Chapter 2
Local anesthesia for the pediatric patient
Jane A. Soxman and Stanley F. Malamed
The number one reason children give for fear of going to the dentist is the fear of injection (AlShareed, 2011). Parents/guardians should be told not to discuss the injection before an appointment for restoration or extraction with the child. With the use of topical anesthetic, distraction, and good injection technique, most children are unaware of receiving the injection. Anxiety is the biggest predictor of poor pain control (Nakai et al., 2000). Before beginning any procedure, note red splotches, rash, or evidence of trauma to rule out allergic reaction to the local anesthetic or responsibility of the practice for an injury that previously occurred. Any unusual finding is immediately shown to the parent/guardian and documented in the chart. Anxiety may cause a diffuse rash (Figure 2.1). An allergic reaction to medication being taken may also present as a rash (Figure 2.2).
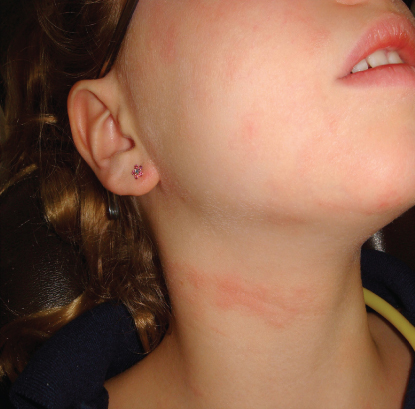
Figure 2.1 Diffuse rash due to anxiety.
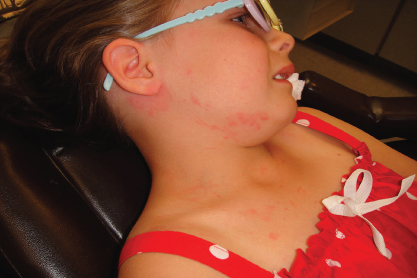
Figure 2.2 Rash due to suspected allergic reaction to penicillin.
The local anesthetic may be described as to “sleepy juice.” The child is told that his/her tooth will go to sleep for a little while but will “awaken” later, just as the child awakens each morning. The dentist or a staff member should monitor the child after the injection, while awaiting effective anesthesia. The rubber dam is referred to as a blanket to cover the sleeping tooth. After the rubber dam is removed, the child is told that the tooth, lip, and/or tongue will soon awaken. A time frame described in hours for a return to normal sensation, when the tooth will feel exactly the same as before taking the nap, is meaningless to a child. A concrete time, such as lunchtime or dinnertime, may be better word choices for the child to understand.
Infiltration in the mandible results in lip anesthesia, which can be distressing and compounds the anesthetic sensation. If possible, begin with buccal infiltration in the maxilla for a primary molar to desensitize the child. This approach will help him/her to become accustomed to the sensation created by the local anesthesia before introducing more profound mandibular anesthesia, including the lower lip and/or tongue. Parents/guardians are informed before administering the local anesthetic that the feeling of being numb after the procedure is completed is often more distressing for the child than the injection or procedure. This exaggerated response is usually seen immediately after the rubber dam is removed (Figure 2.3). The young child complains, “it hurts.” A sticker, reminding the child not to bite or suck on his/her lip/cheek or tongue, should be placed on the child’s shirt on the same side as the anesthetized lip and/or tongue. Hot beverages should be avoided. These instructions are given with the parent/guardian present. A photograph of the appearance of a lip after chewing or biting during anesthesia can be shown to the parent/guardian and, if old enough to understand, also the child (Figure 2.4). If damage to the lip or oral mucosa occurs, Vitamin E applied to the area may soothe and hasten healing. The patient’s chart should include the dosage of local anesthetic administered in milligrams, the site of injection, and the type of injection(s) such as infiltration, intraosseous, or block, along with needle gauge and length (extra short or short). The patient’s reaction to the injection and post-injection instructions given to the parent/guardian and patient should also be included in the chart (American Academy of Pediatric Dentistry, 2014).

Figure 2.3 Child immediately after procedure distressed by the numb sensation.
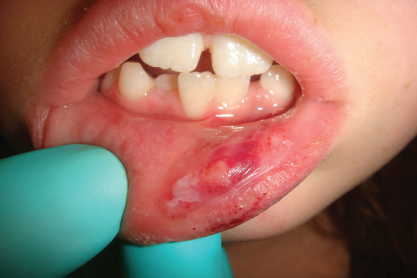
Figure 2.4 Lip swelling and ecchymosis due to lip chewing.
Local anesthetic choice
Bupivacaine, prilocaine, articaine, lidocaine, and mepivacaine are injectable amide local anesthetics approved for pediatric use. Bupivacaine is not recommended for a young child or for some special needs patients with mental or physical disabilities because of prolonged anesthesia with risks of self-inflicted soft tissue injury. One of prilocaine’s end products causes the formation of methemoglobin, which decreases the ability of hemoglobin to carry oxygen (American Academy of Pediatric Dentistry, 2014). Prilocaine should be used cautiously or avoided in children with oxygen transport diseases such as sickle cell disorder, anemia, respiratory disease, cardiovascular disease, or abnormal hemoglobin. Gutenberg et al. found that administration of 4% prilocaine without a vasoconstrictor with a dose of 5 mg/kg resulted in significantly elevated levels of methemoglobin. Because peak methemoglobin blood levels are reached 1 h after injection, children should be observed for at least 1 h after a procedure using 4% prilocaine as the local anesthetic. Gutenberg et al. (2013) did not find increased methemoglobin levels using 2% lidocaine with 1 : 100,000 epinephrine. Two percent lidocaine with 1 : 100,000 epinephrine is most often used for pediatric patients, but 4% articaine has gained some popularity. Prolonged numbness with 4% solutions may be distressing to children younger than 7 years, with 40% reporting numbness after 3 h and 11% after 5 h. Soft tissue injury, particularly of the lip, is more likely to occur (Adewumi et al., 2008). The use of 1 : 200,000 epinephrine instead of the 1 : 100,000 concentration with the 4% articaine should not change the efficacy and may be preferable for the pediatric patient. A study by Meechan did not find effectiveness of buccal infiltration in the mandibular first molar area to be influenced by the concentration of the epinephrine solution (Meechan, 2011). The efficacy of articaine 4% has been reported to be more effective in obtaining good anesthesia in infected sites and so may be a good local anesthetic choice for extraction due to abscess (Kurtzman, 2014). The low pH of the epinephrine in both articaine and lidocaine may cause a burning sensation. Three percent mepivacaine, pH 4.5–6.8, does not contain epinephrine and may reduce injection discomfort (Friedman, 2000). Because mepivacaine does not contain a vasoconstrictor, rapid systemic uptake can occur. The maximum dosage of 3% plain mepivacaine, 4.4 mg/kg or 2.0 mg/lb, should be carefully calculated (American Academy of Pediatric Dentistry, 2014). Three percent mepivacaine may offer a good alternative for single quadrant occlusal or interproximal restorations in the primary dentition with the shorter duration of those procedures and soft tissue anesthesia.
Dosage
Local anesthetic overdoses were found in 41% of malpractice insurance claims involving anesthesia for pediatric dental patients. Of those claims, 43% occurred when local anesthetic was the only drug administered (Chicka et al., 2012). The cortical plate of bone is thin, and the bone is more vascular with rapid uptake of local anesthesia in the pediatric patient. The use of a vasoconstrictor, epinephrine, reduces the risk of rapid systemic absorption and overdose. A vasopressor-containing local anesthetic is recommended for use when more than one quadrant is being restored in the same visit (American Academy of Pediatric Dentistry, 2014).
Dosage is based on a child’s weight and should never exceed the listed maximum dosage. The maximum dosage of 4% articaine with 1 : 100,000 epinephrine recommended is 7.0 mg/kg or 3.2 mg/lb (Webb et al., 2012; Widmer et al
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


