12 RESTORATION OF THE ENDODONTICALLY TREATED TOOTH
TREATMENT PLANNING
Because of extensive caries or periodontal disease, removal of a tooth may be more sensible than endodontically treating it, although a severely damaged tooth occasionally can be restored after orthodontic repositioning or root resection (Fig. 12-1; see also Fig. 16-7). This should be done if loss of the tooth will significantly jeopardize the patient’s occlusal function or the total treatment plan, particularly if dental implants are not an option. When the decision is made to treat the tooth endodontically, consideration must have been given to its subsequent restoration. Before being restored, teeth that have been endodontically treated must be carefully evaluated for the following1:
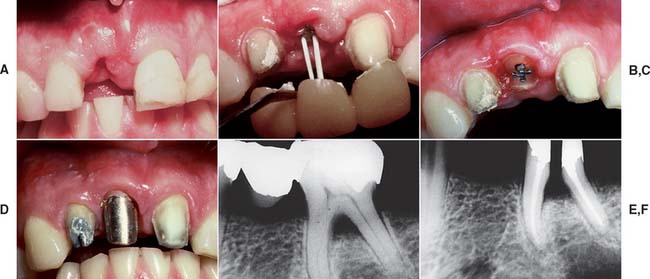
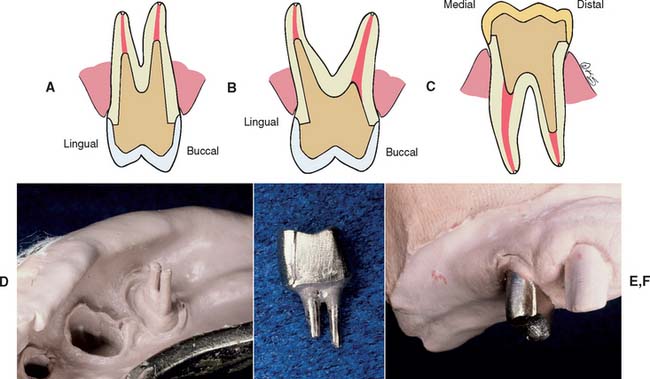
Fig. 12-1 A to D, A severely damaged tooth can sometimes be retained after orthodontic extrusion (see Chapter 6). E and F, Plaque control around periodontally compromised teeth may be improved after hemisectioning (see Chapter 5).
(E and F, Courtesy of Dr. H. Kahn.)
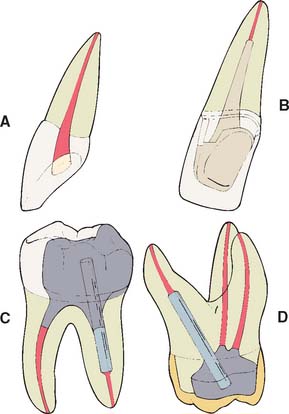
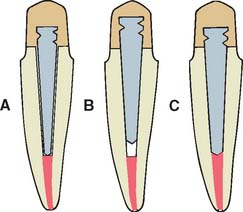
If the coronal structures are largely intact and loading is favorable, as on anterior teeth that are farther removed from the fulcrum (see Chapter 4), a simple filling can be placed in the access cavity (Fig. 12-2A). However, if a substantial amount of coronal structure is missing, a cast post and core is indicated instead (Fig. 12-2B). Molars are often restored with amalgam or a combination of one or more cemented posts and amalgam or composite resin (Fig. 12-2C and D).
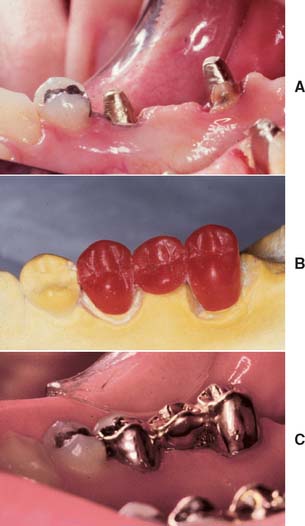
Although one-piece post-crowns were once made, such prostheses are of only historical interest. Superior results are obtained with a two-step technique (Fig. 12-3) consisting of initial placement of a post and core foundation followed by placement of a separately fabricated crown. Most often a metal post is used, which provides the necessary retention for the core. The core replaces any lost coronal tooth structure, allowing optimal tooth preparation geometry to be achieved. Thus, the shape of the residual coronal tooth structure, combined with the core, should result in an ideal shape for the preparation (Fig. 12-4).
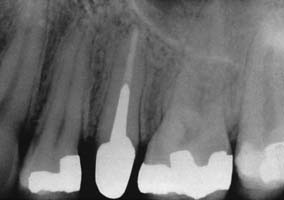
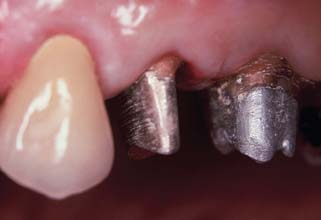
Fig. 12-4 The second premolar has been restored with a cast post and core, before a metal-ceramic crown.
(Courtesy of Dr. R. Webber.)
Prefabricated metal, carbon fiber, ceramic, and glass fiber posts are available. The last two options provide esthetic alternatives to metal posts.2,3 Typically, prefabricated posts are used in a two-step procedure: first the post is cemented, after which a plastic core material such as composite resin, amalgam, or glass ionomer is applied. After shaping of the core and remaining tooth structure to optimal crown preparation form, a crown is fabricated in the conventional manner.
A cast post and core needs to be slightly undersized compared with the canal to achieve optimal internal seating, whereas the crown needs to be slightly larger to achieve optimal seating (see Chapter 7). Thus, it is easier to achieve a satisfactory marginal adaptation because the expansion rate of the two castings can be controlled individually. An added benefit is that it is possible to fabricate a replacement crown, if necessary, without the need for post removal, which may jeopardize the prognosis of the tooth. Finally, a path of placement different from the one selected for the post and core may be selected for the crown. This is often helpful when the tooth is restored to serve as an abutment for an FDP.
Clinical Failure
In one retrospective analysis4 involving 638 patients, investigators evaluated 788 post and cores: 456 custom cast post and cores and 332 foundations with ParaPosts. Four to five years after cementation, reported failure rates in male patients were significantly higher than in female patients, and failure rates after age 60 were three times as high as failure rates for younger patients. Maxillary failure rates (15%) were three times as high as mandibular failure rates (5%) and more prevalent in lateral incisors, canines, and premolars than in central incisors and molars. Failure rate under FDPs was significantly lower than under single crowns. The latter finding may have been caused by load reduction resulting from bracing by the FDP. No correlation was apparent between failure and reduced marginal height of the encasing bone. Custom cast post and cores exhibited slightly higher failure rates than did amalgam foundations. This observation was also made by Sorensen and Martinoff.5 However, Torbjörner and colleagues4 suggested that custom cast post and cores tend to be used more often in teeth that already have considerably weakened root structure. Thus, regardless of the technique selected for subsequent restoration, the teeth themselves are already more prone to failure. Distal cantilevers appear to contribute to post and core failure in endodontically treated abutment teeth that support the cantilever.
Most of the failures just discussed are influenced by load. In general, as loading increases, failure rates appear to increase concomitantly. Failure has been shown to occur at lower loads as teeth are loaded less parallel to their long axes,6 which suggests that clinical failure occurs more readily under lateral loading.
In the planning of the restoration of endodontically treated teeth, the practitioner must account for the strength of the remaining tooth structure, weighed carefully against the load to which the restored tooth will be subjected.
Considerations for Anterior Teeth
Although it is commonly believed, it has not been demonstrated experimentally that endodontically treated teeth are weaker or more brittle than vital teeth. Their moisture content, however, may be reduced.7 Laboratory testing8 has actually revealed a resistance to fracture similar between untreated and endodontically treated anterior teeth. Nevertheless, clinical fracture does occur, and attempts have been made to strengthen the tooth by removing part of the root canal filling and replacing it with a metal post. In reality, placement of a post requires the removal of additional tooth structure (Box 12-1), which is likely to weaken the tooth.
Box 12-1 Disadvantages to the Routine Use of a Cemented Post
Placing the post requires an additional operative procedure.
Preparing a tooth to accommodate the post entails removal of additional tooth structure.
The post can complicate or prevent future endodontic re-treatment that may be necessary.
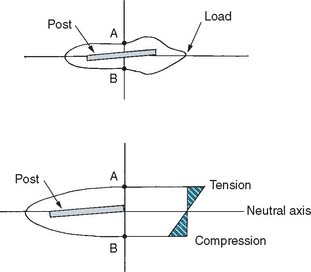
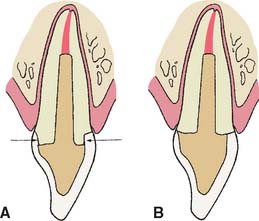
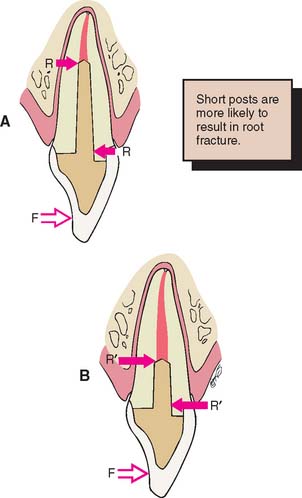
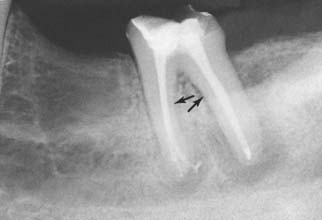
Cementing a post in an endodontically treated tooth is a fairly common clinical procedure, despite the paucity of data to support its success. In fact, a laboratory study9 and two stress analyses10,11 have determined that no significant reinforcement results. This might be explained by the hypothesis that when the tooth is loaded, stresses are greatest at the facial and lingual surfaces of the root and an internal post, being only minimally stressed, does not help prevent fracture (Fig. 12-5). Results of other studies, however, contradict this assumption.8,12 Cemented posts may further limit or complicate endodontic re-treatment options if these are necessary. In addition, if coronal destruction occurs, post removal may be necessary to provide adequate support for a future core.
For these reasons, a metal post is not recommended in anterior teeth that do not require complete coverage restorations. This view is supported by a retrospective study13 that did not show any improvement in prognosis for endodontically treated anterior teeth restored with a post. In another study, post placement did not influence the position or angle of radicular fracture.14 A conflicting report however, suggests that endodontically treated teeth not crowned after obturation were lost six times more frequently than teeth that were crowned after obturation.15
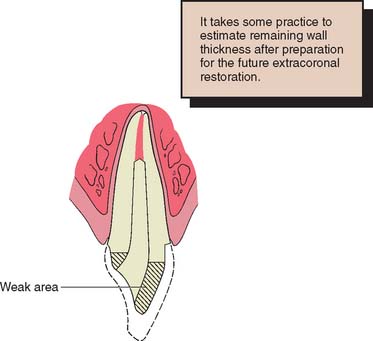
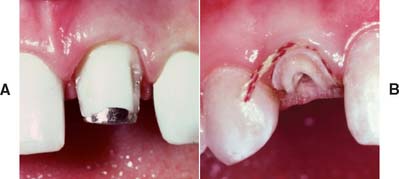
Discoloration in the absence of significant tooth loss may be more effectively treated by bleaching16 than by the placement of a complete crown, although not all stained teeth can be bleached successfully. Resorption can be an unfortunate side effect of nonvital bleaching.17 However, when loss of coronal tooth structure is extensive or the tooth will be serving as an FDP or partial removable dental prosthetic abutment, a complete crown becomes mandatory. Retention and support then must be derived from within the canal, because a limited amount of coronal dentin remains once the reduction for complete coverage has been completed. Coupled with the loss of internal tooth structure necessary for endodontic treatment, the remaining walls become thin and fragile (Fig. 12-6), which often necessitates their reduction in height.
Considerations for Posterior Teeth
Complete coverage is recommended on teeth with a high risk of fracture. This is especially true for maxillary premolars, which have been shown to have fairly high failure rates if restored with two or three surface amalgam restorations.18 Complete coverage gives the best protection against fracture, because the tooth is completely encircled by therestoration. However, when a metal-ceramic crown is to be used, considerable tooth reduction is required, which results in further weakening of the remaining tooth structure. In general, when significant coronal tooth loss has occurred, a cast post and core (Fig. 12-7) or an amalgam foundation restoration is needed.
PRINCIPLES OF TOOTH PREPARATION
Many of the principles of tooth preparation discussed in Chapter 7 apply equally to the preparation of endodontically treated teeth, although certain additional concepts must be understood in order to avoid failure.
Conservation of Tooth Structure
Preparation of the canal
In creating post space, great care must be used to remove only minimal tooth structure from the canal (Fig. 12-8). Excessive enlargement can perforate or weaken the root, which then may split during post cementation or subsequent function. The thickness of the remaining dentin is the prime variable in fracture resistance of the root. Experimental impact testing of teeth with cemented posts of different diameters7 showed that teeth with a thicker (1.8 mm) post fractured more easily than those with a thinner (1.3 mm) one.
Photoelastic stress analysis also has shown that internal stresses are reduced with thinner posts. The root can be compared to a ring. The strength of a ring is proportional to the difference between the fourth powers of its internal and external radii. This implies that the strength of a prepared root comes from its periphery, not from its interior, and so a post of reasonable size should not weaken the root significantly.19 Nevertheless, it is difficult to enlarge a root canal uniformly and to judge with accuracy how much tooth structure has been removed and how thick the remaining dentin is. Most roots are narrower mesiodistally than faciolingually and often have proximal concavities that cannot be seen on a standard periapical radiograph. Experimentally, most root fractures originate from these concavities, because the remaining dentin thickness is minimal.20 Therefore, the root canal should be enlarged only enough to enable the post to fit accurately and yet passively while ensuring strength and retention. Along the length of a tapered post space, enlargement seldom needs to exceed what would have been accomplished with one or two additional file sizes beyond the largest size used for endodontic treatment. Because of the more coronal position of the post space, a much larger file must be used to accomplish this (Fig. 12-9).
Preparation of coronal tissue
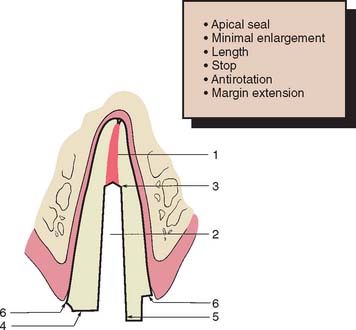
Endodontically treated teeth often have lost much coronal tooth structure as a result of caries, as a result of previously placed restorations, or in preparation of the endodontic access cavity. However, if a cast core is to be used, further reduction is needed to accommodate a complete crown and to remove undercuts from the chamber and internal walls. This may leave very little coronal dentin. Every effort should be made to save as much of the coronal tooth structure as possible, because this helps reduce stress concentrations at the gingival margin.21 The amount of remaining tooth structure is probably the most important predictor of clinical success. If more than 2 mm of coronal tooth structure remains, the post design probably has a limited role in the fracture resistance of the restored tooth.22,23 The once common clinical practice of routine coronal reduction to the gingival level before post and core fabrication is outmoded and should be avoided (Fig. 12-10). Extension of the axial wall of the crown apical to the missing tooth structure provides what is known as a restoration with a ferrule, which is defined as a metal band or ring used to fit the root or crown of a tooth, as opposed to a crown that merely encircles core material (Fig. 12-11). This is thought to help bind the remaining tooth structure together, simultaneously preventing root fracture during function.24–26 Although there is evidence that preserving as much coronal tooth structure as possible enhances prognosis, it is less clear whether the prognosis is improved by creation of a ferrule in an extensively damaged tooth through a surgical crown-lengthening procedure. In this latter circumstance, although the crown lengthening allows fabrication of a crown with a ferrule, it also leads to a much less favorable crown/root ratio and therefore to increased leverage on the root during function (Fig. 12-12).
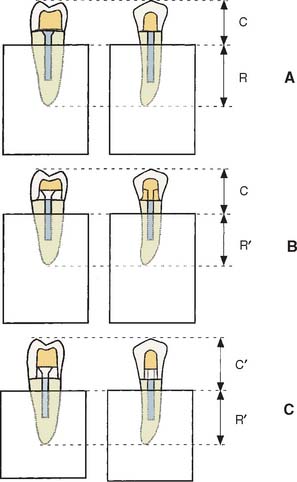
Fig. 12-12 Effect of apical preparation on crown/root ratio. A, Schematic of extensively damaged premolar tooth. Apical extension of the gingival margin would encroach on the biologic width (Chapter 5). This preparation has no ferrule. C, crown length; R, root length. B, Creating a ferrule with orthodontic extrusion (see Fig. 6-21) reduces root length (R′), whereas crown length remains unchanged. C, Surgical crown lengthening also reduces root length (R′) but increases crown length (C′). This results in a much less favorable crown/root ratio, which may, in fact, weaken the restoration.
(Courtesy of Dr. A. G. Gegauff. From Gegauff AG: Effect of crown lengthening and ferrule placement on static load failure of cemented cast post-cores and crowns, J Prosthet Dent 84:169, 2000.)
One laboratory study showed that creating a ferrule through surgical crown lengthening resulted in a weaker, rather than a stronger, restored tooth.27 In comparison, creating a ferrule with orthodontic extrusion may be preferred, because even though theroot is effectively shortened, the crown is not lengthened (see Fig. 12-12B).
Retention Form
Anterior teeth
Simultaneous dislodgment of an anterior crown with the post and core that retains it is frequently seen clinically and results from inadequate retention form of the prepared tooth.13,28 The normal faciolingual convergence of anterior teeth, coupled with smaller tooth size, complicates achieving such retention form. Post retention is affected by the preparation geometry, post length, post diameter, post surface texture, and the luting agent.
Preparation geometry
Some canals, particularly in maxillary central incisors, have a nearly circular cross-section (see Table 12-3). These can be prepared with a twist drill or reamer to provide a cavity with parallel walls or minimal taper, allowing the use of a preformed post of corresponding size and configuration. Conversely, canals with elliptical cross-sections must be prepared with a restricted amount of taper (usually 6 to 8 degrees) to ensure adequate retention and eliminate undesired undercuts. This is analogous to an extracoronal preparation (see Chapter 7). With extracoronal preparations, retention increases rapidly as vertical wall taper is reduced (see Chapter 7). Although retention can be further increased by use of a threaded post, which screws into dentin, this procedure is not recommended because of residual stress in the dentin. If the procedure is used, however, threaded posts must be “backed off” to ensure passivity; otherwise, the root will fracture.
| Circular | Elliptical | |
|---|---|---|
| Buccolingual | Mesiodistal | |
| Maxillary central incisor | ||
From Weine FS: Endodontic Therapy, 4th ed, pp 225–269. St. Louis, Mosby, 1989.
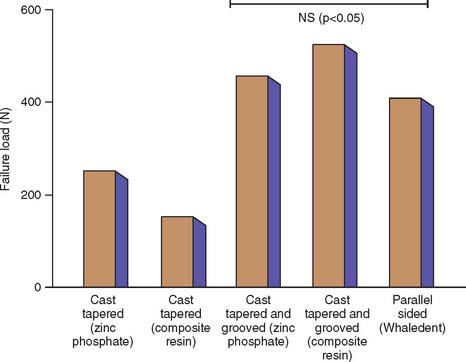
In accordance with this explanation, laboratory testing29–31 has confirmed that parallel-sided posts are more retentive than tapered posts and that threaded posts are the most retentive (Fig. 12-13). However, these comparisons are relevant only if the post fits the root canal properly, because retention is proportional to the total surface area.
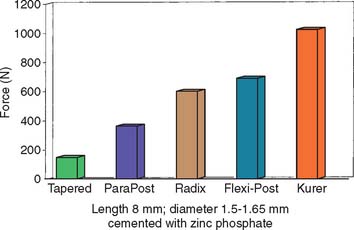
Fig. 12-13 Comparison of forces needed to remove different prefabricated post systems.
(Redrawn from Standlee JP, Caputo AA: The retentive and stress distributing properties of split threaded endodontic dowels. J Prosthet Dent 68:436, 1992.)
Circular parallel-sided post systems are effective only in the most apical portion of the post space, because the majority of prepared post spaces demonstrate considerable flare in the occlusal half. Similarly, when the root canal is elliptical, a parallel-sided post is not effective unless the canal is considerably enlarged, which would significantly weaken the root unnecessarily (Fig. 12-14).
Post length
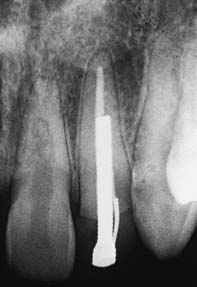
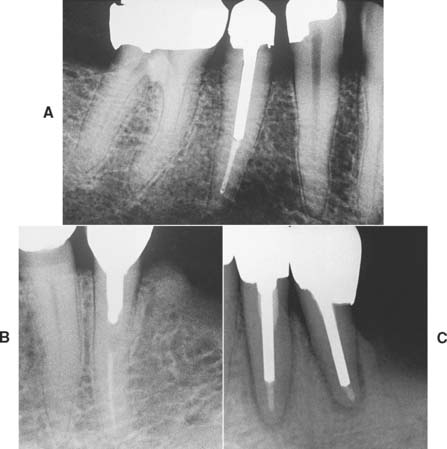
Studies29,31,32 have shown that as post length increases, so does retention. However, the relationship is not necessarily linear (Fig. 12-15). A post that is too short will fail (Fig. 12-16), whereas one that is too long may damage the seal of the root canal fill or risk root perforation if the apical third is curved or tapered (Fig. 12-17). Absolute guidelines for optimal post length are difficult to define. Ideally, the post should be as long as possible without jeopardizing the apical seal or the strength or integrity of the remaining root structure. Most endodontic texts advocate maintaining a 5-mm apical seal. However, if a post is shorter than the coronal height of the clinical crown of the tooth, the prognosis is considered unfavorable, because stress is distributed over a smaller surface area, thereby increasing the probability of radicular fracture. A short root and a tall clinical crown present the clinician with the dilemma of having to compromise the mechanics, the apical seal, or both. Under such circumstances, an apical seal of 3 mm is considered acceptable.
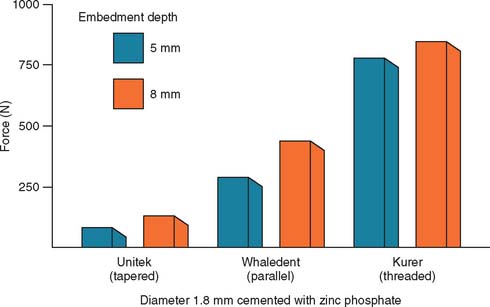
Fig. 12-15 Effect of the depth of embedding a post on its retentive capacity.
(Data from Standlee JP, et al: Retention of endodontic dowels: effects of cement, dowel length, diameter, and design. J Prosthet Dent 39:401, 1978.)
Post diameter
Increasing the post diameter in an attempt to increase retention is not recommended because the results are minimal retentive gain and unnecessary weakening of the remaining root. Although one group of investigators33 reported that increasing the post diameter increased retention, other reports do not confirm this.29,30 Empirical evidence suggests that the overall prognosis is good when post diameter does not exceed one third of the cross-sectional root diameter.
Post surface texture
A serrated or roughened post is more retentive than a smooth one,30 and controlled grooving of the post and root canal34 (Fig. 12-18) considerably increases the retention of a tapered post.
Luting agent
In considering traditional cements, the choice of luting agent seems to have little effect on post retention35,36 or the fracture resistance of dentin.37 However, adhesive resin luting agents (see Chapter 31) have the potential to improve the performance of post and core restorations; laboratory studies have shown improved retention.38,39 Resin cements may be indicated if a post becomes dislodged. Resin cements are affected by eugenol-containing root canal sealers, which should be removed by irrigation with ethanol or etching with 37% phosphoric acid if the adhesive is to be effective.40 Zinc phosphate and glass ionomer have comparable retentive properties, whereas polycarboxylate and composite resin cements have slightly less.41 Some resin and glass ionomer cements have demonstrated significantly higher retention than resin-ionomer cements,42 although the choice of luting agent may become more important if the post has a poor fit within the canal.43 A post and core should be remade if any rotation or wobble is present.
Posterior teeth
Relatively long posts with a circular cross-section provide good retention and support in anterior teeth but should be avoided in posterior teeth, which often have curved roots and elliptical or ribbon-shaped canals (Fig. 12-19). For these teeth, retention is better provided by two or more relatively short posts in the divergent canals.
When amalgam is used as the core material, it can be condensed either around cemented metal posts or directly into short, prepared post spaces. If a reasonable amount of coronal tissue remains, use of a single metal post that is cemented in the largest canal can provide adequate retention for the core material. When more than 3 to 4 mm of coronal tooth structure with reasonable wall thickness remains, use of a post in the root canals for retention is not necessary, and this reduces the risk of perforation.44 When a post is not used, the chamber must provide adequate retention for the core material. It may then be advantageous to prepare several short divergent post spaces into which the core material extends. Use of the canals for retention can provide good results,45 although once a complete crown has been provided, the strength of the tooth is not dramatically influenced by differences in technique.
Mandibular premolars and molars with a reasonable amount of remaining coronal tooth structure, when coupled with a circumferential cervical band of tooth structure with restricted taper of about 2 mm, can often be restored with amalgam directly condensed into the chamber. Core buildups in molars with one or more missing cusps benefit from one or more cemented posts around which the amalgam can be condensed. The posts provide the additional retention, which was compromised because of the missing tooth structure. In mandibular molars, the larger distal canal is recommended for post placement. In maxillary molars, the palatal canal is used (see Fig. 12-2C and D).
Although it is possible to restore a severely compromised molar with three or more missing cusps with multiple posts and amalgam, the tooth’s overall importance must be assessed, as the prognosis of such teeth is often guarded. If retaining the tooth is crucial and optimal strength is needed, a multipiece cast core can be used (made in sections that have different paths of withdrawal) (Fig. 12-20). An alternative preparation method for a posterior tooth is selecting the canals that are widest (normally the palatal of maxillary molars and the distal of mandibular molars) for the major post and then preparing short auxiliary post spaces in the other canals with the same path of withdrawal (Fig. 12-21).
Resistance Form
Stress distribution
The influence of post design on stress distribution has been tested with photoelastic materials,20,32,46–48 strain gauges,49,50 and finite element analysis.51,52 From these laboratory studies, the following conclusions have been drawn:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses