Chapter 11
Case Histories
Despite its apparent simplicity, the definitive diagnosis and management of oral potentially malignant disorders remains both a complex and controversial topic for clinicians. In this chapter, therefore, we will present a number of illustrative case histories summarising the clinical presentation, histopathological diagnoses, treatment and clinical outcome for a diverse group of patients. A commentary to highlight some of the salient features of each scenario is also included. The aim of reviewing these cases is to demonstrate the principles and practice of diagnosis and clinical management, and to examine the decision-making processes expounded in the preceding chapters of this book when applied to the actual treatment of specific potentially malignant disorders of the oral mucosa.
The patient scenarios have been chosen not only to summarise common clinical presentations but also to help demonstrate some of the inherent management dilemmas seen in these clinical situations. Sometimes the decision-making process can be quite demanding and unfortunately, as we have discussed previously, there is a very limited evidence base to help guide clinicians in the treatment of many of these situations.
Case 1: Diagnosis of Unexpected Malignancy
Clinical Presentation
A 65-year-old male patient presented with a localised patch of erythroleukoplakia arising in the right anterior floor of mouth (Figure 11.1A). He had a 40-year history of tobacco smoking, usually in excess of 20 cigarettes per day, heavy and regular alcohol consumption for many years and was suffering from early-stage alcohol-related dementia when first seen. Otherwise, his medical history was relatively uncomplicated.
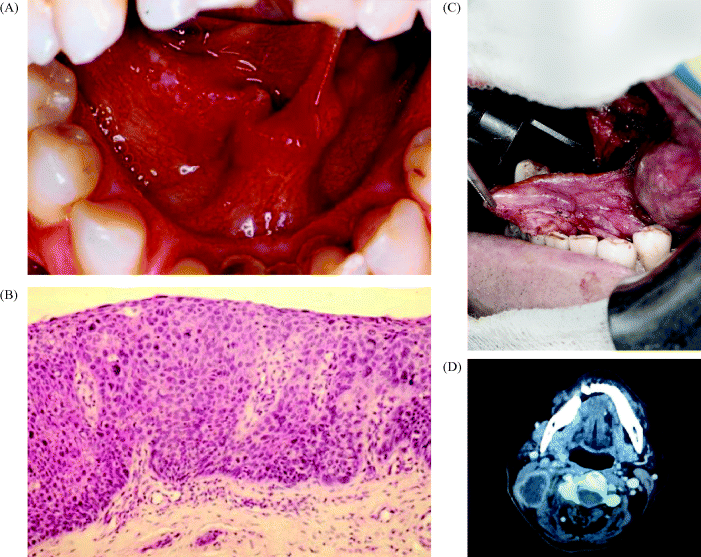
Figure 11.1 A 65-year-old male patient presenting with erythroleukoplakia in the right anterior floor of the mouth (A), provisionally diagnosed as severe dysplasia histopathologically on incisional biopsy (B). (C) Ultimately it proved to contain an early invasive squamous cell carcinoma following laser excision. (D) Fourteen months following laser surgery, a large necrotic tumour mass presented in the neck, visualised in this CT image, which also shows a smaller metastatic node situated just anterior to the sternomastoid muscle.
Histopathological Diagnosis
An incisional biopsy of the floor of mouth lesion was carried out under local anaesthesia and revealed a provisional histopathological diagnosis of severe epithelial dysplasia (Figure 11.1B).
Management
In view of the presence of the severely dysplastic oral mucosa and concerns that the patient would be unlikely to stop both his smoking and his alcohol consumption, treatment comprised laser excision of the erythroleukoplakic lesion, together with a wide margin of apparently normal mucosa (Figure 11.C). This was carried out within 2 months of his initial biopsy under general anaesthesia using the protocol described in detail in Chapter 7.
Upon histopathological examination of the excision specimen, however, a focus of superficially invasive, moderately differentiated squamous cell carcinoma was found although this had been completely excised during the laser surgery. All excision margins were reported to be free of both carcinoma and dysplasia.
The patient subsequently attended the multidisciplinary head and neck cancer clinic 1 month post-laser surgery. Following clinical assessment, which confirmed no residual oral disease, and computed tomography (CT) scanning, which showed no cervical lymphadenopathy suspicious of metastatic disease, he was placed under regular monthly review and careful clinical examination.
Clinical Outcome
Unfortunately, the patient only attended semi-regularly for his follow-up appointments probably as a result of his mild mental confusion, which resulted in him forgetting a number of scheduled appointments. Ultimately, at 14 months following laser surgery and after an absence from the clinic of some 4 months he re-presented, being brought back to hospital on this occasion by a concerned relative.
On clinical examination, there was a 5 cm diameter firm and fixed mass at level II in the right neck which was highly suspicious of a large deposit of metastatic carcinoma. The patient could not recall when the mass first appeared, but a visiting relative had noticed it on a domestic visit 2 weeks previously and the patient now felt it was both painful and growing rapidly in size. Intra-oral examination confirmed good healing, with minimal scarring, of the floor of the mouth at the site of the previous laser surgery and no sign could be found of any recurrent or further oral mucosal disease. Neither was there any evidence of a second primary carcinoma in the head and neck to account for the presumed metastatic lymph node disease.
Fine needle aspiration of the neck mass was carried out that confirmed the presence of squamous cell carcinoma. A CT scan of the neck was performed that visualised the large necrotic level II lymph node together with a smaller but suspiciously enlarged additional node, both of which displayed features characteristic for metastatic carcinoma. A representative image from this CT scan is shown in Figure 11.1D.
The patient subsequently underwent a radical neck dissection, which completely excised the tumour mass and confirmed the diagnosis of metastatic carcinoma with extracapsular lymph node spread around both the nodes described above, but with no other lymph node involvement. A course of adjuvant postoperative radiotherapy was applied bilaterally to the neck, and to date the patient remains well with no evidence of further disease.
Comment
It is unlikely that such a rapidly growing lymph node metastasis could have been predicted from the initial presentation of this oral lesion. Indeed, as discussed in Chapter 9, foci of unexpected carcinoma are found in approximately 10% of laser excision specimens and following their removal patients usually respond very well, attending for regular and detailed postoperative surveillance.
The site of the large necrotic node at level II was a slightly unusual presentation for an anterior floor of mouth carcinoma, which one would normally expect in the first instance to metastasise to level I submandibular lymph nodes. Nonetheless, no evidence of a synchronous primary tumour elsewhere in the head and neck region could be found, and the histological features of the neck metastasis were consistent with an origin from the initial floor of mouth lesion.
It was clearly unhelpful that the patient’s mental state and social situation in this case prevented his re-attendance at clinic for several months when an earlier diagnosis of cervical lymphadenopathy may have been possible. The long-term prognosis for such a patient, of course, must remain guarded. Whilst the patient has agreed to stop smoking, there remain ongoing concerns regarding his alcohol consumption and the risks for both recurrent and further disease development.
Case 2: Multiple Lesion Disease Responding to Conservative Management
Clinical Presentation
A 49-year-old male smoker, who had smoked approximately 15 cigarettes per day for over 30 years, presented with widespread, faint leukoplakic lesions affecting the bilateral buccal mucosae and also the dorsolateral tongue. The clinical appearance of these lesions, all of them entirely asymptomatic, is shown in Figure 11.2.
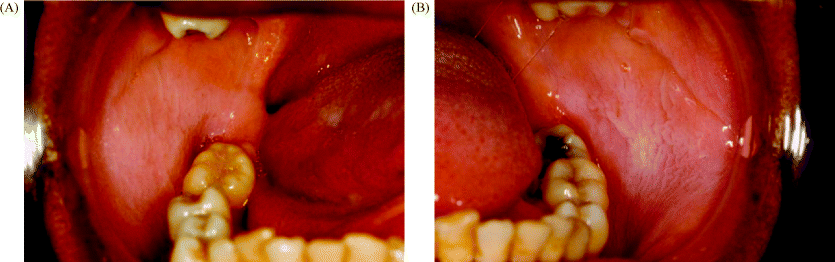
Figure 11.2 An example of widepsread, multifocal leukoplakia. There is feint leukoplakia on the right buccal mucosa (A), whilst the lesion on the left buccal mucosa exhibits a rippled or ‘ebbing’ tide appearance (B). A small, irregular patch of dorsolateral tongue leukoplakia is also seen in (A).
Histopathological Diagnosis
Incisional biopsies were taken from both buccal mucosal sites and also the dorsolateral tongue. These revealed histopathological diagnoses of hyperkeratosis at all sites, together with the presence of mild dysplasia, but this was only seen in the thickened leukoplakia arising on the left buccal mucosa.
Management
Following informed discussion, the patient undertook a period of smoking cessation counselling and, using nicotine replacement therapy, quit smoking completely by 4 weeks post diagnosis. No surgical intervention was undertaken.
Clinical Outcome
The patient was followed up closely with 3-monthly review appointments arranged during the succeeding 12 months, during which time continuous improvement in the clinical appearance of the oral mucosa was observed. The patient remained a non-smoker.
A repeat incisional biopsy was taken from faint residual leukoplakia on the left buccal mucosa 18 months following the initial diagnosis. On this occasion the biopsy showed hyperkeratosis only, with no cellular atypia or any residual dysplasia evident. Further clinical improvement was noted over the next 18 months and, at approximately 3 years following initial presentation, the patient was discharged from the dysplasia clinic to the care of his general dental practitioner.
Comment
The importance of stopping smoking in improving the long-term prognosis for oral potentially malignant disorder patients cannot be overemphasised. This is especially so for multiple lesion cases in which widespread laser excisions of dysplastic mucosa may be both impractical and potentially destructive. Repeat incisional biopsies at intervals in cases that are treated by reducing risk factor behaviour and clinical observation alone are extremely useful ways of monitoring progress and, even better, demonstrating the resolution of oral potentially malignant lesions.
Case 3: Multiple Lesion Disease Requiring Repeated Laser Treatments
Clinical Presentation
A 62-year-old female smoker presented with multifocal, non-homogeneous leukoplakia arising on the right dorsolateral tongue, the floor of the mouth and mandibular alveolus (Figure 11.3A). Similar non-homogeneous lesions also affected the left posterior buccal mucosa and edentulous mandibular alveolus (Figure 11.3B). The patient reported that she smoked about 20 cigarettes per day and had done so for nearly 45 years, but consumed little in the way of alcohol.
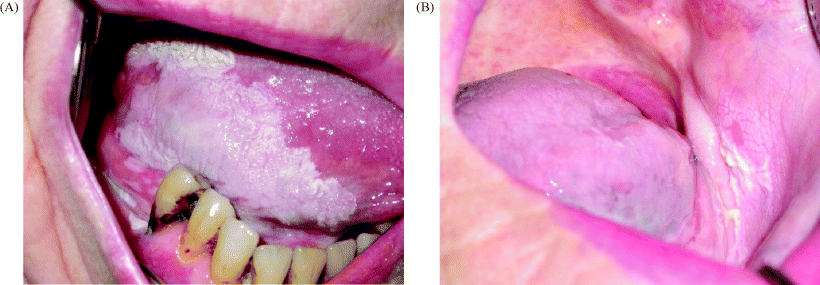
Figure 11.3 In this example of multiple lesion disease, there is widespread non-homogeneous leukoplakia affecting the right dorsolateral tongue, floor of the mouth and mandibular alveolus (A), whilst further non-homogeneous leukoplakia appears on the left buccal mucosa (B).
Histopathological Diagnosis
Examination under anaesthesia was undertaken and field mapping biopsies were taken from the right dorsolateral tongue, right floor of the mouth, right and left edentulous mandibular alveolar regions and left posterior buccal mucosa. Histological examination of the biopsy specimens revealed hyperkeratosis at each site but features consistent with a diagnosis of moderate dysplasia were seen in the tongue biopsy, whilst severe dysplasia was also identified in the buccal mucosa.
Management
Concerted efforts were made to encourage the patient to stop or at least reduce her smoking. Laser excisions of the right dorsolateral tongue leukoplakia and the left posterior buccal mucosa leukoplakia were undertaken.
Clinical Outcome
Complete resolution of the left buccal mucosa disease was seen but unfortunately the patient continued to smoke, albeit at a reduced number of cigarettes per day. Residual disease was observed on the right posterolateral tongue 6 weeks following laser treatment and further laser surgery was arranged to excise this lesion 4 months later. Clinical resolution occurred subsequent to this further surgery, but at 2 years follow up a recurrent patch of leukoplakia was observed arising at a more anterior location on the right lateral tongue. Incisional biopsy confirmed moderate dysplasia at this site and thus a third laser excision was carried out to remove this lesion.
Since then, the patient has remained free of lesions on the lateral tongue, whilst the leukoplakia seen originally at the floor of mouth and mandibular alveolar sites has remained although this is asymptomatic and has reduced in both lesion extent and thickness.
Comment
Repeated laser treatments are sometimes required, especially in cases with widespread multifocal disease. Patients usually tolerate multiple treatments well, scarring is not usually a problem and ultimately clinical resolution may be achieved. Long-term follow up is, of course, mandatory and, ideally, improved risk factor behaviour should be attempted.
Case 4: Proliferative Verrucous Leukoplakia
Clinical Presentation
A 45-year-old male patient presented who complained of an ‘uncomfortable and roughened patch of gum’ affecting his left mandibular buccal gingiva in the premolar and molar regions. He also reported intermittent soreness of his gingiva at various other oral sites. The patient was a non-smoker, consumed less than 5 units of alcohol per week and was generally fit and well.
Clinical examination revealed a linear, raised patch of proliferative verrucous leukoplakia (PVL) extending from the first premolar to the second molar tooth and affecting both the marginal and attached buccal gingivae (Figure 11.4A). There were also lichenoid lesions affecting the right posterior maxillary buccal gingiva and the adjacent buccal mucosa together with a localised verrucous leukoplakic patch affecting the right anterior maxillary gingiva.
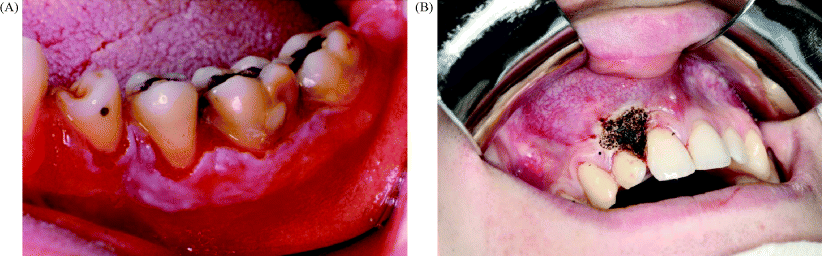
Figure 11.4 (A) An example of proliferative verrucous leukoplakia arising on the mandibular buccal gingival. (B) Following laser ablation of a more localised verrucous lesion on the maxillary gingiva.
Histopathological Diagnosis
Incisional biopsies were taken under local anaesthesia from both the mandibular leukoplakic gingival lesion and the maxillary buccal gingiva. The lesions had common histopathological appearances, specifically the appearance of verrucous hyperplasia and lichenoid inflammatory change in the subjacent connective tissue. In addition, mild epithelial dysplasia was observed in the left mandibular gingiva specimen. A provisional diagnosis of PVL was thus made.
Management
A detailed examination of the entire oral cavity and oropharynx was carried out under general anaesthesia, although no additional mucosal lesions were identified. Immediately following this, laser ablation of the left mandibular gingival lesion and the right maxillary anterior gingiva was carried out using the surgical technique described in Chapter 7. Figure 11.4 B demonstrates the post-laser ablation appearance of the maxillary gingiva. The patient was subsequently followed up in the dysplasia clinic.
Clinical Outcome
Excellent gingival healing with minimal />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


