Chapter 14
Gingival recession
Introduction
Gingival recession is defined as the apical migration of the gingival margin below the cementoenamel junction, resulting in exposure of the root surface. It can be localized or generalized and is a common problem that can be caused by periodontal disease, periodontal treatment, or chronic trauma in otherwise periodontally healthy patients. Recession can sometimes be self-limiting and cause few problems, but it can also result in a range of problems for patients and represents a difficult challenge to manage.
The principles of management of gingival recession include the following:
• Assessment of the aetiology of the condition
• Identification of the patient’s concerns about the condition
• Removal of any aetiological factors when possible
• Monitoring the stability of the recession
• Management of any sequelae of the condition, such as dentine sensitivity
• In some cases, correction of the gingival recession is indicated
Assessment
In assessing gingival recession, a careful history of the condition needs to be taken followed by clinical examination to assess the extent and severity of the condition and to identify the aetiology. A list of the aetiological factors of recession is shown in < ?xml:namespace prefix = "mbp" />
Table 14.1 Aetiological factors in gingival recession
| Aetiological factor | Specific examples | Comments |
|---|---|---|
| Chronic trauma | Particularly vigorous toothbrushing; also habitual trauma such as picking at gums and from tongue studs; direct trauma to gingivae from opposing teeth due to malocclusion | Usually gingivae healthy and uninflamed; seen particularly where there are associated anatomical factors such as thin gingival biotype |
| Gingival biotype | Thickness of the gingivae varies considerably between patients and at different sites in the mouth; bony dehiscences | Typically affecting labial surfaces of lower incisors and upper canines |
| Malocclusion | Proclination or rotation of teeth, resulting in root surfaces outside the bony envelope of the jaws, creating bony dehiscences | Similar effect to thin gingival biotype |
| Frenal attachments/lack of attached gingivae | Typically labially on lower anterior teeth | Frenal pulls may directly enhance recession but also may impair plaque control |
| Periodontal disease | Although attachment loss in periodontitis usually causes pocketing, where predisposing anatomical factors present it may result in recession instead | Gingivae inflamed and plaque accumulation evident |
| Smoking | Smoking reported to increase gingival recession | |
| Periodontal treatment | All types of periodontal treatment can result in some recession; most marked in pocket elimination surgery (apically positioned flaps) in which recession is a deliberate outcome | Widespread and generalized with loss or recession of interdental papillae; determined by the amount of underlying bone loss |
| Overeruption of teeth | Due to tooth wear or lack of opposing teeth |
Anatomical factors of the soft tissues may also play a major role in the aetiology of recession. These are particularly related to the presence of frenal attachments, especially in the lower labial mucosa. A high frenal attachment may extend close to the gingival margin of the tooth, and there may also be an associated lack of attached gingiva, such that the forces during, for example, mastication are directly transmitted to the gingival margin and promote recession. In addition, high frenal attachments may also impair adequate plaque control in the region, resulting in localized periodontal disease that manifests as recession.
Gingival recession defects can be classified according to Miller’s classification, which grades the severity of defects according to whether the recession extends to the mucogingival junction and whether it has resulted in interproximal attachment loss and recession of the interdental papilla (
Table 14.2 Miller’s classification of gingival recession defects
By itself, gingival recession may often be localized, self-limiting, and harmless. However, in many cases, there are important sequelae associated with the condition, and it is important to assess these when deciding on the management of recession. A list of problems associated with gingival recession is shown in
Table 14.3 Problems associated with gingival recession
Case 1
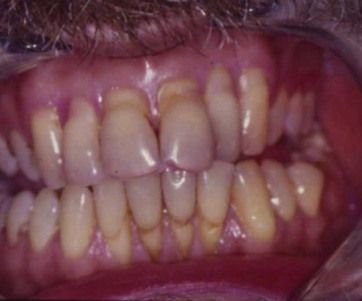
A 46-year-old man presented complaining of generalized gingival recession. He had been aware of the recession for a number of years but believed that it had become noticeably worse in the past 12 months. He had persisting tooth sensitivity to cold stimuli but was not concerned about the appearance of the recession because he believed that his lips concealed the recession. He was also concerned about the risk of tooth loss in the long term. He was medically fit and well and a nonsmoker.
He was brushing his teeth four times a day with a hard toothbrush. He had a low-sugar diet and drank approximately 1 L of orange juice every day. He had previously used a toothpaste for sensitive teeth but was not currently using this.
The clinical appearance at presentation is shown in
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses