Treatment Planning for the Periodontal Patient
• Describe the goals and rationale for periodontal treatment planning.
• Define the role of the dental hygienist in determining the dental hygiene care plan.
• Classify the phases of dental treatment included in the comprehensive care plan.
• List the major classifications of periodontal disease.
• Identify the considerations for sequencing dental hygiene treatment with periodontal diseases.
• Identify the patient factors to be considered when establishing the treatment plan sequence.
• Discuss informed consent and its importance to the process of patient care.
Defining a treatment plan for the periodontal patient is a process that requires the assessment, preventive, therapeutic, and evaluative skills of the dental hygienist and the dentist. The treatment plan is the blueprint for management of the dental case and is an essential aspect of successful therapy.1 This plan includes all procedures performed to attain and maintain the long-term oral health of the patient and should involve all members of the health care team and the patient. This chapter describes current strategies and classifications for planning the treatment of the periodontal patient. No treatment should be provided to a patient until a treatment plan has been established and agreed on. The only exception to this would be emergency care to relieve a patient of pain due to injury or acute disease.
Goals of Treatment
The total treatment plan is the sequential outline of the essential services and procedures to be provided to eliminate disease and restore the oral cavity to health and function. The dental hygiene treatment plan consists of services that are performed by the dental hygienist within the total treatment plan.2 Treatment planning occurs after the assessment of all clinical data and reflects the diagnosis and prognosis of the patient. The treatment plan defines the methods and sequence of delivering appropriate treatment.1,3,4
The goals of the treatment plan are to eliminate and control etiologic and predisposing factors of disease, maintain health, and prevent recurrence of disease.1,4 These goals are the same, regardless of the sequence of treatment or the individual who is delivering the dental care. Treatment planning provides an opportunity to explain problems and treatment goals to the patient in understandable terms.4–6 Listening to the patient’s concerns is a crucial element in the treatment planning process so that the plan can address the patient’s perceived needs along with the disease identified by the clinician. The dental hygienist must also use the visual and verbal feedback from the patient to judge the patient’s level of understanding. A true partnership between the patient and the dental team working toward mutual treatment goals has the greatest opportunity for success.
Phases of Treatment
Carranza and collaborators divided the treatment plan into four main phases. Each phase suggested a particular group of procedures and included evaluation of the patient’s response. The treatment sequence begins with a preliminary phase (incorporating immediate treatment needs), followed by Phase I (etiologic treatment), Phase II (surgical treatment), Phase III (restorative treatment), and Phase IV (maintenance treatment). The phases of therapeutic periodontal procedures, along with the sequence of other needed dental procedures, are presented in Box 10-1.
Phase I therapy describes the procedures that are designed to control or eliminate the etiologic factors of the disease process. Patient education and plaque control instruction occur at the beginning of this phase. Scaling, root debridement and planing are performed. Antimicrobial agents are used or recommended for home use. This stage has also been referred to as initial therapy, nonsurgical therapy, cause-related therapy, or the hygienic phase of treatment.7,8
Phase IV therapy is the maintenance phase. Patients remain in this phase for a lifetime. Although this phase is often referred to as “recall,” the accepted terms are periodontal maintenance or periodontal recall because the patient’s periodontal health must be continuously monitored from this point. The maintenance phase begins after Phase I, but not necessarily before all phases of treatment have been completed. Patients with extensive surgical and restorative needs often have treatment extend over many months, even years. Periodontal maintenance occurs while the other phases of treatment are ongoing because the completion of the entire treatment plan can take months or years, and decline in the status of periodontal patients has been observed much earlier, after as little as 90 days. In their classic studies, Ramfjord and Ash demonstrated that 3-month maintenance intervals were responsible for the long-term success of periodontal treatment.7
The interval between periodontal maintenance appointments is determined by the periodontal condition and the plaque control that the patient is able to attain and maintain. Most patients who have been treated for moderate to advanced periodontal disease require maintenance visits every 3 months.9–12
Role of the Dental Hygienist
The dental hygienist is often responsible for treatment of the periodontal patient in the nonsurgical, or Phase I, and maintenance, or Phase IV, stages of periodontal treatment. Because of the complexity of the periodontal treatment required to meet planned goals, a series of appointments is often required. The sequence of treatment depends on a number of factors, including the periodontal diagnosis and prognosis, the patient’s systemic and periodontal condition, and the patient’s preferences. Figures 10-1 to 10-4 are examples of successful therapeutic results achieved by a dental hygienist providing Phase I therapy.
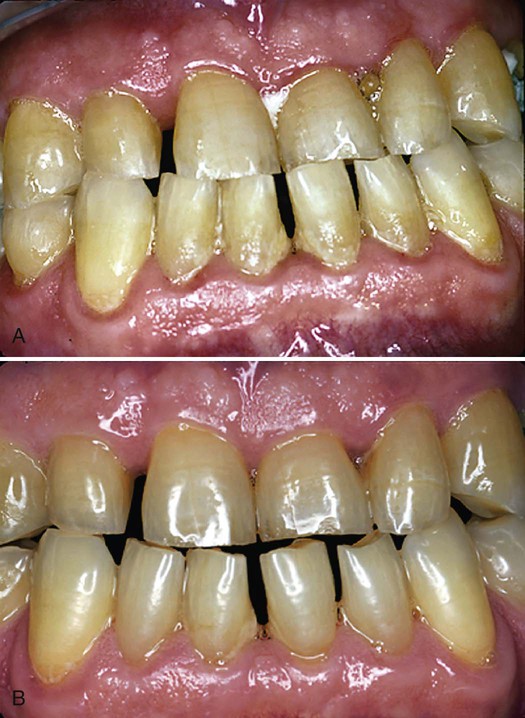
A, The dental hygienist provided four quadrants of scaling and root planing with the use of local anesthetics, plus home care instruction and reinforcement, for this 60-year-old man. The patient had 4- to 6-mm probe depths, slight CAL, and heavy deposits of plaque biofilm and subgingival calculus. B, One month after the last treatment appointment, the pocket depths have resolved by 2 mm and the patient’s home care has improved dramatically. Note the tissue changes from red and edematous to a uniform coral pink.
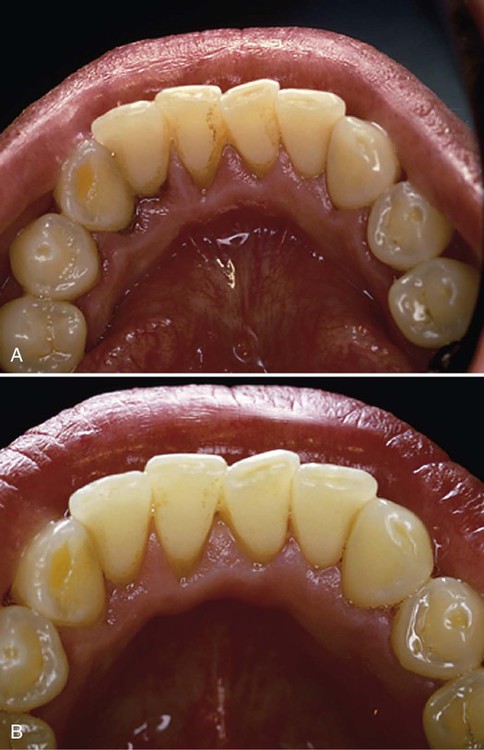
A, This 27-year-old woman had relatively shallow pocket depths, 2 to 4 mm throughout, but moderate subgingival calculus accumulated on the lingual and interproximal surfaces of the mandibular teeth. The patient sought treatment because she was concerned about breath odor and stains on the teeth. The dental hygiene care plan included oral hygiene instruction, scaling and root planing half of the mouth at each visit, polishing to remove extrinsic stains, and a follow-up assessment. B, One month after the second treatment visit, the tissue had improved significantly. Probing depths were 2 to 3 mm, the tissue was firm and pink, and the patient’s home care habits had improved greatly. The patient was very pleased because the stains were gone from her teeth and she thought that her breath odor was gone. The patient was initially placed on a 4-month recall to help reinforce her good oral hygiene habits and is now maintained (Phase IV) with therapy at 6-month intervals.
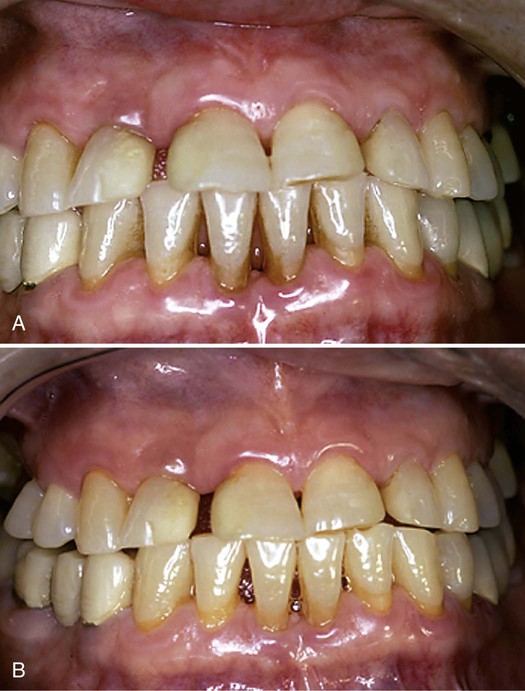
A, This 36-year-old woman was concerned about bleeding gingivae. She had heavy subgingival calculus and 5 to 6 mm of CAL in most areas of her mouth. Probing depths were 4 to 6 mm throughout the mouth, with class II furcations involvement in the molar teeth. B, The patient was treated with quadrant scaling and root planing requiring local anesthesia, oral hygiene instruction, and reinforcement. She required periodontal surgery to reduce the remaining pockets and permit cleaning of the furcation areas. Note the improved tissue color and tone in the anterior areas. The patient was maintained on a 3-month recall regimen that began after Phase I therapy was completed. She had the periodontal surgery performed while on the maintenance regimen, and the dental hygienist was able to maintain the successfully treated areas of the mouth and modify recommended oral hygiene procedures to assist her in cleaning the furcation areas.
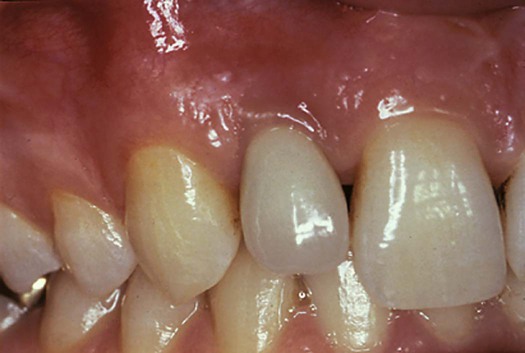
This 41-year-old male patient had completed Phase I therapy consisting of quadrant scaling and root planing and oral hygiene instructions. The maxillary right area did not respond well around tooth #7. The dental hygienist noted the redness and swelling that remained in the tissue and reinstrumented the area. Substantial amounts of calculus remained on the tooth. After this second treatment, the pocket depth resolved to 2 to 3 mm, and tissue color and texture then appeared similar to the other areas of the mouth—pink and firm. Note the residual calculus on the mesial surface of tooth #9, at the right edge of the figure. Calculus at this location adheres to the root surface right at the cementoenamel junction and is very difficult to remove.
Disease classifications are useful for diagnosis, prognosis, and treatment planning because they help define the extent of disease and facilitate communication among members of the treatment team. Various periodontal classification systems have been used over the years and have been modified to reflect advances in knowledge and research.1 A classification system is simply a method for comparing treatment approaches and likely results. Using a system that is understood and used by a large number of dental professionals greatly facilitates communication regarding cases.
In 1999, an international group of periodontal experts approved the classification system currently in use. This system is based on the clinical manifestations of disease and conditions. The overall approach of this classification system separates gingival disease from periodontal disease and conditions affecting the periodontium. This system was adopted by the American Academy of Periodontology (AAP) and is widely accepted by the dental community as the preferred classification system.13 The classifications are outlined in Box 10-2.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


