The aim of this study was to present the orthodontic treatment of a 15-year-old boy with a unilateral maxillary molar distalization system, called the zygoma-gear appliance. It consisted of a zygomatic anchorage miniplate, an inner bow, and a Sentalloy closed coil spring (GAC International, Bohemia, NY). A distalizing force of 350 g was used during the distalization period. The unilateral Class II malocclusion was corrected in 5 months with the zygoma-gear appliance. The maxillary left first molar showed distalization of 4 mm with an inclination of 3°. The maxillary premolars moved distally with the help of the transseptal fibers. In addition, there were slight decreases in overjet (−0.5 mm) and maxillary incisor inclination (−1°), indicating no anchorage loss from the zygoma-gear appliance. Preadjusted fixed appliances (0.022 × 0.028-in, MBT system; 3M Unitek, Monrovia, Calif) were placed in both arches to achieve leveling and alignment. After 14 months of unilateral distalization with the zygoma-gear appliance and fixed appliances, Class I molar and canine relationships were established with satisfactory interdigitation of the posterior teeth. Acceptable overjet and overbite were also achieved. This article shows that this new system, the zygoma-gear appliance, can be used for unilateral maxillary molar distalization without anchorage loss.
Treatment of a Class II malocclusion usually requires distal movement of the maxillary molars to achieve a Class I molar and canine relationship. The most conventional method to distalize maxillary molars is to use cervical headgear, which can be used for either orthodontic or orthopedic corrections. However, the major disadvantage of an extraoral method is lack of patient cooperation during treatment. Although it has been shown that a unilateral Class II malocclusion can be corrected by headgear with asymmetric face-bows, the force delivery system unavoidably contains a lateral component that can result in a posterior crossbite.
Because of these disadvantages, intraoral distalization appliances have been introduced that minimize patient compliance requirements and applied continuous forces. Those appliances effectively distalize the maxillary molars; however, in most of these studies, anchorage loss is unavoidable, characterized by maxillary incisor protrusion, increased overjet, and decreased overbite. To overcome these anchorage problems, skeletal anchorage units applied to the palatal regions—eg, miniscrews, osteointegrated im-plants, and Graz-type implants—were combined with these tooth-supported and tissue-supported intraoral appliances. Although anchorage loss has been eliminated in this way, the bulky acrylic Nance appliance behind the maxillary incisors can become a problem during retraction of the anterior teeth.
Recently, Nur et al designed an intraoral appliance, called the zygoma-gear appliance, for bilateral maxillary molar distalization using titanium anchor plates placed in the zygomatic process of the maxilla. They stated that absolute anchorage control was provided by using zygomatic anchorage plates during distalization of the molars and retraction of the incisors.
In this article, the zygoma-gear appliance with zygomatic miniplates was used to distalize the maxillary molars unilaterally, relieve crowding, and establish a Class I molar relationship.
Diagnosis and etiology
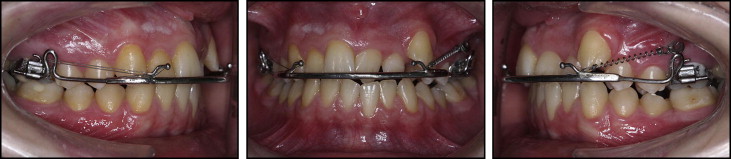
The patient was a 15-year-old boy with a chief complaint of dental crowding in the maxillary anterior teeth. The pretreatment photographs showed an ectopically erupted canine and a maxillary left central incisor in crossbite ( Fig 1 ). He had an Angle Class II molar relationship on the left side and a weak Class I molar relationship on the right side. Although they were measured from the most labially positioned tooth (right central incisor), overjet was 3 mm and overbite was 2 mm. The mandibular midline was 1.0 mm to the left of the facial midline because of the crowded mandibular left incisors. The maxillary and mandibular arch-length deficiencies were 6 and 2 mm, respectively. The Bolton tooth-ratio analysis (sum of incisors, 4:3.08; anterior ratio, 76.4%; overall ratio, 91.1%) indicated that the maxillary teeth were generally larger than the mandibular teeth. On the other hand, there was no transverse discrepancy. The patient had an SNA angle of 74°, an SNB angle of 72.5°, and an ANB angle of 1.5°. The mandibular plane was normal relative to the cranial base (SN-GoGn, 33°). The mandibular incisors had a 96° angle relative to the mandibular plane, and the maxillary incisors had a 117° angle relative to the palatal plane ( Table ). The temporomandibular joint evaluation showed no signs of clicks or crepitation, and the facial and masticatory muscles were asymptomatic.
| Measurement | Before distalization | After distalization | After treatment |
|---|---|---|---|
| SNA (°) | 74 | 74 | 74 |
| SNB (°) | 72.5 | 72 | 72 |
| ANB (°) | 1.5 | 2 | 2 |
| Wits (mm) | 1 | 0 | −0.5 |
| SN-GoGn (°) | 33 | 34 | 35 |
| ANS-PNS/GoGn (°) | 25 | 26 | 28 |
| FMA (°) | 24.5 | 25 | 26 |
| U1-NA (mm) | 8 | 7.5 | 8 |
| U1-NA (°) | 28 | 27 | 29 |
| U1-ANS-PNS (°) | 117 | 116 | 114 |
| L1-NB (mm) | 6 | 6 | 8 |
| L1-NB (°) | 25 | 25 | 27.5 |
| IMPA (°) | 96 | 96 | 97 |
| U1-PtV (mm) | 62.5 | 62 | 62 |
| U6-PtV (mm) | 31 | 27 | 28 |
| U6/ANS-PNS (°) | 75 | 72 | 74 |
| Overjet (mm) | 3 | 2.5 | 2 |
| Overbite (mm) | 2 | 1 | 2 |
| Lower lip–E-line (mm) | −3 | −3.5 | 1.5 |
| Upper lip–E-line (mm) | −4 | −5 | 6 |
| Nasolabial angle (°) | 117 | 115 | 114 |
The treatment objectives for this patient were to (1) relieve the crowding, which was his chief complaint; (2) establish Class I molar and canine relationships; (3) create ideal overbite and overjet; (4) correct the midline shift; and (5) establish a proper soft-tissue profile.
There were 3 treatment alternatives for this patient: (1) extraction of the maxillary left first premolar, (2) extraction of the maxillary left second premolar, and (3) distalization of the maxillary left first molar.
The patient and his family chose the nonextraction alternative, and distal movement of the maxillary left first molar was planned. There were 2 choices to achieve this movement: intraoral distalization mechanics and asymmetric headgear. The patient refused to wear headgear because of social and esthetic concerns. The maxillary left canine needed to be aligned; thus, preventing anchorage loss of the first premolar was important. We planned to use intraoral distalizing mechanics combined with zygomatic miniplates for distalization of the maxillary left first molar.
A miniplate (left medium plate; Walter Lorenz Surgical, Jacksonville, Fla) was placed at the zygomatic buttress of the maxilla under local anesthesia. The miniplate was adjusted to fit the contour of the lower face of the zygomatic process and was fixed by 3 titanium bone screws (length, 5.0 mm; diameter, 2.0 mm). The inner bow was a modified version of the inner part of a conventional face-bow. Two hooks were soldered onto the inner bow at the lateral tooth regions, and U bends were bent bilaterally in front of the maxillary first molars. The inner bow was adjusted to the headgear tubes on the maxillary first molar bands because the anterior component of the inner bow was about 3 mm from the anterior teeth. To prevent a crossbite on the left side from the distalization force, the bend was made on the inner bow. On the right side not requiring distalization, the maxillary molar tube and the hook were ligated.
Three weeks after the surgery, a distalization force of 350 g was unilaterally applied to the maxillary left first molar with a Sentalloy closed coil spring (GAC International, Bohemia, NY) attached with 0.01-in stainless steel ligature ( Figs 2 and 3 ). The force of the coil spring was calibrated with a gram-force gauge (Correx; Haag-Streit, Koeniz, Switzerland) during the initial activation and checked at 4 weekly intervals to ensure that the same force was maintained throughout the treatment. The appliance was adjusted by widening the U bends with a plier when the distance between the anterior teeth and the inner bow was near 1 mm during the distalization and distalization was still required, as described by Nur et al. The zygoma-gear appliance was removed at the end of distalization, and the maxillary first molars were stabilized by a transpalatal arch for 1 month before the fixed orthodontic treatment ( Fig 4 ). The maxillary premolars drifted distally without any orthodontic force with the help of the transseptal fibers ( Fig 5 ). Preadjusted fixed appliances (0.022 × 0.028-in, MBT system; 3M Unitek, Monrovia, Calif) were placed in both arches to achieve leveling and alignment. After leveling and alignment, a power chain was applied to move the canine and the premolars distally. At the end of active treatment, finishing procedures were used for final alignment of the teeth and detailing of the occlusion. The fixed appliances were removed after active treatment was completed, and a maxillary Hawley retainer and a 3-3 mandibular fixed lingual retainer were constructed for the patient and then placed. The miniplate was stable during the total treatment period and successfully removed with local anesthesia after the debonding.