Fig. 6.1
Glass-ionomer sealant (Fuji IX GP Extra, GC Corp, Tokyo, Japan) on first permanent molar (Courtesy of A/Prof J. Lucas)
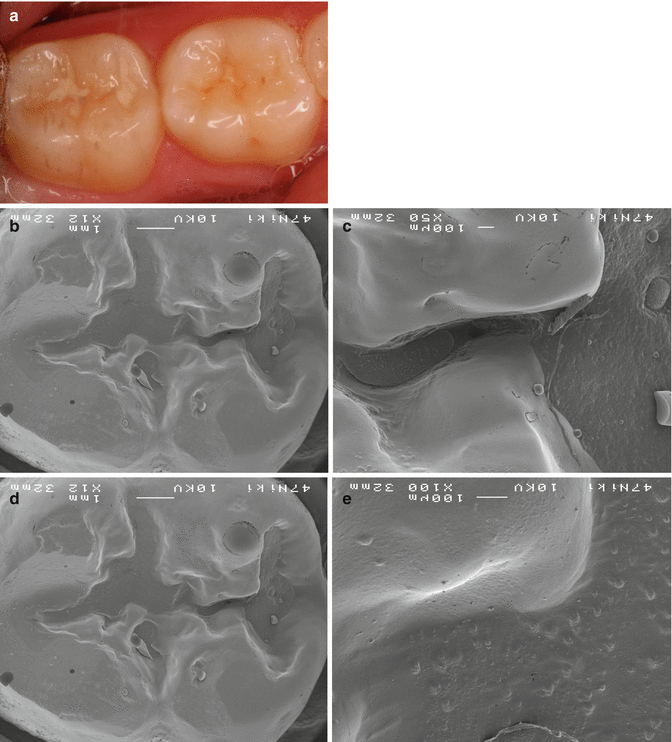
Fig. 6.2
Glass-ionomer cement (Fuji IX, GC Corp) sealant placed on tooth 46 (13 years previously) and tooth 47 (12 years previously). (a) Clinical image of GIC sealant. (b) SEM of resin replica of remnant GIC in 47 fissure (area highlighted in Fig. 6.2a is highlighted here) (×12). (c) SEM of resin replica of remnant GIC in 47 fissure: higher magnification of area outlined in Figs. 6.2a, b (×50). (d) SEM of close surface adaptation of GIC in 47 fissure (×12). (e) SEM of close surface adaptation of GIC in 47 fissure: higher magnification of area outlined in Fig. 6.2d (×100) (Courtesy of Prof J. Frencken)
Whilst resin-based sealants have higher retention rates, this does not necessarily equate to higher rates of caries prevention (Ulusu et al. 2012). Much of the evidence regarding both resin and GIC sealants may be affected by selection and publication bias (Simonsen 1996). The literature does not suggest that there is any difference between the caries-preventive effects of GIC and resin-based fissure sealants (Mickenautsch and Yengopal 2011). When GIC sealants clinically appear partially or totally lost, often the base of the fissures still remains sealed (Mickenautsch et al. 2011). There is evidence to suggest that whilst the bulk of the GIC sealant material placed may be lost within 2–3 years post-placement, newly erupted teeth that are sealed with GIC show a significantly lower dentine caries rate than those that were not sealed (Taifour et al. 2003).
Glass-ionomer sealants have the added benefit that they may be placed outside the traditional ‘dental environment’, as they can be placed with limited dental instrumentation and infrastructure. This may have added benefits in developing countries or for school-based sealant programmes, especially as they can be hand mixed, negating the need for electricity for a triturator or suction and a light-curing unit required for resin-based sealants. However, this is not to suggest that GIC sealants can be placed in an environment heavily contaminated by saliva, as this will reduce the sealing capability and retention rate, although nowhere near the effect contamination has on resin-based sealants – environmental control is still important for GIC sealants (Kulczyk et al. 2005; Farmer et al. 2014).
6.3 Effects on Approximal Surfaces
GIC sealants may have some benefit in promoting remineralisation and inhibiting demineralisation in approximal surfaces. They were shown to be effective as a sealant of approximal white spot lesions after the teeth had been separated to obtain direct access (Trairatvorakul et al. 2011). There is evidence to suggest that fluoride-containing glass-ionomer sealants also provide protection to teeth immediately adjacent to the sealed tooth (Cagetti et al. 2014). It has been reported that the distal surfaces of second primary molars next to first permanent molars sealed with a glass-ionomer have significantly lower levels of carious lesion development than those approximating a first permanent molar sealed with a resin-based material (Cagetti et al. 2014).
6.4 Restorative Care
The atraumatic restorative treatment or ART technique, developed by Frencken and Holmgren, was first published in 1994 (Frencken et al. 1994). This technique allows a carious lesion to be prepared using hand instruments for carious tissue removal and restored using an adhesive material such as GIC. This technique is more often than not carried out without local anaesthetic. The ART technique should be used with careful case selection and is not a gold standard alternative to conventional tooth preparation and restoration where this is available.
This technique may be useful in populations where access to conventional dentistry is not available or in young and uncooperative children where access to general anaesthesia may be limited. A definitive diagnosis must be made before considering whether ART is an appropriate treatment; teeth with signs and symptoms of irreversible pulpitis, or those with lesions that extend to the pulp on radiographs, are not appropriate for this mode of treatment. The extent of the lesion must also be assessed as ART has higher success rates in teeth with single surface lesions compared to multiple surfaces (Frencken et al. 2007). The site of the lesion also has some influence, with survival rates after 6.4 years of non-occlusal posterior restorations reported to be 80.2 %, as compared to 64.8 % for occlusal posterior restorations (Frencken et al. 2007).
Glass-ionomer cement is an ideal material for this treatment as it is relatively cheap and adheres well to the tooth structure and can be hand mixed if necessary, although some would consider the quality of capsule-mixed GIC to be higher than hand mixed. As ART is usually carried out in environments with limited dental infrastructure or in pre-cooperative or uncooperative children, obtaining a retentive cavity preparation or ideal moisture control may be difficult; therefore, GIC becomes a more favourable material compared to resin composite and silver amalgam. However, the clinician should not ignore the effect of good moisture control on the success of GIC restorations. In hot and humid areas, care taken over maintaining ‘normal’ temperatures of the materials should be considered, as setting times and handling characteristics can vary greatly, often to the detriment of the success of the procedure.
6.5 ‘Contemporary’ Carious Tissue Removal
A relatively recent treatment modality in dentistry, which coincides with the increased popularity of ART, is that of a more conservative attitude towards dentine caries removal (Borges et al. 2012). Teeth must be carefully selected for this procedure; clinical and radiographic diagnosis must rule out any signs and symptoms of pulpitis unable to be reversed or the presence of periapical lesions. The technique relies on the removal of the soft infected dentine and recommends leaving a small amount of firmer affected dentine. This serves to preserve tooth structure and to avoid carious or iatrogenic pulp exposure, with improved outcomes in both primary and permanent teeth (Ricketts et al. 2013). The main limitation with this concept is that it is basically impossible to determine what is affected or infected dentine in the clinical situation – and physical features such as hardness or resistance to the excavation instrument should be considered as a primary indicator, although these are also prone to subjective variability. A sound perimeter is required so that a seal can be obtained at the margins, decreasing the chance of leakage and subsequent lesion progression (Fig. 6.3).
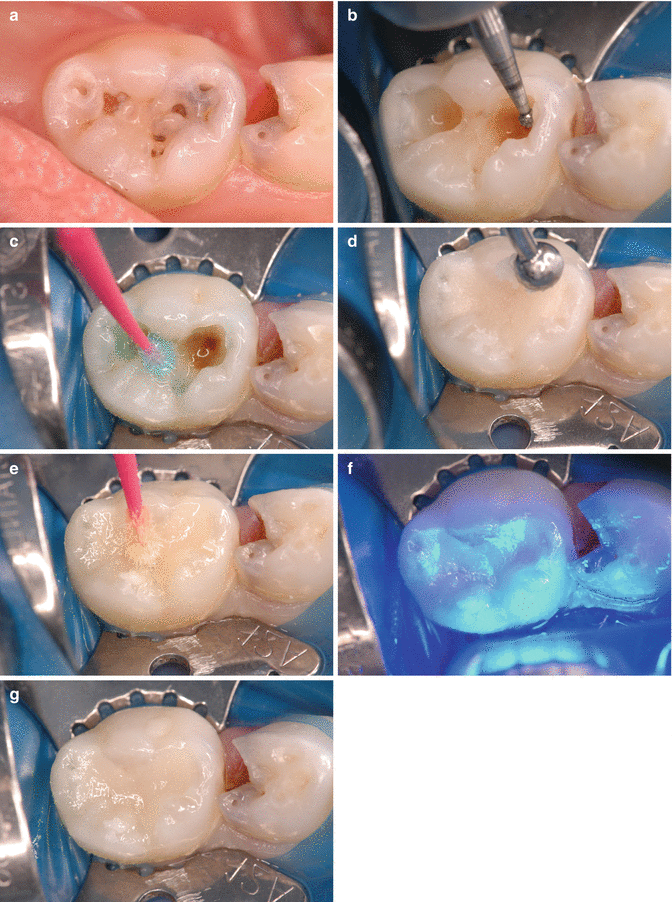

Fig. 6.3
Placement of GIC (Fuji IX) restoration in second primary molar. (a) Occlusal (pit and fissure) carious lesions. (b) Removal of degraded carious tissue. (c) Conditioning of prepared surfaces (note residual hard stained dentine). (d) Placement of GIC restorative (Fuji IX Extra, GC Corp). (e) Placement of resin laminate coating (G-bond, GC Corp). (f) Light-curing of resin laminate coating. (g) Final restoration. Note the carious lesion in the first primary molar. This would be suitable for preformed crown placement luted with low-viscosity GIC over GIC core – with pulp therapy if indicated (Courtesy of A/Prof J. Lucas)
For any restorative technique to be successful, there must be arrest of the carious process, hardening (remineralisation) of the dentine on the cavity floor, and the formation of reactionary dentine to provide protection to the pulp. The material placed over the pulp must provide an adequate seal, and antibacterial properties may be of advantage, although the seal is the primary feature the clinician should seek (Duque et al. 2009). Historically, calcium hydroxide cements have been used for both direct and indirect pulp capping. However, they have some disadvantages such as high solubility and low-compression resistance, and they do not bond well to dentine (Duque et al. 2009). There is now evidence indicating that GICs may assist with the remineralisation process of the affected dentine, due to their antibacterial properties, ion exchange capabilities involving strontium and fluoride, and favourable bonding characteristics to dentine (Duque et al. 2009; Watson et al. 2014). Recently a calcium-based remineralising agent, casein phosphopeptide-amorphous calcium phosphate (CPP-ACP), has been added to a low-viscosity GIC material to increase calcium ion release (Fuji VII EP, GC Corp, Tokyo Japan). However, there is limited evidence whether this material increases remineralisation of dentine due to its high concentration of bioavailable calcium and phosphate. The recent introduction and promotion of a calcium silicate cement (Biodentine®, Septodont, Saint-Maur-des-Fossés, France) as a dentine substitute has created another option for coverage of deep lesions. Recent research indicates that Biodentine may produce better outcomes at 12 months compared with glass-ionomer cement in deep lesions at least three-quarters into the dentine when it is used as an indirect pulp capping material. However, further research with longer-term follow-up and increased subject numbers is needed (Hashem et al. 2015).
Glass-ionomer cements may be used as a conventional restorative material in carefully selected cases. There are several factors that should be considered when selecting a restorative material for the primary dentition. The age of the child and caries risk are the first factors that should be considered, in conjunction with the size of the lesion. Caries risk is often thought of as a static factor; however, it can vary throughout life, so consistent assessment is necessary to allow the clinician to make informed decisions regarding the most appropriate preventive and restorative care of the child. The estimated time until tooth exfoliation is another important factor that varies with tooth type. Location of the lesion to be restored with respect to functional load also influences material selection, and the use of GIC in areas of high loading or in poorly supported multi-surface lesions is often inappropriate.
Glass-ionomer cements are a good base material for two-surface resin composite restorations in children. With options of the ‘open’ or ‘closed’ sandwich technique, this restoration is comprised of a GIC or resin-modified GIC (RMGIC) base that is sealed with a resin composite restoration. The open technique leaves a layer of GIC material exposed at the gingival margin of the approximal box. It is advisable to avoid having GIC at the contact point, due to possible material wear and subsequent loss of arch space. The success of open sandwich restorations has been reported to be high (Atieh 2008). The closed sandwich uses GIC as a dentine seal with resin composite enclosing the GIC. With this technique, the presence of enamel at the gingival floor of the cavity preparation is an advantage as bond strengths are increased and microleakage decreased compared to a dentine margin.
Cavity design is based around removal of soft demineralised necrotic dentine and establishment of a sound perimeter or margin. Currently, there is a lack of evidence-based definitions that relate to the treatment of carious lesions, such as what is ‘hard’ dentine, what is necrotic dentine, how does the clinician identify these conditions and also what a sound margin actually is? Fortunately, the recently established International Caries Consensus Collaboration (ICCC) is establishing guidelines for these often subjective definitions.
It is recommended that after a pulpotomy is performed on a primary molar tooth, a preformed metal crown is cemented with GIC. This provides protection of the remaining structure and a high success rate when compared to an intra-coronal tooth-coloured restoration (Kindelan et al. 2008; Hutcheson et al. 2012).
GICs can be effective materials for the cementation of preformed metallic crowns, which rely on high retentive strength and a good marginal seal to ensure that they are a successful restoration (Yilmaz et al. 2004). Poor seal may lead to the development of biofilm at the margins and subsequent microleakage, both of which may result in the development of a new carious lesion or periodontal complications. Another major issue with the lack of patency of a cement seal is the problem with pulpal health, and leakage increases the chances of pulp inflammation and necrosis, whether a pulpotomy has been undertaken or not. Adhesive cements such as glass-ionomer cements have the advantage of providing a mechanical and adhesive bond between the stainless steel crown and the tooth (Memarpour et al. 2011).
Whilst preformed metallic crowns are the most durable restorations we have in paediatric dentistry, they are still prone to wear due to excessive occlusal forces. With significant wear, areas of the occlusal surface of the crown can be perforated, exposing the luting cement and tooth structure below. In cases where the crown is soundly sealed at the gingival margin and displays no movement or signs of symptoms, one option is for the occlusal surface to be repaired, especially if the tooth is within a few years of exfoliation, with the other option being crown replacement. The material that is chosen to repair the crown must display satisfactory sealing ability to both the crown and the tooth surface, as well as create a seal that will prevent microleakage that can lead to failure of the repair or the crown/pulp complex itself. It has been shown that preformed metallic crowns that have been repaired with a GIC display lower levels of microleakage than crowns that were repaired with a resin composite (Yilmaz et al. 2011). Crown repair would usually be appropriate when the tooth is within a year or two of exfoliating; if the child is younger than this, replacement is more appropriate.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


