Chapter 61 Salvage of failed palate procedures for sleep-disordered breathing
1 INTRODUCTION
Surgical procedures designed to shorten or otherwise modify the palate may provide relief of upper airway collapse at the palatal level in patients with sleep disordered breathing (SDB). For patients who fail, or suffer a relapse after an initial surgical success, salvage surgical techniques may be appropriate. Although the principles of these salvage techniques are similar to the commonly performed primary surgical procedures, subtle modifications of the approach are sometimes required, and these are emphasized in this chapter.
The uvulopalatopharyngoplasty (UPPP) procedure has become a mainstay in the management of palatal collapse for patients with SDB. A review of literature has shown that 40.7% of patients who have undergone this procedure have a favorable response. A favorable response is defined as either an Apnea/Hypopnea Index (AHI) of less than 10 episodes per hour or an AHI <20 per hour as well as a 50% decrease in the AHI from the base line.1 In addition, in an effort to decrease the morbidity of surgical treatment, several office-based surgical interventions have been developed and implemented for the treatment of obstruction at the palate level, including laser-assisted uvulopalatoplasty (LAUP), and radiofrequency ablation of the palate (RFAP). While these procedures have proven effective in treating mild SDB in short-term analyses, the long-term evaluation of these procedures has revealed a substantial rate of recurrence of both the snoring and daytime sleepiness, and in some cases a steady trend toward recurrence has been shown over time.2 In patients with severe sleep apnea, however, it was demonstrated that UPPP has virtually no place in its management.
2 SALVAGING LAUP WITH RFAP
2.1 PATIENT SELECTION
Patients who have had their snoring successfully mitigated with LAUP but have experienced a relapse may be appropriate candidates for re-treatment with LAUP. If they are reluctant to suffer the discomfort associated with this procedure, or if they are experiencing any type of dysphagia symptoms or occasional aspiration as a result of the prior treatment, it may be preferable to consider a trial of RFAP. Radiofrequency energy causes a low-temperature molecular disintegration, resulting in volumetric tissue removal with minimal collateral tissue damage.3
2.2 PROCEDURE
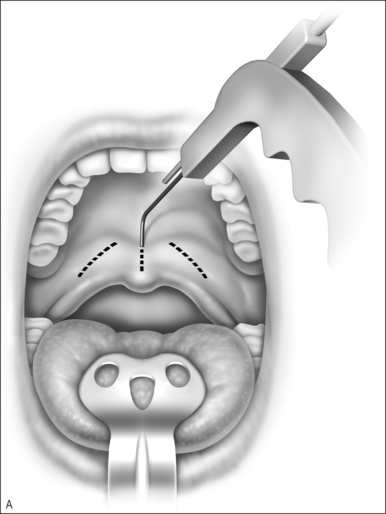
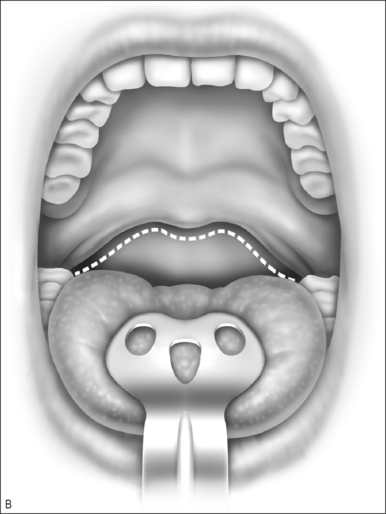
The treatment is performed as previously detailed withthe patients seated in the office. After achieving local anesthesia, a commercially available RFAP hand-piece connected to a 465 kHz radiofrequency device (Somnus, Inc., Sunnyvale, CA) is introduced submucosally in a midline (600 J) and two lateral locations (300 J) for three separate sequences of energy, delivering a total of 1200 J at atarget temperature of 85°C and 10 watts of power. The intended effect is the shrinkage of the soft tissues, resulting in tightening and modest shortening of the palate(Fig. 61.1).
2.3 COMPLICATIONS
RFAP is not associated with any major complications. The salvage operation may involve the risks of attaining suboptimal results as in primary surgery. RFAP, although intended to be mucosa sparing, is nevertheless associated with a high incidence of mucosal injuries, many of which are occult.4 Mucosal edema, if it happens, settles by itself. Superficial ulceration of the soft palate was also reported.5
3 SALVAGING UPPP WITH LAUP
3.1 PATIENT SELECTION
The failed UPPP may present particular challenges in treatment because of the diminished palatal tissue (raising the risk of velopharyngeal insufficiency) and the substantial scar tissue that may be present. Therefore the midline palate must be treated with respect, and operated on only rarely, and with caution. This procedure is especially suitable when the palate remains somewhat low-lying and the relapse of symptoms is felt to be related to softening of scar tissue.
< div class='tao-gold-member'>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses