Chapter 55 Tracheostomy for sleep apnea
Tracheostomy historically is the first treatment offered for obstructive sleep apnea. It remains the only surgical option directed at obstructive sleep apnea that uniformly eliminates sleep apnea permanently. Since it was first introduced in 19681 and subsequently reported in several large studies,2,3 newer choices of medical and surgical intervention have reduced the number of people needing a tracheostomy to relieve severe and life-threatening obstructive sleep apnea (OSA).
There remain some patients for whom other treatments have been ineffective, intolerant or refused. Current reports4,5 have agreed with the long-term success at maintaining an open upper airway by creating a tracheostomy to reduce morbidity and mortality.
While tracheostomy for obstructive sleep apnea was reported by Kuhlo in 1968,1 Fee and Ward6 described a technique of skin-lined flap tracheostomy to overcome the above complications in the obese patient with obstructive sleep apnea. The goal had been to create a stoma of permanence with a diameter of 8–10 mm.
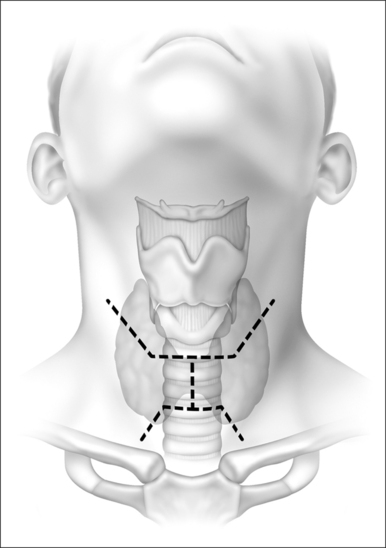
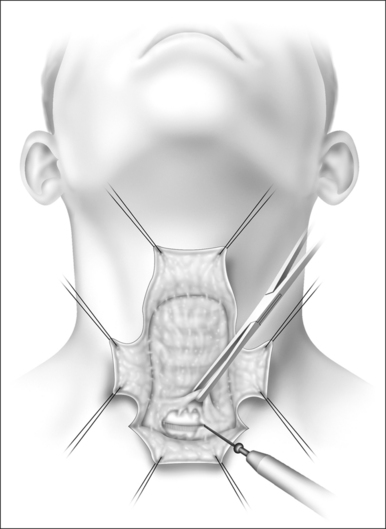
Their plan was to create a series of vertical and horizontal skin incisions which allow easy access to the fibrofatty pad of tissue overlying the muscles from the level of the hyoid bone above to the sternal notch below (Fig. 55.1). This flap elevation includes defatting the skin flaps safely and creating two vertical and two horizontal skin flaps that will be sutured to the trachea mucosa. Defatting and elevating the skin flaps safely with respect to vitalizingthe skin is most important. When elevation is complete, the surgical field is ready for a lipectomy, which is achieved from the level of the hyoid bone often down to the levelof the fifth tracheal ring (Fig. 55.2). The skin flap elevation allows access to perform a hyoidopexy to the mandibleor thyroid cartilage, if indicated, and allows removal of submental fat which will permit the healed patient to maintain an open tracheal lumen without a submental flap occluding the stoma when the head falls to the chest during sleep.
< div class='tao-gold-member'>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


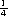 inch (6.35 mm) to secure the tube in place are placed around the neck and secured with one or two fingers laxity between tape and neck skin. Patients with sleep apnea are anticipated to have an active and productive life once sleep apnea has been treated surgically and even with significant co-morbidities, we anticipate an active lifestyle. However, the tracheostomy technique described above does not allow temporary extubation, and under only extraordinary circumstances would allow a tube-free tracheostomy, even for short times during the day or overnight. Therefore, most patients, including many of normal body habitus, who have severe obstructive sleep apnea and have been untreatable with mechanical positive pressure or upper airway surgery are recommended to have a tracheostomy as described below. Most of these patients are severely obese with a Body Mass Index greater than 36 and with sizable adipose tissue between skin and trachea. These people need a more thorough approach to the airway and a better solution to stoma hygiene in what is anticipated as life-long airway and apnea management.
inch (6.35 mm) to secure the tube in place are placed around the neck and secured with one or two fingers laxity between tape and neck skin. Patients with sleep apnea are anticipated to have an active and productive life once sleep apnea has been treated surgically and even with significant co-morbidities, we anticipate an active lifestyle. However, the tracheostomy technique described above does not allow temporary extubation, and under only extraordinary circumstances would allow a tube-free tracheostomy, even for short times during the day or overnight. Therefore, most patients, including many of normal body habitus, who have severe obstructive sleep apnea and have been untreatable with mechanical positive pressure or upper airway surgery are recommended to have a tracheostomy as described below. Most of these patients are severely obese with a Body Mass Index greater than 36 and with sizable adipose tissue between skin and trachea. These people need a more thorough approach to the airway and a better solution to stoma hygiene in what is anticipated as life-long airway and apnea management.