Fig. 5.1
The bone remodeling cycle. Remodeling is the replacement of old by new bone tissue that mainly occurs in the adult skeleton to maintain bone mass. This process involves the coupling of bone formation and bone resorption and consists of the following phases: resting, osteoblasts become resting bone-lining cells on the newly formed bone surface; activation, preosteoclasts are stimulated and differentiate under the influence of cytokines and growth factors into mature active osteoclasts; resorption , osteoclasts digest mineral matrix (old bone); transition , the end of resorption; and formation , osteoblasts synthesize new bone matrix
As humans age, the balance between bone formation and bone resorption is shifted in a negative direction. The number of remodeling sites across the skeleton increases under conditions of sex hormone deficiency [5]. Bone loss is the result of an imbalance in bone turnover, with bone resorption occurring at a faster rate than new bone formation. Thus, bone loss is an inevitable component of the aging process, particularly in postmenopausal women and in men with declining sex hormone levels [6]. The resulting reduction in bone mass and the accompanying damage to bone microarchitecture increase the risk of fracture. The spine (vertebral fractures), hips, and wrists (nonvertebral fractures) are the most common sites of osteoporosis-related bone fractures (i.e., fractures that are out of proportion to the level of external trauma), although osteoporosis-related fractures can occur at almost any skeletal bone site [7]. The most common form of osteoporosis, experienced by postmenopausal women, results from reduced estrogen production, which disrupts the fine balance of the bone remodeling cycle [8], and from increasing bone resorption. Osteoporosis is related to an increased risk of fractures, frequently resulting in chronic pain, disability, and death [9]. It affects approximately 26% of women and 4% of men after the age of 65 years [10, 11].
5.2 Bisphosphonates in Osteoporosis
Bisphosphonates (BPs) have been the principal anti-resorptive agents used in the therapy of osteoporosis over the last decade. Since the introduction of the first agent, alendronate, 191 million prescriptions have been written for their use [12]. Bisphosphonates work because of two key properties: (1) strong binding to bone due to a high affinity for hydroxyapatite [13, 14] and (2) the ability to inhibit osteoclast function owing to the inhibition of the enzyme farnesyl diphosphate synthase.
The Food and Drug Administration has approved the use of BPs for the treatment and/or prevention of osteoporosis. Oral alendronate (Fosamax; Merck) and oral risedronate (Actonel; Procter and Gamble Pharmaceuticals) were approved in 1995 and 2000, respectively. In 2003, oral ibandronate (Boniva; Roche Therapeutics) received approval, followed by intravenous ibandronate in 2006. Most recently, intravenous zoledronate (Reclast; Novartis) joined the market for these drugs in 2007.
Moreover, in several European countries, clodronate (a first-generation BP) has been used since 1985 for the treatment and prevention of postmenopausal osteoporosis (Fig. 5.2, Table 5.1). The diagnosis of osteoporosis relies on the quantitative assessment of bone mineral density (BMD), which correlates positively with bone strength and helps to predict future fracture risk (Fig. 5.3).
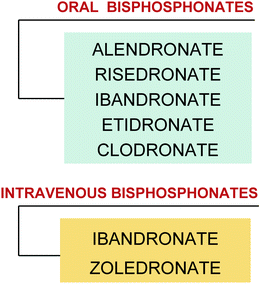
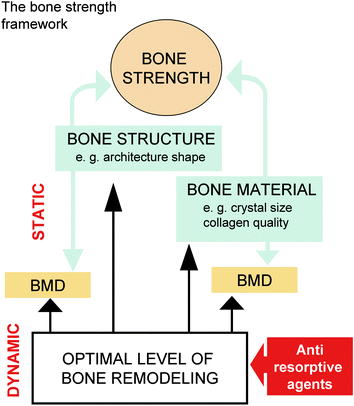

Fig. 5.2
Classification of bisphosphonates (oral and intravenous)
Table 5.1
Bisphosphonates: indication, dosage, and administration requirements
|
Bisphosphonate
|
Indications
|
Dosage for osteoporosis
|
Administration requirements (for osteoporosis)
|
|
|---|---|---|---|---|
|
Prevention
|
Treatment
|
|||
|
Alendronate (Fosamax)
|
Prevention and treatment of osteoporosis in postmenopausal women
|
35 mg tablet weekly
|
70 mg weekly tablet or oral solution
|
Patient must remain upright for 30 min following dose
|
|
Treatment to increase bone mass in men with osteporosis
|
5 mg tablet daily
|
10 mg tablet daily
|
||
|
Ibandronate (Boniva)
|
Prevention and treatment of osteoporosis in postmenopausal women
|
2–5 mg tablet daily
|
Same as prevention dosage
|
Oral (tablet)Patient must remain upright and refrain from eating 60 min following dose
|
|
150 mg tablet monthly
|
||||
|
3 mg intravenous injection every 3 months
|
Intravenous injection 15- to 30-s bolus i.v. injection that must be administered by a health care professional
|
|||
|
Risedronate (Actonel)
|
Prevention and treatment of osteoporosis in postmenopausal women
|
75 mg consecutive days/month
|
Same as prevention dosage
|
Patient must remain upright for 30 min following dose
|
|
Treatment to increase bone mass in men with Osteporosis
|
5 mg/day
|
|||
|
35 mg/weekly
|
||||
|
Zoledronate (Reclast)
|
Prevention and treatment of osteoporosis in postmenopausal women
|
A single 5-mg infusion once a year given intravenously over no less than 15 min in a 100-ml ready-to-infuse solution
|
||
|
Administer through a separate vented infusion line and do not allow contact with any calcium- or divalent-cation-containing solutions
|
||||

Fig. 5.3
The bone strength framework: relationship between bone mineral density and anti-resorptive agents
The World Health Organization (WHO) defines osteoporosis as a hip or spine BMD of ≤2.5 SD below the normal mean reference values for a young population, which has reached peak bone mass [15]. In addition, the WHO recently introduced a Fracture Risk Assessment Tool (FRAX) to help predict the 10 year probability of a hip or other major osteoporotic fracture in untreated men and women between the ages of 40 and 90 years. The tool makes use of the femoral neck BMD as well as risk factors that are largely independent of BMD [16].
The major treatment goal for patients with osteoporosis is to prevent fractures by maintaining or increasing BMD and reducing excessive bone turnover. In fact, BPs, a mainstay among the various classes of anti-osteoporotic drugs, have been shown in numerous clinical trials to increase BMD and to reduce the risk of osteoporotic fractures [17]. Nevertheless, clinical case reports have described unusual fractures with irregular healing in cases in which an oversuppression of remodeling by BP was thought to be the cause. For example, reports of fractures of the subtrochanteric femur, pelvis, and tibia, which are uncommon in osteoporosis, focused attention on the possibility of oversuppression [18–20]. This possibiity has led some clinicians to recommend the delay of BP therapy in patients hospitalized for treatment of hip fractures, thus adding to the already difficult problem of delivering follow-up anti-fracture therapy to patients known to have osteoporosis [21, 22].
5.3 Clinical Efficacy and Safety of Bisphosphonates
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


