(1)
Department of Endodontics, New York University College of Dentistry, New York, NY, USA
Abstract
Prior to initiating endodontic treatment, achieving profound anesthesia is of primary importance. A patient’s assessment of the treatment and the dentist’s skills is largely based on achieving complete anesthesia. Many of the “horror stories” that patients relate about pain and root canal therapy are probably due to inadequate anesthesia.
This chapter will review the causes of anesthetic problems and how they are best managed. There are some cases that are more likely than others to experience anesthetic problems. It is helpful to identify those potential problem cases before treatment.
An example of an anesthetic problem is treatment of a “hot tooth” (presence of a numb lip but pain persists). Most often, this problem is associated with long-standing irreversible pulpitis in a mandibular molar. Predictable anesthetic strategies to resolve that problem are presented. The use of a variety of supplemental injections and nitrous oxide is also reviewed.
Determining the presence of profound anesthesia is essential and using a numb lip or sticking the gingiva are not dependable tests. An evidence-based approach to recognizing profound anesthesia is described.
The greatest evil is physical pain. Saint Augustine
6.1 Depth of Local Anesthesia
Profound anesthesia is the key factor in determining patients’ endodontic experience and their assessment of the dentist. Incomplete anesthesia results in pain and increases patient’s anxiety with a concomitant drop in their pain threshold. This negative spiral of events affects the patient’s endodontic experience and can be prevented. Procedures should be initiated only after profound anesthesia is achieved. Compromising the level of anesthesia is a poor strategy for a clinician hoping to have a satisfied patient.
6.1.1 Soft Tissue and Dental Anesthesia
Soft tissue anesthesia and dental anesthesia must not be confused. A numb lip is often representative of only soft tissue anesthesia or incomplete dental anesthesia rather than profound pulpal anesthesia.
A clinical study determined that patients with lip symptoms following an injection of local anesthesia with a negative response to a cold test were approximately 80 % less likely to experience pain during endodontic treatment compared to those who had only soft tissue signs of anesthesia [9].
Clinical Tips
Profound Local Anesthesia
-
Prior to initiating treatment, the clinician should test the tooth using the chief complaint as a provoking stimulus.
-
If the patient’s chief complaint is cold sensitivity, a test using Endo-Ice or the equivalent is invaluable in evaluating the depth of anesthesia.
-
Similarly, if percussion sensitivity was the primary complaint, that test should be used prior to initiating treatment.
-
If profound local anesthesia is defined as complete absence of pain, a single injection for a mandibular molar with irreversible pulpitis is usually insufficient.
-
A slow inferior alveolar nerve block injection (60 s) results in a higher success rate of pulpal anesthesia than a rapid injection (15 s) [12].
6.2 Anesthesia and Irreversible Pulpitis
Studies in patients with irreversible pulpitis determined that success (mild or no pain upon endodontic access or initial instrumentation) with the inferior alveolar nerve block varied between 15 and 57 % of the time. It is clear that profound anesthesia is often difficult to achieve in patients with irreversible pulpitis with only the INAB. It is often necessary to utilize supplemental injections for these patients [12].
6.3 Anesthetic Failure
A tooth with irreversible pulpitis is significantly more challenging to anesthetize than a normal tooth. There are a number of hypotheses used to explain anesthetic failure and it may be that no single hypothesis explains all clinical situations.
The following hypotheses represent possible causes of anesthetic failure [1]:
-
An anesthetic solution may not penetrate to the sensory nerves that innervate the pulp, especially in the mandible.
-
The central core theory hypothesizes that nerves on the outside of the nerve bundle supply molar teeth, whereas nerves on the inside supply anterior teeth. Even if deposited at the correct site, anesthetic solution may not diffuse adequately into the nerve trunk to produce an adequate block. This theory may explain elevated anesthetic failure rates in experiments on anterior teeth with inferior alveolar nerve blocks.
-
It has been hypothesized that long-term low-level pain may sensitize nociceptors, resulting in a lower pain threshold (allodynia) associated with an exaggerated response to a stimuli (hyperalgesia).
-
Basic chemistry postulates that the lowered pH of inflamed tissues reduces the amount of the base form of anesthetic available to penetrate a nerve’s membrane. Consequently, there is less of the ionized form within the nerve to achieve anesthesia.
-
Although the theory based on pH may have some validity, it is an unlikely cause of anesthesia problems in the mandible. The injection site is distant from the area of inflammation associated with a tooth, and changes in local tissue pH would be unrelated to the anesthesia problem.
-
Patients in pain are often apprehensive, which can lower their pain threshold. A negative cycle may occur starting with initial apprehension leading to reduced pain threshold, anesthesia complication, and still further increased apprehension. This can result in a lack of confidence in the dentist.
-
The dentist may not allow sufficient time for the anesthetic to diffuse. Onset of complete anesthesia may be slow, particularly with the inferior alveolar block.
6.3.1 Individual Variations
There are significant individual variations among patients and their response to a local anesthetic. Patients may report a history of years of bad experiences with dental anesthesia. It is difficult to ascertain if the problem is due to anatomic factors, a high level of anxiety, or other causes, but the clinician should be prepared to use supplemental techniques. The clinical situation determines the supplemental technique to use.
Clinical Tips
-
A patient with irreversible pulpitis and a numb lip and no response to cold testing may still not have complete pulpal anesthesia. Profound lip numbness does not guarantee pulpal anesthesia.
-
Pricking the soft tissue with a sharp explorer does not indicate pulpal anesthesia.
-
Following an inferior alveolar nerve block, pulpal anesthesia fails in approximately 17 % of first molars, 11 % of first premolars, and 32 % of lateral incisors. All of the patients tested had profound lip numbness [12].
-
The onset of lip numbness occurs within 5–9 min.
-
Pulpal anesthesia usually occurs within 15–16 min [12].
-
Slow onset of pulpal anesthesia occurs after 15 min. In approximately 19–27 % of mandibular teeth, pulpal anesthesia requires more than 15 min. Between 6 and 8 % of patients have onset after 30 min [12].
6.3.2 Supplemental Anesthesia
It is helpful to determine if the patient has a previous history of difficulty in achieving complete local anesthesia. Patients with that history may be more likely to experience continuing anesthetic problems. It is also an indication that supplemental injections may be required.
6.4 Case Selection
Supplemental anesthesia is a critical component of endodontic treatment. Clinicians may vary as to their preferred supplemental approach, but there are some clinical indicators and contraindications to be aware of. It is advised that dentists become proficient in a variety of supplemental injections. Specific clinical factors will dictate, on a case-by-case basis, the most appropriate supplemental injection. For example, deep periodontal pockets would dictate against a ligamental injection.
Another example of case selection for supplemental injections occurs when identifying appropriate cases for an intra-pulpal injection. In cases where there is an anesthesia problem, the intra-pulpal injection is a good choice if there is an existing pulp exposure or near exposure. When a substantial amount of excavation is required prior to the intra-pulpal injection, an alternative supplemental injection should be selected.
Clinical Tips
-
Following supplemental injections, it is recommended that all tissue be removed from the canals, in order to avoid problems at the next visit.
6.4.1 Buccal Infiltration
Buccal infiltration injection of articaine after an inferior alveolar nerve block in mandibular first molars without irreversible pulpitis was found to increase anesthetic success. It was determined that a buccal infiltration of 4 % articaine with 1:100,000 epinephrine after an inferior alveolar nerve block significantly increased success (88 %) when compared to using a lidocaine formulation (71 % success). However, for patients with irreversible pulpitis, the supplemental buccal infiltration of articaine was found to be only 58 % successful [12].
Clinical Tips
-
Buccal infiltration alone is insufficient for endodontic treatment.
-
Mandibular buccal infiltration (and other supplemental injections) should be preceded by an inferior alveolar nerve block and lip symptoms.
-
Thick buccal bone in the area of the mandibular second molar may interfere with diffusion of anesthetic during buccal infiltration injections.
6.4.2 Intra-ligamental (PDL) Injection
The periodontal ligament injection (PDL) is a useful injection for posterior teeth after an inferior alveolar nerve block that does not provide profound anesthesia. Back pressure during the injection is an important factor in its success. Absence of back pressure usually leads to failure of the injection [7, 17] (Fig. 6.1).
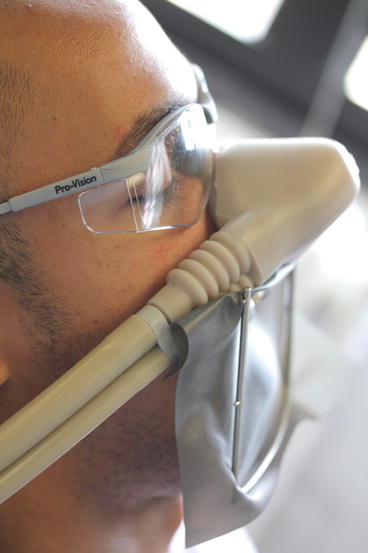

Fig. 6.1
Patient receiving nitrous oxide with rubber dam in place
Special ligamental syringes have not been found to be more effective than a standard syringe [4, 14]. However, the CompuDent CCLAD system (Milestone Scientific Livingston, New Jersey) has been found to increase the duration of anesthesia [2]. It is not uncommon for the patient to experience moderate pain postoperatively following the injection.
The intra-ligamentary injection forces anesthetic solutions through the cribriform plate into the marrow spaces around the tooth [5, 17]. The primary route is not through the periodontal ligament, and the injection may be considered a type of intraosseous injection rather than a pressure injection [7, 17] like intra-pulpal anesthesia.
The intraosseous injection is more successful than the intra-ligamentary injection [13] due to the greater amount of anesthetic solution delivered with the intraosseous injection. However, the intra-ligamentary injection may be helpful if the clinician is not familiar with the intraosseous injection. A supplemental intra-ligamentary injection is about 75 % successful (Fig. 6.2). Reinjection will increase success to approximately 95 % [10, 11]. However, duration is fairly short when compared to the intraosseous injection.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


