Chapter 20
Behavior guidance
Jane A. Soxman
The various forms of behavior that present when treating the pediatric patient can be daunting. Describing the child’s behavior with terms such as fearful, strong avoidance, combative, stubborn, defiant, and hysterical is a method to more clearly define the type of behavior affecting our ability to safely and/or ideally perform treatment. Individual temperament, the characteristic physiological and emotional state of an individual, which tends to condition responses to the various situations of life, significantly influences our ability or inability to modify behavior with basic techniques. Salem et al. (2012) found that dental fear and anxiety were more influenced by temperament than parental influence. Techniques using tell–show–do, desensitization, modeling, and distraction prove to be successful, especially for a child who is purely fearful or mildly apprehensive. Parents/guardians should be informed regarding limitations imposed by a child’s behavior on our ability to provide quality care. Societal and parental influences are increasingly influential in our ability to guide behavior (Juntgen et al., 2013). Diverse ethnic communities and various cultural influences increasingly impact our behavior guidance and the compliance of parents/guardians (Goleman, 2014).
Age-appropriate expectations
An age-appropriate approach insures that expectations of the dentist, staff, and parent/guardian are realistic regarding the child’s ability to cooperate.
Toddlers are developing a sense of independence, but a strong attachment to the parent is appropriately present until the age of 2 years. Once a high level of distress is reached, calming the toddler is difficult. If the child is crying or exhibiting avoidance behavior, examine the child as quickly as possible to determine the existence of caries or pathology. The knee-to-knee examination for an infant provides safe, adequate immobilization for the examination (Figure 20.1). Apprehensive 2- or 3-year-old children may sit on the parent/guardian’s lap for examination or a preventive care visit. A neck pillow may be offered for neck support for the parent/guardian (Figure 20.2). With combative or strong avoidance behavior, the child sits on the lap of the parent/guardian, and the parent/guardian holds the child’s hands and places one of his or her legs over the child’s legs (Figure 20.3). To avoid startling a child, place your hand on his or her shoulder before reclining the chair, while telling him or her that the chair is going to move backward (Figure 20.4). Tell–show–do, to explain what to expect, is a good tool for guidance at any age, but may begin with the toddler. The procedure is described in as few words as possible, the materials to be used are shown to the child, and the procedure begins (Figures 20.5a, 20.5b, and 20.5c). Start with the maxillary incisors, desensitizing the child, before examining or performing prophylaxis on the molars.
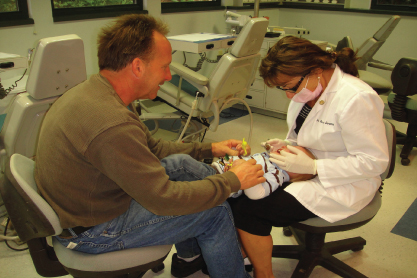
Figure 20.1 Knee-to-knee examination.
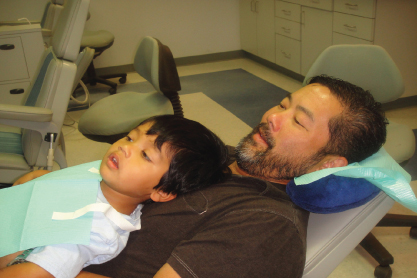
Figure 20.2 Child on parent’s lap for examination.
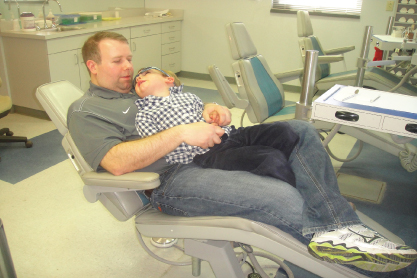
Figure 20.3 Parent stabilizing the child.
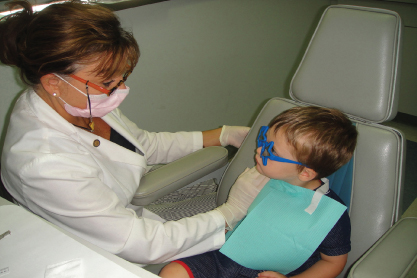
Figure 20.4 Placing hand on child’s shoulder before reclining chair.
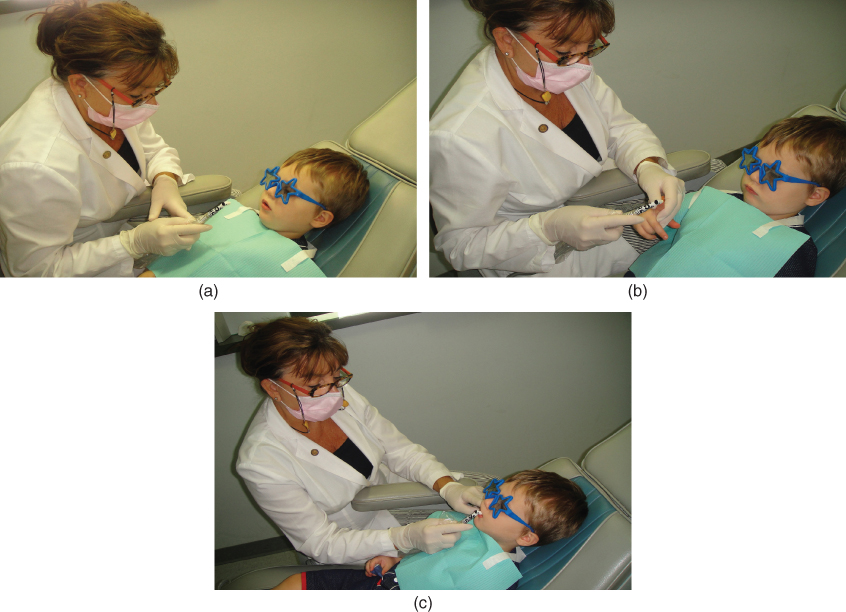
Figure 20.5 (a) Telling about the procedure. (b) Showing the procedure. (c) Doing the procedure.
Suggest ideas for preparing the preschooler for the first visit to the parent/guardian such as reading a story about going to the dentist, using a reclining chair at home to experience the sensation of the chair moving backward, and using a battery powered spin brush. Preschool-age children are in the midst of multiple inoculations; fear of a “shot” may be the predominant concern (Salem et al., 2012). Most preschool children are learning the ABC’s and to count. Most children can count to 10 by the age of 3 years. Saying the ABC’s or counting the teeth during the examination provides distraction and familiarity. Count the child’s fingers before placing the mirror in the child’s mouth. Introduce the mirror by touching the inside of his cheek while describing the softness of the mirror. Explain that because you are counting baby teeth, you must be gentle, just as you would be with a baby. Pretending is common play for the preschool child. Modeling is a term used to describe a fearful or apprehensive child watching a relaxed child of similar or younger age undergoing a procedure. Modeling is typically not beneficial until the age of 4 years. Unless modeling with siblings, the parents/guardians of both children should give consent for this method of guidance (Figure 20.6). A parent/guardian, who believes a procedure may be too difficult for his or her child to cooperate, may also observe another child of same or younger age undergoing treatment with a similar procedure. An emotionally healthy 4-year-old child may be able to separate from the parent after the first visit.
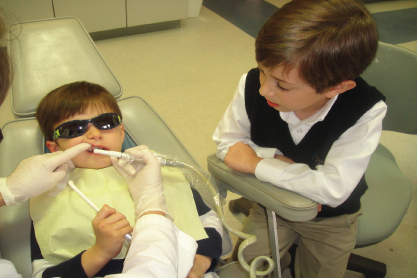
Figure 20.6 Modeling.
The school-age child should be able to sit still and focus. He or she now understands consequences. Competence is gaining value in his or her life, and so accomplishing treatment goals is important not only for the dentist, but also for the child. If fearful behavior prohibits completion of the planned procedure, make an effort to accomplish something so the child does not leave the office with a sense of failure. In the same manner, do not permit combative or avoidance behavior to postpone treatment, possibly guaranteeing the same behavior in a manipulative child at the next appointment. Placing sealants is a good procedure to use modeling for behavior guidance. Voice control is a form of behavior guidance that uses the tone of voice, loudness, or pace to gain cooperation or attention. Parents/guardians should be advised of this technique before use, as some may deem voice control unacceptable (American Academy of Pediatric Dentistry, 2014). School-age or older children would be preferable for this form of guidance.
Watching television or playing computer games before a dental visit may relax a child (Campbell et al., 2005). Sitting quietly beside a parent/guardian, who is reading a story before treatment, may be helpful for an apprehensive child. Systematic desensitization is also useful to reduce anxiety. An effort is made to begin treatment with a procedure that would evoke minimal fear and progress toward more fear-provoking stimuli (Widmer et al., 2008). Think about desensitizing when determining the sequence of a treatment plan, considering local anesthesia and the length of the procedures. Davidovich et al. determined that treatment duration was the main factor influencing behavior for younger and older children. Treatment time should not exceed 30 min (Davidovich et al., 2013).
Mouth props
The Parkell dry-field posterior mouth prop (Parkell, Inc.) is made of clear, autoclavable plastic providing a dry field, throat partition and retraction of the cheek and tongue (Figure 20.7a). An anterior version, to restore an incisor, is also available (Figure 20.7b). The Open Wide Disposable Mouth Rest (Specialized Care Company, Inc.) can be used with any age child who is unwilling to open his or her mouth or who is unable to reliably maintain an open mouth. This mouth prop is especially useful for children with special needs (Figure 20.7c). The rubber handle of a pediatric toothbrush may also be used (Figure 20.7
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


