Chapter 1
Aging: Implications for the Oral Cavity
Bei Wu
School of Nursing and Global Health Institute, Duke University, Durham, NC, USA
Aging of the US population
The US aging population is increasing. The US older population, that is individuals aged 65 and older, reached 40.3 million in 2010. This is an increase of 5.3 million compared to the 2000 census. The percentage of the US population aged 65 and older also increased from 2000 to 2010. In 2010, the older population represented 13.0% of the total population, an increase from 12.4% in 2000 (Vincent & Velkoff, 2010). In the USA, by 2030 it is projected that there will be about 72.1 million older people, more than twice their number in 2000. Individuals aged 65 and older are expected to grow to become 19% of the US population by 2030 (Administration on Aging, 2012). By 2050, it is projected that there will be about 88.5 million older adults, 20.2% of the US population (US Census Bureau, 2008a).
Ethnic diversity
The US population is becoming increasingly diverse, and this is true for the aging population too. In the USA, among those aged 65 and older in 2050, 77% of the elder population are projected to be White-alone, down from 87% in 2010. Within the same age group, 12% are projected to be Black-alone and 9% are projected to be Asian-alone in 2050, up from 9% and 3%, respectively, in 2010. The Hispanic proportion of the older population is projected to quickly increase over the next four decades. By 2050, 20% of the US population aged 65 and over are projected to be Hispanic, up from 7% in 2010. The smallest race groups are projected to see the largest growth relative to their populations. Among the population aged 65 and older, it is projected that in 2050, the American Indian and Alaska Native-alone population will be 918 000, up from 235 000 in 2010, and the Native Hawaiian and Other Pacific Islander-alone population will be 219 000, up from 39 000 in 2010 (Vincent & Velkoff, 2010). There is also a trend of increasing number of old-old (age 75 and older) and oldest-old (age 85 and older) populations in the USA. The old-old and oldest-old carry much of the chronic disease burden in the population.
In the USA, among those aged 65 and older in 2050, the White-alone population will comprise approximately 77% of the aging population, whereas in 2010 the racial composition of the elder population was 87% White-alone, 9% Black, 3% Asian-alone, 7% as Hispanics, and 0.6% American Indian and Alaska Native. Between 2010 and 2030, the percentage of minority elders will increase much faster than the White population. The White population aged 65 and older is projected to increase by 59% compared with an average increase of 160% for older minorities, including Hispanics (202%), African Americans (114%), American Indians, Eskimos and Aleuts (145%), and Asians and Pacific Islanders (145%) (Administration on Aging, 2012).
While an increasing number of studies have examined oral health disparities across race/ethnicity in the USA, a limited number of such studies have been conducted for older adults. Policy makers, public health officials, and other healthcare providers need to better understand how social factors, along with medical conditions, may contribute to racial/ethnic disparities in oral health with the demographic transitioning to a more diverse older population in the USA (US Census Bureau, 2008b).
A report from the Surgeon General (US Department of Health and Human Services, 2000) noted ongoing racial/ethnic disparities in oral health across all ages, and it stressed the need for research to explain these differences. The first step towards explaining the disparities is to know how oral health differs between the groups.
Trends in oral health in older adults
There is substantial evidence that oral health in the USA has significantly improved in the past four decades. Dye et al., using data from the National Health and Nutrition Examination Survey (NHANES, III, 1988–1994) and NHANES 1999–2004, found that the oral health of the USA has substantially improved during this period (Dye et al., 2007). Specifically, Dye et al. show that the rates of periodontal disease and caries have decreased for most age groups.
Edentulism, or complete tooth loss, is one of the most important indicators of oral health. Edentulism reflects both the accumulated burden of oral diseases and conditions and the result of dental extraction treatment (Sanders et al., 2004). Studies suggest that edentulism significantly affects quality of life, self-esteem, and nutritional status (Nowjack-Raymer & Sheiham, 2003; Slade & Spencer, 1994; Starr & Hall, 2010). In economically developed countries, the trend of edentulism has declined consistently. For example, in England and Wales, the prevalence of edentulism for the adult population declined from 37% in 1968 to 12% in 1998 (Kelly et al., 2000). In Australia, the prevalence of edentulism for the adult population declined from 20.5% in 1979 to 8.0% in 2002. Among Australian older adults aged 65 and older, the reduction for males was from 59.7% to 26.5%, and for females was from 71.5% to 40.3% (Sanders et al., 2004). Similarly in the USA, the few studies available on middle-aged and older adults have shown that edentulism in these age groups has been dropping for the past several decades. One study revealed that within the period of 1971 and 2001, for those in a low socioeconomic position (SEP), the prevalence of edentulism declined from 50% to 32% in adults aged 55–64 and from 58% to 43% in adults aged 65–74; the comparable declines for these age groups for individuals in a high SEP were from 22% to 6% and from 30% to 9%, respectively (Cunha-Cruz et al., 2007). A report conducted by the US National Centers for Health Statistics using the US National Health and Nutrition Surveys of 1988–1994 (NHANES III) and NHANES 1999–2004 found that the prevalence of edentulism declined in the USA over these two time periods from 34% to 27% among adults aged 65 and older (Dye et al., 2007).
In the USA, minority elders have been identified as a key demographic group at greatest risk for edentulism (US Department of Health and Human Services, 2000). Black elders, in particular, have higher rates of edentulism than non-Hispanic Whites and Mexican Americans (Dye et al., 2007; Schoenborn & Heyman, 2009; Wu et al., 2011a). One study reported that the rates of edentulism among Blacks were declining, even though they were still higher than other ethnic groups (Dye et al., 2007). This study reported that the rates of edentulism for Black elders declined from 38% in 1988–1994 to 33% in 1999–2004 (Dye et al., 2007). For Whites, the percentages were much lower: 34% in 1988–1994 and 26% in 1999–2004. By comparison, Mexican American adults had even lower edentulism rates (27% and 24%, respectively).
Information regarding edentulism for Asian Americans and Native Americans is very limited. A recent report determined that 21% of Asian Americans aged 65 and older had lost all of their teeth compared to 25% of Whites. Asian Americans also had the lowest percentage of edentulism compared to other minority groups (Schoenborn & Heyman, 2009). The Third Oral Health Survey conducted by the Indian Health Service in 1999 found that 21% of Native American adults aged 55 and older were edentulous, representing a decrease of 5% over 15 years (Indian Health Services, 2001).
One recent study examined the trend of edentulism among adults aged 50 and older in five ethnic groups: Asians, Blacks, Hispanics, Native Americans, and non-Hispanic Whites (Wu et al., 2012a). This study used the National Health Interview Survey (NHIS), which is a cross-sectional household interview survey conducted annually. Ten waves of NHIS data were aggregated from 1999 to 2008. Eligible respondents were those aged 50 and older who completed the question on tooth loss. The sample included 616 Native Americans, 2666 Asians, 15 295 Blacks, 13 068 Hispanics, and 86 755 non-Hispanic Whites. Self-reported responses to a question about whether the individual had lost all upper and lower natural teeth were used to determine edentulism. Results show that for the past 10 years, there was an overall declining trend of edentulism for all racial and ethnic groups, except for Native Americans (Table 1.1). Table 1.1 presents the predicted rate of edentuliusm adjusting for time, sociodemographic characteristics and level of education. In 2008, Native Americans had the highest rate of edentulism (23.98%), followed by Blacks (19.39%), Whites (16.90%), Asians (14.22%), and Hispanics (14.18%). Figure 1.1 presents the trend of predicted rate of edentulism adjusting for time, sociodemographic characteristics and level of education.
Table 1.1 Trend of edentulism by racial/ethnic groups (1999–2008) (%) (weighted)a
| Year | White | Black | Hispanic | Asian American | Native American |
| 1999 | 21.49 | 24.62 | 17.78 | 17.04 | 33.20 |
| 2000 | 21.18 | 23.74 | 17.60 | 13.54 | 34.02 |
| 2001 | 20.20 | 23.02 | 17.71 | 11.88 | 31.78 |
| 2002 | 19.77 | 22.42 | 16.68 | 13.55 | 29.72 |
| 2003 | 18.90 | 21.78 | 16.21 | 15.88 | 29.67 |
| 2004 | 18.80 | 20.60 | 15.44 | 14.09 | 28.12 |
| 2005 | 17.98 | 20.65 | 15.13 | 13.57 | 24.72 |
| 2006 | 17.58 | 20.62 | 15.20 | 15.26 | 30.18 |
| 2007 | 17.05 | 19.58 | 14.74 | 14.08 | 27.07 |
| 2008 | 16.90 | 19.39 | 14.18 | 14.22 | 23.98 |
aThe predicted rates of edentulism were calculated adjusting for time, race/ethnicity, sociodemographic characteristics, and level of education.
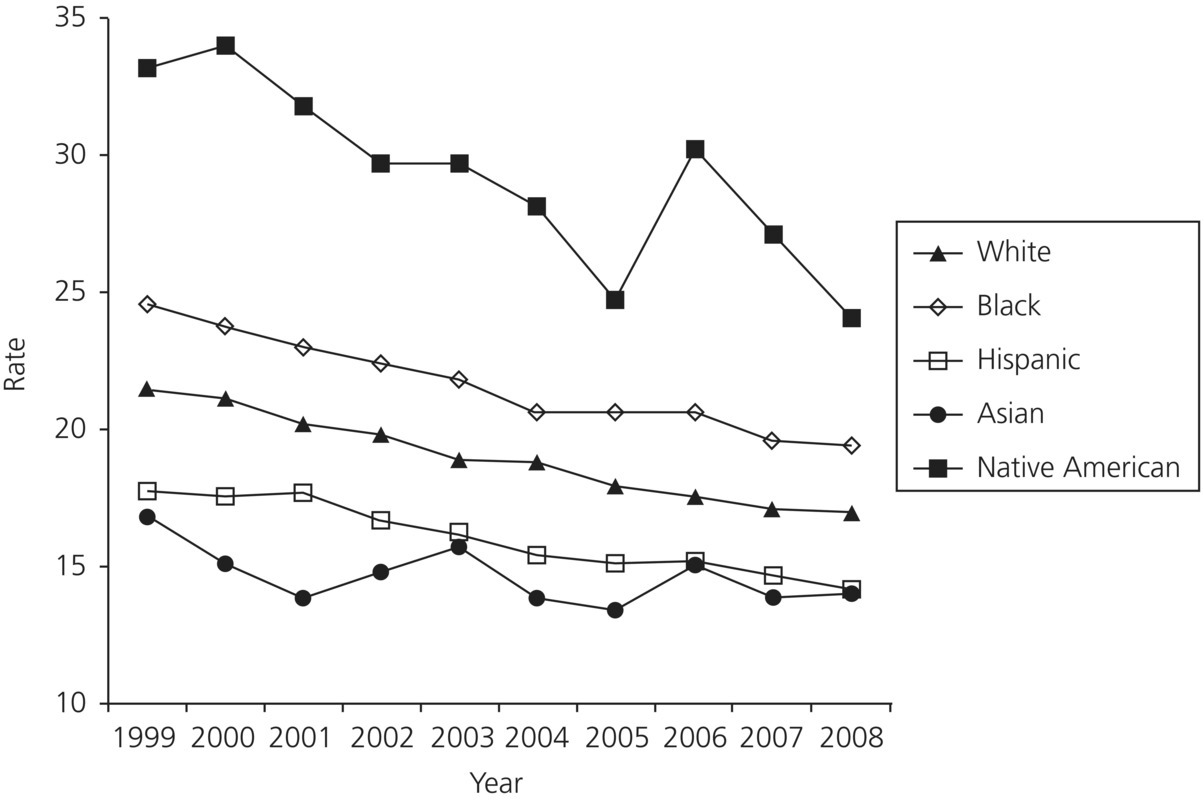
Figure 1.1 Predicted rate of edentulism.
From Wu et al. (2012a).
This is the first study to provide national estimates for the rate of edentulism and associated trends over time for five major ethnic groups in the USA simultaneously: Native Americans, Asian Americans, Blacks, Hispanics, and non-Hispanic Whites. Significant disparities in edentulism exist across these ethnic groups. Relative to Whites, Blacks and Native Americans had a higher rate of edentulism, whereas the rate of edentulism was lower among Hispanics and Asians. After controlling for covariates (e.g., sociodemographic characteristics, smoking, and common chronic conditions), Blacks and Hispanics were less likely to be edentulous than White respondents, while Native Americans were still more likely to be edentulous. In contrast, when covariates were included in the models, no significant differences were found between Asian Americans and Whites in edentulous rates. Overall, there was a significant downward trend in edentulism rates between 1999 and 2008; however, oral health disparities, as measured by rates of edentulism, increased among Native Americans over time compared to Whites.
The improvement in tooth retention was not equally distributed across the five racial and ethnic groups examined in this study. Native Americans, in particular, were at a significant disadvantage. Compared to Whites, Native Americans were more likely to lose natural teeth over time, but the risk became smaller after controlling for individuals’ socioeconomic status, health behaviors, and medical conditions. This study found that edentulism has continued to decline across the USA during the past decade. This comprehensive study supports previous reports about edentulism among adult populations collected in earlier time periods and across selected racial/ethnic groups (Dye et al., 2007; Indian Health Services, 2001; Schoenborn & Heyman, 2009).
One study found that current smoking and fewer years of education were two of the covariates most strongly associated with being edentulous (Wu et al., 2012a). Others have attributed the declining edentulous rate to the decrease in smoking and the increasing years of education among more recent cohorts (Cunha-Cruz et al., 2007). The authors also found that selected medical conditions were associated with edentulism; these were generally consistent with previous research (Holm-Pedersen et al., 2008). Self-reported memory problems and needing assistance with routine activities were also associated with increased risk of edentulism. Given the fact that the information on covariates was not collected prospectively, the authors cannot determine whether the factor preceded the edentulism. Many other factors could also contribute to the decrease of the edentulous rate, such as the introduction of fluoridation through community water treatment (Adair et al., 2001) and fluoridated toothpaste and mouth rinse (Featherstone, 1999; Marthaler, 2004). Health practices such as dietary supplements, and professionally applied or prescribed fluoride gel, foam, and varnish may also contribute to improved tooth retention (Adair et al., 2001; Marthaler, 2004; Weyant, 2004). Others point to advancements in dental technologies and treatment modalities, changes in patient and provider attitudes and treatment preferences (Starr & Hall, 2010), improved oral hygiene, and regular use of dental services (Eklund, 1999; Starr & Hall, 2010; Truman et al., 2002).
Oral health disparities in older adults
Some studies have reported that older Hispanic and Black Americans have more missing teeth, and decayed teeth than their White counterparts (Kiyak et al., 2002; Quandt et al., 2009; Randolph et al., 2001; Watson & Brown, 1995). Using the US National Health and Nutrition Examination Survey (NHANES 1999–2004), a Centers for Disease Control and Prevention (CDC) report found that both Blacks and Mexican Americans have a higher prevalence of untreated tooth decay and missing teeth than Whites (Dye et al., 2007). However, Mexican American adults were least likely to have lost all teeth compared to Whites and African Americans (Dye et al., 2007). In fact, a few studies have suggested that older Black adults have even worse oral health than Hispanics (Borrell et al., 2004; Craig et al., 2001; Kiyak et al., 2002). Many of the previous studies used small convenience samples or only individuals with low socioeconomic status; some were not able to compare the three racial/ethnic groups in the same sample, and some did not evaluate potential confounders that may help to explain differences among the racial/ethnic groups.
In order to address many of the methodologic issues noted earlier in this chapter, one study compared racial/ethnic differences in oral health among community dwelling non-Hispanic White, non-Hispanic Black, and Mexican American older adults aged 60 and older using NHANES (1999–2004) (Wu et al., 2011a). The descriptive results of the study showed that in comparison with Whites and Mexican Americans, Blacks had a significantly higher number of missing teeth, with an average of 3.5 more than whites (12.7 missing teeth) (P < 0.05) and 4.3 more than Mexican Americans (12.0 missing teeth) (P < 0.01). Blacks also had significantly higher rates of edentulism (28.6%) than both Whites (24.5%) and Mexican Americans (18.1%). However, Mexican Americans had the lowest rate of edentulism (18.06%) among the three groups but the highest number of decayed teeth by comparison. Additionally, minorities had many fewer filled teeth than Whites, particularly Blacks who had 2.7 filled teeth compared with 7.3 for Whites and 4.7 for Mexican Americans. (Fig. 1.1)
The findings from this multivariate analysis (Wu et al., 2011a) also showed that Blacks and Mexican Americans had significantly higher numbers of decayed teeth but fewer numbers of filled teeth than Whites, even controlling for many confounding variables. The results also found that Blacks were more likely to have a higher number of missing teeth than Whites; nonetheless, they were less likely to be edentulous. Compared with Whites, Mexican Americans were less likely to be edentulous, and dentate respondents were also less likely to lose their natural teeth. Further, the study reported that racial/ethnic differences were confounded by other health-related and social factors that often differ by race/ethnicity. Overall, oral health disparities across racial/ethnic groups persisted even after controlling for other covariates.
In this study (Wu et al., 2011a), racial/ethnic differences remained even after controlling for all other covariates. The findings reflect a historic lack of access to dental care for racial/ethnic minorities (Davidson & Andersen, 1997; Manski & Magder, 1998). Minority elders often demonstrate a low use of dental services, particularly preventative services. Racial/ethnic disparities in dental care could be partially explained by differential treatment as a result of limited dental coverage and inadequate participation of dentists in the Medicaid program (Doty & Weech-Maldonado, 2003).
Oral health is associated with individual’s socioeconomic status (Borrell et al., 2004). This association is often explained by the fact that individuals with higher income and a higher level of education are more likely than others to seek preventive dental care, have healthy behaviors, or to have access to dental services when they are needed. Another study confirmed the finding that individuals with higher level of education and income and education had better oral health outcomes, even controlling for the factors on health behaviors and preventive dental care (Wu et al., 2011a). The authors suspect that the results may arise from unmeasured differences in the quality of dental care currently received. Another possibility is that the cross-sectional data do not capture the cumulative effects of access to dental care throughout the life course (Wu et al., 2011a).
The observed disparities may also reflect current or lifetime dietary habits, and current or lifetime smoking habits and other negative health behaviors among minorities. Additionally, the results presented in this study could reflect unmeasured racial/ethnic differences in oral health beliefs and oral hygiene practice, and a lack of dental knowledge. Other researchers have suggested that clinicians should be aware that minorities may be less likely than Whites to believe in the benefits of preventative practices (Nakazono et al., 1997).
Using the same NHANES data (1999–2004), one study also examined racial/ethnic differences in self-reported oral health (Wu et al., 2011b). This study found that Blacks and Hispanics reported poorer self-rated oral health than Whites. In separate dentate and edentulous groups, socioeconomic status, social support, physical health, clinical oral health outcomes, and dental checkups accounted for much of the difference in self-rated oral health in Blacks, but significant differences remained for Hispanics. In addition to some potential reasons discussed earlier, other cultural factors could also contribute to the differences in self-rated oral health. Perception of health is socially constructed (Kaplan & Baron-Epel, 2003). Health beliefs and perceptions are rooted in social and cultural contexts and are influenced by prevailing social and medical ideologies. Responses to the self-rated oral health question may be the product of multiple present and past experiences. Factors such as differences in cultural perception and interpretation of overall health, and perceived needs of dental care, could contribute to the differences in self-rated oral health.
These cited studies suggest that reducing racial/ethnic oral health disparities requires multiple clinical approaches. First, it is important to improve access for dental care for minority elders. Second, it is critical to increase older adults’ knowledge of the importance of oral health, including the linkage between oral health, referred to as “dental literacy”, and systemic medical conditions, oral hygiene, and preventive dental care services. Third, programs are needed to improve individuals’ overall health behaviors – perhaps through encouraging positive behaviors that can help older Americans retain their natural teeth and maintain good oral health later in life. Fourth, develop and improve culturally competent services for minority communities by recruiting more underrepresented minorities to the dental professions, and enrich dental education curriculum (Lopez, N. et al., 2003; Wu et al., 2011a).
Functional status and oral health
The aging population is at increased risk for physical disability. Among people aged 65 and older, 18.1 million people (51.8%) had a disability, defined as having at least one disability of Activities of Daily Living (ADL) or Instrumental Activities of Daily Living (IADL). About 12.9 million people aged 65 and older (36.9%) had a severe disability. The prevalence of disability increases as people get older. For those aged 65 and those aged 69, 37.4% had disability and 7% need personal assistance with ADL or IADL. For individuals aged 80 and older, the percentage increases to 71% and 29.2%, respectively (Brault, 2008). Disability leads to reduced quality of life for individuals and increased costs to society in the provision of services. It is likely that disabled older adults are at higher risk of oral diseases. One reason is that disability may affect individual’s ability to maintain good oral hygiene and restrict their access to n/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


