Chapter 15
Prosthetic Considerations for Frail and Functionally Dependent Older Adults
Ronald L. Ettinger
Department of Prosthodontics, Dows Institute for Dental Research, University of Iowa College of Dentistry, Iowa City, IA, USA
Introduction
Earlier chapters have dealt with the demographic imperative and the decline in edentulousness, which has changed the treatment needs of the older population from noninvasive replacement of dentures to the complex needs of the dentate.
There is no such person as a typical older adult because they are extremely heterogeneous, ranging from the healthy to the frail, from the highly educated to the illiterate, from the affluent to the poor (Ettinger, 1993). This heterogeneity results from the fact that each person is influenced by their heredity, their diet, exercise, various diseases accidents, and lifestyle (Chalmers & Ettinger, 2008). The variance among older adults also influences their health literacy, with varying levels of knowledge and motivation regarding health and oral health (Shelley et al., 2008).
In the past, the primary focus of prosthodontics for older adults was how to deliver complete dentures to the population (Eklund, 1999). The retention of teeth and the influence of aging, wear and tear, as well as iatrogenic issues, means that the dental needs of older adults have now become much more complex when compared to younger persons. The need for tooth/teeth replacement, which is the area of dentistry known as prosthodontics, has increased significantly in this population and the younger cohorts of older adults will no longer accept the simple solutions of the past, that is, the extraction of remaining teeth and the construction of complete dentures (Berkey et al., 1996).
The aging population
The elderly have been defined as a cohort of persons aged 65 years and older. The utilization of only a chronological criterion is not particularly useful in dentistry because, as previously discussed, there is a great variation in the population. These older adults have experienced differences in physical health, medical issues and mental conditions as well as different life experiences. Thus, from an oral health perspective, a functional definition is much more useful. Ettinger and Beck (1984) separated the older population into three broad functional categories to reflect their ability to seek dental services:
- Functionally independent older adults: These adults live in the community unassisted and comprise about 70% of the population over age 65 years. Many of these persons may have some chronic medical problems such as, hypertension, type 2 diabetes (DM2), or osteoarthritis for which they are taking a variety of medications. Assuming the dental practitioner understands his or her patients’ medical issues and the effects of their medications, treatment will depend on their perception of need and the amount they are prepared to pay for it. These older adults can access dental care independently using their own vehicles or public transportation, if it exists. Their prosthodontic treatment has been well-described by Budtz-Jorgensen (1999) in his textbook “Prosthodontics for the Elderly.”
- Frail older adults: These are those persons who have lost some of their independence, but still live in the community with the help of family and friends or who are using professional support services such as Meals on Wheels, visiting nurses, home health aides, etc. They make up about 20% of the population over age 65 years. These older adults can no longer access dental services without the help of others. Their oral health needs require a greater understanding of medicine and pharmacology and a careful evaluation of their ability to maintain daily oral hygiene. The prosthodontic decision making for this segment of the population is the primary focus of this chapter.
- Functionally dependent older adults: These are those persons who are no longer able to live in the community independently and are either homebound (about 5% of population over 65) or living in institutions (another 5% of population over 65). These older adults can only access dental services if they are transported to a dentist’s office and many may use wheelchairs so the offices should be wheelchair accessible. If they cannot be transported, then the services need to be brought to them through mobile programs. This means that dental offices need to be wheelchair-accessible, the dental professional needs mobile equipment to visit the patient, or the institution in which the older adult resides must have a dental facility. This chapter does not deal in detail with the prosthodontic care of this group of older adults. (See Chapters 17 and 18 for alternative dental care delivery models.)
Decision making in prosthodontics
The knowledge base required to manage the oral problems of frail older adults does not depend on the development of new technical skills but rather on the following:
- An understanding of normal aging;
- An understanding of pathologic aging;
- An understanding of older adults’ medical problems and recognizing the oral implications of their systemic diseases;
- A knowledge of pharmacology and drug-induced dental diseases;
- The interpersonal skills needed to communicate with the patient, his or her family, and his or her other healthcare providers;
- Knowing special communication techniques with older persons who have sensory deficits;
- Having practical experience in clinical decision-making for frail and functionally dependent older adults.
The bulk of dental care for frail older adults still remains reconstructive, that is, the restoration of teeth and the restoration of function of the stomatognathic system with fixed and removable partial dentures (Douglass & Watson, 2002). The clinical techniques are usually similar to those needed for treating younger persons; however, more problems are encountered. For example, in recurrent caries the margins of interproximal restorations will need to be placed subgingivally with all the associated problems due to bleeding, marginal adaptation of restorative materials, and finishing (Bader et al., 1991).
Deciding what constitutes appropriate care may vary for an older cohort of individuals because those decisions must include the consideration of a variety of age-related and age-associated psychologic, sociologic, biologic, and pathologic changes. Therefore, it is essential to identify modifying factors before a comprehensive treatment plan is formulated, as illustrated by the the following case study of a functionally independent older adult (Case study 1).
Treatment plan no. 2
Maxilla
New complete denture.
Mandible
Surgical removal of the tori FPD nos. 20–22, crown no. 27–29, RCT nos. 23–26 with post and core and crowns, distal extension RPD.
Comment
This treatment plan stabilizes the mandibular arch, is less stressful, but is time-consuming and expensive.
Treatment plan no. 3
Maxilla
New complete denture.
Mandible
Surgical removal of the tori extract nos. 20, 23, 24, 25, 26, 28, 29; cut down nos. 22 and 27 as vital overdenture, abutments for a complete overdenture. Wait 6 weeks before constructing dentures.
Comment
This treatment plan is the least expensive and least stressful and provides the patient with a functional dentition
After presentation of these treatment plans, a modified final treatment plan was developed with the patient and his wife that was within their budget and was aesthetic and functional (Fig. 15.4a–d).
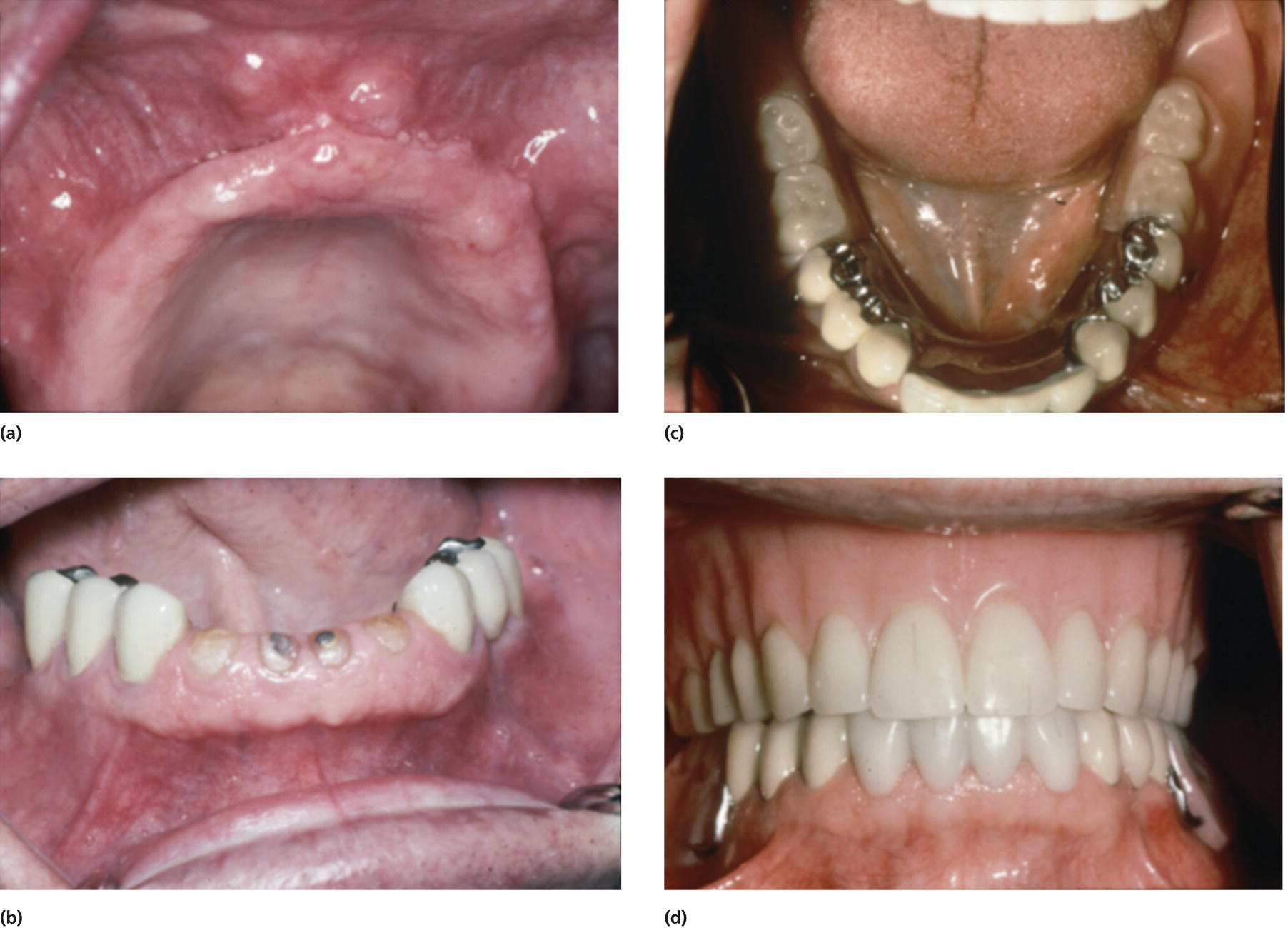
Figure 15.4 (a–d) The restored dentition
(see Case study 1 for more details).
Maxilla
New complete denture.
Mandible
Surgical removal of the tori. FPD nos. 20–22, crowns nos. 27–29, RCT no. 25, Teeth nos. 23–26 cut down as vital overdenture abutments for a cast partial distal extension overdenture. He was prescribed PreviDent® 5000 gel to be used in his RPD on a daily basis after breakfast and after cleaning.
Evaluation of treatment
This dental treatment did solve the patient’s chewing and eating problems and improved the quality of his life. His wife approved of the change in his appearance due to the increase in the vertical dimension of occlusion. The problem of the wear of his denture was resolved by a combination of fixed prosthodontics and a removal partial denture. The continuing wear of his teeth was halted by the use of acrylic resin teeth on his complete maxillary denture and his removable partial overdenture. The patient was asked to return in 3 months for evaluation.
Key: FPD = fixed partial denture; RPD = removable partial denture; RCT = root canal treatment.
Sociodemographic information
To understand the prosthodontic needs of a patient, one must understand the environment in which the patient functions and how oral health care fits into their life style. It is not sufficient to gather a lot of data on age, gender, occupation, and education without understanding how these factors influence the needs and expectations of a patient. Life experiences such as the Depression of the 1930s, the World War of the 1940s, the Korean War of the 1950s, and the Vietnam War of the 1960s influence attitudes, values, and beliefs. The value of a dentition depends on the attitude of the patient, his or her family, or caregivers, which impacts treatment. The question is, does this person utilize health care or dental care only in response to some symptoms such as pain and discomfort? If so, how can the dentist influence and educate the patient to change these behaviors? Is this a patient who is educated about health issues and who would appreciate the presentation of several treatment plans of varying costs, which would allow the patient to choose one which best fits their expectations and lifestyle? If not, how can we help to educate the patient to increase oral health literacy?
Health history
As a population ages, there is a higher risk for chronic diseases and the patient is more likely to take medications, some of which have the potential to affect the oral tissues (Jainkittivong et al., 2004). The most common side effect of many of the drugs used by this population is hyposalivation, which may induce xerostomia and increase the risk of caries and periodontal disease (Guggenheimer, 2002; Shinozaki et al., 2012; Thomson, 2005). If a person has severe xerostomia induced by disease (Sjögren’s syndrome), therapy (radiation or chemotherapy), or by drugs (e.g., amitriptyline), which may increase the risk of ulcerations when wearing dentures and a loss of retention of the maxillary denture (Thomson, 2005). The risk of mucosal infection by Candida albicans, especially underneath a maxillary denture, is increased. Saliva substitutes such as Oral Balance® or MI Paste® can help with the lubrication and retention of a complete denture (Gil-Montoya et al., 2008).
When caring for frail or functionally dependent older adults, an evaluation of their health history will help determine whether these problems will affect them. (See Chapter 14 for a more detailed discussion of xerostomia.)
Tips and techniques for treating frail or functionally dependent elders
Time of the appointment
Due to the circadian changes in platelet aggregation related to hemostasis, patients with cardiovascular disease should not be seen between 6 AM and 9 AM because of an increased risk of a cardiovascular event (Chursciel et al., 2009). Patients with arthritis are preferably not seen before late morning or early afternoon due to stiffness of their joints in the morning (Walker, 2011). Patients with dementia should be seen in mid-morning when they are fresh as tiredness can bring on unacceptable behaviors (Mancini et al., 2010).
Length of the appointment
Many frail or functionally dependent older adults cannot sit for extended periods of time. Patients who are underweight may need pillows and support in the dental chair to cushion their spines. It is suggested that a dental visit should not be longer than 90 minutes from the time the patient leaves their residence to the time they return. They may require additional and shorter appointments for their prosthodontic procedures.
Patient positioning
Patients who have hiatus hernia, severe cardiopulmonary disease, or a variety of pulmonary diseases may not be comfortable when laid flat in a dental chair for the length of time of an appointment. Apart from asking directly, it may be useful to ask the patient how many pillows they sleep with or if their bed is propped up for sleeping.
Need for antibiotic prophylaxis
The 2007 American Heart Association guidelines revised the recommendations for antibiotic prophylaxis to reduce the risk of infective endocarditis (Wilson et al., 2007). Persons with prosthetic valves, a previous history of infective endocarditis, a cardiac transplant, or who are significantly immunocompromized are best treated with prophylactic antibiotics for any invasive dental procedures such as extractions, deep scaling, crown lengthening, etc. The guidelines suggest that all others who are at risk should rinse with chlorhexidine gluconate 0.12% prior to any invasive procedures. Persons who have had a major joint replaced should have antibiotic coverage for the first 2 years after their replacement. If they have not had any complications, or dislocations, then further coverage is not recommended (ADA & AAOS, 2003). The antibiotic prophylaxis guidelines were revised because of a lack of evidence-based data that antibiotics were beneficial compared to the existing data of the danger of an allergic reaction to antibiotics or the potential for development of resistant organisms.
Use of local anesthetic with vasoconstrictor (epinephrine)
It has been suggested that the amount of epinephrine used in local anesthesia be limited to 0.036 mg of epinephrine. in patients with cardiovascular disease (Neves et al., 2007). This translates to the approximate equivalent of two cartridges of 2% lidocaine (1.7 ccs) with 1 : 100 000 epinephrine (Brown & Rhodus, 2005).
Level of cognitive impairment
Since communication is an extremely important interaction between the patient and the dentist, the level of cognitive impairment influences treatment. Here are some areas to consider before beginning treatment. The clinician needs to determine if the patient can explain his or her chief complaint. Can the patient give an accurate medical history or do we need to procure it from their physician or significant other? Can the patient give us informed consent to proceed with treatment or will we need to obtain it from their legally appointed guardian for health affairs (healthcare proxy)? How will we be paid? Has the patient a legally appointed guardian for their financial affairs? Where is the patient living and is there anybody who can or will supervise their daily oral hygiene? Finally, will the patient be cooperative with you as the clinician? Since prosthodontics usually requires multiple appointments, how do you assess the risk/benefit ratio of treatment, modified treatment, or no treatment? Will the patient benefit from the stress associated with these appointments? Will there be a need for physical or chemical restraint and who will give informed consent for that treatment?
These assessments are needed to determine whether the replacement of lost teeth is necessary and if it would be beneficial to the patient. The assessment will facilitate decision making with regard to replacement either with implants, a fixed partial denture (FPD), a removable prosthesis (RPD), or no replacement at all.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


