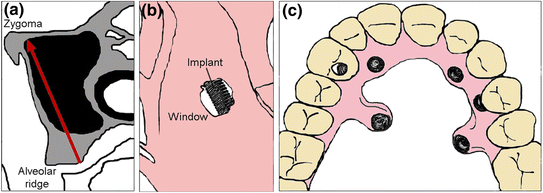
Fig. 2.1
Classification of bone quality
Type 1 (D1) bone quality is defined as the bone jaws that comprised of homogenous compact bone. While for Type 2 (D2), the bone consists of a dense cancellous bone core surrounded by a 2 mm thick layer of cortical bone. Type 3 (D3) bone consists of a thin layer of cortical bone surrounding a core of dense cancellous bone and Type 4 (D4) bone characterized as a thin layer of cortical bone surrounding a core of low density cancellous bone of poor strength [5, 8, 11]. Generally, the anterior region of maxilla can be classified as Type 3 whilst the posterior region or specifically the molar region is classified as Type 4 [5, 8]. Mandibles are generally more densely corticated than maxillae and both jaws tend to have thinner cortical and increased cancellous porosity towards the posterior [5, 8]. It is important to note that there is a high correlation between implant failure and poor bone density.
2.2 Potential of the Zygoma for Implantation
There was a possibility of placing dental implants in the zygomatic bone as mentioned by Aparicio et al. [13] in 1993. Other than that, the use of zygomatic bone as a support structure for the patients who undergone maxillectomies had been cited by Weischer et al. through a study in 1997 [14]. The measurement of maxilla and zygoma for pre-surgical planning of implant fixation was conducted by Uchida et al. in 2001 using 12 cadavers. The results showed that an implant diameter of 3.75 mm requires a zygoma thickness of at least 5.75 mm [15]. They concluded that an angulation of 43.8º or less increases the risk of perforating the infratemporal fossa or the lateral area of the maxilla. However, an angulation of 50.6º or more increases the risk of perforating the orbital floor [15]. Due to the curvy and complex shape of the zygoma, implants have to be placed at an appropriate angle with respect to the occlusal plane [16].
Another study done by Nkenke et al. determined the potential of zygomatic bone as a remote site for implant anchorage [17]. Computed tomography images and histomorphometry technique were used to examine 30 human zygomas. The authors revealed that zygoma consists of cancellous bone which is unfavourable for implant placement. Success of implants placed in the zygomatic bone could be achieved by crossing the implant through four cortical layers [17]. In contrast, Kato et al. investigated the internal structure of cadaveric edentulous zygomatic bone using micro-computed tomography and found the presence of wider and thicker cancellous bone at the apical end of the fixture that could be used to promote initial fixation [18].
2.3 Edentulous Jaw Classification
The classification of edentulous jaw is used in dentistry to identify the types of treatment suitable for patients. Jaw atrophy involves a reduction of alveolar height and width as well as bone remodelling that affects the external shape and the internal structure [19]. It occurs in chronic and irreversible fashion due to tooth extraction, trauma, infection, pneumatization of the maxillary sinus and ablative tumour surgery [17]. The pattern of alveolar ridge atrophy, however, is different between maxilla and mandible—maxilla exhibits centripetal resorption while mandible shows centrifugal resorption [20]. There is a higher tendency for bone resorption to occur at the edge of alveolar rather than at the bottom part of the socket after tooth extraction [8, 21]. Based on Tallgren’s classic study, more than 2 mm vertical resorption was found in the anterior jawbone between the first year after teeth extraction and insertion of complete dentures. However, the resorption rate of alveolar edge reduced to 0.05 mm/year in the edentulous maxilla and 0.20 mm/year in the edentulous mandible [22].
The resorption of maxilla will move the residual alveolar bone superiorly and medially [8]. In the posterior region of maxilla, critical bone atrophy can result in Class VI thin bone layer with a characteristics of reduced cortical bone thickness, or in a more severe cases a total loss of bone as illustrated in Fig. 2.2 [5]. This is probably due to critical remodelling process which occurs within the cancellous bone itself after tooth extraction. The thinning of cortical bone layer reduced the implant anchorage strength, causing a potential failure of osseointegration [8]. The lack of sufficient bone quantity can be solved through various bone augmentation techniques to increase bone volume for dental implant placement in the posterior region of maxilla [2, 23].
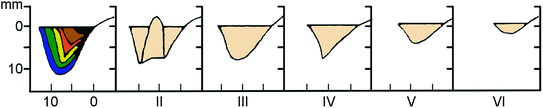

Fig. 2.2
Classification of jaw atrophy in posterior maxilla
2.4 Conventional Surgical Procedure by Using Bone Augmentation
Treatments for edentulous maxilla patients specifically with severe degree of resorption can be performed through several techniques—bone augmentation or grafting; using angled implants in parasinus region; placing implant in the pterygoid apophysis; using short and wide implants; or using zygomatic implants [24, 25]. Bone augmentation has been regarded as the gold standard procedure to treat atrophic maxilla, and the iliac crest is normally used as bone graft [24, 26]. Crestal onlay grafting, inlay grafting (maxillary antrum and nasal floor) or sinus lifting, Le Fort I osteotomy with interpositional grafting and distraction osteogenesis are among augmentation procedures performed to restore the lost bone (Fig. 2.3) [26, 27]. However, this procedure is resource demanding and requires a relatively longer time of treatment and a longer healing period for the patients [26]. In addition, harvesting of bone grafts could cause morbidity or infection of the donor site [17, 26–29].
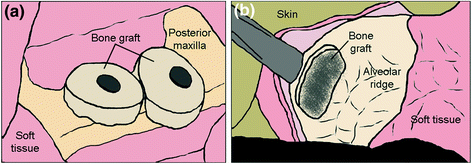

Fig. 2.3
Based on literature reviews, the survival rate of implant is lower for grafted maxillae compared to non-grafted maxillae especially in the posterior region [27, 28, 30]. It was reported that the use of autogenous drafts lead to a success rate of 87–95 % [27]. Keller et al. conducted a follow-up study of 248 implants placed in grafted maxillae using inlay autogenous bone grafts and reported a success rate of 87 % within a period of 57.1 months [31]. Another study reported by Branemark et al. in 2001 showed 80 % implants with favourable outcome within 2–15 years follow-up using the autogenous onlay bone grafting and simultaneous endosseous implant placement [32]. Similar results were reported by Lekholm et al. using the same technique of onlay bone grafting with a slightly lower success rate of 75 % [33, 34]. These results were true with the notion that implants placed in native bone has a greater probability of success compared to those implanted in grafted bone [27, 30]. In a comparative study by Widmark et al., a higher success rate was found for implants placed in native bone (96) compared to those using bone graft (82 %) after 1 year follow-up [27]. At 3–5 years follow-up, the success rate of corresponding implants reduced to 87 and 74 %. The nongrafting surgical procedures are therefore preferable for the edentulous atrophic maxilla as the bone augmentation technique resulted in less effective outcomes.
2.5 Advanced Surgical Procedure by Zygomatic Implant Application
Brånemark introduced an alternative system utilising zygomatic implants to overcome complications related to bone augmentation technique [24, 25, 27, 28, 34, 36, 37]. Zygomatic implants were previously utilised to rehabilitate patients who had undergone maxillectomy due to tumour resection, trauma or congenital defect [17, 28, 38]. However, the function of this implant had been extended for rehabilitation of edentulous atrophic maxilla patients. This implant was introduced to obtain a steady anchorage in zygomatic bone where placement of standard implants would not be possible in the posterior region of maxilla [39].
Zygomatic implant used for the treatment of edentulous atrophic maxillae comes in various dimensions in terms of length, diameter, thread distribution and other features (Fig. 2.4) [40]. Two treatment plans are currently used, either two or more zygomatic implants placed bilaterally without conventional implants support [27, 39], or one zygomatic implant placed bilaterally together with at least two conventional implants placed at the anterior region of maxilla [39, 41–43]. The selection of treatment plan depends on the degree of bone resorption in maxilla. The insertion path of zygomatic implant is usually from the alveolar ridge bone in second premolar or first molar region, going through maxillary sinus or its wall into zygomatic bone [24, 28, 40, 44]. The apical part of implant body will be directed or inserted into the wider and thicker cancellous bone of the zygoma [45].
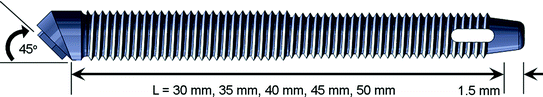

Fig. 2.4
Zygomatic implant specifications
2.5.1 Advantages and Disadvantages of Zygomatic Implants
The use of zygomatic implants to treat edentulous atrophic maxillae has a lot of advantages over the use of bone graft augmentation incorporation with conventional implants placement in the posterior region. The most prominent advantage is by not using the bone graft itself which is associated with donor site morbidity in the respective region [24, 27, 39, 43, 46]. The total treatment time also reduced as bone grafting procedure requires three to 6 months to heal before the bone can be loaded with traditional dental implants [39, 43, 46, 47]. An additional 6 months are then required to complete the whole process. In the case of immediate implant stabilisation through simultaneous loading and bone grafting, the whole process of prosthetic restoration will therefore take about 6 months to complete. However, this type of treatment is not suitable for patients with sufficient posterior bone volume [27]. The existing patient’s maxillary denture can be used as a temporary removable prosthesis prior to the actual prosthesis after soft tissue reline [27, 48]. Treatment using zygomatic implants also requires less hospitalization as the bone grafting technique needs 6 months for bone formation before the actual implant placement. Zygomatic implant approach could also reduce the number of supporting implants at the anterior region due to a steady implant anchorage is achievable in the zygoma, thus, reducing a potential complications [27, 48]. In terms of cost, treatment via zygomatic implant is almost similar to bone grafting.
The main disadvantages of zygomatic implant application are the complexity of implant installation as well as the emergence of implant head in palatal region resulting in an excess bulk of prosthesis causing discomfort. The difficulties to articulate and to perform oral hygiene are some of the common problems caused by the excess protrusion of the implant head. Placement of the zygomatic fixture also requires a well-trained surgeon and restorative dentist has to properly plan the fabrication of a full arch implant-supported prosthesis. Due to the limitation and intricacies of zygoma anatomy, it is difficult to treat patients pronounced concavity of the maxillary lateral wall. Among reported complications associated with zygomatic implants are sinusitis, oroantral fistula formation, periorbital and conjunctiva hematoma or edema, lip lacerations, pain, facial edema, temporary paresthesia, epistaxis, gingival inflammation and orbital injury [27]. Limited intraoperative visibility, complexity of anatomical structures and intricacies of zygoma curve has made this procedure a demanding task [36].
2.5.2 Indications and Contraindications
The role of the zygoma as an implant support structure is indicated in both partial and total maxillary edentulism with a high degree of resorption in the sinusal area [49, 50]. Patients with systemic diseases associated with atrophy of the posterior maxilla are also an indication for the use of zygomatic implants. Balshi and Wolfinger [51], reported a case of congenital ectodermal dysplasia successfully treated with bilateral zygomatic implants in combination with four conventional implants in the anterior region and two pterygoid implants. Peñarrocha et al. [44] published a case of ectodermal dysplasia, where two zygomatic fixtures were placed together with three implants in the anterior maxillary region. An upper complete prosthesis was screwed onto the implants and after 18 months of follow-up, the patient reported significant improvement in oral function and self-esteem.
The reconstruction of maxillary defects following tumour resection or due to maxillectomy is another situation where zygomatic implants have been applied [50]. In this particular case, zygomatic implants are used to anchor an obturator [14] and has been reported to provide increased prosthetic stability, thus improving the life quality of patients. There are several advantages when using zygomatic implants for maxillectomy. Firstly, early detection of postoperative recurrence is easier compared to the one with closed flap. Secondly, when a maxillary prosthesis is supposed to be placed at the midfacial region, zygomatic bone is generally preferred because of its thickness. This could also avoid contracture of the facial soft tissues in the early stages.
Schmidt et al. [52] carried out a retrospective analysis of patients rehabilitated with zygomatic implants following maxillary resection, and presented nine cases of partial or total maxillectomies rehabilitated using 28 zygomatic and 10 conventional implants. Although six zygomatic and three standard implants failed, they concluded that the combination of conventional and zygomatic implants could be used in patients with extensive resection of the maxilla. Landes [53] evaluated the level of satisfaction and indications for zygomatic implants in patients undergoing maxillary resection for various defects. Twelve patients received 28 zygomatic implants and 23 dental implants with a follow-up of 14–53 months. The success rate was 71 % and the quality of life was comparable to those with fixed prostheses over natural dentition.
There are also references to nasomaxillary reconstructions with the aid of zygomatic implants in patients with serious oronasal communications originating from tumour surgery. Bowden et al. [54] presented two cases of nasal reconstruction using implants anchored in the zygoma.
Contraindications of the treatment using zygomatic implants are similar to those applied in the placement of conventional dental implants [13]. Although the intervention in the maxillary sinus cavity could be noted, however, it is not significant to cause local infection. Patients with zygomatic implants may contract an upper respiratory tract infection, which might close to the maxillary ostium, resulting in sinusitis. When this occurs, the sinusitis can become chronic and it is necessary to surgically restore ventilation to the sinuses. There seems to be no increased risk of inflammatory reactions in normal nasal and maxillary mucosa in the regions where titanium implants passed through the mucosa [55].
2.5.3 Types of Surgical Approach
There are various types of surgical approach applicable in practice for the placement of zygomatic implants to treat severe edentulism maxilla patients such as intrasinus, sinus slot (Stella), extrasinus and extramaxillary approach since the zygomatic bone has been accepted as a possible implant-anchoring structure. The choice of the surgical technique is determined by the patient’s bone anatomy as well as technical skill of the clinician. The original surgical approach of intrasinus was defined by Brånemark System® in 1988, which involved the insertion of a long implant (between 35 and 55 mm) anchored to the zygomatic bone, following an intra-sinusal trajectory [56]. The intrasinus has been well-known as a traditional and the most common approach applied to treat atrophic maxillae associated with the use of zygomatic implants posteriorly, with or without additional retentions by conventional dental implants anteriorly.
In the intrasinus approach, the position of zygomatic implant body has to be maintained at the boundaries of the maxillary sinus causing the implant head to emerge in a more palatal aspect resulting in a bulky dental prosthesis (Fig. 2.5a) [27–29, 57]. Patients complaints regarding discomfort should be a cause for concern as this could be due to mechanical resistance of the prosthesis and may affect oral hygiene. Moreover, the penetration of implant body through the maxillary sinus needs to be considered as the condition of the soft tissues will be affected [41]. To perform the surgery via this approach, several protocols have to be followed as described by Brånemark System®. The following descriptions explain the procedures involved for the installation of zygomatic implant via intrasinus approach [58]:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses