Prescribing Diagnostic Imaging
Sharon L. Brooks
The decision to prescribe diagnostic images should be based on the individual needs of the patient. In this chapter, the term diagnostic images includes conventional (film-based) radiographs as well as any digital image format produced by x rays. Likewise, the commonly used term radiograph is not restricted to images produced on film, but rather it also includes common intraoral and extraoral digital images.
Patient imaging needs are determined by findings from the dental history and clinical examination and modified by patient age and general health. Diagnostic imaging is necessary when the history and clinical examination have not provided enough information for complete evaluation of a patient’s condition and formulation of an appropriate treatment plan. Patients should be exposed to x rays only when, in the dentist’s judgment, it is reasonably likely that the patient would benefit by the discovery of clinically useful information in the resultant image.
Role of Radiographs in Disease Detection and Monitoring
The goal of dental care is to preserve and improve patients’ oral health, while minimizing other health-related risks. Although the diagnostic information provided by diagnostic imaging may be of definite benefit to the patient, the radiologic examination does carry the potential for harm from exposure to ionizing radiation. One of the most effective means of reducing possible harm is to avoid making radiographs that would not contribute information pertinent to patient care. The judgment that underlies the decision to make a radiologic examination centers on several factors, including the following:
• Prevalence of the diseases that may be detected radiographically in the oral cavity
• Ability of the clinician to detect these diseases clinically and in diagnostic images
As a general principle, diagnostic imaging is indicated when a reasonable probability exists that it would provide valuable information about a disease that is not evident clinically. Conversely, radiographs are not indicated when they are unlikely to yield information contributing to patient care. Information derived from the image considered to be clinically useful includes data that are valuable in detecting disease, in monitoring the progression of known diseases, and in planning dental treatment.
For many clinical situations, it is not readily apparent to the practitioner whether diagnostic images have a reasonable probability of providing valuable information. In these situations, the practitioner must use clinical judgment after weighing the patient factors to decide whether imaging is indicated.
The philosophy of prescribing images only when there is a high probability of obtaining clinically useful information has been advocated by all the organizations responsible for developing or endorsing guidelines for ordering diagnostic imaging. However, many dentists use radiographs as a screening tool, simply to see “what’s there,” without having a specific suspicion of disease arising from the dental history or clinical examination. There are probably numerous reasons for this use of radiographs. Some dentists think that they have not provided an adequate service to their patients if they cannot assure them that they have searched diligently for disease with all reasonable diagnostic methods, including diagnostic images. They may state that having complete information, regardless of whether it affects the treatment plan, is of such benefit that it outweighs the risk of the radiation exposure. Other dentists raise medicolegal issues, stating fear of lawsuits if they fail to detect disease. Others express concern about the effect on the efficiency of the dental office of the extended examinations required for prescribing diagnostic images on the basis of signs and symptoms. The next few paragraphs address these concerns.
In contrast to dentistry, screening imaging is rarely used in medicine with the exception of mammography for women older than a certain age or with increased risk factors for breast cancer, and there is controversy over whether even this type of examination should be used as frequently as it is today. Breast cancer is a relatively common yet serious disease that should be detected early, before the cancer becomes large enough to be found clinically. However, diseases of the jaws (with the exceptions of caries and periapical and periodontal disease) are rare and concentrated in certain ages, sexes, and ethnicities. These diseases are unlikely to be discovered on routine screening radiographs before they have produced signs or symptoms that could be found with a thorough clinical examination and history. Periodontal disease can be diagnosed clinically, although diagnostic images are used to determine the extent of bone loss and the presence of other factors that may affect prognosis. Periapical disease is usually associated with extensive restorations or caries that can be detected clinically. However, dental caries on proximal surfaces may not be detectable on clinical examination until it has reached an advanced stage; thus, this is one occult disease for which screening radiographs are considered appropriate. Regarding the threat of lawsuits for failure to diagnose, dentists who follow guidelines on the use of diagnostic imaging developed or endorsed by authoritative bodies that help establish the standard of care should have no concerns. Although lawsuits can be filed for many reasons, it is unlikely that they will be successful if it can be shown that the practitioner did a thorough clinical examination and history and carefully considered the guidelines when determining whether to order diagnostic imaging.
Some dentists set up their practices so that new patients are automatically seen first by the dental hygienist, who takes a predetermined set of diagnostic images at the first appointment, before the dentist sees the patient. Although this may make efficient use of the dentist’s time, it is contrary to the recommendations of the American Dental Association (ADA) that the selection of number and type of radiographs should be based on the findings of the clinical examination. Performing a thorough examination before ordering images should not be an insurmountable obstacle for an efficient dental practice.
Regarding the issue of cost versus benefit of diagnostic images, there is little risk of harm for any individual patient from one set of images, even if no important diagnostic information is revealed. However, there is a large societal cost, both in terms of health care dollars and radiation risk, if millions of dental patients receive unproductive examinations, as would happen if routine screening were widespread. In addition, there is a growing concern among the public and the medical profession about the increasing use of ionizing radiation in health care in general and the risks it poses to the public.
Our philosophy is that the prescription of diagnostic imaging should be based on the need for diagnostic information for patients on a case-by-case basis. The next section discusses some of the clinical situations that may call for a radiologic examination.
Caries
Dental caries is the most common dental disease, affecting people of all ages. Although the caries prevalence rates of developed countries have been decreasing since the 1970s, probably partially as a result of the widespread use of fluoride, increasing numbers of older adults are maintaining their teeth throughout their lifetimes, leaving them at risk for developing both coronal and root caries. In addition, caries prevalence is not uniformly distributed throughout the population, with children of lower socioeconomic background having a higher rate of untreated caries than other children.
Although occlusal, buccal, and lingual carious lesions are reasonably easy to detect clinically, interproximal caries and caries associated with existing restorations are much more difficult to detect with a clinical examination only (see Chapter 18). Studies have repeatedly demonstrated that clinicians using intraoral images detect caries not evident clinically, both in enamel and in dentin. Although a radiologic examination is very important for diagnosis of dental caries, the optimal frequency for such an examination should be based on mitigating features, such as the patient’s age, medical condition, diet, oral hygiene practices, oral health status, and the nature of the caries process itself.
Carious lesions demonstrate one of three behaviors: (1) progression, (2) arrest, or (3) regression. Only about 50% of lesions progress beyond the initial, just-detectable defect, and in most instances the lesions demonstrate a slow rate of progression through enamel (months to years). Mechanisms are also in use to enhance remineralization of early enamel lesions. However, the rate of caries progression is significantly faster in deciduous enamel than in permanent enamel, and patients vary widely in their rates of formation of caries and in their rates of caries progression.
Because the presence of caries cannot be determined with confidence by clinical examination alone, it is necessary to expose patients periodically through bitewing radiographs to monitor dental caries. The length of the exposure intervals varies considerably because of different patient circumstances. For most patients in good physical health with adequate oral hygiene, an infrequent radiologic examination is needed to monitor dental caries. However, if the patient history and clinical examination suggest that the individual has a relatively high caries experience, shorter intervals allow careful monitoring of disease.
Periodontal Diseases
Some form of periodontal disease affects most people at some point during their lives, gingivitis more often in younger individuals and periodontitis more commonly in older adults. Periodontal diseases are responsible for a substantial portion of all teeth lost. A consensus exists among practitioners that radiologic examinations play an important role in the evaluation of patients with periodontal disease after the disease is initially detected on clinical examination (see Chapter 19). In addition to providing a picture of the extent of alveolar bone support for the dentition, radiologic examinations help demonstrate local factors that complicate the disease, including the presence of gingival irritants such as calculus and faulty restorations. Occasionally, the length and morphologic features of roots, visible on periapical radiographs, are crucial factors in the prognosis of the disease. These observations suggest that when clinical evidence exists of periodontal disease other than nonspecific gingivitis, it is appropriate to make intraoral images, generally a combination of periapical and bitewing images, to help establish the severity of the disease. Follow-up images after therapy is complete help the clinician monitor the progression of disease and determine whether the destruction of alveolar bone has been halted.
Periapical Inflammatory Disease
When a patient presents with a toothache, deep caries, or a large or deep restoration, the likelihood of an inflammatory lesion of pulpal origin occurring at the apex of the tooth increases. Usually the clinical examination combined with a periapical radiograph is sufficient to make the diagnosis and plan the treatment, endodontic therapy, or extraction. However, in cases with complex root canal anatomy, evidence of failed endodontic treatment, intraoperative or postoperative complications, or situations where the periapical view does not provide adequate information, a limited-volume, high-resolution cone-beam computed tomographic (CBCT) examination might be useful.
Dental Anomalies
Abnormal formation of teeth may be manifested as deviations in number, size, and composition. These abnormalities in dental development occur more frequently and are more likely to have a serious impact in the permanent dentition than in the primary dentition. The most frequently encountered anomalies are the presence of supernumerary teeth, usually mesiodens, or developmentally absent teeth, usually second premolars (see Chapter 31).
Only a few anomalies exist for which orthodontic treatment or surgical correction or modification must start at an early age. When the dentist suspects an abnormality requiring treatment, diagnostic images to confirm and localize it are not required until the time when the treatment is most appropriate. For example, a panoramic examination of a 5-year-old child to determine the presence or absence of permanent teeth may be poorly timed. Although the examination provides evidence that one or more second premolars or lateral incisors are developmentally missing, this information usually does not influence the current treatment plan. When examination for dental anomalies is appropriate, both the radiation dose and the anticipated diagnostic benefit should be considered. Projections that best demonstrate the required diagnostic information should be selected. A panoramic image of the lower face is usually best for observing the presence or absence of teeth in all quadrants, although a periapical or occlusal radiograph is sufficient for an examination limited to one area.
Growth and Development and Dental Malocclusion
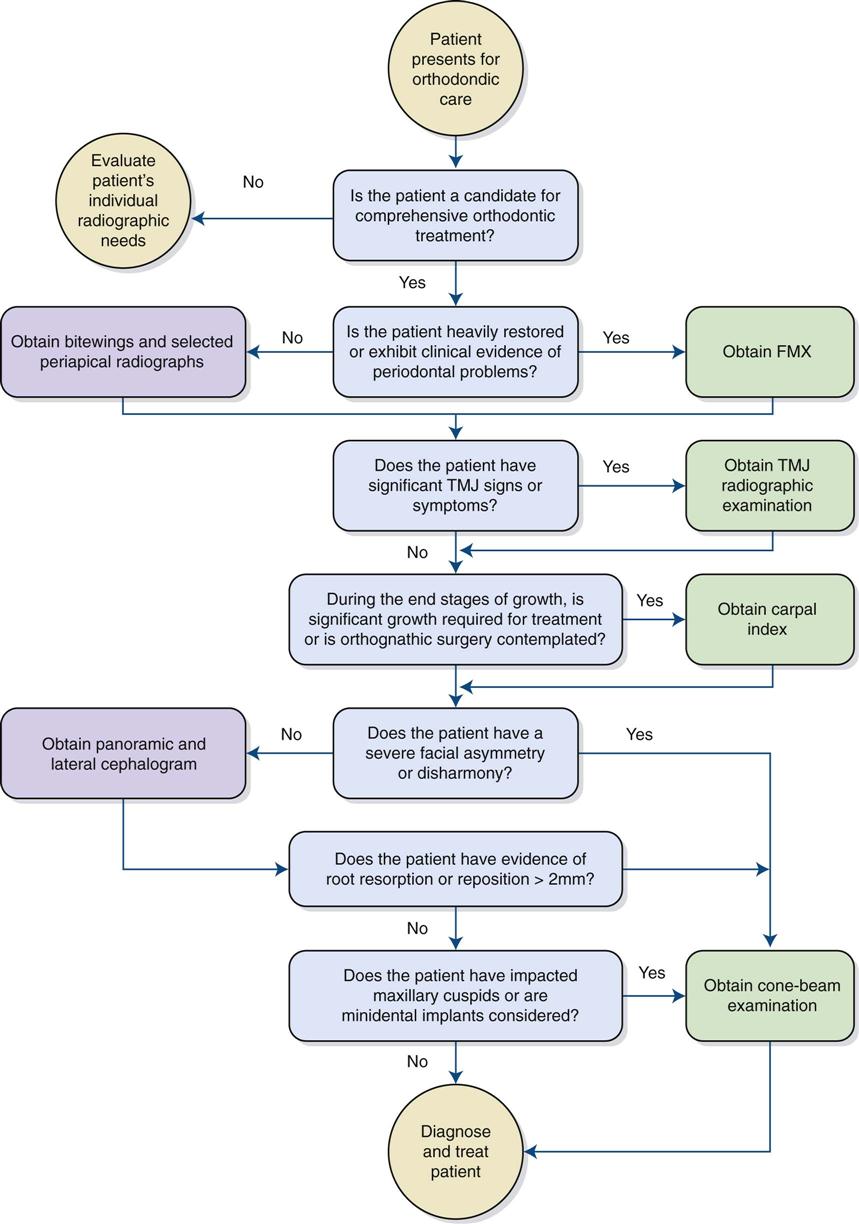
Children and adolescents are often examined to assess the growth and development of the teeth and jaws. This assessment considers the relationship of one jaw to the other and to the soft tissues. An examination of occlusion, growth, and development requires an individualized radiologic examination that may include periapical radiographs or a panoramic view to supplement other images ordered to assess dental disease. In addition, a patient of any age group who is being considered for orthodontic treatment may need other images, such as lateral or posteroanterior cephalometric, occlusal, carpal index (wrist), or temporomandibular joint (TMJ) images, depending on the clinical findings (Fig. 16-1).
CBCT imaging is being used increasingly frequently for orthodontic evaluation to provide three-dimensional information about jaw relationships and to substitute for multiple other imaging examinations (see Chapters 11 and 12). At the present time, it is unclear which patients would benefit from CBCT imaging in terms of treatment considerations. There is adequate information in the literature to demonstrate the value of CBCT imaging in the evaluation and treatment of impacted teeth but less information on other conditions of interest in orthodontics. The American Association of Orthodontists and the American Academy of Oral and Maxillofacial Radiology more recently developed a joint position statement on the use of CBCT imaging in orthodontics. Broadly, the statement recommends using CBCT imaging only when justified by individual need and the clinical question cannot be answered by using lower dose conventional imaging. Dose-reduction protocols should be used when possible. CBCT imaging is also used in some cases of impacted mandibular third molars when the relationship of the inferior alveolar nerve to the root apex is unclear with conventional images.
The dentist who is the primary provider of orthodontic treatment should select the number and type of images needed. The needs of each patient should be considered individually. Selecting the appropriate images should allow a maximal diagnostic yield with a minimal radiation exposure after consideration of the clinical examination, the study of plaster models and photographs, and the optimal time to initiate treatment.
Occult Disease
Occult disease refers to disease that presents no clinical signs or symptoms. Occult diseases in the jaws include a combination of dental and intraosseous findings. Dental findings may include incipient carious lesions, resorbed or dilacerated roots, and hypercementosis. Intraosseous findings include osteosclerosis, unerupted teeth, periapical disease, and a wide variety of cysts and benign and malignant tumors (see Chapters 20 to 26). Small carious lesions, resorption of root structure, and bony lesions may go unnoticed until signs and symptoms develop.
Although the consequences of some occult diseases may be quite serious, most serious diseases are rare. Often a historical or clinical sign or symptom of intraosseous disease suggests its presence. For instance, an unusual contour of bone or an absent third molar, not explained by a history of extraction, suggests the possibility of an impaction with the potential for an associated dentigerous cyst. Although patient history and clinical signs and symptoms do not always accurately predict dental and intraosseous findings, most of these true occult diseases are not clinically relevant, or they are so rare that except for caries as described previously the dentist need not obtain a radiologic examination of the jaws solely to screen for them in dentate individuals in the absence of unusual clinical signs or symptoms. Caries is an exception because of its much higher prevalence than other occult diseases.
There is a considerable difference of opinion regarding whether asymptomatic edentulous patients seen for routine denture construction should have screening images taken to look for occult disease. Several studies have demonstrated a relatively large number of findings in diagnostic images of edentulous patients, including retained root tips and areas of sclerotic bone, but almost all these findings required no treatment and did not affect the outcome of care. For that reason, some experts recommend no images of edentulous patients if the clinical examination is negative for signs and symptoms of disease. Others think that screening radiographs of these patients are of value. As the standard of care for completely or partially edentulous patients moves toward dental implants rather than removable prosthetics, imaging to assess the quantity and quality of bone available for implants is gaining in importance.
There has been increasing interest in the last few years in using panoramic images to screen patients for the presence of calcified atheromas in the bifurcation of the carotid artery, a finding that may indicate an increased risk for the development of a cerebrovascular accident (stroke). However, the value of this finding has been questioned more recently because a noncalcified vulnerable plaque, which is not visible on panoramic radiographs, may put the patient at more risk for stroke than a more stable calcified plaque. Nevertheless, the general consensus at this time is that panoramic images made for dental purposes should be evaluated for this calcification, particularly in patients older than 55 years, but that these images should not be made simply to screen for atheromas without other dental indications. (See Chapter 28 for more details.)
Jaw Disease
Imaging of known jaw lesions, such as fibro-osseous diseases or neoplastic diseases, before biopsy and definitive treatment, is also important for appropriate management of the patient. For small lesions of the jaws, periapical or panoramic radiographs may be enough as long as the lesion can be seen in its entirety. If clinical evidence of swelling exists, some type of radiograph at 90 degrees to the original plane (often an occlusal image) should be made to determine whether there is expansion of the jaw or perforation of the buccal or lingual cortical bone. If lesions are too large to fit on standard dental radiographs, extend into the maxillary sinus or other portions of the head outside the jaws, or are suspected to be malignant, additional imaging such as medical computed tomographic (CT) imaging or CBCT imaging is appropriate before biopsy (see Chapters 11 to 14). Both of these types of images can provide excellent bone detail, but if there is a suspicion that the lesion may involve the surrounding soft tissue, medical CT imaging should be used instead of CBCT imaging because it can provide images of the soft tissue. These types of imaging can define the extent of the lesion, indicate an appropriate biopsy site, suggest an operative approach, and provide information about the nature of the lesion. If the lesion is not based in bone but in the adjacent soft tissue, magnetic resonance (MR) imaging, which has superior contrast resolution of soft tissue, should be used. In the initial steps of the investigation, referral to an oral and maxillofacial radiologist to order and report on the most appropriate diagnostic imaging before the biopsy procedure is reasonable.
Temporomandibular Joint
Many types of diseases affect the TMJ, including congenital and developmental malformations of the mandible and cranial bones; acquired disorders such as disk displacement, neoplasms, fractures, and dislocations; inflammatory diseases that produce capsulitis or synovitis; and arthritides of various types, including rheumatoid arthritis and osteoarthritis. The goal of TMJ imaging, similar to that for imaging other body parts, should be to obtain new information that would influence patient care. Radiologic examination may not be needed for all patients with signs and symptoms referable to the TMJ region, particularly if no treatment is contemplated (see Chapter 27). The decision regarding whether and how to image the joints should depend on the results of the history and clinical findings, the clinical diagnosis, degree of diagnostic certainty required, and results of prior examinations as well as the tentative treatment plan and expected outcome.
The cost of the examination and the radiation dose should also influence />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses