The geriatric population comprises an increasing percentage of the overall population in the United States. Currently 13.6% of the population is age 65 or older, and 6% are 80 or older. It is predicted that by 2010 the geriatric population will exceed 39.4 million. The longevity and healthy lifestyle changes that many patients are experiencing will increase the need for oral and maxillofacial surgeons to treat their health needs. The importance of oral facial health within the geriatric sector has been given significant attention because there is a synergistic relationship between oral health and overall health. Advances in surgical and anesthetic techniques combined with sophisticated perioperative monitoring are factors that have contributed to an expanding number of older adults undergoing oral and maxillofacial surgery (OMFS). As such, surgical management becomes more challenging and the role of oral and maxillofacial surgeons becomes paramount. It involves clinical competency and the ability to evaluate carefully the pathophysiologic risk of co-morbid conditions/diseases in order to provide safe, expedient, and effective surgical care.
With the increase in life expectancy, the elderly population has become more active physically and socially, thereby predisposing them to accidents and traumatic events. Because the elderly often have multiple co-morbid conditions limiting their functional capacity to withstand the stress of surgery and postoperative recovery, they often require a greater degree of medical attention and longer hospital stays, especially if they are victims of a maxillofacial traumatic injury (see below).
This chapter discusses the treatment of the geriatric patient who has sustained maxillofacial trauma. The specific aims of this chapter are to:
- 1.
Give an epidemiologic overview of trauma in the geriatric population with an emphasis on the etiologies and patterns of maxillofacial trauma in this group of patients.
- 2.
Discuss the importance of preoperative risk assessment in the geriatric oral/maxillofacial surgical patient.
- 3.
Discuss the complexity of maxillofacial fractures in the elderly in order to assess the surgical indications, techniques of treatment for successful outcomes, and possible post-operative complications associated with each method of fixation.
- 4.
Provide future directions for treatment
EPIDEMIOLOGY OF TRAUMA IN THE GERIATRIC POPULATION
Trauma has been characterized as the seventh most common cause of death in people over the age of 65. Census data in 1990 revealed that over 4.5 million persons involved in a traumatic injury were older than 65 years of age. Over the past 15 years, these numbers have increased, with elderly patients representing over 29% of all trauma admissions. With the predicted increase in growth of the U.S. population, there is expected to be a concomitant increase to 40% of the geriatric trauma population by 2050. MacKenzie et al. predicted that the elderly will comprise up to 40% of the trauma population by the mid-twenty-first century.
Ironically, although advances in treatment/technology for cardiovascular diseases, diabetes, arthritis, and pulmonary disease are at the forefront, traumatic injuries within the geriatric population are increasing concomitantly with healthiness of lifestyles. More active lifestyles, as well as increasing longevity, lend themselves to an increased risk for injury, specifically as a result of the aging process. Age-related deterioration of sight and hearing, as well as coordination of musculoskeletal reflexes, reduces the elder’s ability to react to environmental stimuli. They are more likely to be responsible for accidents caused by age-related decreases in auditory and visual acuity as well as slower reaction time.
With the increasing number of elderly trauma patients comes increased need for care, frequent hospital admissions, projected longer length of stay, an increased risk of complications, subsequent hospitalizations/disabilities from traumatic injuries, and decreased survival compared with their younger cohorts. Although the population-based death rate for trauma appears greatest for victims over the age of 65, patients aged 80 or greater were most susceptible to such unfavorable outcomes. Reasons for such a disparity include more severe overall cardiac and pulmonary injury, ventilator dependence, and postoperative cardiac mishaps, as well as more severe head and neck trauma (see following section on maxillofacial trauma). Retrospective studies, using hospital database chart reviews, have examined the predictor variables of age and severity of illness in geriatric surgical patients on outcome and length of stay. When age and severity of illness are compared, the severity of illness provides a better predictor of surgical outcome and length of hospital stay. Gray et al. used a retrospective chart review of a trauma registry in order to (1) evaluate patients between the ages of 56 and 91 who sustained multiple trauma, including maxillofacial injuries, and (2) develop a model that predicts risk variables to measure the outcome of length of hospital stay. The predictive variables of infection, respiratory compromise, and hematological complications were statistically significant predictors of length of stay and unsuccessful surgical outcome after a traumatic injury.
Etiologies of trauma in the above studies, as well as other studies, include motor vehicle trauma, falls, and assaults ( Table 21-1 ). The leading cause of accidental death in the elderly aged 65 to 74 was motor vehicular trauma (MVA). MVA was the second leading cause of fatality, following falls, in those aged 75 or greater. Ironically, although the elderly drive fewer miles, they are involved in more accidents per mile. The cause of accident is more often due to age-related decreases in visual and auditory acuity as opposed to speed.
| Age >65 | ||
|---|---|---|
| Mechanism of Injury | % Relative Frequency | % Case Fatality |
| Fall | 40.6 | 11.7 |
| Motor vehicle accident | 28.2 | 20.7 |
| Pedestrian hit | 10.0 | 32.6 |
| Stab wound | 2.6 | 17.3 |
| Gunshot wound | 5.5 | 52.1 |
| Motorcycle | 0.4 | 11.8 |
| Other | 7.0 | 13.8 |
| Unknown | 0.3 | 19.0 |
| Total | 100 | |
* Adapted from Santora TA, Schinco MA, Trooskin SZ: Management of trauma in the elderly patient. Surg Clin North Am 1994;74(1):163-86.
The second most common etiology of trauma in the elderly is falls. Falls account for the sixth leading cause of death in people over the age of 65 years and first in ages greater than 75. The etiology of falls is multifactorial and includes acute illnesses such as transient ischemic attacks (TIAs), stroke, and pneumonia as well as chronic illnesses, cognitive impairment, female gender, low serum CBC, low body mass index, curbs, stairways, and improper lighting. Half of these injuries result in fractures, with one sixth resulting in death. Figures 21-1 through 21-6 illustrate the case of an elderly woman who fell on the step between her patio and her house.
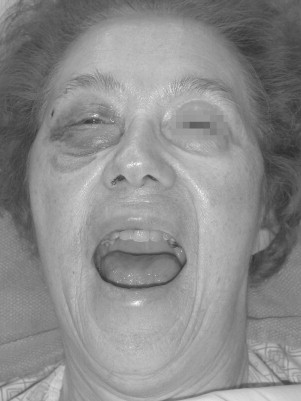
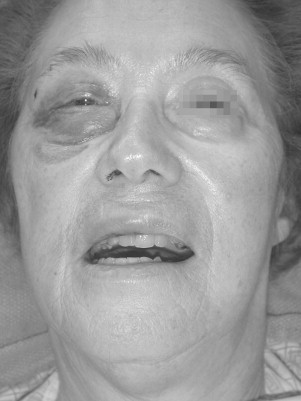
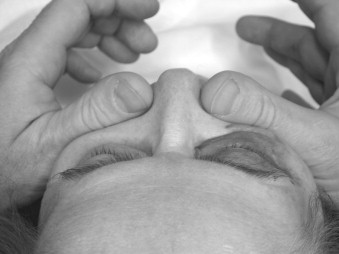
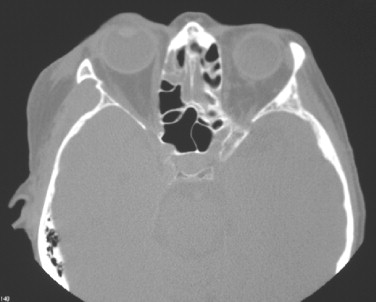
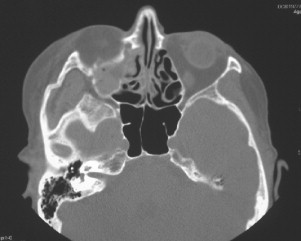
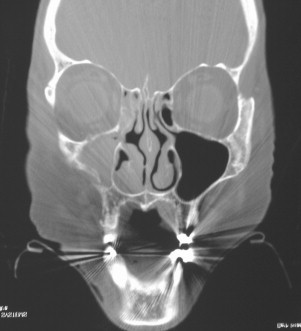
Falls may occur as a direct result of assault (e.g., elder abuse). It is estimated that 4-6% of all elderly patients are victims of some form of abuse, whether it be physical or mental. There is a growing concern about elder abuse. Studies have demonstrated ways of recognizing and dealing with abuse in older people. The oral and maxillofacial surgeon is in a pivotal position to identify and intervene. Other etiologies of trauma include recreational injury, suicide, and nursing home trauma caused by a shortage of nurses.
MAXILLOFACIAL TRAUMA IN THE ELDERLY
EPIDEMIOLOGY
Epidemiological databases of craniomaxillofacial trauma indicate that young males are the predominant victims of maxillofacial trauma. The incidence rate of facial trauma, however, is increasing in the elderly. Geriatric patients represent approximately over 10% of all maxillofacial trauma. This is a reflection of more active healthy lifestyles (see above), as well as the elderly being characterized as easy targets for assault. Retrospective chart reviews have characterized patterns of age, gender, and fracture location among different populations of patients ( Table 21-2 ). The predominant pattern of fracture injury was seen in the midface, evenly distributed among the nasal, zygomaticomaxillary complex (ZMC), and orbits, followed by skull fractures and mandible fractures. The pattern of mandible fractures was primarily in the sub-condylar region and parasymphyseal location. Fractures of the mandible occur with a greater frequency in the elderly because of etiology and age-related changes in anatomy (see below).
| Literature | n | Age | % Fracture: Upper/Midface | % Fracture: Mandible | Location of Study |
|---|---|---|---|---|---|
| Gerbino et al. (1999) | 222 | 60-91 | 74.6% | 25.4% | Italy |
| Eyrich et al. (1997) | 34 | 70s | Not Available | 100% | Switzerland |
| Goldschmidt et al. (1995) | 109 | 60-79 | 69.8% | 27.5% | CT, USA |
| Chew and Edmundson (1996) | 22 | 65-88 | 49% | 50% | United Kingdom |
| Rehman and Edmundson (2002) | 42 | 65-90 | 45% | 19% | United Kingdom |
| Gray et al. (2002) | 196 | 56-91 | 83% | >17% | OR, USA |
| Fasola et al. (2003) | 53 | >65 | 9% | 91% | Nigeria |
The treatment of maxillofacial injuries reported by the previously mentioned studies varied. Gray et al. operated on 47% of their midface surgical patients, 75% by ORIF, and 25% by closed reduction. Goldschmidt et al. treated 49% surgically. Gerbino et al. treated 50% with ORIF and 9% with closed reduction out of a total of 51% fractures treated. This group further concluded that surgical intervention is not always necessary because of “.…physiologic, psychologic and social changes brought about by the aging process.” These investigators indicated that there was a significant reluctance by the elderly to accept surgical intervention unless a significant functional deficit would ensue. This is in contrast to younger surgical patients who valued aesthetic reconstructions as a major concern. The overall importance of restoring form, function, and occlusion was paramount in all groups surgically treated among all studies.
A 64-year-old female after a fall with resulting fracture of right ZMC
AGING OF THE FACE AND NECK
The oral and maxillofacial surgeon is well versed in the anatomic and physiologic characteristics of the aging process. Morphologic alterations lead to atrophy of the subcutaneous fat and a slow degeneration of the skin’s elastic and collagen network. Gradual resorption of the facial skeleton may occur. This results in a loss of skin tone and elasticity and relatively loose cervicofacial skin cover. When atrophy of subcutaneous and buccal fat accompanies these changes, the aging face reveals marked hollowing over the cheeks.
Hard tissue changes during the aging process are coincident with failing health. There are redistributions in weight and body proportions caused by decreases in proteins and adipose tissue. Airway morphology is altered with anatomic aging of the cervical spine and neck. In addition, osteoporosis remains a significant independent risk factor for the development of facial fractures The potential for osteosynthesis after fracture reduction may be hampered by these deficiencies depending upon the technique applied (see the section on non-surgical/surgical approaches for reduction of maxillofacial fractures). The aging process can also affect the temporomandibular joint (TMJ). There is loss of elasticity and hardening of the articular disc and capsular ligament, thinning of the articular disc, fibrosis of the articular space, and flattening of the articular surfaces. Complaints can include joint clicking, dislocation, subluxation, and fracture of the articular head with subsequent decrease in mouth opening. In addition, tooth loss and bone resorption contributes to degenerative joint disease, as well as an alteration in the vertical dimension and the dynamics of TMJ function that are difficult to overcome.
AGING AND WOUND HEALING
Studies with animal models and humans have suggested that mechanisms of wound healing become compromised during aging. The inflammation, proliferation, and timing of healing slows down. There is a delay in epithelialization, angiogenesis, and fibroblast proliferation. The ability of fibroblasts to secrete soluble collagen and elastin is decreased with concomitant dysfunction of these two proteins as viable building blocks in the healing process. The effect of age on the rate of wound healing does not seem to be related to the cell count in the repair tissue but rather to the functional capacity of the cells. The equilibrium between synthesis and decomposition of the connective tissue becomes less congruent with age. In older patients, there may be a greater amount of collagen deposited at the end of wound healing, but this may not be as well organized as in younger patients. These concepts must be kept in mind in managing soft tissue injuries, such as the dog bite wound in the patient pictured in Figures 21-7 through 21-9 .
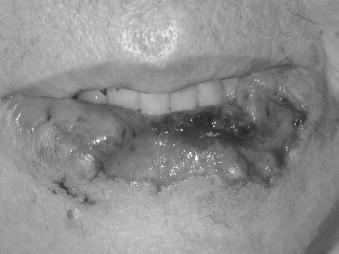
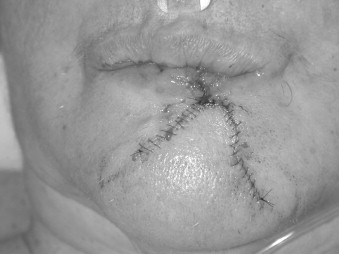
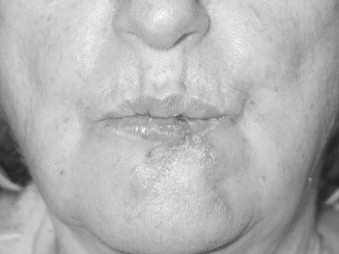
A female in her 60s after a dog bite with significant soft tissue avulsion of lower lip repaired with modified ABBE technique
The ability to mount an immunologic response ages as the individual does. Quantitative and qualitative changes in immune cell production and activity are significantly altered, especially T-cell and B-cell production. With the decrease in lymphoid cells, there is an associated decrease in cell-mediated and humoral responses to specific antigenic stimuli. The latter significantly compromise an individual’s ability to combat infection and heal properly. As such, the age-associated changes described above pose a significant dilemma for the oral and maxillofacial surgeon. Concerns for compromised wound healing are compounded by concurrent systemic aging, such as medical conditions, cardiovascular disease, organ perfusion, nutritional status, cognitive skills, endocrine imbalances, social habits, and musculoskeletal deterioration.
MAXILLOFACIAL TRAUMA IN THE ELDERLY
EPIDEMIOLOGY
Epidemiological databases of craniomaxillofacial trauma indicate that young males are the predominant victims of maxillofacial trauma. The incidence rate of facial trauma, however, is increasing in the elderly. Geriatric patients represent approximately over 10% of all maxillofacial trauma. This is a reflection of more active healthy lifestyles (see above), as well as the elderly being characterized as easy targets for assault. Retrospective chart reviews have characterized patterns of age, gender, and fracture location among different populations of patients ( Table 21-2 ). The predominant pattern of fracture injury was seen in the midface, evenly distributed among the nasal, zygomaticomaxillary complex (ZMC), and orbits, followed by skull fractures and mandible fractures. The pattern of mandible fractures was primarily in the sub-condylar region and parasymphyseal location. Fractures of the mandible occur with a greater frequency in the elderly because of etiology and age-related changes in anatomy (see below).
| Literature | n | Age | % Fracture: Upper/Midface | % Fracture: Mandible | Location of Study |
|---|---|---|---|---|---|
| Gerbino et al. (1999) | 222 | 60-91 | 74.6% | 25.4% | Italy |
| Eyrich et al. (1997) | 34 | 70s | Not Available | 100% | Switzerland |
| Goldschmidt et al. (1995) | 109 | 60-79 | 69.8% | 27.5% | CT, USA |
| Chew and Edmundson (1996) | 22 | 65-88 | 49% | 50% | United Kingdom |
| Rehman and Edmundson (2002) | 42 | 65-90 | 45% | 19% | United Kingdom |
| Gray et al. (2002) | 196 | 56-91 | 83% | >17% | OR, USA |
| Fasola et al. (2003) | 53 | >65 | 9% | 91% | Nigeria |
The treatment of maxillofacial injuries reported by the previously mentioned studies varied. Gray et al. operated on 47% of their midface surgical patients, 75% by ORIF, and 25% by closed reduction. Goldschmidt et al. treated 49% surgically. Gerbino et al. treated 50% with ORIF and 9% with closed reduction out of a total of 51% fractures treated. This group further concluded that surgical intervention is not always necessary because of “.…physiologic, psychologic and social changes brought about by the aging process.” These investigators indicated that there was a significant reluctance by the elderly to accept surgical intervention unless a significant functional deficit would ensue. This is in contrast to younger surgical patients who valued aesthetic reconstructions as a major concern. The overall importance of restoring form, function, and occlusion was paramount in all groups surgically treated among all studies.
A 64-year-old female after a fall with resulting fracture of right ZMC
AGING OF THE FACE AND NECK
The oral and maxillofacial surgeon is well versed in the anatomic and physiologic characteristics of the aging process. Morphologic alterations lead to atrophy of the subcutaneous fat and a slow degeneration of the skin’s elastic and collagen network. Gradual resorption of the facial skeleton may occur. This results in a loss of skin tone and elasticity and relatively loose cervicofacial skin cover. When atrophy of subcutaneous and buccal fat accompanies these changes, the aging face reveals marked hollowing over the cheeks.
Hard tissue changes during the aging process are coincident with failing health. There are redistributions in weight and body proportions caused by decreases in proteins and adipose tissue. Airway morphology is altered with anatomic aging of the cervical spine and neck. In addition, osteoporosis remains a significant independent risk factor for the development of facial fractures The potential for osteosynthesis after fracture reduction may be hampered by these deficiencies depending upon the technique applied (see the section on non-surgical/surgical approaches for reduction of maxillofacial fractures). The aging process can also affect the temporomandibular joint (TMJ). There is loss of elasticity and hardening of the articular disc and capsular ligament, thinning of the articular disc, fibrosis of the articular space, and flattening of the articular surfaces. Complaints can include joint clicking, dislocation, subluxation, and fracture of the articular head with subsequent decrease in mouth opening. In addition, tooth loss and bone resorption contributes to degenerative joint disease, as well as an alteration in the vertical dimension and the dynamics of TMJ function that are difficult to overcome.
AGING AND WOUND HEALING
Studies with animal models and humans have suggested that mechanisms of wound healing become compromised during aging. The inflammation, proliferation, and timing of healing slows down. There is a delay in epithelialization, angiogenesis, and fibroblast proliferation. The ability of fibroblasts to secrete soluble collagen and elastin is decreased with concomitant dysfunction of these two proteins as viable building blocks in the healing process. The effect of age on the rate of wound healing does not seem to be related to the cell count in the repair tissue but rather to the functional capacity of the cells. The equilibrium between synthesis and decomposition of the connective tissue becomes less congruent with age. In older patients, there may be a greater amount of collagen deposited at the end of wound healing, but this may not be as well organized as in younger patients. These concepts must be kept in mind in managing soft tissue injuries, such as the dog bite wound in the patient pictured in Figures 21-7 through 21-9 .
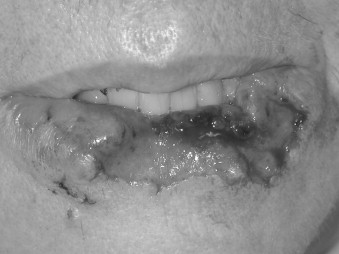
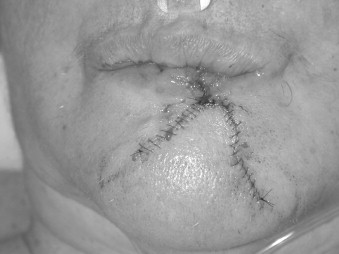
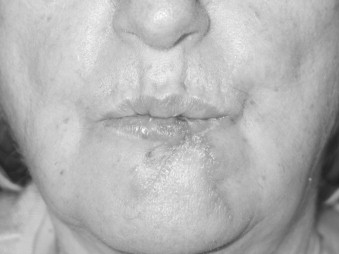
A female in her 60s after a dog bite with significant soft tissue avulsion of lower lip repaired with modified ABBE technique
The ability to mount an immunologic response ages as the individual does. Quantitative and qualitative changes in immune cell production and activity are significantly altered, especially T-cell and B-cell production. With the decrease in lymphoid cells, there is an associated decrease in cell-mediated and humoral responses to specific antigenic stimuli. The latter significantly compromise an individual’s ability to combat infection and heal properly. As such, the age-associated changes described above pose a significant dilemma for the oral and maxillofacial surgeon. Concerns for compromised wound healing are compounded by concurrent systemic aging, such as medical conditions, cardiovascular disease, organ perfusion, nutritional status, cognitive skills, endocrine imbalances, social habits, and musculoskeletal deterioration.
MEDICAL EVALUATION OF THE GERIATRIC MAXILLOFACIAL TRAUMA PATIENT
Medical history-taking for peri-operative assessment of the elderly with maxillofacial injuries requires modifications as compared with younger OMFS patients. As such, the perioperative assessment of the elderly patient should begin the moment he or she enters the office. A first impression of the patient’s physical appearance, gait, posture, attitude, and behavior should be noted. Many practitioners find inconsistencies when history forms are filled out in the waiting area and then reviewed prior to treatment planning. Medical consultations must be judiciously undertaken for patients both whose medical histories are uncertain as well as when the physical assessment uncovers an untreated medical problem. A thorough pre-operative work-up includes nutritional status, social and cognitive history, medications, laboratory profile and physical examination.
NUTRITION AND FLUID ELECTROLYTES
Nutritional deficits of a multi-factorial etiology are most prevalent in the elderly surgical patient. Risk factors for malnutrition are either macronutrient (protein, fats, and carbohydrates) or micronutrient (vitamins and minerals) in origin. In addition, malnutrition can be “iatrogenic” because of adverse drug-nutrient interactions causing a depletion of daily needed elements as a trade-off for treatment of systemic illnesses. Peri-operative risk assessment of nutritional status requires clinical, biochemical, anthropometrics, and dietary monitoring strategies. Specifically, rapid weight loss greater than 10% should be of concern. Laboratory panels should be ordered to characterize the severity of malnutrition. Protein energy malnutrition (PEM) is most common and arises from a deficit in serum albumin. Post-operative sequelae in patients with PEM include poor wound healing, increased wound infection, and risk of mortality. Albumin levels of less than 3.2 g/dL in hospitalized older persons were shown to be highly predictive of subsequent mortality. Cholesterol levels of less than 160 mg/dL in a frail elderly person have also been shown to be a risk marker for increased mortality. Complete blood cell counts should include a total lymphocyte count (<1500/mm ) and anergy skin testing. Although the latter have not proven to be useful nutritional markers in older persons, these predictors must be considered since the elderly population often suffers from opportunistic infections and delayed healing caused by chronic diseases such as diabetes and peripheral vascular disease.
Specific nutritional supplements for proteins and kilocalorie replacement should be prescribed pre-operatively and during the peri-operative period. Common protein supplement recommendations include Ensure/Ensure Plus (Abbott Laboratories, Abbott Park, Illinois) and Sustacal (Mead Johnson, Evansville, IN) along with resumption of a well-balanced diet as tolerated. Carnation Instant Breakfast offers a broad range of flavors and more acceptable taste to lactose-tolerant individuals. Post-operative laboratory analyses using the criteria above will allow for immediate resolution of any physiologic imbalances that can impede surgical recovery. Post-surgical care should include nutritional counseling with dietary suggestions that can be easily understood and reinforced at follow-up visits. Post-operative planning includes a team approach with the general dental practitioner since loss of teeth or poor-fitting dentures further significantly contribute to both malnutrition and depression with resultant weight loss in these patients.
Fluid and electrolyte balance plays a pivotal role in peri-operative surgical risk assessment. With aging there are increases in total body fat and decreases in total body water. Both can contribute to an imbalance in fluids and electrolytes. Decreased urinary concentrating ability; limitations in excretion of water, sodium, and potassium; and “iatrogenic injury” with intravenous fluid overload can further exacerbate trauma to tissues and alter the hemodynamic state of the patient. Furthermore, impaired thirst perception; decreased glomerular filtration rate; and alterations in hormonal levels of antidiuretic hormone, atrial natriuretic peptide, and aldosterone can initiate and/or exacerbate the systemic neurologic and cardiovascular complications of hyperkalemia, hypernatremia, and volume depletion, as well as the complication of postoperative delirium (see below).
Strategies to prevent imbalances include peri-operative measurements of electrolytes, serum urea nitrogen, serum creatinine, and creatinine clearance, as well as a baseline urinalysis. Normal fluid management should be maintained in a range of 1.5-2.0 L/day with an average urine output of 20-30 mL/hr. Elderly patients who have undergone uncomplicated dentoalveolar surgery are encouraged to resume oral intake as soon as possible in order to maintain fluid and electrolyte balance. Patients who may vomit or develop severe diarrhea after surgery should also be monitored since metabolic acidosis and/or alkalosis can precipitate the adverse events of delirium and cardiac dysrhythmias. Patients who are in the post-operative phase after general anesthesia must be monitored for ongoing fluid losses from all sites, including insensible losses. Adverse drug effects from postoperative “polypharmaceutical administration” can also alter salt and water balance. The adequacy of free-water replacement should be guided by the serum electrolyte concentration gradients with judicious monitoring to prevent these events. Dehydration is seen more often than over-hydration and it may be wise to parenterally maintain fluids and electrolytes and to monitor vital signs both pre- and post-operatively.
SOCIAL HISTORY
Social history and lifestyle issues, especially use of tobacco and alcohol need to be documented. Cessation of smoking can be accomplished even in the geriatric patient. Studies have suggested that elderly patients should refrain from tobacco use up to 6 months prior to any surgical procedures. Alcohol consumption has been associated with complex changes in cerebral vasculature and structure in older adults. Often alcohol abuse is misdiagnosed and often the cause of falls and accidents. Sometimes, intoxication in the elderly occurs as a result of the combination of previously customary amounts of alcohol in combination with newly prescribed medicines. It is also associated with severe malnutrition, poor wound healing, and decreased immune-competence. The role of alcohol consumption and the incidence of dementia are less clear but often considered in the elderly. Studies have suggested that participants who drank no alcohol at midlife and those who drank alcohol frequently were both twice as likely to have mild cognitive impairment in old age as those participants who drank alcohol infrequently. Pre-operative risk assessment with the cap analysis gene expression (CAGE) protocol or use of lab tests, as stated previously, will allow the surgeon to determine if patients need any prophylaxis against the complications of alcoholic withdrawal during the peri-operative period.
COGNITIVE EVALUATION AND INFORMED CONSENT
Cognitive assessment and the ability to give informed consent are of major concern when evaluating the geriatric patient for surgery. Simple questions can evaluate the patient’s orientation to time and place and the ability to recall information, perform simple calculations, or understand speech. The doctor should speak directly to the patient when reviewing the health history and should make sure the wording is understood since many patients will have issues of hearing and visual impairments. Many patients will not readily admit that they did not understand a question. Although the practitioner may consider modifying his or her history-taking by including family members and caregivers, it is important to remember that even the cognitively impaired patient can provide useful information if the questions are presented in a concrete and simple manner. Decision capacity should be predicated upon formal mental status criteria in order to judge whether the patient is capable of receiving informed consent. Remember that one can be lucid during specific periods of time and not others (sundowning) and still be able to give informed consent. If the patient cannot provide informed consent, the alternative choices include written documents for power of attorney by chosen executors and/or power of living wills.
MEDICATIONS/OVER-THE-COUNTER DRUGS
The physiologic and pathologic changes occurring in the older patient can lead to adverse events with respect to medications taken. Blood flow to the liver decreases with age, and the bioavailability of drugs can be altered depending upon their metabolic pathway. Renal clearance is significantly altered with age because of the morphological decrease in mass associated with decreased tubular function and glomerular filtration rate. Other systemic factors can affect the distribution of a drug in the elderly such as decreased cardiac output, increased peripheral vascular resistance, and increases in percentage of adipose tissue in the body. Other organ function can be affected, such as the digestive system, as can gastric acid production and gastric emptying time. It is not unusual for the patient to be taking from four to eight other medications depending upon his or her degree of chronic illnesses. The surgeon must be judicious in cataloguing of all drugs prior to beginning treatment. Patients may often not remember the names of all the medications they are taking, and a medical consult will be necessary to obtain an accurate list. The most common types of medications that the elderly take are over-the-counter (OTC) medications for pain and other chronic ailments.
Data have shown that only 11% of physicians routinely ask about OTC use during primary care visits. It is important to discuss the use of nonprescription medications with the elderly since adverse effects can be seen when combined with any prescribed agents during the peri-operative period. Many geriatric patients forget to write the type and number of OTC medications on the history form. The most common ailment for which 66% of the elderly use OTC drugs is arthritis, and the most medications used are acetaminophen, aspirin, or other NSAIDs. Other OTC drugs used on a daily basis include a variety of gastrointestinal agents such as antacids and H 2 blockers, both of which can adversely interfere with medications for cardiovascular function (i.e., anticoagulants and anti-arrhythmia agents such as digoxin, lidocaine, and procainamide). Good documentation of current medicines will avoid any undue drug–drug interactions.
PERI-OPERATIVE RISK ASSESSMENT OF CO-MORBID SYSTEMIC DISEASE
Table 21-3 lists the common chronic illnesses seen within the geriatric population. Each disease has a characteristic pathophysiology that can compromise the surgical management of facial fractures in the elderly because of complications during the peri-operative and post-operative period of treatment.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


