Complete and accurate evaluation of a patient with a dentofacial deformity must include assessment of the transverse dimension. Unfortunately, few practitioners adequately evaluate the transverse dimension; transverse maxillomandibular discrepancy often remains undiagnosed. When a transverse maxillomandibular discrepancy exists, adult patients traditionally have been treated with orthodontic expansion or a segmental maxillary osteotomy, frequently leading to transverse maxillary instability and relapse following orthodontic appliance removal.
Orthopedic or rapid maxillary expansion (RME) is a technique that is used to treat transverse maxillomandibular discrepancy. If used in the correct patient population, this technique is predictable and stable for the correction of transverse maxillomandibular discrepancy. RME was first described in 1860 by Angell, who used an expansion screw attached to the maxillary first bicuspids of a 14-year-old girl. The technique was not commonly accepted or used. Haas reintroduced it in 1965. The procedure is of limited benefit in mature teenage and adult patients because with aging, the maxillary articulations become increasingly resistant to expansion. Techniques of surgically assisted maxillary expansion (SAME) have been developed to overcome this age limitation. The SAME procedure is, in essence, a combination of distraction osteogenesis and controlled soft tissue expansion. Discussion of SAME often is confusing because various combinations of maxillary, pterygopalatine, lateral, nasal, septal, and palatine osteotomies have been performed, in keeping with the surgeon’s theory of where resistance to expansion is located. The purposes of this chapter are to describe the clinical and radiographic evaluation of the transverse dimension in patients with dentofacial deformity, and to present the indications for SAME and an anatomically based SAME technique.
INCIDENCE AND ORIGIN OF TRANSVERSE MAXILLARY DEFICIENCY
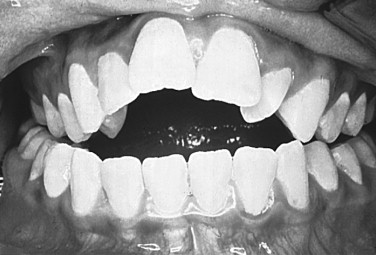
The incidence of transverse maxillary deficiency is estimated to be between 8% and 18% among patients who present for orthodontic consultation. The origin of transverse maxillary deficiency is multifactorial, and causes may be congenital, developmental, traumatic, or iatrogenic. An example of a developmental origin is the deformity caused by a long-term thumb-sucking habit ( Figure 10-1 ). This deformity includes a bilateral posterior crossbite and a high arched palate with apertognathia. After cessation of the oral habit, the apertognathia often resolves owing to passive eruption of the anterior maxillary dentition. However, the transverse maxillary deficiency does not routinely resolve, and correction requires orthodontic and/or surgical intervention. An example of an iatrogenic cause of transverse maxillary deficiency is the restricted growth caused by palatal scar formation in patients with cleft palate following surgical correction with a palatoplasty procedure.
DIAGNOSIS OF TRANSVERSE MAXILLARY DEFICIENCY
Accurate diagnosis and treatment of transverse maxillary deficiency are essential to long-term stability following correction of any dentofacial deformity that includes a transverse discrepancy. However, diagnosis of transverse maxillary deficiency may be difficult because minimal facial soft tissue changes are associated with isolated transverse maxillary hypoplasia. These soft tissue changes generally are limited to paranasal hollowing and a narrowed alar base. Deepening of the nasolabial folds and zygomatic deficiency also may be present, depending on the degree of associated zygomaticomaxillary hypoplasia. In contrast, isolated anteroposterior or vertical skeletal deformities are easier to diagnose because often, they have obvious associated facial soft tissue findings. Consequently, the transverse deformity often is not diagnosed when sagittal and vertical deformities exist concomitantly. Complete diagnosis of this deformity must include both clinical and radiographic evaluation.
CLINICAL EVALUATION
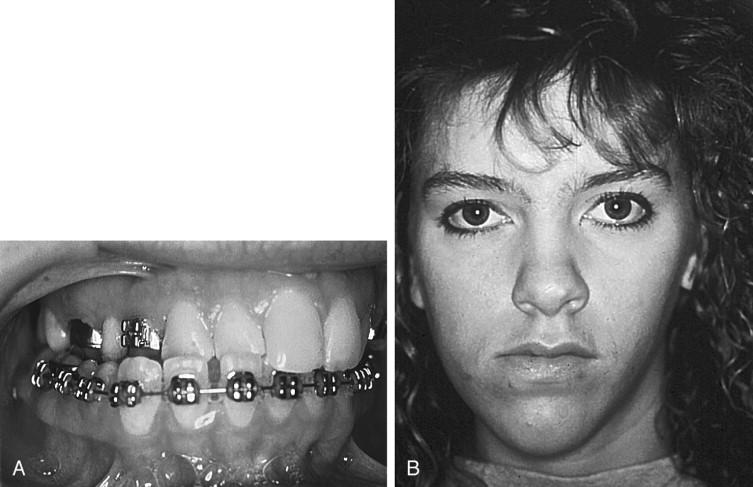
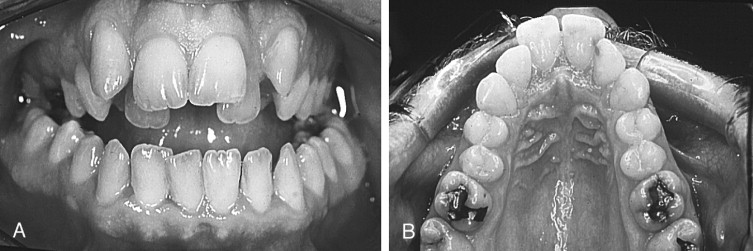
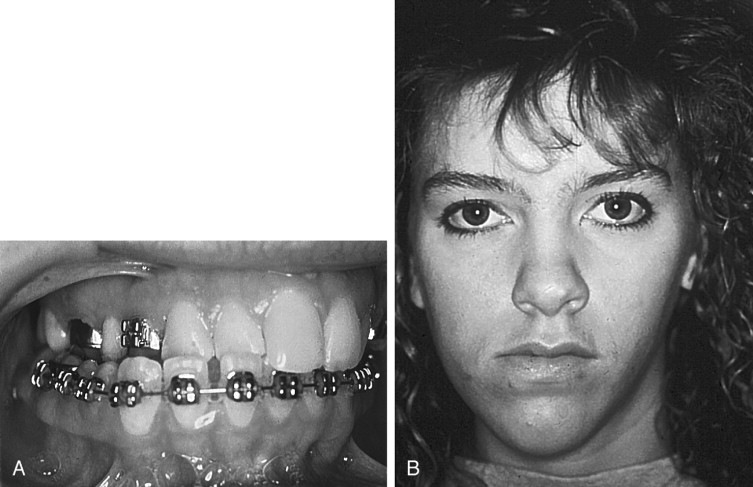
Determination of the existence and extent of a transverse discrepancy and differentiation between the skeletal and dental components of the deformity must be achieved before surgery is contemplated. Several clinical indicators of transverse maxillary deficiency are noted, including unilateral or bilateral posterior crossbite; crowded, rotated, and palatally or buccally displaced teeth; a narrow and tapering maxillary arch form, described as hourglass shaped; and a high, narrow palatal arch ( Figure 10-2 ). When a crossbite is evaluated in an adult patient, a distinction must be made between a dental crossbite and a true skeletal crossbite. Dental crossbites may be treated with orthodontic therapy alone. Jacobs and colleagues stated that if a crossbite involves more than one or two teeth, it is probably skeletal in nature. Depending on the degree of transverse discrepancy, skeletal crossbite can present as unilateral or bilateral. Unilateral skeletal crossbites are less common and usually are associated with a mild to moderate transverse discrepancy and possibly a functional jaw shift ( Figure 10-3 ). Bilateral crossbites are more common and are associated with a moderate to severe transverse discrepancy.
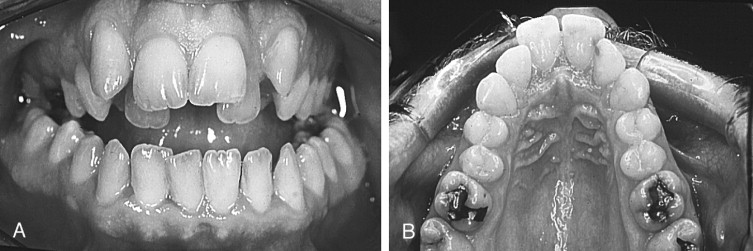
Skeletal crossbites result from one of the following maxillomandibular combinations: (1) narrow maxilla and normal mandible, (2) normal maxilla and wide mandible, or (3) narrow maxilla and wide mandible. Correction of the transverse dimension in a patient with a narrow maxilla and a wide mandible is most difficult and is most susceptible to relapse. “This is because the mandible cannot effectively be narrowed in the anterior region except through extraction and osteotomy, often mandating correction of the remaining transverse discrepancy in the maxilla.”
The skeletal deformities that are most commonly associated with transverse maxillary deficiency involve maxillary vertical and anteroposterior hypoplasia. This is so because, as the maxilla grows, it translates down and forward and also widens. Therefore, if transverse maxillary hypoplasia is present, vertical and/or sagittal hypoplasia is often present as well. Vertical maxillary excess is commonly accompanied by transverse deficiency. Other dentofacial deformities associated with transverse maxillary deficiency include mandibular prognathism or mandibular sagittal deficiency, apertognathia, and repaired cleft palate.
RADIOGRAPHIC EVALUATION
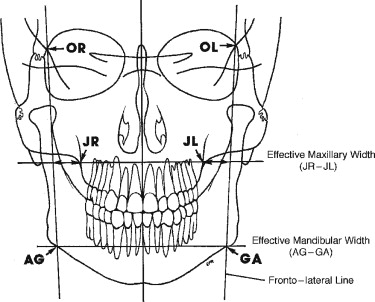
A standard posterior-anterior (PA) cephalogram is the radiograph of choice for identification and evaluation of a transverse discrepancy. This radiographic technique allows for superimposition of radiographs, comparison of linear measurements, and evaluation of radiographs over time. Ricketts developed the Rocky Mountain analysis and established relative norms by using specific radiographic landmarks and measurements to analyze transverse discrepancies between the maxilla and the mandible ( Figures 10-4 and 10-5 ). These landmarks have been modified slightly and include JR (jugale right), JL (jugale left), AG (antegonion right), GA (antegonion left), OR (orbitale right), and OL (orbitale left). With use of these landmarks, it is possible to determine the effective maxillary width, effective mandibular width, and frontolateral facial lines. The effective maxillary width is the width of the maxilla between the points JL and JR, which represents the jugal process at the intersection of the maxillary tuberosity and the zygomatic buttress. The effective mandibular width is the width of the mandible between the AG and the GA, which are the bilateral points at the inferior margin of the antegonial protuberance, below the antegonial trihedral area. The frontolateral facial lines are the lateral lines constructed from OR and OL (representing the intersection of the orbits with the middle cranial fossa) to the points AG and GA, respectively.
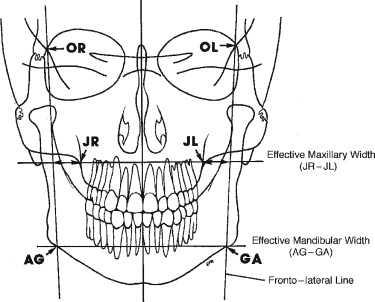
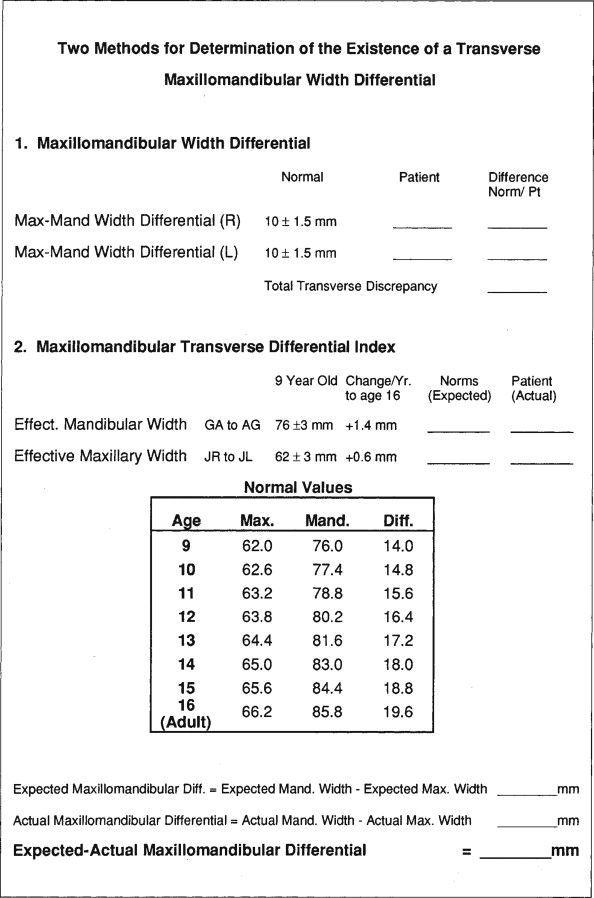
With these cephalometric landmarks, it is possible to determine the maxillomandibular width differential and the maxillomandibular transverse differential index for quantification of the transverse maxillary discrepancy. The maxillomandibular width differential is the distance (in millimeters) measured from the frontolateral facial line to JL and JR, respectively, along a line from the frontolateral facial lines through JR and JL. This measurement is calculated independently for each side and is compared with a normal value of 10 ± 1.5 mm. If this value is greater than 10 mm, a transverse discrepancy between the maxilla and the mandible exists. Values greater than 10 mm on each side are summed to quantify the total transverse deficiency. This technique is useful in determining the total discrepancy and discerning whether a greater deficiency or excess is present on one side or the other. However, this differential does not elucidate in which jaw the discrepancy exists and may be misinterpreted when mandibular asymmetry is present. The maxillomandibular transverse differential index is the age-specific expected maxillomandibular difference minus the actual measured maxillomandibular difference. The expected maxillomandibular difference is the age-appropriate expected AG-GA distance minus the age-appropriate expected JR-JL distance. The actual maxillomandibular difference is the actual AG-GA measurement minus the actual JR-JL measurement. In the adult patient, a maxillomandibular transverse differential index greater than 5 mm suggests the need for surgical expansion. If the differential index is less than or equal to 5 mm, orthodontic or orthopedic expansion may effectively correct the transverse discrepancy. As well as quantifying the total discrepancy, this method allows for the identification of which jaw is deficient or excessive, in that actual values can be compared with normal values. Normal values have been suggested only for Caucasians, and these values should not be considered normal values for other races. A recent abstract suggests that differences may be seen among races (e.g., African American and Caucasian) and between genders. Therefore, separate normal values should be established by gender and race.
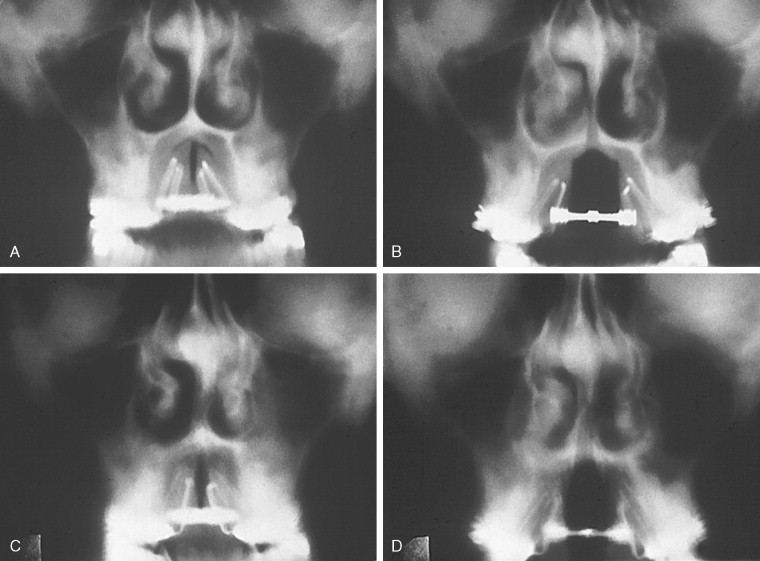
Alternative imaging modalities to the standard PA cephalogram include frontal tomography and computed tomography ( Figure 10-6 ). These imaging modalities allow for accurate calculation of any transverse discrepancy, but they are not cost effective and they deliver an unacceptable dose of radiation to the patient. Also, a cephalometer is readily available in most orthodontic and surgical offices, making the PA cephalogram easy to obtain.
DIAGNOSIS OF TRANSVERSE MAXILLARY DEFICIENCY
Accurate diagnosis and treatment of transverse maxillary deficiency are essential to long-term stability following correction of any dentofacial deformity that includes a transverse discrepancy. However, diagnosis of transverse maxillary deficiency may be difficult because minimal facial soft tissue changes are associated with isolated transverse maxillary hypoplasia. These soft tissue changes generally are limited to paranasal hollowing and a narrowed alar base. Deepening of the nasolabial folds and zygomatic deficiency also may be present, depending on the degree of associated zygomaticomaxillary hypoplasia. In contrast, isolated anteroposterior or vertical skeletal deformities are easier to diagnose because often, they have obvious associated facial soft tissue findings. Consequently, the transverse deformity often is not diagnosed when sagittal and vertical deformities exist concomitantly. Complete diagnosis of this deformity must include both clinical and radiographic evaluation.
CLINICAL EVALUATION
Determination of the existence and extent of a transverse discrepancy and differentiation between the skeletal and dental components of the deformity must be achieved before surgery is contemplated. Several clinical indicators of transverse maxillary deficiency are noted, including unilateral or bilateral posterior crossbite; crowded, rotated, and palatally or buccally displaced teeth; a narrow and tapering maxillary arch form, described as hourglass shaped; and a high, narrow palatal arch ( Figure 10-2 ). When a crossbite is evaluated in an adult patient, a distinction must be made between a dental crossbite and a true skeletal crossbite. Dental crossbites may be treated with orthodontic therapy alone. Jacobs and colleagues stated that if a crossbite involves more than one or two teeth, it is probably skeletal in nature. Depending on the degree of transverse discrepancy, skeletal crossbite can present as unilateral or bilateral. Unilateral skeletal crossbites are less common and usually are associated with a mild to moderate transverse discrepancy and possibly a functional jaw shift ( Figure 10-3 ). Bilateral crossbites are more common and are associated with a moderate to severe transverse discrepancy.
Skeletal crossbites result from one of the following maxillomandibular combinations: (1) narrow maxilla and normal mandible, (2) normal maxilla and wide mandible, or (3) narrow maxilla and wide mandible. Correction of the transverse dimension in a patient with a narrow maxilla and a wide mandible is most difficult and is most susceptible to relapse. “This is because the mandible cannot effectively be narrowed in the anterior region except through extraction and osteotomy, often mandating correction of the remaining transverse discrepancy in the maxilla.”
The skeletal deformities that are most commonly associated with transverse maxillary deficiency involve maxillary vertical and anteroposterior hypoplasia. This is so because, as the maxilla grows, it translates down and forward and also widens. Therefore, if transverse maxillary hypoplasia is present, vertical and/or sagittal hypoplasia is often present as well. Vertical maxillary excess is commonly accompanied by transverse deficiency. Other dentofacial deformities associated with transverse maxillary deficiency include mandibular prognathism or mandibular sagittal deficiency, apertognathia, and repaired cleft palate.
RADIOGRAPHIC EVALUATION
A standard posterior-anterior (PA) cephalogram is the radiograph of choice for identification and evaluation of a transverse discrepancy. This radiographic technique allows for superimposition of radiographs, comparison of linear measurements, and evaluation of radiographs over time. Ricketts developed the Rocky Mountain analysis and established relative norms by using specific radiographic landmarks and measurements to analyze transverse discrepancies between the maxilla and the mandible ( Figures 10-4 and 10-5 ). These landmarks have been modified slightly and include JR (jugale right), JL (jugale left), AG (antegonion right), GA (antegonion left), OR (orbitale right), and OL (orbitale left). With use of these landmarks, it is possible to determine the effective maxillary width, effective mandibular width, and frontolateral facial lines. The effective maxillary width is the width of the maxilla between the points JL and JR, which represents the jugal process at the intersection of the maxillary tuberosity and the zygomatic buttress. The effective mandibular width is the width of the mandible between the AG and the GA, which are the bilateral points at the inferior margin of the antegonial protuberance, below the antegonial trihedral area. The frontolateral facial lines are the lateral lines constructed from OR and OL (representing the intersection of the orbits with the middle cranial fossa) to the points AG and GA, respectively.
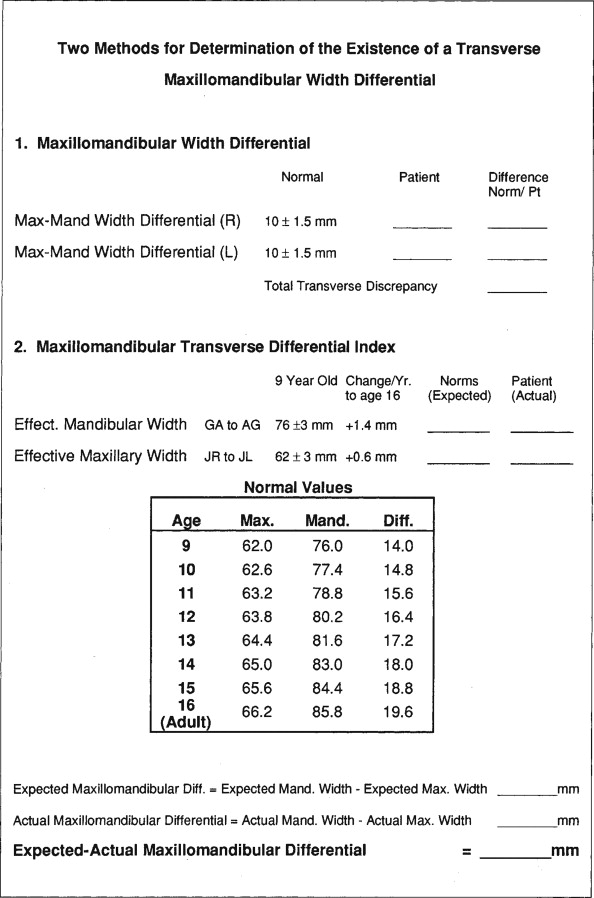
With these cephalometric landmarks, it is possible to determine the maxillomandibular width differential and the maxillomandibular transverse differential index for quantification of the transverse maxillary discrepancy. The maxillomandibular width differential is the distance (in millimeters) measured from the frontolateral facial line to JL and JR, respectively, along a line from the frontolateral facial lines through JR and JL. This measurement is calculated independently for each side and is compared with a normal value of 10 ± 1.5 mm. If this value is greater than 10 mm, a transverse discrepancy between the maxilla and the mandible exists. Values greater than 10 mm on each side are summed to quantify the total transverse deficiency. This technique is useful in determining the total discrepancy and discerning whether a greater deficiency or excess is present on one side or the other. However, this differential does not elucidate in which jaw the discrepancy exists and may be misinterpreted when mandibular asymmetry is present. The maxillomandibular transverse differential index is the age-specific expected maxillomandibular difference minus the actual measured maxillomandibular difference. The expected maxillomandibular difference is the age-appropriate expected AG-GA distance minus the age-appropriate expected JR-JL distance. The actual maxillomandibular difference is the actual AG-GA measurement minus the actual JR-JL measurement. In the adult patient, a maxillomandibular transverse differential index greater than 5 mm suggests the need for surgical expansion. If the differential index is less than or equal to 5 mm, orthodontic or orthopedic expansion may effectively correct the transverse discrepancy. As well as quantifying the total discrepancy, this method allows for the identification of which jaw is deficient or excessive, in that actual values can be compared with normal values. Normal values have been suggested only for Caucasians, and these values should not be considered normal values for other races. A recent abstract suggests that differences may be seen among races (e.g., African American and Caucasian) and between genders. Therefore, separate normal values should be established by gender and race.
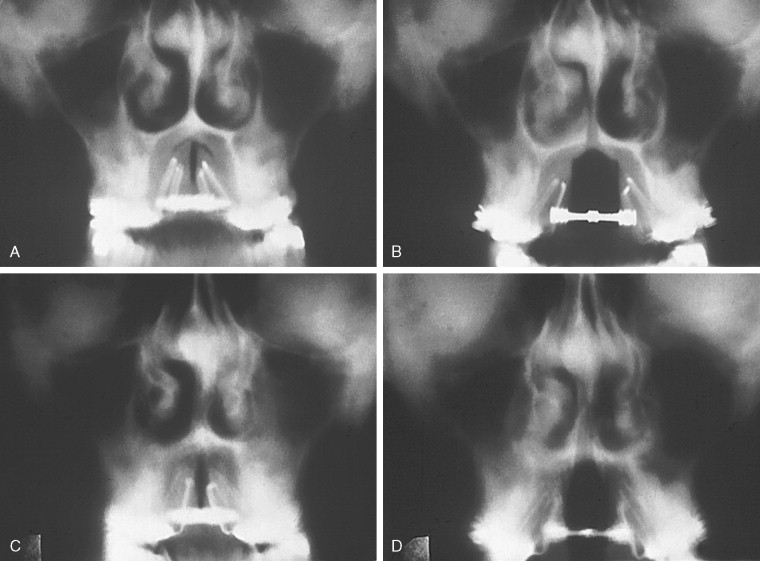
Alternative imaging modalities to the standard PA cephalogram include frontal tomography and computed tomography ( Figure 10-6 ). These imaging modalities allow for accurate calculation of any transverse discrepancy, but they are not cost effective and they deliver an unacceptable dose of radiation to the patient. Also, a cephalometer is readily available in most orthodontic and surgical offices, making the PA cephalogram easy to obtain.
TREATMENT OF TRANSVERSE MAXILLOMANDIBULAR DISCREPANCY
Treatment of transverse maxillomandibular discrepancy may be attempted by one of four techniques: slow dentoalveolar expansion (SDE), orthopedic rapid maxillary expansion (ORME), surgically assisted maxillary expansion (SAME), or segmental maxillary osteotomy. Orthodontic appliances can achieve SDE through the movement of the teeth over a 2- to 4-month period, whereas ORME achieves skeletal expansion of the maxilla over a 1- to 4-week period. SAME combines an orthodontic or orthopedic appliance with osteotomies to achieve maxillary skeletal expansion in 1 to 2 weeks. The efficacy and long-term stability of ORME depend on the type of expansion forces used and the degree of skeletal maturity attained. To achieve the desired expansion and stability, transverse maxillary expansion should be accomplished via sutural adjustments in the craniofacial complex, not by alveolar bending and dental tipping. This requires that expansion forces used should be greater than the tensile strength of the sutures. Alveolar bending and dental tipping lead to instability and uncontrolled relapse following appliance removal. The technique chosen to correct the transverse discrepancy is dependent on many factors, but most important is the skeletal maturity of the patient. Additional factors include the magnitude of the transverse discrepancy and whether gingival dehiscence or bony fenestration is already present on the maxillary canine and bicuspid teeth. Generally, low SDE forces are effective only in the primary dentition, whereas patients in the mixed dentition stage are treated by RME, and adults are best treated by SAME or segmental Le Fort osteotomy.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


