Periodontal Emergencies
Dorothy A. Perry and Phyllis L. Beemsterboer
• Define the role of the dental hygienist in the recognition and treatment of periodontal emergencies.
• Describe the etiology of periodontal abscesses.
• Compare and contrast the signs, symptoms, and treatment considerations in patients with gingival, periodontal, and periapical abscesses.
• Describe the distinguishing features of necrotizing ulcerative gingivitis.
• List the identifying features of pericoronitis.
• Outline the treatment for necrotizing ulcerative gingivitis and oral herpetic lesions.
• Describe the symptoms and oral lesions of acute herpetic gingivostomatitis.
Periodontal Abscesses
A periodontal abscess is an inflammation of microbial origin that is associated with accumulations of suppuration or purulence (pus) in the periodontal tissues. The pus is often referred to as exudate or purulent exudate. Such infections have rapid onset and are usually characterized by pain, swelling, and discomfort. The periodontal abscess is caused by microbiota that have become established in the tissue as a result of trauma, advancing disease process, or incomplete scaling and root planing. The response of the tissue to this inflammatory process depends on the patient’s resistance. Individual factors, such as systemic disease, can affect the clinical situation and worsen the acute condition. There are three basic types of abscesses: periodontal, gingival, and periapical. Each type may be acute or chronic—although the chronic periodontal abscess is likely an acute abscess that drains—and there are combination abscesses.1
Acute Periodontal Abscesses
Acute periodontal abscesses are associated with preexisting periodontal disease. They may occur around any tooth in the mouth when the periodontal pocket becomes occluded, often as a result of a foreign object. An exacerbated inflammatory reaction then occurs. If the pocket can drain through a sulcus or a fistula (opening in the tissue), the infection can stabilize and be considered in a chronic state.1 Stabilization will not occur if a foreign object, such as a peanut skin, popcorn hull, or berry seed, remains in the pocket.
Acute periodontal abscesses appear as shiny, red, raised, and rounded masses on the gingiva or mucosa.2 They can point and drain through the tissue or drain through the pocket opening. Pus is usually seen around the opening of the abscess, but not always. In these cases, visual examination is not sufficient to recognize the abscess and finger pressure is required to express pus into the oral cavity so it can be seen. Examples of acute abscesses are shown in Figure 16-1.
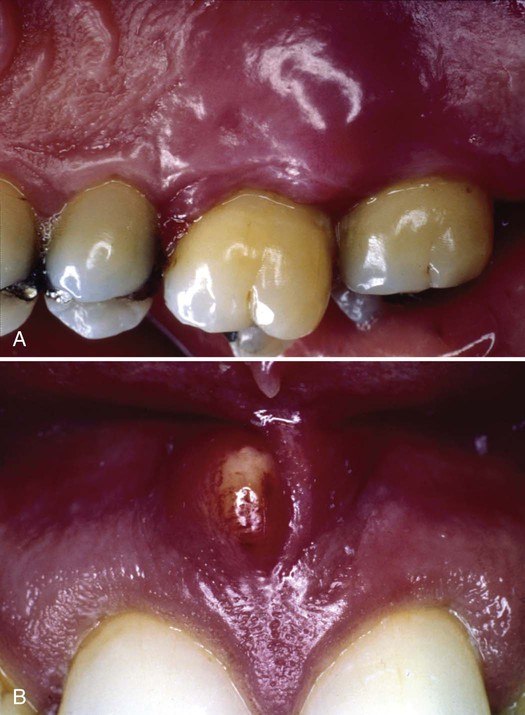
A, Clinical appearance of an acute periodontal abscess. There is marked swelling of the periodontal tissues. Clinically, the tissue appears shiny, reddened, and raised. The patient had severe pain. B, Acute periodontal abscess associated with a central incisor with a large fistulous track. The fistula drained periodically, thus relieving the swelling and pain for a short time. The fistula then closed temporarily and the swelling and pain recurred. (A courtesy of Dr. Philip R. Melnick.)
The most common symptom of acute periodontal abscess is pain. Other symptoms include the following:
The patient may also report that the tooth feels “high” in the occlusion because it may become slightly extruded as a result of swelling of the periodontal ligament.1 Radiographs may be helpful in locating a preexisting area of bone loss, which may be the origin of the abscess. However, the infection moves through the tissue in the direction of least resistance so that the external features may appear at some distance from the affected tooth. The opening of a fistula or sinus along the lateral aspect of the tooth in the adult dentition is usually indicative of a periodontal abscess. However, it may be the result of a periapical abscess. In the primary dentition, a sinus opening on the lateral aspect of the tooth is usually associated with a periapical rather than a periodontal abscess.2
The microbiota in the acute periodontal abscess are predominantly gram-negative and anaerobic. In contrast, healthy gingival biota are predominantly gram-positive and aerobic.3
Treatment Considerations
Treatment of acute periodontal abscesses consists mainly of drainage and the use of antibiotics or antimicrobial agents. The abscess must be treated immediately to alleviate pain and prevent spread of infection. It may be drained through the pocket opening or by access through an incision. Drainage through the pocket opening is usually possible. The teeth in the affected area are scaled and root-planed when the patient is anesthetized and curettage may be performed to remove granulation tissue. Postoperative instructions call for rest, fluid intake, and warm salt water rinses (1 tsp of salt in a glass of warm water) to help reduce swelling. Follow-up treatment, often involving periodontal surgery, is required to eliminate the problem.4
The initial treatment of the abscess through the pocket is often the responsibility of the dental hygienist. However, sometimes flap surgery is required at the initial appointment to obtain access for complete debridement. This treatment is performed by the dentist or periodontist. Antibiotics and pain medications are not usually required.4 If the patient has a fever or if lymphadenopathy is present, antibiotics should be prescribed. The antibiotic recommended can be an analogue of tetracycline because these drugs have the ability to create high titers in the gingival sulcus and inhibit collagenase in the host.5
Chronic Periodontal Abscess
Chronic periodontal abscesses resemble acute periodontal abscesses; in fact, they may be indistinguishable.1 These abscesses are characterized by an overgrowth of pathogenic organisms that result in suppuration. Chronic abscesses are usually painless because they drain into the oral cavity, either through the opening of the pocket or through a sinus tract. On careful questioning, patients often recount previous experiences of pain and swelling, probably caused by acute episodes of infection.2
The chronic periodontal abscess exhibits suppuration that exudes into the oral cavity on digital pressure through the pocket or sinus tract. The associated gingival tissue is red and swollen. As long as the chronic abscess is draining, it is unlikely to be painful, so patients tolerate the condition or do not realize it is occurring. The dental hygienist must understand that suppuration that exudes from the periodontium indicates a chronic abscess and requires appropriate treatment. An example of a chronic abscess with a sinus tract through the tissue is presented in Figure 16-2.
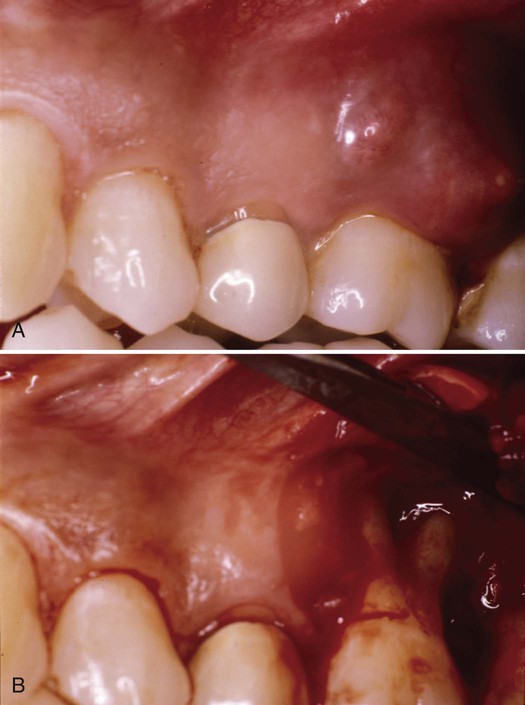
A, Inflammatory exudate drained continuously through the opening of the pocket. B, On surgical opening of the defect, an extensive furcation involvement was seen. (Courtesy of Dr. Philip R. Melnick.)
Treatment Considerations
The treatment of chronic periodontal abscesses is similar to the treatment of acute periodontal abscesses. The affected tooth crown and root surfaces must be scaled and root-planed, curettage performed, local antimicrobial therapy completed if needed, and the patient seen for follow-up care to evaluate the need for further periodontal treatment, often including periodontal surgery.4 The patient must be made aware of the chronic condition, informed about possible acute episodes if no further treatment is performed, and encouraged to cooperate with meticulous maintenance therapy.
Tooth Loss Associated with Periodontal Abscesses
Periodontal abscesses do not necessarily result in tooth extraction. A classic retrospective study of 114 patients treated and maintained at a university periodontology clinic, all having had moderate to severe periodontal disease, suggested that teeth that develop periodontal abscesses can be treated successfully and maintained for years. Over the 13-year study, 109 periodontal abscesses occurred. Symptoms of the infected teeth were pain, swelling, exudate, and fistulous tracts. In total, 45% of teeth were extracted, but 55% of the teeth were treated and maintained for an average of 12.5 years; the range was 5 to 29 years.6 For this reason, it is important for the dental hygienist to recognize periodontal abscesses and refer them for immediate treatment.
Gingival Abscess
Gingival abscesses are primarily distinguished from acute periodontal abscesses by taking a good medical and dental history. Gingival abscesses often occur in disease-free areas, and they may be related to forceful inclusion of some foreign object into the area. Usually, gingival abscesses are found on the marginal gingiva and are not associated with any abnormality of the deeper tissues.1 A gingival abscess is shown in Figure 16-3.
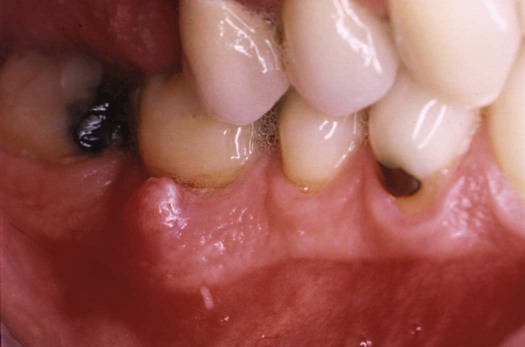
This gingival abscess appeared as a localized area of swelling away from the sulcus. It was painful for the patient. (Courtesy of Dr. Philip R. Melnick.)
The gingival abscess typically appears as a shiny raised area of acute inflammation that may be painful. The swelling, although it may be quite large, is usually confined to the marginal gingiva.2 A suppurative lesion is usually evident on the gingival tissues.1
Treatment Considerations
The gingival abscess must be drained and irrigated. The treatment is usually performed by the dentist or periodontist. It is incised, drained, and irrigated with warm water. Warm salt water rinses should be recommended for postoperative therapy. After treatment of the abscess, scaling and root planing of the teeth should be performed, usually the next day. If the reduced lesion is still large, it may require excision.4
Endodontic Abscess
An endodontic abscess is sometimes difficult to distinguish from an acute periodontal abscess. The facial pain and tenderness to the tooth are similar in both cases. Endodontic abscesses result from infection through caries, traumatic fracture of the tooth, or trauma from a dental procedure.1 In addition, pulpal infection of a tooth can spread to the pulp from an adjacent infected tooth through the lateral canals.7 Most commonly, microorganisms are spread from a carious lesion into the pulp through the dentinal tubules. The microorganisms colonize in the pulp and produce a variety of toxins that result in pulp cell death. Bacteria and their metabolic products then exit the apical foramen and can cause abscess formation.8
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


