(1)
Department of Endodontics, New York University College of Dentistry, New York, NY, USA
Abstract
This chapter reviews pharmacologic strategies including the use and abuse of antibiotics and analgesics. New guidelines are available to describe the indications for antibiotics. Antibiotics should be thought of as a supplement to clinical procedures in specific situations. The chapter explains why antibiotics should not be thought of as a means of “curing” an endodontic infection. The relationship of antibiotics, bacterial susceptibility, and acute abscesses is considered and evidence-based principles of antibiotic dosing are suggested.
Analgesics are presented as part of a pain-preventive (preemptive) strategy, in contrast to the historic use of analgesics only after a patient develops pain. Useful clinical tips include the advice that analgesics should be taken by the clock rather than only when a patient experiences pain.
Also reviewed is current evidence-based research supporting the use of a combination of acetaminophen and ibuprofen, to prevent and/or treat pain. That strategy is compared to the traditional use of narcotic agents to treat pain. Issues associated with addiction and drug overdose are also discussed.
Also discussed in this chapter is recent evidence concerning possible complications associated with the use of NSAIDs and acetaminophen in pregnant women and children as is evidence of sex bias in analgesic research.
8.1 Pharmacotherapeutics
8.1.1 Antibiotics
It is important to understand the role of antibiotics in the treatment of endodontic infections. In specific situations, they can play a supportive role in the reestablishment of the proper balance between the host’s defenses (immune and inflammatory) and microbes. Clinical and pharmacologic strategies are used independently or in unison to prevent or treat pain and infection.
Antibiotics should be considered as a useful supplement to endodontic cleaning/shaping and irrigation in specific situations. They are not analgesics and should not be used to treat pain. Short-term, high-concentration, broad-spectrum antibiotic prophylaxis is indicated for some heart conditions and in some situations for prosthetic joints [9].
Clinical Tips
-
When there are questions concerning antibiotic premedication, it is advisable to communicate with the patient’s physician.
-
The clinician must stay alert for changes in medical indications for antibiotic prophylaxis as well as dose modifications.
8.1.2 Use and Abuse of Antibiotics
-
The American Association of Endodontists, Colleagues for Excellence, published a newsletter in 2012, titled “Use and Abuse of Antibiotics.” This article reviews the most current guidelines for antibiotic prophylaxis for endocarditis and joint replacement. The newsletter is available at http://www.aae.org/colleagues/.
-
There are guidelines for the use of antibiotics during endodontic therapy, but each case may present variables that can influence the decision. Not all swellings require antibiotic therapy. For example, a large diffuse swelling increasing in size and producing no drainage on instrumentation may be a candidate for incision and drainage and perhaps an antibiotic. In contrast, a small, well-circumscribed swelling does not usually require antibiotic therapy. Antibiotics may be used in select non-vital cases that meet the criteria described below (Fig. 8.1).
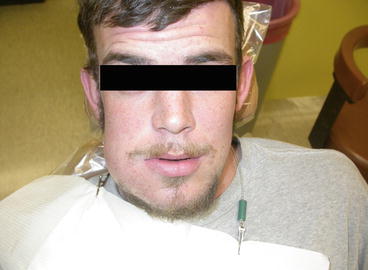 Fig. 8.1Emergency patient, presenting with cellulitis due to a necrotic mandibular molar
Fig. 8.1Emergency patient, presenting with cellulitis due to a necrotic mandibular molar
Indications and Contraindications for Antibiotics
The following are important facts concerning the use of antibiotics in the treatment of endodontic infections.
Indications for Adjunctive Antibiotics
-
Fever >100 ° F
-
Malaise
-
Lymphadenopathy
-
Trismus
-
Increased swelling
-
Cellulitis
-
Osteomyelitis
-
Persistent infection
Conditions Not Requiring Adjunctive Antibiotics
-
Pain without signs and symptoms of infection
-
Symptomatic irreversible pulpitis
-
Acute periradicular periodontitis
-
-
Teeth with necrotic pulps and a radiolucency
-
Teeth with a sinus tract (chronic periradicular abscess)
-
Localized fluctuant swellings [24]
8.1.3 Facts Concerning the Use of Antibiotics
-
The cause of the infection must be addressed (cleaning/shaping and irrigation) prior to, or concomitant with, antibiotic therapy
-
Cleaning/shaping and irrigation without antibiotic therapy will result in healing of most endodontic infections. The majority of endodontic infections do not require systemic antibiotic therapy.
-
It has been estimated that up to 60 % of human infections resolve due to host defenses alone following removal of the cause of the infection without antibiotic intervention.
Antibiotics, Bacterial Susceptibility, and Acute Abscesses
A study examined the susceptibility of bacteria, recovered from acute apical abscesses, to five commonly used antibiotics. Antibiotic susceptibility data drawn from 12 acute apical abscesses led to the following conclusions [2]:
-
Pen-V-K is the antibiotic of choice for endodontic infections due to its effectiveness in polymicrobial infections, its relative narrow spectrum of activity against bacteria most commonly found in endodontic infections, and its low toxicity and low cost.
-
Clindamycin is the antibiotic of choice for patients allergic to penicillin.
-
While amoxicillin and Augmentin (amoxicillin and clavulanic acid) demonstrated higher antibacterial effectiveness than Pen-V-K. Due to the broader antibacterial spectrum of amoxicillin and the increased cost of Augmentin, it was recommended that amoxicillin/Augmentin should be reserved for unresolved infections and patients who are immunocompromised.
-
Metronidazole demonstrated the greatest amount of bacterial resistance and is only effective against anaerobes. Therefore, it should not be used alone for the treatment of endodontic infections [2].
Additional Facts Concerning Antibiotics
The following section on the use of antibiotics has been adapted and modified from an excellent publication for the dental community presented by the American Association of Endodontists Colleagues for Excellence, as the winter 2012 edition. It is entitled, “Use and Abuse of Antibiotics” and can be found at www.aae.org/colleagues/.
-
Antibiotics that can penetrate into the mammalian cell (erythromycin, tetracycline, clindamycin, and metronidazole) are more likely to affect the host defenses than those that cannot (beta-lactams).
-
Tetracyclines may suppress white cell chemotaxis. Most antibiotics (except tetracycline) do not depress phagocytosis.
-
The use of multiple antibiotics has not been proven superior to a single antibiotic.
-
Bactericidal agents are not always superior to bacteriostatic agents. Bactericidal agents are required for patients with impaired host defenses.
-
However, bacteriostatic agents are usually satisfactory when the host’s defenses against infections are unimpaired.
-
Postantibiotic effects (PAEs—persistent suppression of bacterial growth after previous exposure to antibiotics) are more persistent and reliable with bacteriostatic agents (erythromycin, clindamycin) than with bactericidal agents (beta-lactamase) because the clinical effects of bacteriostatic agents are less dose-dependent.
The following principles of antibiotic dosing have been suggested:
-
The shorter the duration of therapy, the lower the risk to the patient for the development of antibiotic-induced toxicity and/or allergy and a reduced risk of developing resistant microorganisms.
-
It is advisable to initiate antibiotic therapy with a loading dose (an initial dose higher than the maintenance dose). An antibiotic loading dose should be used whenever the half-life of the drug is longer than 3 h or whenever a delay of 12 h or longer to achieve a therapeutic blood level is expected.
-
Most antibiotics used in the treatment of orofacial infections have a half-life shorter than 3 h, but, due to their acute nature, most orofacial infections require therapeutic drug blood levels sooner than 12 h. Steady-state blood levels of any drug are usually achieved in a time equal to three to five times the drug’s half-life.
-
Amoxicillin has a half-life of one to one-and-a-half hours. A steady-state blood level would then be achieved in three to seven-and-a-half hours thereby leading to a substantial delay in achieving therapeutic antibiotic blood levels. A loading dose of two times the maintenance dose is recommended for acute orofacial infections, which better achieves the goal of rapid, high blood levels rather than initiating therapy with the maintenance dose.
-
An oral antibiotic should ideally be administered at dosing intervals of three to four times its serum half-life, particularly if steady-state blood levels are desired (as may be indicated with beta-lactam agents). For example, the serum half-life of Pen-V-K is 0.75 h. Higher continuous blood levels of this antibiotic are more likely to be obtained with 4-h rather than 6-h dosing intervals. The shorter the serum half-life of the drug, the shorter the dosing interval will need to be in order to maintain continuous therapeutic blood levels of the drug.
-
A common misconception asserts that prolonged (after clinical remission of the disease) antibiotic therapy is necessary to prevent “rebound” infections from occurring. Orofacial infections do not “rebound” if the source of the infection is eliminated.
-
Most orofacial infections persist for 2–7 days and often less. Patients placed on antibiotic therapy for an orofacial infection should be clinically evaluated on a daily basis. When there is sufficient clinical evidence that the patient’s host defenses have regained control of the infection and that the infection is resolving or resolved, the antibiotic therapy should be terminated.
Clinical Tips
-
When a patient is taking an antibiotic for an endodontic infection, it is essential that the patient be seen frequently for concomitant instrumentation, irrigation, and evaluation.
Bacterial Resistance
Microbial antibiotic resistance is an important issue. Its cause is the use and abuse of antibiotics and a simultaneous decline in research and development of new antimicrobial drugs. In Europe alone, it has been estimated that 25,000 people die every year from antibiotic-resistant bacteria, and that only represents infections that were identified in hospitals.
8.1.4 New American Association for Orthopedic Surgeons/American Dental Association (AAOS/ADA) Guidelines for Antibiotic Usage
The new AAOS/ADA practice guideline [1] principal recommendation is the following:
The practitioner might consider discontinuing the practice of routinely prescribing prophylactic antibiotics for patients with hip and knee prosthetic joint implants undergoing dental procedures.
The language of the new recommendation seems somewhat vague. What does “might consider” mean? Also, if we discontinue “routinely prescribing prophylactic antibiotics,” what sorts of cases would count as not routine?
Some believe that it is likely that the personal and public health harm of widespread antibiotic use for prophylaxis would outweigh its dubious benefits. It is important for dentists, orthopedic surgeons, and patients to communicate with each other as they decide who should receive prophylaxis and when to discontinue it. The decision concerning antibiotic prophylaxis, at this time, should be made on a case-by-case basis.
8.1.5 Systemic Penicillin and Pain
A prospective, randomized, double-blind study determined that the administration of penicillin did not significantly (P > .05) reduce spontaneous pain, pain due to percussion, or the number of analgesic medications taken by patients with untreated irreversible pulpitis [19].
The majority of patients with untreated irreversible pulpitis had significant pain and required analgesics to manage their pain. It was concluded that penicillin should not be prescribed for untreated irreversible pulpitis because penicillin is ineffective for pain relief [19].
8.1.6 Self-Assessment
Question:
A patient presents with acute pain of pulpal origin originating from tooth #30 due to a deep carious lesion. The patient has pain when biting, sensitivity to percussion, and a lingering painful response to cold stimuli. Should an antibiotic be prescribed for this patient?
Answer:
The history and clinical tests indicated that tooth #30 has irreversible pulpitis and extension of the inflammatory process into the periodontal ligament resulting in pericementitis. Proper treatment includes initiating endodontics and prescribing an analgesic. There is no indication for an antibiotic. Due to pericementitis, it would be appropriate to reduce the occlusion.
8.2 Preventive (Preemptive) vs. Reactive Analgesic Strategy
Historically, patients have heard these words, “if you have pain, take the medication.” That approach to pain is essentially reactive and does not recognize the biological process resulting in pain.
In that scenario, a clinician waits and, if the patient experiences pain, then reacts. A more biologically based preventive approach relies on our knowledge of tissue damage, mediator release, and the subsequent processes.
Preoperative ibuprofen was shown to delay the onset and decrease the severity of pain. There was an additive effect when it was combined with long-lasting local anesthetic.
“After acetaminophen (1,000 mg) was administered 30 min prior to surgery, onset of the peak pain was delayed and patient discomfort was decreased 3, 4, and 5 h after surgery.”
Clinical Tips
-
The use of long-lasting rather than short-acting local anesthetics represents an important part of a pain-preventive strategy by blocking pain impulses from the operative site to higher centers during the immediate postoperative period.
-
An additional component of a pain-preventive strategy includes having the patient take analgesics at the treatment visit and later. This strategy is directed at blocking production of mediators associated with pain.
-
Analgesics should be taken by the clock rather than when a patient experiences pain.
8.3 Analgesics
Various classes of drugs have been studied for the management of posttreatment endodontic pain [22, 25, 27]. These include nonnarcotic analgesics including NSAIDs, acetaminophens, opioids, and steroids.
Opioids and acetaminophen are considered to act primarily on the central nervous system. In contrast, inflammation-suppressing drugs such as corticosteroids and nonsteroidal anti-inflammatory drugs (NSAIDs) are effective in reducing pain with their action at the site of injury. Combination of NSAIDs with acetaminophen, which apparently acts centrally, is even more effective [14, 15].
Patient’s pain perception is complex. Factors include genetics, gender, age, organ function, physiological variables, anxiety, severity and type of pain, social–environmental variables, comorbidities, placebo effect, patient compliance, and pharmacodynamics. However, it is important to remember that the clinical treatment we provide is the key factor.
The effectiveness of treatment for pain depends in part on the strength of the clinician–patient relationship. Pain treatment is never about the intervention alone, but about the clinician and patient working together [23].
8.3.1 Exceptions
Although uncommon, some patients may continue to have pain at moderate to severe levels persisting for days, even after appropriate endodontic intervention. Posttreatment analgesic intervention is required in a significant percentage of endodontic cases.
Numerous clinical studies have evaluated the efficacy of a variety of analgesics for their ability to ameliorate dental pain [5, 6, 14, 15]. Most of these studies have used a third-molar surgical extraction model for evaluation of pain of an acute inflammatory nature. It is important to recognize that there are significant differences between a molar extraction and pain associated with an endodontic problem.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


