Fig. 12.1
Schematic diagram to show how saliva stimulation contributes to the management of dry mouth and also participates in a positive cycle in maintenance of oral health. Saliva coverage of oral mucosa is key to preventing dry mouth. Dry mouth compromises oral health and mastication abilities, including patients’ ability to chew and swallow. Mastication stimulates saliva flow and helps maintain oral health. Good oral health and a preserved dentition lead to good occlusion. This translates to sufficient mastication, thereby creating positive 360° feedbacks. A healthy and functional mouth plays an integral role in saliva secretion
Nonprescriptive Sialogogues as Dry Mouth Treatment
Saliva stimulants, or sialogogues, are treatment options for dry mouth as long as the salivary glands remain functional. Prescription sialogogues, such as pilocarpine and cevimeline, stimulate saliva via muscarinic receptors and the parasympathetic nervous system (Chap. 3). Excess sweating is a common side effect of these drugs because their efficacy is not localized to the oral cavity.
By definition, food is also a sialogogue and can be used as a functional natural stimulant. Chewing gum and lozenges are the two major food products used for this self-care purpose. The mechanism by which chewing gum and lozenges stimulate saliva is also by the autonomic nerve system (ANS). It is indeed the same mechanism by which food stimulates saliva production. While sialogogue drugs stimulate muscarinic cholinergic receptors, nondrug sialogogues stimulate the ANS via taste receptors and periodontal mechanoreceptors. Among the five basic tastes, sourness, saltiness, and sweetness are the most potent drivers for salivation in that order. Mechanical stimuli are derived from the physical properties of the food bolus, such as hardness, elasticity, and bolus size. Large cohort studies on normal salivators found the average unstimulated salivary flow rate to be 0.3–0.4 mL/min [5]. This value increases about tenfold with oral stimuli. The taste stimulus diminishes as subjects swallow the dissolved tastants in saliva, while the magnitude of stimulation is greater than with mechanical stimulation. The taste receptors are adaptive to gustatory stimuli [6]. The halftime for adaptation, measured by salivary flow rate, is about 11 s if the source of the stimuli is not moved around in the mouth. The adaptation for taste stimuli falls exponentially and is not dependent on the type of stimulus. In contrast, mechanical stimuli usually cause a lower magnitude of saliva secretion, but it lasts as long as the subject keeps chewing the oral composition in their mouth.
Figure 12.2 illustrates salivary secretion by three types of food substances, that is, chewing gum, lozenge, and gum base, the latter being the elastic substance of chewing gum without sweetener or flavor. Saliva stimulation by chewing gum peaks in the first 1–2 min, reaching about a tenfold increase from the unstimulated salivary flow rate, and then gradually declines to about twice the unstimulated salivary flow rate [7, 8]. This is because the combination of gustatory and masticatory stimuli takes place at the beginning of chewing and the stimuli from sweeteners or acids decrease as they are extracted from chewing gum and then swallowed. The lozenge stimulates saliva via taste receptors. Its effect diminishes as it dissolves and the tastants are swallowed; therefore, the salivary flow rate goes down to the unstimulated level. Gum base stimulates saliva via mechanical stimulation when it is chewed. The magnitude of its stimulation is not as potent as with taste stimuli. However, the effect lasts as long as the patient keeps chewing the gum base. The combination of flavor and sweetener, and also the presence of organic acids, influences the flow rate and pH level of chewing gum-stimulated saliva [9, 10]. The size of bolus is also a factor in salivary stimulation, for example, chewing 1 g of taste-free and flavor-free gum base leads to about a fourfold increase in flow rate, whereas a 9 g piece leads to a 13-fold increase [11].
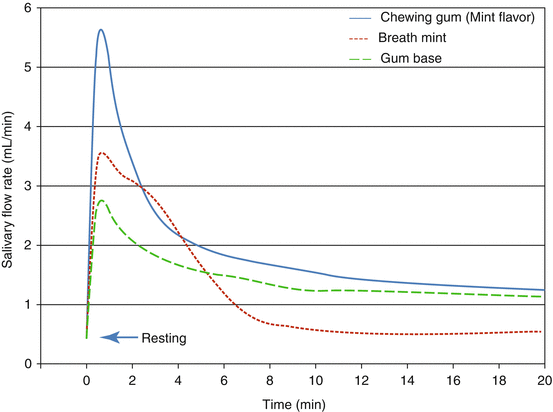

Fig. 12.2
Salivary flow rate stimulated by different oral compositions
The increase in the amount of saliva is not the only mechanism by which these food products work against dry mouth symptoms. Saliva is composed of 99.5 % water with 0.2 % protein and 0.3 % inorganic substances. These relatively small fractions of constituents are critical for saliva’s functions. For example, rinsing the mouth with pure water does not provide the same level of dryness relief as saliva stimulants [12]. The main mechanism is the increase in salivary components that deliver protective functions for the oral cavity. Saliva contains mucins and other glycoproteins that maintain the homeostasis of the mouth, including lubrication and coating of the oral mucosa.
Saliva covers oral surfaces as a thin film which has a higher protein content than the secreted whole saliva. MUC5B, a large-molecular-weight mucin, has been found to be present at a lower concentration in the salivary films of dry mouth patients compared with those from normal salivators [13]. Minor gland saliva, which is rich in mucin content, is considered to play a critical role in coating oral surfaces. In fact, minor salivary gland secretion has a higher correlation with dry mouth symptoms than that of chewing-stimulated whole saliva [14]. Both saliva substitutes and sialogogues focus on maintaining lubrication in the oral cavity to reduce discomfort as well as the dryness of the mouth. The shared advantages of these treatments are the ease of use and localized effect. Artificial saliva contains lubricating macromolecules as substitutes for these glycoproteins. By increasing salivary flow rate, sialogogues also increase specific protein output, that is, the amount of protein secreted per minute increases. Artificial saliva (Chap. 11), in the form of an oral spray, is often presented as a treatment option along with chewing gum. As such, many studies have looked into the efficacy of chewing gum, sucking hard candy, or using artificial saliva, not only for the effectiveness of the treatments but also for patients’ preferences.
Multiple studies have shown consistently that chewing flavored and sweetened gum increases salivary flow rate and provides relief from dry mouth symptoms, as long as the subjects keep chewing. Chewing the sugar-free gum promoted the saliva’s protective function and prevented the fall in cemental plaque pH in response to a sucrose challenge [15, 16]. These effects were consistent for patients with various etiologies of dry mouth [3, 5, 17–24]. For example, patients who suffer from end-stage renal disease have higher risk of dry mouth. This is because patients receiving hemodialysis need to restrict fluid intake, which reduces salivary flow and thus causes chronic thirst and dry mouth. Bots et al. conducted a crossover clinical trial using two chewing gum formulae and also artificial saliva. The results suggested that both chewing gums and artificial saliva were effective in the reduction of dry mouth as well as thirst [23].
Some studies compared multiple chewing gum formulae for their efficacy and saliva stimulation. The majority of gum products used in the dry mouth studies were sugar-free and formulated with active ingredients such as xylitol, chlorhexidine, or urea for dental benefits. One study compared the efficacy of two chewing gums with one formulated with mucin and the other with urea. The mucin gum was perceived more effective for self-perceived dry mouth symptoms compared with urea gum. The subjects also liked the mucin gum better and used it more frequently than urea-containing gum upon ad libitum administration in a 2-week-long crossover trial [22]. No study reported statistical difference among multiple chewing gum formulations compared in terms of salivary flow rate. This was not surprising as these active ingredients were not expected to stimulate salivary secretion. There was a trend that gum containing actives, for example, chlorhexidine, showed additional dental benefits such as lower plaque and gingival indices. To our best knowledge, there has been no dry mouth study conducted using a chewing gum product specifically formulated to maximize salivary flow rate. Organic acids are potent salivary stimulants commonly used in fruit-flavored chewing gums. Organic acids, such as citric and malic acids, are also naturally present in fruits and other foods. Fruit-flavored gums have shown to increase salivary secretion more than mint-flavored gum [25]. However, there appears to be no study using fruit-flavored chewing gum for dry mouth. On the other hand, the same organic acids are formulated in lozenges and citrus candies. These confections are also effective in stimulating saliva and thus relieving dry mouth symptoms although for a shorter duration than chewing gum (see Fig. 12.2) [12, 26, 27]. When consuming acidic food, it is important to maintain the hydrogen ion concentration in saliva in order to minimize the risk for acid enamel loss. This is particularly critical for hyposalivators as the rate of acid clearance by saliva is lower than in normosalivators. Salivary flow rate is positively correlated with acid clearance rate and also the bicarbonate ion concentration. Patients’ ability to secrete stimulated saliva needs to be taken into account when recommending a nonprescriptive sialogogue. It is also recommended to focus on acid clearance and refrain from brushing teeth for at least half an hour after consuming acidic food, including fruits.
Patients’ Preferences on Products
For all three nonprescription treatments (i.e., chewing gum, lozenges, and artificial saliva), their mode of action is to lubricate the oral mucosa.
All products in these three categories are acceptable forms of treatment, although there may be a preference for one treatment over another based on individual patient’s conditions [28]. The drivers for the preference include (1) ease of use, (2) effect in relieving dry mouth symptoms, and (3) taste acceptability (Table 12.1). Side effects also influence the preference of patients (Table 12.2).
Table 12.1
Reasons to prefer one product over the other
|
Chewing gum
|
Artificial saliva
|
|---|---|
|
More effective
|
More effective
|
|
Liking of taste
|
Did not like chewing
|
|
Easier to use
|
Liking of taste
|
|
Fewer side effects
|
Easier to use
|
Table 12.2
Common complaints and side effects associated with nonprescription remedies
|
Chewing gum
|
Artificial saliva
|
|---|---|
|
Irritation of mouth
|
Unpleasant taste
|
|
Nausea
|
Nausea
|
|
Unpleasant taste
|
Irritation of mouth
|
|
Jaw discomfort
|
Vomiting
|
|
Biting cheek or tongue
|
Diarrhea
|
|
Sensitive teeth
|
|
|
Flatus
|
Some studies evaluated subjects’ liking of the flavor or the taste of the tested products. While liking may not provide a short-term clinical advantage for alleviating dry mouth symptoms, the long-term benefit may be that subjects who use sialogogues with higher liking may (1) be more compliant with the treatment procedure and thus more likely to increase the chance of successful treatment and (2) use the product for longer periods, resulting in prolonged stimulation time [17]. There is a reported trend that the more unstimulated salivary flow the patient has, the more likely that they are to prefer chewing gum over artificial saliva. For example, 60 % of tested subjects expressed their preference for chewing gum over artificial saliva in a study with patients on hemodialysis therapy [23]. These patients have several oral complications, including dry mouth, while having functional salivary glands but impairment in renal functions.
Specific Advantages of Different Treatment Options
In addition to the shared advantages, artificial saliva has a distinct advantage in that it may be used by those who do not have sufficient salivary gland function for stimulation of saliva flow (see Chap. 11 for more details about artificial saliva). On the other hand, there are two unique advantages in using sugar-free chewing gum as a sialogogue: (1) It increases salivary pH as well as buffer capacity. It also neutralizes plaque acid created by starchy food, thus enhancing the remineralization potential of dental plaque. (2) The effect lasts much longer because the masticatory stimuli remain effective as long as one keeps chewing the gum cud. To be more precise, this effect lasts as long as the bolus maintains sufficient textural properties to stimulate saliva flow. One study showed the stimulated salivary flow being significantly higher than that of unstimulated throughout a 2 h chewing period using chewing gum with 2.7 g starting weight [7]. Another study found the stimulated salivary flow rate was significantly higher than that of unstimulated for the first 55 min of 90 min chewing, using a smaller gum pellet of 1.5 g [8]. Obviously, this increase in salivary flow rate disappeared when subjects stopped chewing. However, the level of salivary flow just after chewing is stopped is equivalent to the unstimulated flow rate but not lower [29]. In addition, the initial increase in salivary flow rate can be reproduced at least every 90 min if subjects start chewing a fresh piece of gum.
The Importance of Unstimulated Saliva
Although the stimulated salivary flow rate is significantly higher than that of the unstimulated, the oral cavity is mostly exposed to unstimulated saliva, both in terms of the amount and duration. The total volume of saliva for a normal salivator adds up to 500–600 mL/day, of which unstimulated saliva contributes about 340 mL. This comes from 300 mL during the waking period at 0.3 mL/min for 16 h and about 40 mL during sleep at less than 0.1 mL/min for 7 h. The total amount of daily stimulated saliva is estimated to be about 200 mL. The average time spent eating each day has been estimated as 54 min, and the average stimulated flow rate during a meal is estimated to be about 4 mL/min [5].
There are characteristic differences between stimulated saliva and unstimulated saliva. The ratio of the contributions from the different glands changes when saliva is stimulated. In unstimulated saliva, the contribution from amylase-rich serous parotid glands is about 25 %, about 70 % is from mucin-rich viscous submandibular and sublingual gland secretions, and 7–8 % is from mucin-rich minor glands. On the other hand, stimulated saliva is composed of about 50 % parotid saliva, 45 % submandibular-sublingual saliva, and 7–8 % minor gland saliva. This aligns with the main functions of both saliva types, that is, the digestive function of stimulated saliva and the lubricating and protective function of unstimulated saliva. Saliva from minor glands should also be considered, as these viscous secretions have a high impact on dry mouth.
Another reason why unstimulated saliva is important is because saliva lubricates and coats oral mucosal surfaces. As mentioned earlier, the protective property of saliva is exhibited as the thin film layer coating the mucosal surface. Hyposalivators whose unstimulated salivary flow rate <0.1 mL/min had significantly lower mucosal thickness of saliva compared with normosalivators. Normosalivators with dry mouth symptoms also showed thinner salivary film compared with the saliva sampled from normosalivators without the symptoms. The differences among three groups were most prominent at specific sites, namely, the tongue, lips, vestibule, and mouth floor. Considering the flow of saliva in the oral cavity, increasing parotid secretion should contribute to increased wetness of the cheeks, whereas an increase in submandibular-sublingual secretions should contribute to wetness at the floor of the mouth (Fig. 12.3) [30]. The flow schematic also infers that lubrication of lips and vestibule is more dependent on the minor salivary glands, rather than, for example, the parotid glands.
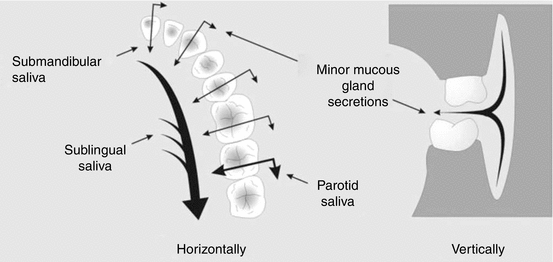

Fig. 12.3
Schematic of salivary flow in oral cavity (Reprinted with permission from [31]). The saliva film moves in a general direction from the upper anterior buccal side to the lower posterior lingual side and then gets swallowed. The velocity of the film increases while traveling through the oral cavity. The thickness of the film has been calculated to average just less than 0.1 mm in the mouth, and an increase in saliva from various glands results in increasing velocity of the film. Another noteworthy point is that saliva secreted on one side tends to remain on the same side and does not migrate evenly around the whole mouth [32]
The fact that unstimulated saliva bathes the floor of the mouth and tongue has implications for taste perception. Dry mouth patients often notice that their taste perception alters after onset of the symptoms (Chap. 5). Taste receptor cells are regenerated and replaced on average every 10 days [33]. This suggests that without saliva protecting the taste cells, the number of taste receptors may not keep up with the turnover and thus the taste sensitivity may decline. Animal studies support this hypothesis. Rats show a decreased taste nerve response upon the elimination of the submandibular and sublingual glands. The sensitivity improved within the same animals after 1 week of treatment with artificial saliva.
In elderly adults, there was a positive correlation between the flow rate of unstimulated saliva and that of stimulated saliva [32, 34]. This implies that improving the unstimulated salivary level will increase the degree of relief delivered by an oral sialogogue.
Maintaining an unstimulated salivary flow rate sufficiently high to coat the oral cavity is one very important approach to preventing dry mouth. There are relatively few studies which have evaluated the drivers for unstimulated saliva flow aside from cholinergic agonists such as pilocarpine.
Regular Chewing and Salivary Secretion
While the increase in saliva during chewing is well established, the question remaining to be answered is: “Will a regular chewing habit increase salivary secretion and improve dry mouth symptoms within the same individual?” This question is critical, not because higher salivation means lack of a dry mouth, but because increase of salivation in the same individual is important for an individual’s perception of oral dryness. For example, dry mouth patients’ subjective symptoms recurred when unstimulated whole saliva flow rate fell to about 40–50 % of the flow rate induced by anticholinergic drugs [35]. Animal and epidemiological studies suggest that masticatory stress positively correlates with salivary secretion. One study showed positive correlations between the unstimulated salivary flow rate and (1) frequency of gum chewing, (2) number of pieces per day, and (3) the duration of each chewing episode [36]. These subjects were stratified with age, gender, and dietary pattern. There are several animal studies on saliva secretion and regular mastication, the latter being altered by changing food texture [35]. Salivary output decreases with reduction in masticatory stress and causes reduced flow rate of parotid saliva in humans. A liquid diet causes parotid gland atrophy and reduction in parotid salivary flow in rats.
Several intervention studies investigated salivary output after the long-term use of chewing gum or lozenges for both dry mouth patients and also normal salivators (Table 12.3). Overall, intervention studies with a planned regular chewing pattern show inconsistent outcomes in whether a regular chewing gum habit increases salivary flow rate. This is possibly due to difference in the output measures between the studies, that is, unstimulated salivary flow or that of mastication stimulated with paraffin or acid. Caution is needed as there is a large variation in the duration and frequency of consumption in the various studies. The subject groups also varied among the studies, from healthy young students to frail institutionalized elderly in whom the masticatory stress would be different when chewing a piece of gum. Other factors, such as compliance rate and saliva sampling timing (see below), further complicate the outcome.
Table 12.3
The impact of regular chewing on salivary secretion
|
Subject group
|
Intervention
|
Subject number
|
Duration
|
Frequency
|
Outcomes after intervention
|
Ref
|
|---|---|---|---|---|---|---|
|
Community-dwelling elderly
|
Sugar-free gum vs. no gum
|
N = 91 and 95
|
6 months
|
Twice a day for 15 min
|
No significant change in paraffin-stimulated salivary flow rate
|
[19]
|
|
Average of 20 natural teeth
|
Parallel, randomized
|
Gum group showed a reduction in plaque and gingival indices
|
||||
|
Wide variance in compliance rate
|
||||||
|
Chronic dry mouth patients
|
Chewing gum, sour lemon lozenge, and sweetened artificial saliva spray
|
N = 80
|
2 weeks
|
Ad libitum (max 10 lozenges a day)
|
No significant increase in paraffin-stimulated salivary flow rate for any of the three products
|
[27]
|
|
No difference in terms of the patients’ preference among three options
|
||||||
|
Subjective and objective dry mouth patients
|
4 lozenges, 1 chewing gum, and 3 artificial saliva types
|
N = 106
|
2 weeks
|
Not regulated
|
None of 8 products caused a significant increase in paraffin-stimulated whole saliva secretion
|
[26]
|
|
Randomized, crossover
|
Chewing gum and acid-containing lozenge were among the most preferred products, based on patients’ ratings
|
|||||
|
Elderly in retirement homes
|
Chewing gum vs. no gum
|
N = 31–43
|
1 year
|
Twice a day for 15 min
|
Gum group increased paraffin-stimulated salivary flow rate over baseline
|
[20]
|
|
Parallel
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


