(1)
Department of Endodontics, New York University College of Dentistry, New York, NY, USA
Abstract
Endodontic diagnosis represents a multidimensional challenge. It should be thought of as a process leading to an answer rather than just a question and answer. During the process the dentist collects data including the chief complaint, medical and dental histories, radiographs, and clinical tests. This is followed by synthesis of findings leading to an evidence-based diagnosis.
Early in the process the clinician must categorize patient’s symptoms as being of odontogenic or non-odontogenic origin. If it is non-odontogenic a referral is often made to another health-care practitioner with expertise in that area. If the problem is odontogenic, the dentist has another question to resolve: “Should I treat the patient or should I refer the patient to a specialist?” This chapter discusses some of the issues and guidelines associated with that question.
The patient’s medical and dental histories and description of the onset of symptoms provide information that may have a bearing on the diagnosis and treatment plan. Specific medical problems including diabetes, liver disease, and alcoholism should be discussed in terms of their impact on treatment.
Reading this chapter will enable a clinician to recognize some of the key words used by patients and how they indicate non-odontogenic or odontogenic causes of pain. Important clinical findings including stomas and the use of local anesthetic as a diagnostic tool are also reviewed. Sample patient–dentist dialogues are presented demonstrating the importance of that conversation.
1.1 Introduction
The International Association for the Study of Pain has defined pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage.” This text will review both sensory and emotional aspects of pain and their relationship to endodontic practice.
At an initial consultation concerning pain, there are an incredible number of factors to be considered. Among them are biological, psychological, and psychosocial factors that have an influence on a patient’s pain and their interaction with the dentist.
The diagnostic process requires organization of a mass of information drawn from a written medical history, a dialogue with the patient, radiographs, sensibility tests, and clinical examination. The diagnostic process proceeds in a logical, systematic manner leading to a synthesis of the findings. Quick judgments should be avoided until all of the data is collected.
This chapter will review varied aspects of the diagnostic process.
A good initial question to start a dialogue with the patient is “How can I help you?” Depending on the patient’s personality and verbosity, this may lead to an extensive description of the patient’s pain or a brief noncontributory response. Even at this early stage of the diagnostic process, listening closely can provide meaningful clues about the patient’s pain and the direction to take the diagnostic process.
1.2 Medical History
The medical history is an important early step in the endodontic diagnostic process. It is advisable to use a written form supplemented by a conversation with the patient.
Often a patient may return a written form with little or no information provided. However, when asked if there is any additional information about past or present illnesses or medication, a stream of important medical details is presented. A dialogue pertaining to the medical history could start with the following statement: “Is there anything in your medical history, past or present that has not been covered on the form?” Some patients are reluctant to provide portions of their medical history in writing but are willing to discuss it in privacy.
It must be determined if there are medical conditions or medications that could cause or affect the patient’s symptoms or modify the diagnostic inquiry. Examples of medical conditions that may require consultation with the patient’s physician, prior to treatment, include recent myocardial infarction, heart valve surgery, recent joint replacements, liver disease, and poorly controlled diabetics. The clinician is advised to have ready access, during the diagnostic and treatment planning process, to a text that can provide guidance in the treatment of medically compromised patients. A good example of such a text is Little and Falace’s Dental Management of the Medically Compromised Patient [12]. Also important is ready access to physicians for consultation.
1.2.1 Diabetes
Patients taking insulin for diabetes must adhere to their diet. Consumption of adequate calories and medication at proper intervals is important to determine before treatment is initiated. Failing to eat in accordance with their diabetes management plan may result in a hypoglycemic event. A hypoglycemic reaction also may be due to an overdose of insulin or an oral hypoglycemic agent [12].
Pulps from patients with diabetes tend to have limited capillary exchange, collateral circulation, impaired immune response, increased risk of acquiring pulp infection (especially anaerobic ones), or necrosis, besides toothache and occasional tendency toward pulp necrosis caused by ischemia. In regard to molecular pathology, hyperglycemia is a stimulus for bone resumption, inhibiting osteoblastic differentiation and reducing bone recovery [11].
A study reviewed data from electronic patient records. It investigated the effect of diabetes mellitus on endodontic treatment outcome. It determined that patients with diabetes have increased periodontal disease with endodontic involvement compared with patients who did not have diabetes. There was also a trend toward increased symptomatic periradicular disease in patients with diabetes who received insulin, as well as flare-ups in all patients with diabetic disease [5].
Two years or longer postoperatively, 68 % of cases followed were successful. Older age, absence of preoperative lesions, presence of permanent restorations, and longer postoperative evaluation periods all were associated with a successful outcome. A multivariate analysis showed that in cases with preoperative periradicular lesions, history of diabetes was associated with a significantly reduced successful outcome. It was concluded that patients with diabetes have increased periodontal disease in teeth with endodontic problems and have reduced likelihood of success of endodontic treatment in cases with preoperative periradicular lesions [5].
Signs and Symptoms of Insulin Reaction
Mild Stage
-
Hunger
-
Weakness
-
Tachycardia
-
Pallor
-
Sweating
-
Paresthesia
Moderate Stage
-
Incoherence
-
Uncooperativeness
-
Belligerence
-
Lack of judgment
-
Poor orientation
Severe Stage
-
Unconsciousness
-
Tonic or clonic movements
-
Hypotension
-
Hypothermia
-
Rapid pulse
1.2.2 Liver Disease
Patients with liver disease and/or alcoholism require special consideration in terms of drugs to be used in conjunction with treatment. For example, a history of liver disease affects the choice of analgesics and precludes the use of acetaminophen.
Alcoholic patients with cirrhosis may require increased amounts of local anesthetics or additional anxiolytics due to liver enzyme induction and central nervous system effects of alcohol [12]. Dental drugs metabolized primarily by the liver include lidocaine (Xylocaine), mepivacaine (Carbocaine), prilocaine (Citanest), and bupivacaine (Marcaine). Their safety depends on the dose of the drug used and the severity of liver disease. Aspirin, acetaminophen (Tylenol), codeine, meperidine (Demerol), and ibuprofen (Motrin) should be avoided or used in a limited dose. Sedatives such as diazepam (Valium) and barbiturates should also be avoided or used in a limited amount depending on the severity of liver disease. The antibiotics metronidazole and vancomycin should also be avoided in the presence of severe liver disease (accute hepatitis and cirrhosis) [12].
Clinical Tips
-
Prior to initiating treatment for patients with a history of liver disease, it is important for the clinician to review the relationship of drugs to be used (local anesthetics, analgesics, antibiotics, and sedatives) and their effect on the liver [12].
-
When questions exist, consultation with the patient’s/physician prior to treatment is always appropriate.
Drug and Alcohol Abuse
Abuse of drugs and alcohol is a growing public health worldwide problem. It impacts many areas of life including health care. Inevitably, dental practitioners will encounter patients whose desire for drugs seems inappropriate based on their actual therapeutic need. Dental/medical management of painful conditions and ascertaining the actual level of pain can be challenging especially in alcoholic patients or drug abusers.
1.2.3 Chronic Facial Pain
A history of chronic facial pain or headaches provides an important clue indicating that the clinician will have to differentiate between non-odontogenic and odontogenic pain.
1.3 History of the Chief Complaint
The patient’s description of the onset of pain, its intensity, and what relieves it provides vital clues to the clinician. A key question for patients concerns the origin of their pain.
When a patient describes a “toothache,” the clinician should not accept that as a final diagnosis. The description of a “toothache” must be verified through interpretation of the history and multiple sensibility and clinical tests and radiographs in order to be sure that the pain is actually odontogenic in nature.
Clinical Tips
-
Absence of any specific dental complaint is a valuable clue indicating possible non-odontogenic origin of pain.
The history of the chief complaint is a starting point in differentiating odontogenic and non-odontogenic pain. Listening closely to the patient’s dental history is a critical part of the diagnostic process. An astute diagnostician listens, like an inquisitive detective collecting information and synthesizing it. Actually, the collection of information starts at the moment the patient enters the treatment area.
The patient’s personality is an important factor. Is the patient extremely anxious and non-communicative, or is the person calm and able to clearly describe their pain? How the patient responds during the diagnostic phase of treatment provides insight into their level of anxiety, and that is important as diagnosis and treatment progresses.
Often, the dentist can make a tentative diagnosis based on the information provided by the patient. One of the first considerations is to determine whether or not the symptoms indicate an odontogenic or non-odontogenic cause. That point represents a critical fork in the road for the clinician and patient. An important question, concerning odontogenic vs. non-odontogenic causation, includes a question concerning what provokes the pain. Others include: “How long have you had the pain?” “What words would you use to describe the pain?” “How long does it last?” “What stops the pain?”
1.3.1 Dental History
The dental history should also include details concerning past dental experiences including recent restorations and periodontal treatment. Either of those could cause postoperative symptoms that may complicate the diagnosis.
The history provides important insight into the patient’s level of dental sophistication in terms of how they value preservation of their natural dentition. For example, a patient missing numerous teeth and having poor oral hygiene is an unlikely candidate for complex treatment with a questionable prognosis. Ultimately, the treatment plan must be individualized and appropriate for the patient. Prudent use of the patient’s financial resources is another factor to consider.
Patients in severe pain may not be able to provide accurate information about the history of pain due to their physical and emotional distress. They may seem angry and depressed which are common outcomes of prolonged pain. Extreme pain can dominate a patient’s life and cause a person’s personality to totally change. Emily Dickinson, the American poet, expressed that feeling in a portion of a poem.
PAIN has an element of blank;It cannot recollectWhen it began, or if there wereA day when it was not.
It is not uncommon for a patient in acute pain at an emergency visit to seem angry and hostile, but after being relieved of pain the patient returns almost as a different human being. Understanding and empathy are important characteristics for a clinician treating a patient in pain.
Clinical Tips
-
If the patient is a child, a parent or adult must be present to provide the medical/dental histories.
-
If the patient is an adult with difficulty communicating, it is essential that another responsible person be present in order to translate and provide information concerning the medical/dental history.
-
Serious complications may occur due to a language barrier resulting in an incomplete medical history. A specific example of this occurs when a patient or translator fails to communicate information concerning a history of a drug allergy. This error can lead to extremely serious complications.
1.3.2 Patient’s Ability to Identify a Painful Tooth
A clinical study examined 79 endodontic emergency patients. Patients and dentists assessed the level of pain by using a verbal numeric rating scale (VNRS.) Results of that study indicated that patients presenting with odontogenic pain localized the painful tooth 73.3 % of the time. Patients experiencing periradicular pain localized the painful tooth (89 %) of the time, significantly more often than those without periradicular symptoms (30 %, p < 0.0001.) It was concluded that the presence of periradicular pain increases the accuracy of pain localization. The VNRS is highly correlated with other pain scales and is an acceptable initial pain assessment tool for endodontic emergency patients [13].
Patients were frequently able to localize pain to the proper arch. The study found that the pain could be localized in 94.6 % of cases when there was pain to percussion and 90 % (p = 0.60) for an overall arch localization of 92.3 %.
Clinical Tips
-
It is advisable to think in terms of evaluating quadrants of teeth, using multiple tests, in both arches rather than testing only a suspect tooth.
-
Always demonstrate the clinical tests in a normal quadrant before the suspect quadrant is evaluated.
1.3.3 Level of Pain
In assessing pain it is useful to have the patient describe the level of pain on a scale of 1–10. A written scale can be used for the patient to self-assess their level of pain. It is helpful in gauging the patient’s progress or regression, if the patient must return for an additional diagnostic visit.
Some clinicians add descriptors to numbers such as “worst pain imaginable” for number 10 or “barely noticeable” for number 1 and ask the patient to indicate where they fall on that scale (Fig. 1.1).
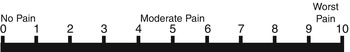

Fig. 1.1
Pain scale
1.4 What Provokes Pain?
It is important to determine what provokes the patient’s pain and medications that provide relief. Understanding when the pain started also provides an important diagnostic clue. For example, pain that started years or months ago and remains at a low level does not fit the common profile of endodontic pain. Pulpal pain when initiated usually increases over a relatively short period of time. A vague response to the question of “What brings the pain on?” should raise doubts about odontogenic causation.
1.4.1 Non-odontogenic Toothache
Non-odontogenic “toothache” is a less common finding than odontogenic toothache. Differentiating odontogenic from non-odontogenic pain can be a challenging process. There are basic steps that can differentiate the site of where pain is experienced from the actual source of pain. Definitive treatment should never be initiated until the source of pain is clearly identified.
Clinical Tips
-
An important clue is the absence of pain when the suspect tooth or quadrant is tested with cold, heat, percussion, and palpation. This clue points the inquiry toward a non-odontogenic cause of pain.
The finding of non-odontogenic pain is often confirmed by the patient’s description of the onset of pain. If the description omits any of the most common causes of dental pain (e.g., thermal sensitivity or pain during mastication), it is another important clue pointing toward non-odontogenic causation. While the precise cause of pain at that stage remains unknown, it is clear that an endodontic dental cause is unlikely.
1.4.2 Non-odontogenic Toothache of Myofascial Origin
A myofascial source may be the cause of a toothache due to referred pain. Myofascial pain is often described as a deep, dull, aching pain that may be associated with referred pain to a tooth. Finger pressure and palpation of a specific myofascial trigger point may result in both muscle and tooth pain. Further tests are then required to identify the primary cause of pain. Palpation of musculature is an essential part of the diagnostic process and is discussed further in Chap. 2. It is not uncommon to find that a patient who has responded normally to sensibility and clinical tests experiences pain on palpation of the musculature.
1.4.3 Maxillary Sinusitis
Non-odontogenic toothache of sinus or nasal mucosal origin may be due to viral, bacterial, or allergic rhinitis and may be expressed as referred pain in the maxillae or maxillary teeth experienced by the patient as a toothache. Bacteria-induced sinusitis pain is often characterized as severe, throbbing pain with a sense of pressure [9].
After a tentative diagnosis of pain due to sinus involvement, it is prudent to refer the patient to a physician for confirmation of the diagnosis and treatment.
Clinical Tips
Findings associated with a diagnosis of pain due to sinusitis:
-
An important diagnostic finding is that more than one tooth may be sensitive to thermal testing and percussion.
-
Teeth test is vital in the suspect quadrant.
-
Maxillary premolars and molars are most commonly affected by sinusitis.
-
Discomfort may be bilateral.
-
Typically, pain and pressure increase as the patient’s head is lowered between their knees.
-
Maxillary local anesthesia may provide partial relief of pain.
-
Sinusitis may be associated with seasonal allergies or upper respiratory infections.
-
An antihistamine may provide relief of pain if the cause is sinusitis.
-
Reduction of pain after intranasal application of a 4 % lidocaine spray has been reported and is considered diagnostic [7].
1.5 Local Anesthesia as a Diagnostic Tool
Local anesthesia can be of great value during the diagnostic process. Anesthetizing a suspect tooth, with a block or infiltration injection, should eliminate pain if the cause of pain is odontogenic.
If pain persists despite symptoms indicating a successful anesthetic block, it is an indication that the cause is not likely to be a tooth in that quadrant. The next step would be to check the opposing quadrant or consider non-odontogenic pain.
In the maxillary arch an infiltration injection can be used to achieve anesthesia, but the clinician must recognize that teeth adjacent to the injection site may also be affected by the anesthetic. If the local anesthetic infiltration fails to eliminate “toothache,” referred pain becomes a more likely diagnosis.
Patients experiencing severe pain or those having a long history of pain prior to the dental visit may have difficulty achieving complete dental anesthesia. Peripheral sensitization of nociceptors and/or central sensitization may be the cause of the problem.
Clinical Tips
-
An incomplete response to a local anesthetic can lead to a diagnostic error.
Although the anesthetic test provides valuable information, false positives are possible. Results of the test must be integrated with other diagnostic data to reach a conclusion about the origin of pain. In maxillary teeth the local anesthetic test provides only an approximation of the origin of pain because multiple teeth may be anesthetized even when intra-ligamental or intraosseous injections are used [10, 18]. The importance of multiple tests and radiographs cannot be overemphasized.
Clinical Tips
-
Spontaneous unprovoked pain may indicate either odontogenic or non-odontogenic pain.
-
Patients should be asked, “Where do you feel pain? Is the pain inside or outside of your mouth?”
-
An indication of non–odontogenic pain occurs when provocation (e.g., application of a cold stimuli or percussion) of the presumed site of pain (the tooth) does not increase the pain.
-
An indication of odontogenic pain occurs when provocation of the presumed site of pain (the tooth) increases tooth pain.
-
A patient may state that “ massaging the jaw” or the area of the temporomandibular joint relieves pain. That would be typical of pain associated with the joint or musculature but is not typical of an endodontic problem.
-
Identification and treatment of myofascial pain may require the assistance of a clinician with advanced training in that area.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


