CLASS III MALOCCLUSION
Definition
Angle first published his classification of malocclusion in 1899, which was based solely on the dental arch relationship using study cast. Class I occlusion occurred when the mesiobuccal cusp of upper first permanent molars occluded on the buccal groove of the lower first molar. Class III malocclusion occurred when the lower teeth occluded mesial to the width of one bicuspid, or even more in extreme cases.
The advent of cephalometric radiology in 1931 allowed clinicians to discern the underlying skeletal pattern of the Class III malocclusion. Tweed divided Class III malocclusions into (1) pseudo–Class III malocclusions with normally shaped mandibles and underdeveloped maxilla and (2) skeletal Class III malocclusions with large mandibles. Moyers divided Class III mesiocclusion into three distinct types: osseous, muscular, and dental. The first condition is an abnormal osseous growth pattern, the second an acquired muscular reflex pattern of mandibular closure, and the third a problem in dental positioning.
Prevalence
Class III malocclusion is a less frequently observed clinical problem than Class II or Class I malocclusion, occurring in less than 5% of the U.S. population. The prevalence is greater in Asian populations. The estimated incidence of Class III malocclusion among the Korean, Japanese, and Chinese is 4% to 14% because of the large percentage of patients with maxillary deficiency. However, a study on Chinese children age 9 to 15 years that divided subjects into those with “pseudo” and “true” Class III malocclusions found a much lower prevalence of these disorders, 2.3% and 1.7%, respectively.
In the African-American population the incidence of Class III malocclusion has been shown to be 6.3%. Class III malocclusions are more prevalent in Hispanic than in African or Caucasian groups. Prevalence of Class III malocclusion in Latino Americans has been shown to be about 9.1%, similar to the 8.3% in Mexican Americans reported by the NHANES survey.
As for the components of Class III malocclusion, a study of Class III surgical patients demonstrated that the combination of underdeveloped maxilla and overdeveloped mandible was most common at 30.1%, whereas those with a normal maxilla and overdeveloped mandible constituted 19.2% of the sample. Most Korean patients, however, had a normal maxilla and overdeveloped mandible (47.7%), with fewer patients having an underdeveloped maxilla and overdeveloped mandible (13.5%).
Etiology
Class III skeletal growth has a multifactorial basis that is influenced by genetics, function, deformities, size, and position of bones. According to Enlow, the facial bones that contribute to a Class III skeletal pattern may include the anterior and posterior cranial base, the nasomaxillary complex, and the ramus and corpus of the mandible. Only a few types of Class III malocclusion are caused by specific interferences with growth. These interferences may be caused by habits or related to growth patterns. Accordingly, individuals with postural habits of the mandible and mouth breathing may present with a Class III type of malocclusion. This investigation also demonstrated that interferences in occlusal function, such as reverse overjet, can alter the direction and shape of the mandible.
The more severe Class III cases are caused by a combination of inherited traits, which are made worse by environmental factors. According to Park and Baik, the etiology of Class III malocclusion can be classified into three types on the basis of the position of the maxilla relative to the craniofacial skeleton. Type A individuals have a normal maxilla and overgrown mandible, which is classified as true mandibular prognathism. Type B individuals have maxillary and mandibular excess, but the mandible has grown more than the maxilla; they present with an acute nasolabial angle and an anteriorly positioned A point. Type C individuals have hypoplasia of the maxilla; their facial profile is concave with an excessively large nasolabial angle, which is frequently camouflaged by dentoalveolar compensation.
Patients with Class III malocclusion may present with various combinations of other abnormal skeletal and dental patterns. The most common skeletal features include a shortened anterior cranial base, more obtuse gonial angle, anteriorly positioned glenoid fossa, decrease in cranial base flexure, sagittal discrepancy of the maxilla and/or mandible, and increase in anterior lower facial height. Dental findings usually include Angle Class III molars and canines, retroclined mandibular incisors, proclined maxillary incisors, and an edge-to-edge incisor relationship or negative overjet.
Differential Diagnosis
The differential diagnosis in skeletal Class III malocclusions plays a major role in the success of treatment results. The timing of orthodontic treatment has always been somewhat controversial, and the prognosis is always guarded until growth is completed. Variations in magnitude and expression of Class III malocclusion can present with some difficulty during diagnosis. As mentioned earlier, a patient may present with a combination of one or more dentofacial deformities, such as true mandibular prognathism or maxillary retrognathism. To differentiate the underlying cause of a Class III malocclusion, a simplified method of evaluating patients has been suggested.
First, it is important to question both the patient and the parents about the presence of a large jaw or anterior crossbite among family members. If a close relative required orthognathic surgery, the patient under examination may also exhibit a severe skeletal discrepancy.
Second, it is important to assess the presence of a functional shift. The relationship of maxilla to mandible should be evaluated to determine whether a discrepancy exists between centric relation and centric occlusion. Anterior repositioning of the mandible may be caused by abnormal tooth contact that forces the mandible forward. These patients tend to present with a Class I skeletal pattern, normal facial profile, and Class I molar relation in centric relation, but a Class III skeletal and dental pattern in centric occlusion. Early correction of this “pseudo” Class III condition may provide for a more favorable environment for future growth.
Third, a lateral cephalometric radiograph is required to complete the diagnosis and assist the clinician in treatment planning. A cephalometric analysis is needed to record quantitatively the severity of the Class III malocclusion and to determine the underlying cause of the deformity. Cephalometric measurements that relate the maxilla to the mandible (e.g., ANB, Wits, and linear measurements of difference between condylion to A point and condylion to gnathion) are particularly helpful in quantifying the severity of the malocclusion ( Table 13-1 ).
| Intermaxillary Cephalometric Variables | Standard (Age 6-18 years) |
|---|---|
| Wits analysis | 0 mm |
| Maxillary-mandibular difference | 23 mm (12 years old) |
| ANB angle | 2 degrees |
| Zero meridian | |
| Maxilla | +2.3 mm |
| Pogonion | 0 mm |
Discriminant analysis has shown that Wits appraisal is most decisive in distinguishing camouflage treatment from surgical treatment. The average Wits for camouflage treatment was −4.6 ± 1.7 mm and for surgical treatment was −12.1 ± 4.3 mm. Accordingly, on the basis of the Wits appraisal, the severity of skeletal Class III patients can been labeled as red, green, and yellow categories. Patients with a Wits appraisal greater than 12 mm are labeled “red” and may eventually require orthognathic surgery to correct the skeletal deformity. Patients with a Wits appraisal smaller than 4 mm are labeled “green” and most likely can be camouflaged by orthodontic tooth movement. Patients with a Wits appraisal between 4 and 12 mm are labeled “yellow” and require further analysis, such as serial radiographs and a growth treatment response vector (GTRV) analysis, before a decision can be made whether to camouflage the malocclusion or wait for completion of growth before surgical treatment is implemented.
Fourth, a thorough clinical assessment may be the most important evaluation for the diagnosis when the objective of treatment planning is to optimize facial esthetics. The anteroposterior skeletal base relationship and the vertical facial proportions should be assessed while the patient is sitting upright in natural head position. Any profile disharmonies should be recorded. Similarly, the transverse dimension should be assessed at this point along with any facial and dental asymmetries. The temporomandibular joints, associated musculature, and oral mucosa should also be examined.
The following discussion highlights diverse approaches for using maxillary protraction for the treatment of Class III malocclusions.
PROTRACTION OF MAXILLA
Patients with developing Class III malocclusion can be treated using chin cap, facemask, removable functional appliances, or fixed appliances. Protraction facemask has been used in the treatment of patients with Class III malocclusions and a maxillary deficiency. The facemask has an adjustable anterior wire that can accommodate a downward and forward pull on the maxilla with elastics. To minimize the tipping of the palatal plane, the protraction elastics are attached near the maxillary canines with a downward and forward pull of 30 degrees from the occlusal plane. Maxillary protraction usually requires 300 to 600 g of force per side, depending on the age of the patient. Patients are instructed to wear the appliance for 12 hours a day.
In the mixed dentition, a banded or bonded expansion appliance can be fabricated as anchorage for maxillary protraction. Patients with an increased lower face height can benefit from using a bonded expansion appliance, which provides a temporary bite-plane effect. Additionally, a bonded maxillary appliance can be used in patients with a deep overbite and overclosure of the mandible to facilitate the jumping of the anterior crossbite. The expansion appliance is activated twice daily (0.25 mm per turn) by the patient or parent for 7 to 10 days. In patients with a more constricted maxilla, activation of the appliance is carried out for 2 weeks or more.
Facial Sutures
Several facial sutures play an important role in the development of the nasomaxillary complex, including the frontomaxillary, nasomaxillary, zygomaticotemporal, zygomaticomaxillary, pterygopalatine, intermaxillary, ethmomaxillary, and lacrimomaxillary sutures ( Fig. 13-1 ).
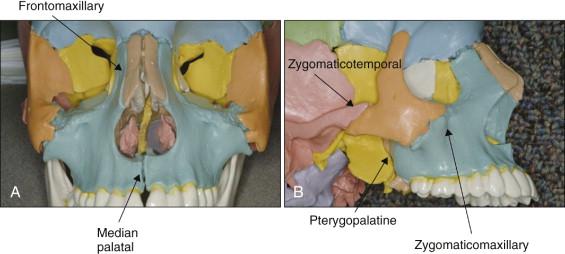
Animal studies have shown that the maxillary complex can be displaced anteriorly with significant changes in the facial sutures. Maxillary protraction, however, does not always result in forward movement of the maxilla. With the same line of force, different midfacial bones are displaced in different directions depending on the moments of force generated at the sutures. The center of resistance of the maxilla is located at the distal contacts of the maxillary first molars, one half the distance from the functional occlusal plane to the inferior border of the orbit. Protraction of the maxilla below the center of resistance produces counterclockwise rotation of the maxilla, which may not be favorable for patients with open-bite tendency.
Crossbite and Overjet/Overbite Correction
Clinically, anterior crossbite can be corrected with 3 to 4 months of maxillary expansion and protraction depending on the severity of the malocclusion. Improvement in overbite and molar relationship can be expected with an additional 4 to 6 months of treatment.
A prospective clinical trial found that overjet correction resulted from forward maxillary movement (31%), backward movement of the mandible (21%), labial movement of the maxillary incisors (28%), and lingual movement of the mandibular incisors (20%). Overcorrection of the overjet and molar relationship was highly recommended to anticipate unfavorable mandibular growth. Overbite was improved by eruption of the posterior teeth. The total facial height was increased by inferior movement of the maxilla and downward and backward rotation of the mandible.
According to several clinical studies, the mean forward movement of the maxilla with 6 to 8 months of maxillary protraction is about 1 to 3 mm. A meta-analysis on the effectiveness of protraction facemask treatment found that the average change in Wits appraisal was 4 to 6 mm and the average horizontal A-point movement was 1 to 3 mm.
Timing of Treatment
A critical question in maxillary protraction concerns the best time to start facemask treatment. The main objective of early facemask treatment is to enhance forward displacement of the maxilla by sutural growth. Histological studies have shown that the midpalatal suture is broad and smooth during the “infantile” stage (8-10 years of age) and becomes more squamous and overlapping in the “juvenile” stage (10-13 years). Biologically, the circum-maxillary sutures are smooth and broad before age 8 years and become more heavily interdigitated around puberty.
These findings relate to observations in clinical studies showing that maxillary protraction is effective in the primary, mixed, as well as early permanent dentitions. Several studies suggest that a greater degree of anterior maxillary displacement can be found when treatment is initiated in the primary or early mixed dentition.
The optimal time to intervene a Class III malocclusion is at the initial eruption of the maxillary incisors. A positive overjet/overbite at the end of the facemask treatment appears to maintain the anterior occlusion.
Another important question is whether the results of early protraction treatment can be sustained when subsequent mandibular growth occurs during the pubertal growth spurt. In a prospective clinical trial, protraction facemask treatment starting in the mixed dentition was stable 2 years after removal of the appliances. This probably resulted from the overcorrection and the use of a functional appliance as retainer for 1 year. When these patients were followed for another 2 years, 15 of the 20 patients maintained a positive overjet. In patients who relapsed to a negative overjet, the mandible outgrew the maxilla in the horizontal direction. When these patients were followed for another 4 years (8 years after treatment, until about 17.5 years of age), 14 of the 20 patients (67%) maintained a positive overjet. For the patients who relapsed to a reverse overjet, the mandible outgrew the maxilla by four times, compared with twice that in the stable group.
These results suggest that in a random clinical trial when patients are followed until after completion of pubertal growth, two of three patients (67%) will have a favorable outcome. About one third of the patients might be candidates for orthognathic surgery later in life because of unfavorable growth pattern. Patients treated by protraction facemask either in the early mixed dentition or in the late mixed dentition and permanent dentition and followed up after a second phase of fixed-appliance therapy demonstrated ongoing improvements in the former group but not in the latter group at the end of phase II treatment. Specifically, 1.8 mm of additional forward movement of the maxilla was noted in the early treatment group compared with the controls. In the late mixed-dentition group, no significant difference in forward movement of maxilla was found after puberty compared with the controls.
PROTRACTION OF MAXILLA
Patients with developing Class III malocclusion can be treated using chin cap, facemask, removable functional appliances, or fixed appliances. Protraction facemask has been used in the treatment of patients with Class III malocclusions and a maxillary deficiency. The facemask has an adjustable anterior wire that can accommodate a downward and forward pull on the maxilla with elastics. To minimize the tipping of the palatal plane, the protraction elastics are attached near the maxillary canines with a downward and forward pull of 30 degrees from the occlusal plane. Maxillary protraction usually requires 300 to 600 g of force per side, depending on the age of the patient. Patients are instructed to wear the appliance for 12 hours a day.
In the mixed dentition, a banded or bonded expansion appliance can be fabricated as anchorage for maxillary protraction. Patients with an increased lower face height can benefit from using a bonded expansion appliance, which provides a temporary bite-plane effect. Additionally, a bonded maxillary appliance can be used in patients with a deep overbite and overclosure of the mandible to facilitate the jumping of the anterior crossbite. The expansion appliance is activated twice daily (0.25 mm per turn) by the patient or parent for 7 to 10 days. In patients with a more constricted maxilla, activation of the appliance is carried out for 2 weeks or more.
Facial Sutures
Several facial sutures play an important role in the development of the nasomaxillary complex, including the frontomaxillary, nasomaxillary, zygomaticotemporal, zygomaticomaxillary, pterygopalatine, intermaxillary, ethmomaxillary, and lacrimomaxillary sutures ( Fig. 13-1 ).
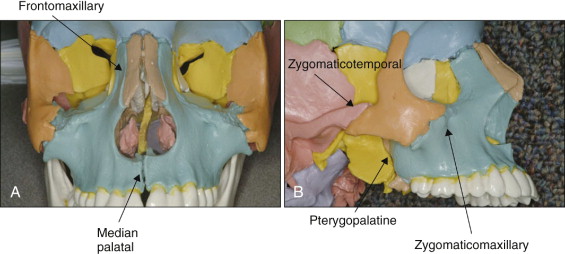
Animal studies have shown that the maxillary complex can be displaced anteriorly with significant changes in the facial sutures. Maxillary protraction, however, does not always result in forward movement of the maxilla. With the same line of force, different midfacial bones are displaced in different directions depending on the moments of force generated at the sutures. The center of resistance of the maxilla is located at the distal contacts of the maxillary first molars, one half the distance from the functional occlusal plane to the inferior border of the orbit. Protraction of the maxilla below the center of resistance produces counterclockwise rotation of the maxilla, which may not be favorable for patients with open-bite tendency.
Crossbite and Overjet/Overbite Correction
Clinically, anterior crossbite can be corrected with 3 to 4 months of maxillary expansion and protraction depending on the severity of the malocclusion. Improvement in overbite and molar relationship can be expected with an additional 4 to 6 months of treatment.
A prospective clinical trial found that overjet correction resulted from forward maxillary movement (31%), backward movement of the mandible (21%), labial movement of the maxillary incisors (28%), and lingual movement of the mandibular incisors (20%). Overcorrection of the overjet and molar relationship was highly recommended to anticipate unfavorable mandibular growth. Overbite was improved by eruption of the posterior teeth. The total facial height was increased by inferior movement of the maxilla and downward and backward rotation of the mandible.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


