Fig. 7.1.
a Maxillary restoration supported by strategically positioned abutments, b In many cases, all it takes to obtain strategic abutments for durable maxillary restorations is to combine a single BOI implant with residual natural teeth
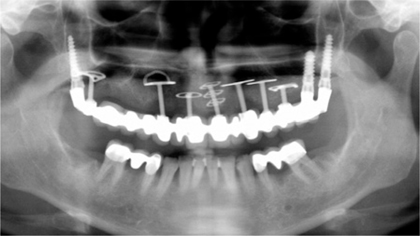
Fig. 7.2.
Maxillary restoration supported by multiple implants. The distal abutments consist of tuberosity and pterygoid screws, while BOI implants were used in the anterior segment in accordance with the available bone width. The BOI implant at 13 was vestibularly folded and adapted to the vestibular surface of the maxilla
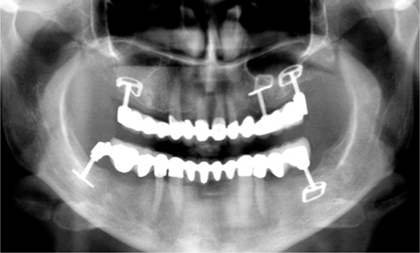
Fig. 7.3.
Canines can offer very good support. They can be used alone or in combination with the first premolar
In situations of advanced resorption, it is no longer possible to differentiate between basal and crestal implantation. The important part is to utilize the cortical bone.
7.2.2 Mandibular Restorations
Since the mandible may be subject to heavy torsion, a multi-implant strategy would overly reduce the elasticity of that bone. For this reason, we generally use four to six implants, with one distal implant on each side only. Stable canines can be used instead of an implant.
Today we tend to use no BOI implants with more than one disk in the distal mandible and prefer to put no implants at the premolar positions to ensure that the elasticity of the mandible is not overly reduced and that no high point is created in the middle of the horizontal part of this bone. Triple- and double-disk BOI implants can be used to good effect along the anterior block of the mandible.
In the maxilla, BOI implants may be combined with natural abutments in virtually any combination, as long as the teeth are stable enough to offer long-term resistance to the forces acting on it. When considering a tooth as part of a larger bridge, it should be considered that overall masticatory forces will increase.
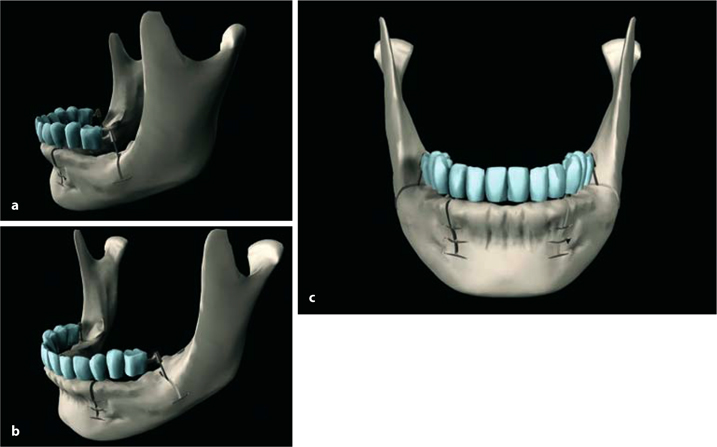
Fig. 7.4a-c.
These schematic drawings illustrate the correct implant positions for strategic implant placement in the mandible
7.3 Which Jaw Should be Restored First?
Concerning the issue which jaw should be restored first, we have developed the following approach in our clinic: if therapeutic modifications are needed in both jaws, the mandible should be treated first if possible. There are several reasons:
-
Complete dentures are not retained nearly as well in the mandible as in the maxilla. Therefore, the need to provide relief is greater in the mandible.
-
In many cases, additional implant treatment in the maxilla turns out to be redundant once a fixed restoration has been inserted in the mandible.
-
The morphological changes in the mandible are often substantial, particularly in the wake of adjustments performed to re-establish a normal masticatory pattern. Simultaneous placement of implants in the maxilla and mandible carries a high risk of overloading the newly inserted implants in the maxilla. Relative elevation of the distal implants is especially liable to inflict damage to maxilla. Conditions are more favourable once the functional adaptation after implant placement in the mandible have been largely completed.
Similar results were reported by Lindquist and Carlsson (1982), who observed that the ability to eat eight out of ten types of foods that the patients had previously been unable to eat was restored after inserting a mandibular restoration supported by enossal implants. Chewing function was significantly improved once these restorations were in place. In patients on a limited budget, a cost-benefit analysis will therefore definitely argue in favour of providing an implant-based solution in the mandible rather than the maxilla. This strategy will be effective in the majority of patients and will often render additional treatment of the maxilla redundant. According to Lindquist and Carlsson, implant treatment of the maxilla is only necessary in specific cases. We feel that this view needs to be put into perspective, as considerable progress has been made with implant treatment in the maxilla since 1982. With today’s BOI technology, implant-supported fixed restorations have become just as affordable, successful and simple to realize in the maxilla as they have been in the mandible all along.
Treating the mandible first makes sense from a functional viewpoint as well. Tallgren et al. (1986) demonstrated that the changes in masticatory function brought about by inserting immediate dentures in the mandible can be reduced if a fixed dentition is at least partially present in the mandible. This conclusion is quite plausible, considering that better muscle orientation is achieved during chewing if reliably positioned teeth are present in at least one jaw.
If a complete denture is present in the maxilla, the necessary elevation of the occlusal plane towards Camper’s plane can be performed more readily than in the presence of a fixed restoration or of elongated natural teeth. In spite of that, the occlusal plane should always be equalized if necessary. Trying to save money on this aspect of treatment will be counterproductive in the long term.
One also has to keep in mind the fact that the teeth in the mandible often resist imbalanced situations better than the teeth in the maxilla. If in the maxilla large bridges are present, this will sometimes lead to a situation where a patient faces a complete breakdown of the maxillary restoration and dentition with the reason for the brakdown being located in the stronger, but unbalanced and/or unfavourably designed prosthetics in the lower jaw. We strongly recommend in these cases always to treat the lower jaw first or simultaneously, because it is dangerous to rely on the patient’s willingness really to treat the mandible after the problems in the (aesthetically to him/her more important) upper jaw. We have seen sad cases where the patients forgot about the agreement about treatment in the mandible, vanished from the scene (even missing regular check-ups in order not to be reminded about the agreement), and returned later with problems again in the upper jaw.
7.4 When Should the Implants be Loaded?
Obviously, there is no way for implants to remain completely “non-loaded” once they are located within the bone. The appropriate point of time at which all or part of the chewing force should be transmitted through all or some of the BOI implants onto the cortical bone will depend on the conditions present during surgery, the number of implants inserted, and the general circumstances under which mastication takes place. Since the cranial bone is permanently in a state of torsion, there can be no such thing as a “non-loaded” state of implants. We therefore maintain that it is more sensible to define the type and direction of loading via a prosthetic superstructure than to leave the bone without this well-dosed stimulus.
Part of this rationale is to insert the superstructure while excellent primary stability is present. Following this logic, prosthetic loading should take place within the 8–12 days (the sooner, the better). Due care must be exercised in deciding on this strategy, which may be contraindicated in specific cases (i.e. in surgically pre-treated areas). The other alternative would be to load the implants after 6-8 weeks when the phase of bone healing and bone repair has been completed. The implantologist may want to select a different time if numerous abutments are present, provided that the superstructure can then be inserted in a tension-free manner. Such re-scheduling is less advisable in the maxilla than in the mandible with its considerable macrotrajectorial stresses.
Both jaws undergo extensive bone remodelling. If a large number of load-transmitting disks have been inserted, it is unlikely that individual implants are loaded to the point of creating deleterious osteolytic processes. On the downside, little bone will remain for a second treatment attempt if implants become unstable because of other factors.
Essentially, we always attempt to insert as many implants and load-transmitting surfaces in the surgical phase of treatment as are necessary to realize immediate loading. In first implantation procedures, the goal of immediate loading can be achieved almost invariably. A temporary restoration is inserted in the maxilla for 2–12 months, while the mandible can usually be treated with a definitive restoration right away. Temporary restorations may need to be replaced or adjusted inside or outside the mouth several times, particularly in the maxilla, as functional and morphological alterations are developing over the course of treatment and/or extensive chewing-related adjustments have to be performed. On occasion, it may be necessary to compensate for spontaneous repositioning of the TMJs. Such repositioning may only occur after weeks or indeed months and may proceed in a stepwise fashion, reflecting the step-by-step release of spastic contractions of the lateral pterygoid muscle. In those cases, the masticatory surfaces must be redesigned several times, also taking into consideration that the steepness of the cusps must fit the age of the patient. Any delays in readjustment may trigger a unilateral or anterior chewing pattern.
7.5 General Biomechanical Considerations in Treatment Planning
BOI implants are designed to replace natural teeth and assume their function of transmitting the incoming masticatory loads into the bone. They consist of one or several load-transmitting disks (also referred to as basal plates or rings), a threaded pin not designed for load transmission, and web bars connecting the disk(s) to the threaded pin. The disks are available in different shapes aimed at optimally adapting the integrated implants to different bone configurations. Correct choice of the dimensions of the BOI implant is required because BOI implants, unlike screw designs, always utilize the available native bone structure to anchor the implant-restoration systems. The bone available at the beginning of the therapy is considered to be the best bone of the patient, because it is assumed to be in the areas of main trajectories under functional conditions.
Cortically anchored basal plates are an integral component of BOI implants designed to guide the masticatory forces into the enossal space. Depending on the indication, one or several disks per implant may be required, along with threaded pins that are relatively rigid or elastic. The enossal surfaces of the implant may be either roughened or smooth, depending on the task they are designed to fulfil both in the early treatment phase and in the long term.
In our experience, disks with a diameter of less than 9 mm will always constitute relatively rigid points of load transmission. Strictly speaking, these designs do not allow implant-restoration systems that truly conform to the principle of basal osseointegration. At least, the elasticity of these systems will be considerably reduced. This clinically undesirable lack of elasticity is aggravated by short threaded pins and disks that are small in diameter but thick.
In addition, the mechanical properties of the implant material are an important factor as well. BOI implants are usually made of Grade 1 (ASTM F 67), Grade 2 or Grade 3 titanium as per that ASTM standard. Some designs are also available as an extremely strong titanium-molybdenum alloy (Ti15Mo). This alloy combines the elasticity of Grade 1 titanium with a level of strength that can otherwise only be attained with Grade 4 titanium. Long-term observations with this new material are not yet available. We currently use this material in structures that have to resist great lever forces. This is frequently the case when massive skeletal discrepancies of maxillary micrognathia or mandibular prognathia have to be overcome.
The purpose of this book is to describe how implant-restoration systems can be integrated more or less isoelastically into the viscoelastic environment of the human jaw. Bone quality as defined by Misch (I-IV) only describes the present condition of the bone, which is obviously poor in edentulous situations as the bone is not trained. Therefore, this classification is largely irrelevant for anatomists and BOI implantologists alike. Measuring Hounsfield units is, in effect, totally useless if we consider that the measured parameters will change instantly once implants have been inserted.
The only interesting aspect is how the bone mechanisms responsible for recognizing, scanning, rejecting or enclosing the implant can be optimally utilized. These mechanisms are more likely to behave according to plan if an intact blood supply is available and if osteogenic stem cells are present in large numbers even at the outset of implant treatment.
There are also situations in which more rigid designs (e.g. triple-disk implants of the “EDDD” type) are an appropriate choice. They can be used in conjunction with other BOI or, indeed, crestal implants to support more rigid implant-restoration complexes, or they can be used as single-tooth implants to replace anterior teeth or premolars in the maxilla or mandible. Bar attachments can be used to good effect on triple-disk implants as well.
Although the concept of (iso)elastic anchorage of dental implants reappears several times in the history of our profession (Breme et al. 1993), the concept was fully realized only on a few occasions. (Intramobile elements were developed and introduced by IMZ in the early days of modern crestal implantology, based on the realization that the human body was a viscoelastic system and should not be treated with rigid implants connected by rigid splinting. Other manufacturers did not follow suit, however, and today the concept is regarded as obsolete. We are told that the market “did not accept” these designs and that they are old-fashioned. More probably, other products were supported by heavier advertising and came in ahead, despite the fact that the IMZ concept as such was biomechanically flawless.)
With crestal implants, mobile incorporation of the implant body is, after all, tantamount to fibro-osseointegration, which will quickly give rise to implant loss once the fibrous area gets infected. This problem does not exist with BOI implants.
Crestal implantologists infer from this that the jawbone will grow towards implants for which primary stability has been achieved “voluntarily” and “deliberately”, as it were, to prepare the ground for functional load transmission. As will be shown further below, a substantially greater incentive for bone remodelling comes from stimulation of neighbouring osteons when force transmitting trajectories are disrupted in the process of preparing the implant bed. This mechanism has been well known also in orthopaedic surgery. The implant itself mediates stimuli only to a very small extent in the direct contact area.
The forces acting on the various bones of the skull vary widely in different cranial areas. These bones are therefore elastic and show very different degrees of mineralization depending on their exact location. These observations are most apparent in the anterior mandible. Areas characterized by lower mineralization and higher elasticity will respond to flexural forces by more extensive deformation. Introducing large (long) implant bodies in areas of this type can give rise to any one of the following scenarios:
-
The elasticity of the surrounding bone may decrease to match the elasticity of the implant. In that case, other zones of high elasticity will form in that jaw instead.
-
The high elasticity may remain intact, but only a small percentage of the enossal surface becomes osseointegrated.
-
The high elasticity may remain intact, and a high percentage of the enossal surface becomes osseointegrated,but the bone is undermineralized, so that the various bone layers are freely mobile.
The term “extraterritorialization” of the implants has been proposed because osseointegration was regarded as a delimiting reaction – a process of “cystification”, as it were. An implant thus becomes extraterritorialized as cortical bone forms in the interface area, ultimately reducing the blood supply and exterminating any osteocytes near the implant. This reaction is also due to a disrupted oxygen and substrate supply, which eventually causes the osteocytes near the implant to become pycnotic and thus threatened by extinction.
In crestal implantology, it has been postulated that the surface available for osseointegration should be as large as possible (DGZMK, DGI, 2001) to optimize the long-term survival of the implant (Brandt 1996). This demand led to the introduction of long implants, followed by large-diameter implants. These developments ignored, however, that the mucosal penetration point of large-diameter implants is considerably larger, thus offering more space for infection. The prognosis of short implants with roughened surfaces is seriously marred by the fact that bacterial loads rise exponentially with increasing implant diameters (Knaus 2000; Müller-Herzog and Lindorf 1996). The intraosseous blood supply is presumably greatly reduced, which may even promote the development of sarcomas down the road. Some of the postulates of crestal implantology are indeed questionable. As a case in point, the prognosis of implants covered with a porous coating allowing perfusion until deep under the surface (Osseopore) becomes poorer with increasing implant lengths because the perfusion system loses its functionality in longer designs.
Longer implants placed in areas of flexion are bound to transverse various enossal layers that will change their relative positions during normal chewing function. These movements are more apparent in the mandible, but they are significant in the maxilla as well. In contrast to the specially prepared skeletized skulls used for anatomical studies, live cranial bones are characterized by relative mobility and high hydrostatic pressures. In addition, they are affected by the rhythmical movements of the craniosacral, respiratory and masticatory systems. Notably by the active movements of mastication and facial expression, the bones are constantly kept in a state of mutual flux and intrabony torsion. Note that the intraosteonal flow of nutrients is enhanced by bone torsion.
The successful outcomes of slightly conical non-threaded implants with a spherical surface (Osseopore) demonstrate that the same degree of anchorage can also be obtained with very short designs. These implants stimulate mineralization in a radiographically demonstrable manner and are capable, according to their users, of supporting prosthetic restorations while involving rather distorted crown-implant ratios. Obviously, these implants cannot be splinted since the tensions developing through the prosthetic structure would eventually result in bone avulsion after all. The first point to consider with these implants is that they should be inserted over their entire length into a bone layer of uniform behaviour. As a result, the level of functional movements inside the bony implant bed will be relatively low. In other words, these implants will remain unaffected by any local or comprehensive movements of the cranial bones – provided, of course, that they are not used to support large-span bridges. The second point to consider is the ingenious surface structure of these implants, which initially prevents the bone from growing too deeply under the surface. The empty space just below the surface represents a confluent system of canals that enables nutrients to be supplied by way of microcirculation very much as they are supplied naturally through osteons. In other words, the surface on which the bone layer will be forming bears greater resemblance to a three-dimensional microtitre plate than to a dead implant surface. This example once again demonstrates that even minute contact surfaces will ultimately be sufficient to adequately guide masticatory loads into the bone. As a prerequisite, however, the surface contact must be located in an area that is well supplied with nutrients. With cortically anchored BOI implants, these nutrients may be derived from the periosteum or from the interior of the jaw bone. With crestal implants, it is sometimes possible to achieve this goal through ingeniously structured surfaces and carefully selected implant sites. From the points that have just been discussed, it becomes clear why the minimum lengths and surfaces that have been “scientifically” postulated for crestal implants only apply to specific implant designs. In other words, they only apply to implants with surface characteristics that are conventional or do not lend themselves to biological integration because they cannot be perfused well in one way or another.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


