Chapter 21
Planning for the Future
Teresa A. Dolan1 and Douglas Berkey2
1 DENTSPLY International, York, PA, USA; University of Florida College of Dentistry, Gainesville, FL, USA
2 University of Colorado School of Dental Medicine, Aurora, CO, USA
Introduction
The aging of America is often referred to as the demographic imperative, or perhaps more dramatically, as a tsunami or the “Age Wave”(Dychtwald & Flower, 1989). These terms refer to the dramatic shift in the age composition of the USA. Never before in human history have so many people lived beyond the age of 65 years. For example, as seen in Fig. 21.1, in 1900 only 4.1% of the US population was over the age of 65 years as compared to 13% in 2010 and a projected 20.2% in 2050. The USA is projected to experience rapid growth in its older population as baby boomers or those born between the years 1946 and 1964 begin crossing into the category of older adults, which can be chronologically defined as those over the age of 65. By the year 2030, the US Census Bureau estimates that there will be 57.8 million baby boomers aged between 66 and 84 (US Census Bureau, 2006). This shift has profound social, political, healthcare, business, financial, workforce, and cultural implications.
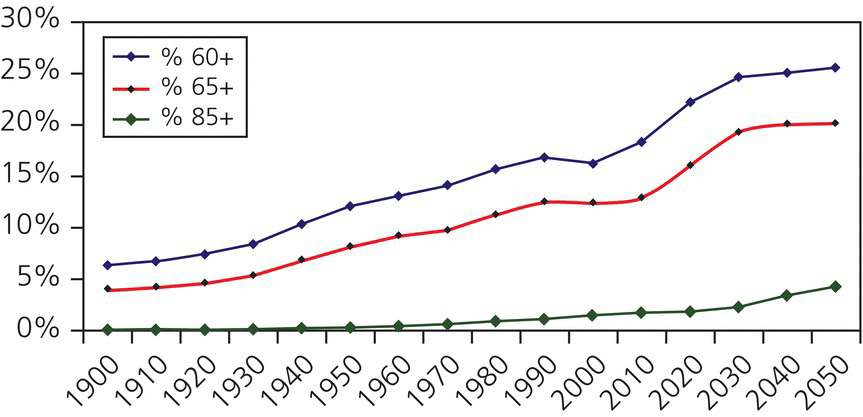
Figure 21.1 Older population by age from 1900 and projected through 2050. Projections for 2010 through 2050 are from US Census Bureau (2008), Table 12. The source of the data for 1900–2000 is US Census Bureau (2002), Table 5. This table was compiled by the US Administration on Aging using the Census data noted.
Policy implications of the aging US population include the impact on federal spending, as well as on our healthcare, long-term care and social service systems. The USA is challenged to ensure appropriate access to necessary healthcare services, and doing so within constrained resources to achieve the best possible health outcomes. From an oral health perspective, we are challenged to ensure that the dental workforce is well prepared to serve the needs of older adults and that dental care is organized and delivered in a way that meets the needs of older patients.
The purpose of this chapter is to explore the impact of the aging population on US health policies, the preparation of health professionals, and delivery of oral health services. In thinking towards the future, how can we anticipate the healthcare needs of all older adults, and particularly vulnerable elders? Can we ensure that our public policies, care delivery, reimbursement systems, and health professionals are aligned and prepared to meet the dental needs of the growing number of elders? Case studies will be used to illustrate some key concepts in geriatric dentistry including innovative models of care delivery, and the development of public policies that are sensitive to the needs of older adults.
The continuum of aging
Because of the great variability in physical, social, medical, oral and mental health status among people over the age of 65 years (Dychtwald & Flower, 1989; Dolan et al., 2005), it is overly simplistic to use a chronological definition of aging. It is more appropriate to discuss the needs of older adults according to their health and functional status, rather than by their age alone (Dychtwald & Flower, 1989). A broader definition offered by the Bureau of Health Professions described “elderly” to mean “a population with healthcare conditions and needs which differ significantly from those of younger people, which are often complicated by the physical, behavioral, and social changes associated with aging. This would include all persons over sixty, but may include slightly younger people who are subject to similar physical and/or mental conditions” (Bureau of Health Professions, 1993).
Ettinger and Beck classified elders as being independent, frail, or functionally dependent (Ettinger & Beck, 1984). While the majority of older adults live independently in the community, a smaller proportion of elders are frail and need some assistance, while others with significant functional dependence require assistance in their “activities of daily living” or ADLs. ADLs refer to the basic tasks of everyday life, such as eating, bathing, dressing, toileting, mobility, and transferring from a chair to a bed, for example. When people are unable to perform these activities, they need help from other people, from mechanical assistive devices or from both (Katz et al., 1963).
Although persons of all ages may have problems performing their ADLs, prevalence rates of people with these limitations are much higher for the elderly than for the nonelderly. The prevalence of a condition is defined as the number of persons in a certain population who have a specific disease or condition at a designated point in time. A prevalence rate is the proportion of persons with a defined disease or condition at the time they were studied (Katz, 1997). As seen in Table 21.1, the prevalence of chronic diseases as well as disabilities and limitations increases with advancing age and is especially high for persons aged 75 years and over (IOM, 2008). For example, about half of adults ages 75 years and older have trouble hearing as compared to only about 16.8% of adults ages 18 years and over. These prevalence estimates do not include adults living in long-term care and other institutional settings. Thus, the prevalence is most likely an underestimate and the number of adults affected by chronic diseases and related limitations is probably higher than reported in the table. These changes in health status with age impacts oral health as well. As people age and become more vulnerable and functionally impaired, they are less likely to have regular dental visits and are more likely to have oral health problems (Dolan et al., 1998).
Table 21.1 Prevalence of chronic diseases and disability or limitations by age group, 2006a
| Ages 18 + (%) | 64–74(%) | Ages 75 + (%) | |
| Prevalence of chronic disease | |||
| Hypertension | 22.9 | 52.9 | 53.8 |
| Chronic joint symptoms | 25.2 | 42.7 | 44.2 |
| Heart disease | 10.9 | 26.2 | 36.6 |
| Any cancer | 7.1 | 17.2 | 25.7 |
| Diabetes | 7.7 | 18.6 | 18.3 |
| Stroke | 2.6 | 7.6 | 11.2 |
| Asthma | 7.3 | 7.8 | 6.1 |
| Chronic bronchitis | 4.2 | 5.6 | 6.7 |
| Prevalence of disability/limitations | |||
| Trouble hearing | 16.8 | 31.9 | 50.4 |
| Vision limitations, even with glasses or contacts | 9.5 | 13.6 | 21.7 |
| Absence of all natural teeth | 8.0 | 22.8 | 29.4 |
| Any physical difficulty | 14.6 | 30.2 | 48.1 |
Note: Does not contain information on the institutionalized adult population.
A person’s health status can be dynamic, and older persons may be independent at one point in time and then become frail or functionally dependent after suffering an acute ailment or the exacerbation of a chronic condition. Likewise, an older person can recover from an acute illness and regain functional independence (Dolan & Atchison, 1993). Thus, organizing and providing health services for older patients can be more complex than for the healthy adult patient. The American Dental Association has been engaged in several national initiatives focused on “vulnerable elders,” defined as patients over the age of 65 who have any or all of the following: limited mobility, limited resources, or complex health status (ADA, 2009). This focus recognizes some of the unique challenges in providing care to older patients who have limitations in their functional abilities and may be homebound or living in long-term care facilities. Regardless of the location of the care being provided, the astute clinician needs to be aware of possible variations in health status, frequently review the health status of the patient, “check in” with how the patient may be feeling during a particular visit, and be willing to adjust the daily care plan accordingly.
Health professionals as well as policy makers should also reflect on their personal beliefs and opinions about the aging process and older adults, and how this could potentially impact the approach to patient care. Our attitudes, beliefs, and conceptions of the characteristics of older persons, termed ageism, may be prejudicial and distorted (Hooyman & Kiyak, 2010). (See Chapter 4 on Palmore’s Facts on Aging Quiz to learn more about facts and myths of aging.) While some may have negative views of older adults, others may hold compassionate stereotypes about older adults in which they assume that most older people are poor, frail, ill-housed, and deserving and/or in need of public or government assistance. We must guard against ageism and both positive and negative stereotypes in our care of older patients. Patient-centered care recognizes and acknowledges the uniqueness of each person as we plan for their individual care. It is important to understand that age or date of birth has limited predictive value in terms of functionality or scope of dental treatment when dealing with our aging population. Likewise, policy makers should be aware of positive and negative stereotypes about older people as they work to set state or national health agendas to care for older adults at the societal level (Hooyman & Kiyak, 2010).
Health and social policies for older adults
The Social Security Act of 1935 established the first significant national public benefits program and consequently the federal government’s role in protecting the social welfare of older adults (Bryce & Friedland, 1997). The act provided an implicit guarantee that the succeeding generations would provide for its older members through employees’ Social Security contributions. Some policymakers at the time intended to expand the plan to include other public benefits including a nationwide health program. However, after the passage of the Social Security Act, national interest in policies to further support older adults diminished until the 1960s. Subsequent landmark legislation passed in 1965 included establishing Medicare and Medicaid (Hooyman & Kiyak, 2010). These public policies were critical in keeping many older adults out of poverty, and ensuring payment for most medical and hospital services.
Congress passed the Older Americans Act (OAA) in 1965 in response to concern by policymakers about a lack of community social services for older persons. The original legislation established authority for grants to states for community planning and social services, research and development projects, and personnel training in the field of aging. The law also established the Administration on Aging to administer the newly created grant programs and to serve as the federal focal point on matters concerning older persons (AoA, 2012).
While this federal legislation provides support for most medical services for older adults, public funding for adult dental services is much more limited. Consequently, the lack of public funding for dental care often results in older adults not receiving routine preventive and restorative dental services. As a consequence, many older patients only seek dental care when they have an emergency or a dental problem. About 70% of older adult patients do not have third party payment coverage for their care (McGinn-Shapiro, 2008). Funding for Medicaid is targeted at low-income people and is shared approximately equally between the state and the federal governments. Although Medicaid requires that coverage of certain dental benefits be provided for children, states can opt out of providing dental benefits for adults and seniors, and most have done so. Only about 2% of the total Medicaid budget is currently allocated to oral health care (CDC, 2003).
Funding for Medicare is fully supported by the federal government, and the primary beneficiaries are adults over age 65, although there are limited provisions for coverage of certain serious illnesses for all age groups. As further described in the next paragraph, Medicare provides no dental coverage for elders except in extraordinary circumstances. Sometimes dental services are covered through employer-provided healthcare plans. This coverage does not usually extend into retirement years. Even if privately or publicly funded plans provide some basic coverage beyond the work years, inadequate reimbursement can emphasize triage and symptomatic care only. Fear or anxiety may also limit dental care usage in older adults. Visual or hearing-impaired elderly can become frustrated trying to communicate with dental staff. As a result, dental care may not be pursued. Because such a small proportion of US elders have private dental insurance and Medicare and Medicaid’s coverage of oral health care is minimal, the dental care needs of underserved older Americans will not be met without significant changes in health policy related to dental care for older adults.
“Medically necessary” oral health care
The US Surgeon General’s report has declared that oral health problems represent the “silent X-factor promoting the onset of life-threatening diseases which are responsible for the deaths of millions of Americans each year” (NIDCR, 2000). Increasingly, studies find that oral disease can significantly affect systemic health. For example, bacteremia or cytokinemia from diseased periodontal tissues may trigger inflammatory and/or immunologic responses contributing to tissue or organ damage (see Chapter 11, Periodontal Disease). Compelling associations exist between oral disease and cardiovascular and respiratory diseases, but oral disease can also exacerbate the effect of diseases such as diabetes. Data-driven conclusions about a potential direct cause-and-effect relationship for many oral–systemic linkages remain lacking, but ongoing research continues to suggest strong inter-relationships. Medical and oral health research collaborations to study these relationships are urgently needed to improve the delivery of oral health care and to set public policy and direct public resources to the most effective therapies, including oral health care.
In establishing the Medicare legislation, Congress included a blanket exclusion of dental services. The enabling legislation specifically omitted payments “for services in connection with the care, treatment, filling, removal, or replacement of teeth or structures directly supporting the teeth” (Section 1862(a)(12) of the Social Security Act). The exclusion was later amended in 1980 when Congress made an exception for inpatient hospital services when the dental procedure itself made hospitalization necessary (CMS, 2013). The exception allowed payment “in the case of inpatient hospital services in connection with the provision of dental services if the individual, because of his/her underlying medical condition and clinical status, or because of the severity of the dental procedure, requires hospitalization in connection with the provision of such services.” Currently, Medicare will pay for dental services that are an integral part either of a covered procedure such as reconstruction of the jaw following accidental injury, or for extractions done in preparation for radiation treatment for cancer involving the jaw (Committee on Medicare Coverage Extensions, 2000). Medicare will also make payment for oral examinations, but not treatment, preceding kidney transplantation or heart valve replacement, under certain circumstances. The Medicare coverage as specified in statue is summarized in Table 21.2.
Table 21.2 Medicare coverage of dental services as specified in statute or by the Health Care Financing Administrationa
| Clinical condition | Medicare-covered service |
| Underlying medical condition and clinical status requires hospitalization for dental care | Inpatient hospital services only (Medicare Part A) |
| Severity of dental procedure requires hospitalization for dental care | Inpatient hospital services only (Medicare Part A) |
| Any oral condition for which nondental services are covered | All dental services if incident to and an integral part of a covered procedure or service performed by the same person (Medicare Part B) |
| Neoplastic jaw disease | Extractions prior to radiation and prior to oral examination if extractions occur (Medicare Part B) |
| Renal transplant surgery | Oral or dental examination on an inpatient basis (Medicare Part A if performed by hospital-based dentist; Part B if performed by a physician) |
a Adapted from Field et al. (2000).
In 2011, Congress considered but ultimately disapproved funding medically necessary dental procedures associated with prosthetic heart valve replacement, organ transplantation, head and neck cancer, lymphoma, and leukemia. Medically necessary dental procedu/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


