Chapter 1
INTRODUCTION
1.1 Introduction
This book has been designed for use in the dental laboratory as a guide for the novice dental technician. Described in the manner of a ‘cook book’, the procedures in this handbook have been designed to be followed step by step. Presented in sections ordered by specialty, each procedure has been completed in a dental laboratory, with photographs illustrating all the important steps of each procedure. The work shown in this book has not been edited or tweaked, but is presented as the instructions given in this book were followed, to ensure that the outcomes are achievable by anyone following the guides (perhaps with a little practice!).
1.2 How to use this book
Working impression
Casting working model
Sectioning
This book is designed for the student of dental technology for use on the bench in the dental laboratory. The construction of many dental prostheses and appliances require progression through a series of stages, often from impression through to finished product. You can use this book to work through each procedure step by step.
The graphic at the beginning of the sections will help you to see where any given procedure fits into the production process. An example of this is shown on the right.
For each procedure you will find a brief introduction, a list of the tools and equipment required, guidance on working safely, and an illustrated step-by-step basic procedure.
In addition, the hints and tips sections give techniques to expand or refine the process, and the extended information sections give an insight into the scientific and clinical aspects that can enhance your understanding of the topic.
1.3 Equipment and instruments
The equipment listed below is commonly found in a dental laboratory, and with which any technician should be familiar.
Plaster bowl, spatula and knife (Figure 1.3.1)
Common to all plaster rooms, these items are used for mixing, shaping and trimming plaster of Paris, Kaffir and die stone materials. Cleanliness of these items is important to prevent rapid setting of materials.

Wax knives and carvers
These instruments are commonly used in the laboratory for a number of procedures. You should purchase your own good quality knives and carvers.

Small wax knife: Most commonly used in the fabrication of crowns for placing and carving inlay wax. You may see technicians using two, a cold and a hot knife to save time (Figure 1.3.2, instrument on left).
Large wax knife: Used for melting, placing and carving modelling wax in the production of dentures. Again it is common to see two knives being used, a cold and a hot knife (Figure 1.3.2, instrument on right).

LeCron carver: This carver is popular for the carving of inlay wax in the production of crowns. It is used cold, but some techniques use it slightly warm, but not hot (Figure 1.3.3, instrument on far right).
Ash 5: This carver is used cold to shape modelling wax in the production of dentures (Figure 1.3.3, instrument in the centre).
Hylin carver: This carver is popular for the carving of inlay wax in the production of crowns. It is used cold (Figure 1.3.3, instrument on far left).

PKT (PK Thomas): A set of instruments (examples of two shown) designed to aid the precise positioning of molten wax in the production of crowns (Figure 1.3.4).
Other hand instruments

Ceramic brushes: Available in a range of sizes like artists’ brushes (Figure 1.3.5), with sizes from 0 to 20 with 0 being the smallest and 20 the largest. These brushes are made from sable and should be treated with care. A size 6 is popular for the placement of ceramics in the production of crowns. Smaller brushes are useful for staining, and a larger brush for condensing ceramic.

Ceramic spatulas: These instruments (Figure 1.3.6) are used for mixing, placing and carving of ceramic powders. They are produced from a material that will not contaminate the ceramic with metal particles that may cause discoloration.
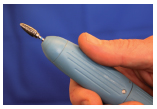
Micromotors: Modern micromotors (Figure 1.3.7) are very advanced in terms of engineering, control and quality. They are powered by low voltage electricity and usually controlled via a foot or knee controller, allowing the speed to be set anywhere between 5000 and 40 000 rpm. The chuck is opened and closed by twisting the handpiece to secure or remove a bur.
Burs
There is a huge range of burs currently on the market and manufactures devote several pages of their catalogues to them. Below is a brief outline of the main types.

Tungsten carbide (TC): These are very popular burs used for many applications within the laboratory from trimming plaster to acrylic and metal. They are available in a large selection of shapes and sizes (Figure 1.3.8). The most useful are the plaster trimmer, flame-shaped for trimming acrylic, and small round (often called rosehead) burs for accessing small areas.
Steel burs: As above but not as hard wearing (and cheaper).

Stone burs: Abrasive stone burs are available in different grades, shapes, sizes and materials. The shapes range from cones to points to discs (Figure 1.3.9) and the different materials are indicated (often by colour) for different applications, i.e. for the trimming and finishing of ceramics, acrylics or alloys.

Diamond discs and burs: Increasing popular over the past decade, these tools are used for the shaping of ceramics and composites. They are available in many shapes and sizes (Figure 1.3.10).

Rubber abrasives for metals: These are available as wheels, cones or points and used mainly in the finishing of metal surfaces (Figure 1.3.11).

Abrasives for acrylics: The simplest is a mandrel that holds a small piece of sandpaper, but rubber-bonded abrasives are now popular (Figure 1.3.12).

Brushes and mops: The main application of these is the polishing of metal surfaces in combination with wax-based polishing compounds (Figure 1.3.13).
Pliers and cutters
For orthodontic appliance manufacture (or for any other occasion where a wire may need to be bent or cut) the technician will have a selection of tools.

Adams 65: Square-ended pliers used in the bending of orthodontic stainless steel wire (Figure 1.3.14).

Adams 64: Square- and round-ended pliers used in the forming of springs and curves in orthodontic wires (Figure 1.3.15). (Sometimes referred to as ‘half-round’.)

Maun cutters: Used for the cutting of orthodontic stainless steel wire (Figure 1.3.16).

Parallel pliers: Used for firmly griping a variety of items (Figure 1.3.17).
Large laboratory equipment
Most laboratories will have most or all of the following (illustrations of some of the following equipment will appear later in the book).

Model grinder: A bench-mounted, water-lubricated, tungsten carbide wheel used to grind plaster products (Figure 1.3.18).



Polishing lathe: Used with brushes and pumice, or mops and polishing wax in the polishing of acrylics and alloys (Figure 1.3.19). Modern lathes have integrated dust extraction and lighting and have two speeds: 1500 or 3000 rpm. The polishing lathe can be fitted with a variety of brushes and mops, for example a bristle-brush for applying abrasive pumice to acrylics (Figure 1.3.20) or a cotton mop for polishing acrylics or alloys (Figure 1.3.21).
Steam cleaner: Used extensively in the dental laboratory for cleaning models and restorations.

Pressure bath: These use compressed air to keep self-curing acrylics under pressure during curing. They also have the facility to keep water warm to aid the process (Figure 1.3.22).
Hydroflask: Used full of water for putting self-curing acrylic under pressure while curing, in the repair of dentures for example.
Vibrating table: Used during the mixing and pouring of plaster materials to help avoid air bubbles.
Vacuum mixer: Essential in the production of models for fixed prosthodontics and for mixing investment materials. This machine mixes plaster materials mechanically in a sealed pot while sucking the air out of the plaster mix.
Boiling out machine: This machine keeps water hot enough to remove wax from moulds (for example in the production of complete dentures). It has a compartment in which moulds can be placed and automatically sprayed, or often there is a hand operated shower for manual spraying.
Presses: Presses are usually bench mounted and used to close denture flask (moulds). Hydraulic presses are also available for the same purpose. These work in the same way as a hydraulic car jack and require less force than manual presses.
Clamps: Denture flask clamps are used to keep flasks under pressure during the curing process required for heat-cured acrylics.
Denture flasks: Brass flasks used to create two part moulds of wax trial dentures in the conversion to acrylic dentures.
Curing bath (dry-heat or water): Used for the curing of heat-curing acrylic. Large enough to accept the mould and spring clamp, these machines have an automatic heating cycle to ensure optimum curing of the acrylic.

Porcelain furnace: These small, automated vacuum furnaces are specifically for the firing of ceramics (Figure 1.3.23). They are computerised and programmable, and can store the data for the various firing cycles required for different ceramics.
Burnout furnace: Relatively large for a dental technology laboratory, these furnaces are used in the heating of moulds and crucibles prior to casting. Modern furnaces are programmable to allow for preheating and the holding of high temperature during the heating cycle.
Casting machines: There are several types of casting machines combining the different casting forces (centrifugal, air pressure/vacuum) and different heating methods (induction, electrical resistance, gas torch, oxy-acetylene).
High-speed grinder: Bench mounted motor used with a cut-off disc or grinding wheel, for removing sprues and finishing cobalt-chromium alloy denture frameworks.
Spot welder: Used to weld stainless steel wire or components in the production of orthodontic appliances.
Ultrasonic bath: Used extensively for cleaning restorations or components of restorations in conjunction with different cleaning solutions.
Drying oven: A low temperature oven used for gently warming and drying refractory models used in the production of cobalt-chromium denture frameworks.
Electrolytic bath: Used in the ‘polishing’ of cobalt-chromium alloy frameworks.
Technician’s workbench: The workbench is often fitted with drawers, a gas supply for Bunsen burners, electrical sockets, a micromotor, dust extraction and colour balanced lighting.
Lighting: Lighting is an important feature of the dental laboratory in terms of long-term well-being for eyes working under demanding conditions. It is also essential to allow correct assessment of colour when producing aesthetic restorations. Tungsten or fluorescent lights can alter the perception of the shade being matched.
Shot-blaster: There are several types of shot-blaster using different sizes of abrasives (such as aluminium oxide or glass beads) for different purposes. Non-recirculating blasters are used in conjunction with extraction in the preparation and finishing of metal surfaces, for example in the production of metal-ceramic restorations. Recirculating blasters are used with larger grit materials in the removal of investment materials from cobalt-chromium frameworks.
1.4 Health and safety in the dental laboratory
There are many hazards in the dental laboratory and many procedures that have an element of risk attached to them; however, if we take time to assess the risks and hazards, hopefully we will be able to minimise, or in some cases eliminate, the potential for harm.
It is the responsibility of all who work in the dental laboratory to ensure that we work safely and that we minimise the risk of injury to ourselves and others. It can be said that the effect of our use or misuse of equipment and materials can affect the degree of risk from known health hazards in the laboratory. In order to make sure that the working environment is a safe one there are some simple steps that can be taken, such as carrying out a ‘risk assessment’ and identifying any hazards present.
What are hazards?
A hazard is anything that could possibly be damaging.
What are risks?
How something might be damaging to you or others.
Risk assessment
A risk assessment is an examination of what could cause harm to people. A risk assessment is done so that one can decide whether or not enough precautions have been taken to prevent accidents or injury.
Workers and others have a right to be protected from harm caused by a failure to take reasonable control measures.
How to assess the risks in your workplace
The easiest and most effective way that you can assess the risks and put in place measures to minimise the risks in your workplace is to follow the five-step plan given below.
1. Identify all hazards
Walk around your workplace to see what may cause harm, check manufacturer’s instructions on chemicals and think about long-term harm such as noise and dust.
2. Decide who might be harmed and how
Everyone does not have to be named but specific groups of people have to be considered, such as plaster room workers or acrylic room workers; members of the public also need consideration if they have access.
3. Evaluate the risks and decide on the precautions
Once the risks have been identified, it has to be decided what can be done to minimise or eliminate the risk. This can be done by some simple means such as limiting access to hazardous chemicals or using less harmful chemicals and substances. Use protective clothing and organise work so that exposure is minimised.
4. Record all your findings and make sure to put them in practice
If proper notes are made it will be easier to implement safe working practices; also remember to involve all staff so that a cohesive plan can be adopted by all to ensure the continued safety of all staff.
5. Regularly review your assessment and update when needed
All things are subject to change – number of employees, chemicals, working practices, etc. – so it is a good idea to review any risk assessment on at least a yearly basis so that any changes that have to be made can be done with relatively little disruption.
Assessing risks need not be an onerous task and if ‘Risk Assessment’ records are kept up to date, they can be carried out quickly and effectively with little hindrance to daily working practices.
Before starting to follow any procedure in this book, you should carry out a risk assessment. To help you, the Working safely section for each procedure outlines the main hazards.
1.5 Sterilisation and impression handling
Cross-infection in the dental laboratory
Cross-infection is a very real risk in the dental laboratory and one that should be taken seriously by all staff. Although it is the responsibility of the dentist to ensure that all items that are sent to the dental laboratory are sterilised, it is wise to treat everything with caution and not assume that we need not take basic precautions to minimise cross-infection.
The greatest risk to all members of the dental team is the patient and impressions that carry saliva; mucus and blood can pass disease on very easily. Workers in the dental laboratory do not usually see patients and in many cases are far away from the surgeries for which they carry out work. Being removed from the patient interface can lead to a feeling of not being directly involved with the clinical aspects of dentistry, but the impressions that we receive are a direct link with the patient and the clinic, and therefore must be treated accordingly.
Often the dentist will not know whether a patient has a communicable disease. Furthermore, the patient may not even know if they have a condition such as human immunodeficiency virus (HIV) infection or hepatitis so we have to make sure that we put into operation a cross-infection control procedure. Not only are we at risk from the patient but the patient also can be put at risk from the things that we do in the laboratory.
Cross-infection control procedure and policy
All laboratory staff should understand the cross-infection control procedure required in the dental laboratory and follow good practice.
For further information contact the Dental Laboratories Association (DLA), British Dental Association (BDA), British Dental Trade Association (BDTA) or the Health & Safety Executive.
1.6 Introduction to model making
Most procedures in the dental laboratory are carried out on some form of plaster model, which is produced from an impression. There are several different model types that are produced for different applications.
In common to all is that care and attention to detail is required to produce an accurate, flaw-free model, which in turn will allow an accurate appliance, restoration, prosthesis or analysis to be made.
The types of model that will be discussed are:
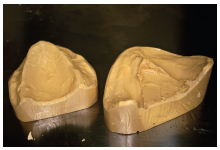
- Models for prosthodontics (Figure 1.6.1)
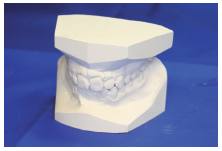
- Orthodontic study models (Figure 1.6.2)
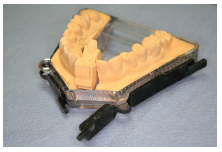
- Sectional models for indirect restorations (Figure 1.6.3).
Materials considerations
Dental models are almost always made from a plaster-based material. Before using these materials, it is important to have an understanding of their composition and handling characteristics.
Plaster of Paris
This is a type of building material based on calcium sulphate hemihydrate, and is often referred to as the ‘beta form’. It is created by heating gypsum (the raw mineral) to about 150°C, which drives off the water to make the powder that is used in the dental laboratory. This powder is then mixed with water (typically 50 ml of water to 100g of powder) to make a thick creamy mix suitable for dental applications.
Plaster of Paris is recognised in the dental laboratory as a white powder (other dental model materials are often coloured to differentiate them from it). The working time is about three to four minutes, and the initial set occurs after about ten minutes. There is a slight expansion on setting in the order of 0.2–0.3%. The setting reaction is exothermic, so plaster of Paris models feel warm to the touch as they set. A rule of thumb to gauge if a model has set sufficiently to be handled is to check that it is cool to the touch (indicating the setting reaction has completed).
Kaffir D
A more expensive gypsum: based, model: making material (and referred to as the ‘alpha-form’), Kaffir D has been heated in an autoclave (a sealed pressurised container) at around 130°C. The outcome is that more water is driven off and the powder produced is more regular in shape, finer and less porous. Less water is required to produce a mix suitable for dental model making (typically 20 ml of water to 100g of powder), and the product is a significantly harder and stronger material.
Kaffir D is recognised in the dental laboratory by its yellow colour. The working time and setting time is usually slightly longer than normal plaster, but the expansion on setting is less at around 0.08–0.1%.
If it is used in equal parts with plaster of Paris, (referred to as a 50:50 mix), Kaffir D can be used for making edentulous models. A 50:50 mix results in a softer, weaker material than Kaffir D on its own, but harder and stronger than plaster of Paris. When making dentate models, a higher strength is required and Kaffir D should be used on its own.
Class IV die stone
This is the strongest, hardest and most accurate gypsum-based model material used in the laboratory. Sometimes called artificial stone, die stone, densite, improved stone or ‘alpha-modified’, it is formed by boiling gypsum in a 30% aqueous solution of calcium chloride and magnesium chloride. This process produces the smoothest, most compact particles of the three types described here.
A mix suitable for dental model making is typically 20ml of water to 100g of powder (although you should check the manufacturer’s instructions), and the product is a significantly harder and stronger material. Care should be taken when mixing the se materials to ensure that the optimum strength and accuracy is achieved. This is the only one of the three materials described here that is regularly mechanically mixed under vacuum.
Manufacturers often colour Class IV die stone (many different colours are used) to help distinguish it from plaster of Paris and Kaffir D. The working time and setting time is the longest of the three materials described here, with a working time of about five minutes, and a setting time of 20 minutes. The expansion on setting is around 0.05–0.07%.
Class IV die stone materials are used whenever a very strong and abrasion-resistant model is required or where the model may need to be sectioned, such as most crown and bridge work and constructing some cast metal partial denture frameworks.
Notes on mixing
With each of the materials above, changes in the powder to water ratio will affect the working and setting times, material strength and hardness, and setting expansion.
As a rule of thumb, by using more water the setting time is extended, but the strength of the set material is reduced. Increasing the mixing time will reduce the setting time, but will tend to increase the setting expansion.
Additives, such as sodium chloride (table salt) and other ‘setting solutions’ act to significantly increase the setting time of a plaster mix, and can be useful when a fast set is required (such as for plaster impressions and articulating models).
1.7 Models for prosthodontics – casting primary impressions
Primary impression taking
Primary impression casting
Customised tray construction
Accurate impression taking and model making are essential to the successful production of a prosthetic device. If either procedure is carried out poorly, the appliance constructed on the model will not accurately fit the patient’s mouth.
Primary impressions are taken in ‘stock trays’, which are ready-made trays. These are available in a range of sizes, however, they rarely fit the patient’s mouth perfectly.
The poor fit results in inaccuracies that are discussed further in the Extended information section below. To overcome these inaccuracies, a ‘customised tray’ is constructed (see Chapter 2), which is tailor-made for the patient on the primary model.
- Gloves
- Plaster of Paris/dental stone (Kaffir D)
- Plaster bowl, spatula and knife
- Weighing scales
- Measuring cylinder
- Vibrating table
- Model trimmer
- Indelible pencil
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


