11
Restoration of the worn dentition
The restorative management of patients with toothwear can range from simple restorations through to complex full-mouth rehabilitations and is dependent on the severity and progression of the tooth surface loss. Pertinent to the topic are the restorative challenges the worn dentition presents, the techniques available, the stability of the oral environment, the consideration of case selection, the patient’s demands and aspirations, the stages of wear and how they affect restorative choices.
TO RESTORE OR NOT TO RESTORE IS A CENTRAL QUESTION
Clinically, the decision to restore dental caries is made through assessment of the extent of cavitation, the caries susceptibility of the individual, the patient’s ability to regularly maintain the region relatively free of plaque and the risk of progression. The previously considered diagnostic modalities utilised for dental caries include radiographs, transillumination and laser diagnostics (chapter 7). However, for regions of toothwear, the decision is more difficult, given no such diagnostic modalities are applicable. In regions of toothwear, no cavitation exists. Affected surfaces have no ‘infected zone’ of bacteria or carious surfaces that need to be removed and instead surfaces have been eroded by extrinsic or intrinsic acids, with or without the influence of attrition and abrasive processes.
As considered in Chapter 8, a patient who is of good health, through normal intake of food and beverages, over a lifetime, will experience a certain amount of wear that would be classified as acceptable and non-pathological. Physiological wear is another term for non-pathological wear. It is when an individual experiences extreme deviation from the norm that accelerated rates of tooth structure loss could lead to ‘pathological’ wear. Smith and Knight (1984) considered whether a tooth surviving the rate of wear could form the basis of distinguishing acceptable and pathological wear at any given age. Hence, it follows that at any given age, a certain amount of toothwear is non-pathological, physiological and normal for that age. Whilst theoretically providing an arbitrary and conceptual approach upon which to base the decision to restore a tooth or not, unless toothwear is extreme or the patient insists on pursuing intervention, it is often difficult to determine this clinically. If a patient is managed optimally with preventive advice, lifestyle and dietary advice, and remineralisation products, could the toothwear be stabilised, and if so, why then restore? The state of balance of the oral environment is one important determinant. In deciding to restore or not to restore, consideration must be given to the benefits and risks of restorative intervention, any restorative challenges, the stage of wear, the patient’s demands and aspirations, as well as the clinician’s skills and preferences and case selection, all of which are further considered.
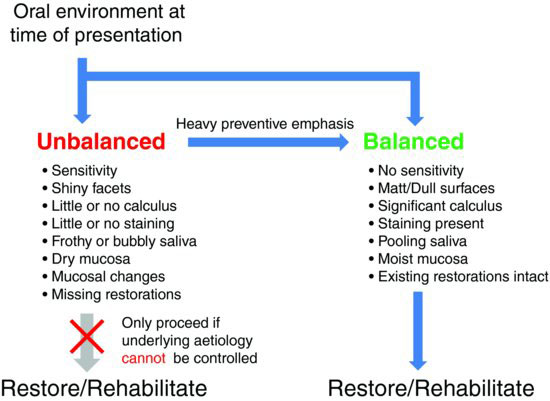
Figure 11.1 Consideration of the oral environment is given at the time of assessment to assist the decision-making process in deciding to commence restoration or rehabilitation of the worn dentition. (From Khan et al., 2010, with permission from Copyright Publishing Pty Ltd.)
PRE-RESTORATIVE TREATMENT – PREPARATION AND PLANNING
Prior to the commencement of any restorative treatment to replace lost tooth structure from toothwear, it is essential to ensure that the oral environment is stable and toothwear and disease have been controlled and particular indicators should be looked for (Fig. 11.1).
When restoring toothwear, it should always be aimed to do so within a balanced oral environment. In cases where the balance cannot be created and, at the extreme, remains heavily unbalanced, a compromised result is envisaged from the start. Cases where the underlying loss of salivary protection cannot be corrected, such as due to medication-induced reduction from a medication that cannot be altered, or patients with chronic reflux conditions, where despite medical intervention and medications, no further improvement can be achieved, will challenge restorative materials. If underlying factors cannot be altered through preventive efforts and adjuncts, limited improvement in the balance of the oral environment will be achieved. Restorative options should be thoroughly discussed with such patients. The restorative result is likely to offer some protection, but its longevity will be significantly reduced.
Raising the patient’s awareness of the causative factors of the toothwear and minimising further damage are essential in this pre-restorative phase of treatment. Changing the balance from demineralisation to remineralisation not only prevents further tooth structure loss but may reduce sensitivity caused by an active erosion process (Prati et al. 2003). This remineralisation is also critical in establishing a stable substrate for adhesive restorations. In the absence of a remineralisation potential, mineral from tooth structure is lost and the resultant demineralised surface is weak, unsupported and prone to breakdown. This surface is also unsuitable for restorative adhesion as the interface between restorative material and tooth substrate will be compromised, and it has been shown that bond strengths to hypomineralised enamel are significantly lower than those to unaffected enamel (William et al. 2006). This hypomineralised surface not only leads to adhesive failures with the restorative material, but it is also possible to obtain cohesive failures within the tooth surface related to weakness in the demineralised surface. To minimise the risk of failure, it is therefore necessary, prior to any restorative treatment, for the tooth surface to be remineralised and strengthened to optimise interface adhesion. Preventive advice, modalities and adjunctive products available are further discussed in Chapter 7. The important role the oral environment and influence of intrinsic and extrinsic acids play in determining restorative success should not be underestimated as restorative clinicians are most often preoccupied in restoring areas of imbalance, namely the sites of low salivary protection and high exposure to acids.
RESTORATIVE CHALLENGES
At the patient level, maintaining a balance in the oral environment and patient compliance to continue with preventive modalities are the primary challenges to restorative success. Health, lifestyle, dietary, work- and sports-related factors will hence have an impact.
At the dentition level, as toothwear progresses, changes in the vertical dimension of occlusion quickly ensue. Whilst in cases of rampant dental caries and coronal breakdown, some changes may be noted, toothwear processes pose a far greater threat to the vertical dimension. In a moderately or severely worn dentition, the sheer numbers of occluding surfaces present a challenge. Treatment more often than not requires multiple teeth to be restored.
The surface area of toothwear lesions is greater. At the tooth level, more dentine is exposed and less enamel is available to bond to. Enamel is often the first surface to be lost, and more often than not, dentine forms the predominant surface to be restored. Whilst the bond strengths of dentine adhesives are improving, these have not reached the bond strengths achievable between composite resin and enamel.
RESTORING THE STAGES OF WEAR
Depending on severity, restoration of a worn dentition varies greatly from placement of a few selective restorations to protect certain areas of wear from progressing to elaborate staged rehabilitation. This process may involve a few or many visits over a considerable time frame of months to years or even an interdisciplinary approach. Clinically, the restorative management of lesions of dental caries differs greatly. Variations in the site specificity and lesion morphology of toothwear have been considered in Chapter 4 and are quite different from those of dental caries. Hence, approaches for restoring dental caries are not applicable for management of toothwear lesions.
Due to differences in exposure and clearance levels of intrinsic and extrinsic acids, attritional and abrasive influences, and salivary protection, it is rare to find lesions of only one stage of wear within a dentition. The more severe the stage of wear affecting a tooth is, the more complex the restorative requirements are likely to be. The importance of offering pulpal protection increases as well. Therefore, consideration is next given to restorative aspects applicable for differing types of toothwear.
Restoring stage A – attrition
Attrition facets are by definition from tooth-to-tooth interaction, hence offering restricted or nill restorative space without changing the occlusion. When found affecting only the enamel, facets do not require restoration. Mandibular anterior teeth are often found to have attritional facets incisally, but are less of an aesthetic concern compared to those on maxillary incisor teeth, which may be affected in severe cases where forward posturing of the mandible has created an edge-to-edge bite, or this was pre-existing. In normal class I occlusion, patients with severe attrition may require restoration of palatal surfaces of the maxillary anterior teeth to offer pulpal protection. Those facets involving dentine exposures on the posterior teeth pose a significant clinical challenge. Over time the direction of the shearing force across the facet affects the margin on the leading edge and the body of the restoration. The same applies, but with lesser forces, to the restorations of the incisal edges of the anterior teeth. In cases of dentine exposure, lack of interarch space restricts use of the glass ionomer and composite resin sandwich technique. Composite resin remains the material of choice.
Restoring stage B – erosion
The chipped and worn incisal edges of the anterior teeth are commonly observed in patients with erosion and often restored given the aesthetic changes. Thinning of enamel and exposure of underlying dentine may, with further lesion progression, result in a deep scooping effect similar to the cupping seen in the premolar and molar teeth. Whilst only the incisal edges are affected, sufficient enamel remains on facial surfaces to allow bevelled extensions of resin restorations to be placed for improved retention, resistance and aesthetics. Cup lesions are characteristically seen on the cuspal inclines or apices of the molar and premolar teeth. These lesions are undercut free. Whilst in time gone by amalgam may have been used to restore these area, placement of undercuts on these surfaces contravenes conservation of tooth structure principles. Placement of a glass ionomer liner for improved dentine bonding and a covering layer of composite, as per the sandwich technique, is the ideal management for lesions extending into dentine, particularly in the mandibular molar teeth, which compared with the maxillary molar teeth are far more commonly and extensively affected by these lesions (Khan et al. 2001). Glass ionomers, may dissolve with time in a highly acidic oral environment or under conditions of low saliva flow. Their wear resistance when placed on occlusal surfaces, unless resin reinforced, is inadequate.
Restoring stage C – cervical lesions
Indications for restorations include the provision of pulpal protection in deeper cervical regions, particularly where underlying lifestyle, dietary and health factors cannot be controlled. Complicating factors in terms of restoration placement mirror those of caries lesions on class V surfaces in that the close proximity to the gingival margins, gingival crevicular fluid and bonding surfaces available all affect restoration longevity, plaque retention, periodontal changes and recurrent caries.
Placing a restoration in order to ‘treat’ sensitivity is conceptually difficult to justify. Deep cervical lesions encroaching upon pulpal regions should be restored to offer protection, providing justification for restorative intervention. Cervical grooved restorations on the facial surfaces of maxillary incisor teeth are well restored with composite veneers or traditional veneers to improve aesthetics of the affected areas. However, the need for restorative intervention for shallow cervical lesions remains uncertain. In a review of the literature on non-carious cervical lesions, Wood et al. (2008) concluded that the value in restoring non-carious cervical lesions is unclear and occlusal adjustments to prevent lesion progression or improve retention of restorations cannot be supported. It follows that tooth flexure and abfraction are not sustainable answers to explain why certain cervical restorations in non-carious regions fail prematurely. Sakoolnamarka et al. (2002) and Tyas and Burrow (2007a, b) considered bond strengths of various dentine-bonding agents and restoration of non-carious cervical lesions, as well as possible reasons for restorative failure of bonded restorations attributable to the differences compared to regions of normal dentine. They concluded that significant doubt exists as to the importance of the involvement of abfraction in restorative failure and instead considered non-carious cervical lesion surfaces to:
1. have a lower phosphate-to-silicon ratio compared with normal dentine;
2. have dentine surfaces that were more highly mineralised with greater proportions of obliterated dentinal tubules;
3. lack a smear layer, such that etching exposed far more collagen fibres compared with normal dentine;
4. create a thinner hybrid layer when bonded to.
If the decision is made to restore non-carious cervical lesions, principles of conservation of tooth structure dictate that ideally no further cavity preparation occurs other than a fine bevel along the coronal enamel margin. Mild pumicing and mild etching are beneficial. However etch times should be reduced.
Restoring stage D – degradation
Degradation describes lesions resulting from the fusion of occlusal and cervical or incisal and cervical regions, involving considerable loss of tooth structure and significant dentine exposure, often with minimal enamel remaining. Posteriorly, few molar teeth reach stage D as cervical lesions are less common. It is the maxillary and mandibular premolar teeth and maxillary incisor teeth that are most commonly affected and require restoration. The direct restorative materials selected are those with stronger dentine-bonding abilities. At the expense of further tooth preparation, the utilisation of onlays, veneers and crowns may offer a longer term option.
Restoring stages E and F – near-exposure and frank exposure
Near-exposures require pulp capping to protect vital structure, and the maxillary anterior and premolar teeth are most commonly affected. Restoring such areas changes the occlusion given the often tight interarch spacing that exists. Enamel available is restricted to gingival margin areas only. The bite opening created requires neighbouring teeth to also be restored, as discussed later. Deep cervical lesions with near-exposures pose a different challenge, namely, at the gingival margin. Moisture control and marginal accuracy are imperative for long-term restorative success. Plaque retention around margins may create potential for periodontal or caries-related changes. Frank exposures involve irreversible pulpitis and involve root canal treatment. The health of the remaining dentition is assessed when deciding the strategic value of the affected tooth, and alternative treatment options include extraction with or without replacement. When a patient presents with a frank exposure, often multiple neighbouring teeth will have near-exposures, warranting restoration to protect vital structures.
Table 11.1 Aesthetic considerations.
| Treatment parameters for aesthetic restorations: |
| Does the clinical crown need restoration to an aesthetically pleasing height? |
| Can the incisal edge be restored aesthetically and be able to resist biting stresses? |
| Has reduction of clinical crown height permitted passive eruption of the opposing teeth? |
| What adjustments need to be made to the occlusal vertical dimension to allow sufficient material thickness to resist the forces of the occlusion? |
| Does intact proximal enamel need to be removed for indirect restorations? |
| Will the restoration thickness be sufficient for the selected dental materials to mask out underlying dentine shades/colour to achieve the aesthetic outcome desired? |
| Will the cervical margin be compatible with gingival health? |
| What materials(s) are needed to cover the lingual or buccal degraded dentine surface to obtain retention and protect the pulp? |
PATIENT DEMANDS, ASPIRATIONS, AESTHETICS AND CASE SELECTION
The demands and expectations a patient presents with range from relief of acute symptoms to full-mouth occlusal rehabilitation and requests for smile makeovers. A patient may be concerned about a particular tooth or their entire dentition. Immense variation between patients exists as to what longevity they expect from the result. This needs to be carefully discussed and potential pitfalls identified given the challenges the worn dentition may present. Treatment costs, the number of appointments required and the need for ongoing maintenance are important discussion points. Informed consent is required.
Trends within society are changing. A set of flat and heavily worn teeth is a deviation from the perceived smile curve that resembles ‘good health’. In most parts of the developed world it is rare to encounter people with missing anterior teeth in public. Most would seek immediate replacement of an anterior tooth. Previously, worn incisal edges were more commonly identified as age related, whilst these days patients are more likely to request restoration regardless of their age. Restorative considerations relevant to toothwear are detailed in Table 11.1. Before and after photographs of any such treatment are important and should be documented for more elaborate cases.
Of the more elaborate and challenging cases, the clinician should choose to restore clinical cases in which a confident diagnosis was reached and thereafter appropriately managed with preventive modalities which have stabilised the oral environment. Furthermore, the patient and clinician both should agree on the further interventions and be satisfied with the treatment processes and risks involved to achieve the outcome. The patient should demonstrate a high level of compliance to assist the dental team in achieving the desired result and maintaining this. Patient compliance may vary significantly over time, and whilst many patients are keen early on, their interest may reduce with time or where multiple restorative failures are encountered or their lifestyle and work-related interests restrict their dental attendance levels. Where the patient continues to exhibit an imbalanced oral environment despite the preventive modalities implemented, the clinician should not feel pressured to proceed with elaborate restorative treatment and instead should be careful to discuss and document their concerns and any effects this imbalance is likely to have on restorative prognosis. Indirect crown and bridge approaches in such patients should be avoided and instead focus should remain on conservative restorative options.
CONSERVATIVE RESTORATIVE OPTIONS FOR PARTIAL OR FULL-MOUTH OCCLUSAL RECONSTRUCTION
Often it is not until toothwear is well advanced that patients seek treatment, at which time the aesthetics are notably affected and/or teeth are hypersensitive (Lussi et al. 2006). It has previously been considered that the definitive restorative treatment for moderate and severe toothwear encompasses multiple crowns and bridges to restore form and function (Thongthammachat-Thavornthanasarn 2007). These indirect restorative treatments tend to be complex, highly invasive and costly, and many patients are not in the position to commence treatment immediately and prefer to delay it until they perceive it becomes essential. Consequently, the extent of toothwear may become even more severe before any definitive treatment is provided, which may further compromise the success of the tr/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


