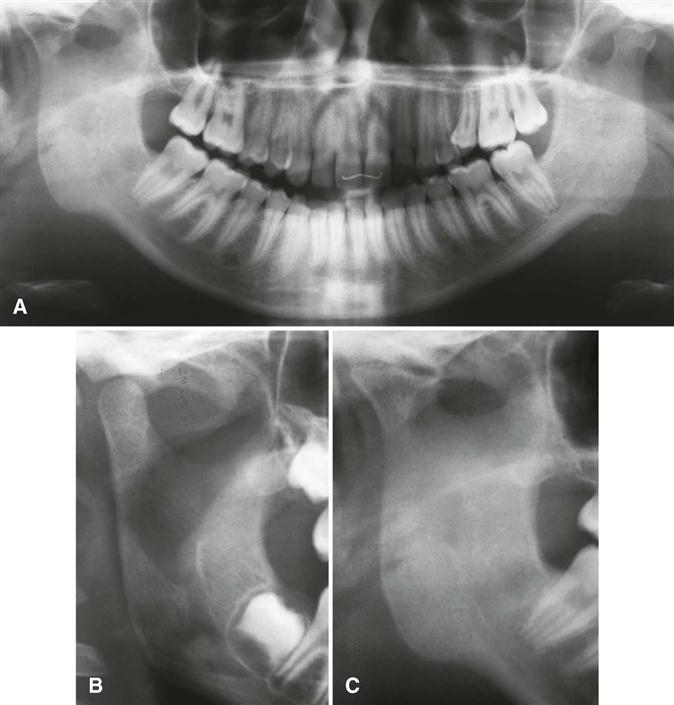
The condyle may be normal in shape and structure but is diminished in size, and the mandibular fossa is proportionally small. The condylar neck is thinner and may appear short or elongated. The coronoid process is usually slender. The posterior border of the ramus and condylar neck may have a dorsal (posterior) inclination, creating a concavity in the outline of the posterior surface of the mandible in the panoramic image. If there is an associated mandibular hypoplasia, it manifests with a deepened antegonial notch and decreased vertical height of the mandibular body (Fig. 27-11). Occasional dental crowding may also result. Degenerative changes in the affected joint may be detected (Fig. 27-12).
Differential Diagnosis.
JIA may cause damage to the condyle, resulting in hypoplasia. However, other signs of joint destruction would also be seen. A survey of other joints or testing for rheumatoid factor may be helpful if there is uncertainty. Changes in condylar morphology in severe DJD or other arthritic conditions may also mimic a hypoplastic condyle, but other signs of arthritis are usually visible in the affected joint. Additionally, arthritis does not cause mandibular hypoplasia of the affected side unless it occurs during growth. Occasionally, it is difficult to determine if there is condylar hypoplasia or if the contralateral side is enlarged. Careful examination of the inferior border for a pronounced antegonial notch (hypoplasia) versus downward bowing (hyperplasia) is helpful.
Treatment.
Orthognathic surgery, bone grafts, and orthodontic therapy may be required.
Juvenile Arthrosis
Synonyms.
Synonyms for juvenile arthrosis include condylysis, Boering’s arthrosis, and arthrosis deformans.
Disease Mechanism.
Juvenile arthrosis is a condylar growth disturbance first described by Boering, usually occurring in females during the second decade. During the first decade of growth, the mandibular condyle appears normal, but there is significant resorption of the condylar head during the second decade. The etiology is unknown, although theories involving a growth disturbance owing to an exuberant form of DJD, avascular necrosis, or hormonal abnormalities have been put forth. In cases where MRI was performed, all cases had severe anterior displacement of the articular disc. This finding supports the DJD theory. There is usually a secondary hypoplasia of the same side of the mandible. Juvenile arthrosis may be unilateral or bilateral.
Clinical Features.
Juvenile arthrosis affects mainly females during the second decade of growth. It usually is an incidental finding in a panoramic projection, or the patient may have mandibular asymmetry, signs and symptoms of TMJ dysfunction, or both. As the condylar changes progress, the patient often develops an anterior open bite.
Imaging Features.
The classic description is that the condylar head develops a characteristic “toadstool” appearance, with marked flattening and apparent elongation of the articulating condylar surface and dorsal (posterior) inclination of the condyle and neck. The condylar neck is shortened or absent in some cases, with the condyle resting on the upper margin of the ramus (Fig. 27-13). However, this description of the condylar changes was based on panoramic or transpharyngeal images with considerable image distortion of the condyle. CBCT images often reveal marked resorption of the superior aspect of the condylar head without a dorsal inclination. The articulating surface of the temporal component often is flattened. Progressive shortening of the ramus occurs on the affected side, and the antegonial notch may be deepened, indicating mandibular hypoplasia. Signs of DJD are always present.
Differential Diagnosis.
Resorption of the condylar head from JIA and severe DJD or severe condylar degeneration after orthognathic surgery or joint surgery may simulate juvenile arthrosis.
Treatment.
Orthognathic surgery and orthodontic therapy may be required to correct the mandibular asymmetry. Caution should be exercised in undertaking orthodontic therapy because stress on the joint may result in further degeneration and orthodontic relapse.
Coronoid Hyperplasia
Disease Mechanism.
Coronoid hyperplasia results in elongation of the coronoid process of the mandible. The etiology may be acquired or developmental. The coronoid processes may impinge on the posterior surface of the zygomatic arch during opening, restricting condylar translation. Sometimes a pseudojoint develops between the hyperplastic coronoid and the posterior surface of the zygoma, a condition called Jacob’s disease.
Clinical Features.
The developmental variant of coronoid hyperplasia is more commonly bilateral. This form is most often diagnosed in young men who have a long history of progressive limitation of mouth opening. The resulting restricted opening may simulate the features of an apparent closed lock owing to disc displacement. Acquired coronoid hyperplasia usually develops secondary to restricted movement of the condyle, such as in ankylosis. The condition is painless.
Imaging Features.
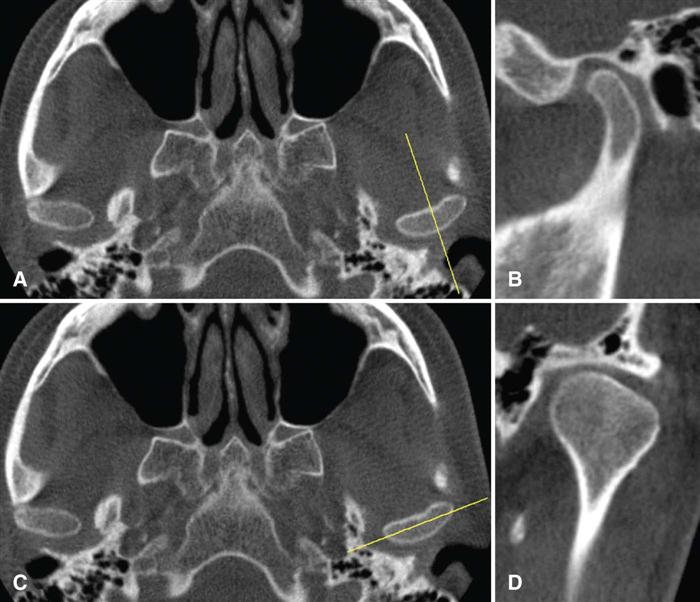
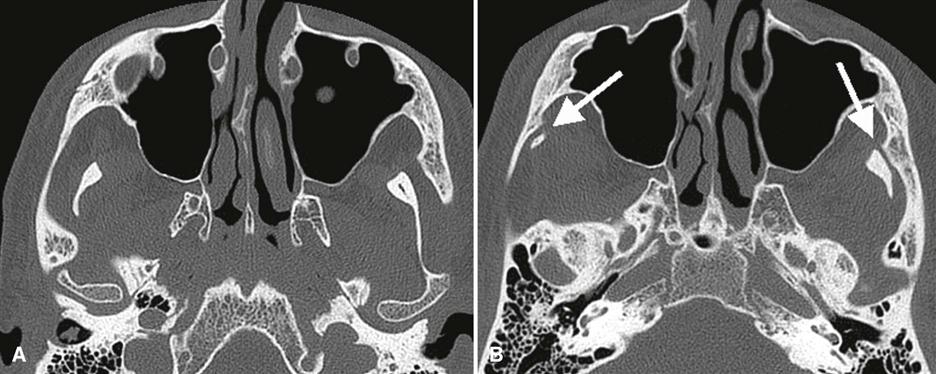
Coronoid hyperplasia is best seen in panoramic images, Waters’ images, and CBCT scans. The coronoid processes are elongated, and the tips extend at least 1 cm above the inferior rim of the zygomatic arch (Fig. 27-14). The coronoid processes may have a large but normal shape or may curve anteriorly and may appear very radiopaque. Impingement of the coronoid against the zygomatic arch can be confirmed by performing CT imaging with the patient’s mouth opened maximally (Fig. 27-15). Remodeling of the posterior surface of the zygomatic process of the maxilla, to accommodate the enlarged coronoid process during function, may also be seen. Because this condition is often bilateral, both sides should be examined for abnormality. The radiographic appearance of the TMJs usually is normal.
Differential Diagnosis.
Unilateral elongation of the coronoid process should be differentiated from a neoplasm, such as an osteochondroma or osteoma. In contrast to coronoid hyperplasia, tumors usually have an irregular shape. Clinical presentation of limited opening most often prompts examination of the TMJs for abnormalities that may restrict joint movement, such as internal derangement, neoplasm, or ankylosis. However, inclusion of the coronoid processes during TMJ imaging helps ensure that coronoid hyperplasia is not missed.
Treatment.
Treatment consists of surgical removal of the coronoid process and postoperative physiotherapy. Regrowth of the coronoid process after surgery has been reported.
Bifid Condyle
Disease Mechanism.
A bifid condyle has a vertical depression, notch, or deep cleft in the center of the condylar head, seen in the frontal or sagittal plane, resulting in the appearance of a “double” condylar head. There may be actual duplication of the condyle. This condition is rare and is more often unilateral, although it may be bilateral. It may result from an obstructed blood supply during development or other embryopathy, although a traumatic cause has been postulated with the divided condyle resulting from a longitudinal fracture.
Clinical Features.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses