Fig. 36.1
Velopharyngeal management algorithm 1
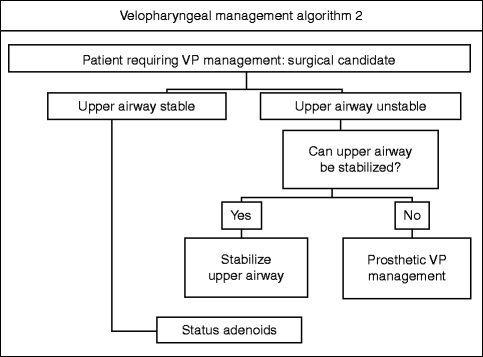
Fig. 36.2
Velopharyngeal management algorithm 2
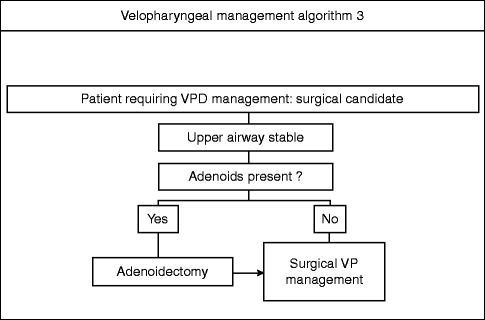
Fig. 36.3
Velopharyngeal management algorithm 3
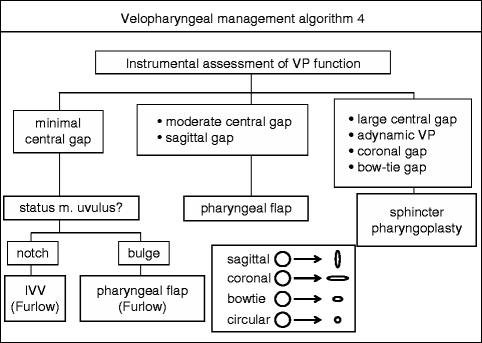
Fig. 36.4
Velopharyngeal management algorithm 4
Individuals with possible VPD present to individual members of the cleft palate team or to the team as a whole for diagnosis and treatment. Historically, the large majority of such individuals had a repaired cleft palate and a small minority, without overt cleft palate, developed VPD following adenoidectomy. While post-palatoplasty patients with impaired speech still comprise the largest group evaluated for VPD (Kummer 2007; Peterson-Falzone et al. 2010), individuals with velocardiofacial syndrome, neurological impairment, and postobstructive sleep apnea surgery (uvulopalatoplasty) comprise a steadily increasing percentage. Whereas identification of the etiology of the VPD is critical to assigning differential management based on differential diagnosis (Marsh 1991; Marsh and O’Daniel 1992), the evaluation of velopharyngeal function is the same regardless of etiology (Witt et al. 1999). I shall first discuss the evaluatory process and then specific managements.
36.1 Evaluation of Velopharyngeal Function
Speech results from modulation of the pressurized air stream that emerges from the lungs during expiration. A number of structures between, and including, the glottis and the lips (articulators) modify that air stream to produce specific sounds. One of those modifiers is the velopharynx, which normally is a dynamic sphincter. A sphincter is an anatomic structure that can open or close to varying degrees and speeds depending on the physiological necessity. The tissues that comprise the velopharyngeal sphincter are the velum (soft palate), the right and left lateral pharyngeal walls, and the posterior pharyngeal wall. The space enclosed by and modified by the velopharyngeal sphincter is the velopharynx. The velopharynx is the connection between the nasopharynx and the oropharynx. Normally at rest, it is a wide opening through which air flows easily and secretions drain; when contracted, it closes the nasopharynx from the oropharynx, preventing passage of gases, fluids, and solids between the two cavities. Dysfunction of the velopharyngeal sphincter impairs that separation of the nasal and oral cavities for both deglutition and speech to varying degrees. Outcome assessment of VPD management requires consideration of velopharyngeal function for all of the following physiological activities: speech, breathing, swallowing, handling nasal secretions, and sleep.
There is a lack of consensus on the preferred term to describe such dysfunction: velopharyngeal incompetency, velopharyngeal insufficiency, and velopharyngeal inadequacy have all been abbreviated as VPI. I prefer the term velopharyngeal dysfunction, abbreviated as VPD, since it connotes physiological impairment without attempting to denote etiology (Loney and Bloem 1987; Folkins 1988; Smith and Kuehn 2007). Regardless of the terminology, a specific set of physical findings suggest VPD. These include excessive nasal resonance during speech (hypernasality), inappropriate nasal airflow noise (nasal turbulence or rustling), and abnormal facial movements (facial grimacing). An individual with one or any combination of these findings will be referred for evaluation of possible VPD.
The first task for the VPD team is to determine whether the patient actually has VPD. This determination has traditionally been made solely on the basis of a perceptual speech/language evaluation by a speech/language pathologist with specific training and experience in velopharyngeal function (Jones 1991). This evaluation includes both spontaneous speech and a provocative speech sample, structured to specifically challenge the velopharyngeal mechanism with increasingly more complex tasks (Philips 1980; Kummer 2007; Peterson-Falzone et al. 2010). The primary activity of this perceptual assessment is auditory, that is, listening for the production of specific phonemes. However, observing the face for grimacing, watching for fogging of a mirror below the nares, and feeling for airflow through the nares with attempted pronunciation of phonemes that require velopharyngeal function are other perceptual assessments that assist the screening evaluation. Some professionals now argue that instrumental assessments of oral-nasal airflow should be part of this determination process. However, we have not yet incorporated nasalance measurement into our initial assessment.
The auditory perceptual screening of velopharyngeal function sorts the patient into one of three groups: normal VP function, minimal VPD without impairment of communication or psychosocial stigmatization, or sufficient VPD to interfere with speech comprehension by others and/or stigmatize the speaker. If the assessed individual screens normally, no further evaluation of the velopharynx is indicated until the return for routine follow-up or some concern regarding speech arises. If the possible dysfunction is minimal, meaning that the affected individual and his or her parents, in the case of a child, were not aware of a speech problem and the cleft team, in concert, feels that the dysfunction is unlikely to cause impairment of communication or have psychosocial consequences, then the affected individual will have a repeat auditory perceptual speech evaluation at an interval shorter than the usual follow-up and the individual/parents will be informed of the concern regarding velopharyngeal function as well as of the signs and symptoms of increasing dysfunction so that they can contact the cleft team should they occur. If, on the other hand, it is the perception of the sophisticated observer that there is a possibility of morbid velopharyngeal dysfunction, further evaluation is considered.
If one accepts the principle that treatment should be diagnosis specific, and I do, then effective management of velopharyngeal dysfunction requires both recognition of the condition and definition of the responsible pathoetiology (Jones 1991). While auditory perceptual evaluation can separate normal from abnormal velopharyngeal function, it cannot identify the etiology of the dysfunction. Instrumental velopharyngeal evaluations, in contrast, can be etiology specific (Yules and Chase 1968; Shprintzen and Golding-Kushner 1989; Hirschberg and Van Demark 1997). Instrumental evaluations can be divided into those that visualize the velopharynx and those that indirectly assess its function (Albery et al. 1982; Dalston and Warren 1986; Dalston et al. 1991; D’Antonio et al. 1988; Hardin et al. 1992). Clinically useful visualization utilizes still (lateral skull x-ray) or real-time x-ray (speech videofluoroscopy). Documenting the effect of velopharyngeal sphincter function on airflow air pressure or sound or light transmission across the velopharyngeal port produces indirect data about velopharyngeal function. A multidisciplinary consensus regarding reporting of visualization studies provides a useful means for standardized interpretation of such studies (Golding-Kushner et al. 1990). For the past 20 years, the cleft teams that I have been associated with have used both nasendoscopic and fluoroscopic imaging of the velopharynx during standardized speech tasks to evaluate velopharyngeal function (Sinclair et al. 1982; D’Antonio et al. 1988; Shprintzen and Golding-Kushner 1989; Stringer and Witzel 1989). These evaluations are audio-video recorded, previously on magnetic tape and now digitally, in order:
1.
To permit review by other members of the cleft team who were not present during the actual examination
2.
To permit comparison of serial assessments of the same individual
3.
To permit comparative assessment of the effects of therapeutic intervention in the same individual
4.
To facilitate cross-sectional comparison of various interventions
These tapes are then reviewed by a subset of the cleft palate team, which consists of representatives from the disciplines of otolaryngology, plastic surgery, and speech/language pathology (D’Antonio et al. 1989; Sell and Ma 1996). A consensus opinion regarding interpretation of the images and preferred method of management is then arrived at by group discussion. The conclusions are communicated to the patient/family for reaction and to appropriate primary and secondary care providers, such as the patient’s speech therapist and pediatrician/physician. When velopharyngeal management, either prosthetic or surgical, is recommended and performed, the velopharyngeal function is reevaluated 3 months after the intervention with auditory perceptual and instrumental evaluations mirroring those performed preoperatively.
36.2 Differential Diagnosis of Velopharyngeal Dysfunction
For the purposes of differential management based upon differential diagnosis, velopharyngeal dysfunction can be divided into four broad etiologic categories:
1.
Anatomic deficiency
2.
Myoneural deficiency
3.
Anatomic and myoneural deficiency
4.
Neither anatomic nor myoneural deficiency
Each category has several specific causes for that deficiency. Anatomic deficiency includes those static tissue problems that prevent adequate velopharyngeal sphincteric closure, such as an unrepaired cleft palate, a palatal fistula, a short velum, or a deep velopharynx. Myoneural deficiency implies that there is adequate palatal and velopharyngeal structural anatomy but one or more components of the velopharyngeal port have inadequate or absent function, such as may occur with head trauma or degenerative neurologic disorders. Combined anatomic and myoneural deficiency may occur with repaired cleft palate, unoperated submucous cleft palate, or post-ablative surgery and/or radiotherapy for oronasopharyngeal malignancy. Rarely an individual presents who has intact velopharyngeal anatomic structures and is myoneurally intact but whose speech nonetheless exhibits signs and symptoms of velopharyngeal dysfunction due to either learned behavior, such as having a parent with cleft VPD and living in a rural area, or psychiatric disorder.
The initial goal of the instrumental evaluation of the presumably impaired velopharynx is to determine which of the four categories the patient belongs to since that broadly determines the type of therapeutic intervention(s) to be considered (see below). The combination of visual direct and indirect (mirror, endoscope) intraoral inspection and indirect velopharyngeal functional inspection (nasendoscopy, multiview fluoroscopy) permits definition of the structural and functional impairments contributing to the VPD. Once the category has been defined, further general health history, physical examination, and testing determine the specific etiology for that patient’s VPD.
36.3 Differential Management of Velopharyngeal Dysfunction
The four etiologic categories enumerated above broadly determine the differential management of velopharyngeal dysfunction. Anatomic deficiency is usually managed by restoration of the deficiency by either surgical or prosthetic means (Marsh and Wray 1980) (Fig. 36.1). Myoneural deficiency is usually managed prosthetically until the neurologic status has stabilized and the patient becomes a candidate for velopharyngeal surgery, which may or may not occur (Riski and Gordon 1979). Combined anatomic and myoneural deficiency is usually managed by restoration of the deficiency by either surgical or prosthetic means. Speech therapy, often pre- and usually post-intervention, is an essential element of management of these three categories in addition to surgical or prosthetic intervention. For learned or behavioral VPD, speech therapy with or without behavioral management is the treatment of choice; there is no role for surgery in such cases (Heller et al. 1974).
Prosthetic management for VPD is indicated when:
1.
The patient is unsuitable for surgical velopharyngeal management due to other major medical problems, such as inoperable congenital cardiac disease or severe pulmonary insufficiency (if and when the other medical problem becomes resolved or stabilized enough to minimize the anesthetic/surgical risk, conversion to surgical velopharyngeal management is considered).
2.
The parents/legal guardians refuse to permit surgery because of religious or emotional considerations.
3.
The patient has a complex speech/language problem, and it is not clear that velopharyngeal management will significantly improve speech intelligibility (if the trial of a speech prosthesis demonstrates significant improvement in intelligibility, then conversion to surgical velopharyngeal management is considered).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


