Introduction
The development of incipient caries, or white spot lesions (WSLs), is a significant clinical problem in orthodontics. The purpose of this study was to retrospectively determine the incidence and severity of WSLs by examining pretreatment and posttreatment digital photographs.
Methods
A total of 332 consecutive finished patients from a university graduate orthodontic clinic were evaluated. Initial and final digital images were compared to assess WSLs. The facial surfaces of the anterior 8 maxillary teeth were analyzed. The percentage area of WSL per total facial tooth surface was calculated to control for magnification differences. Reliability of the method was assessed by comparison with direct clinical examination data. Patient and operator factors, and treatment complexity and outcomes were evaluated as predictors of WSL incidence and severity.
Results
Agreement between direct clinical examination and digital photo data was excellent, with an intraclass correlation coefficient 0.88 and a 0.3% average difference between methods. The incidence of at least 1 WSL on the labial surface of the anterior 8 maxillary teeth was 36%. The order of incidence was lateral incisor (34%), canine (31%), premolar (28%), and central incisor (17%).
Conclusions
Risk factors for the development of incipient caries during orthodontic treatment were young age (preadolescent) at the start of treatment, number of poor hygiene citations during treatment, unfavorable clinical outcome score, white ethnic group, and inadequate oral hygiene at the initial pretreatment examination. The use of computer software to evaluate digital photos retrospectively is a valid method for assessing the incidence and severity of WSLs on the maxillary anterior incisors, canines, and premolars.
Dental caries starts on an enamel surface when there is a shift in equilibrium between demineralization and remineralization. The formation of incipient caries, commonly called white spot lesions (WSLs), is an unesthetic, common side effect of orthodontic treatment with fixed appliances. Bands and brackets increase the retention of plaque and food on smooth tooth surfaces that would otherwise tend to have a low prevalence of caries. Despite intensive efforts to educate patients about effective oral hygiene procedures, enamel demineralization associated with fixed orthodontic appliances remains a significant clinical problem.
A review of literature in 2005 showed great variations, from 2% to 97%, for WSL prevalence associated with orthodontics treatment. Much of the variation in detecting WSLs relates to analytical methods. The highest prevalence of demineralization was detected by quantitative light-induced fluorescence, a method that is much more sensitive than direct visualization. Studies are comparable only when the analytic methods are similar.
The reported incidence and prevalence of WSLs vary by sex: 1 study found that female patients have a higher incidence of WSLs, another found no significant difference in WSL prevalence, and a third study found that male patients have a higher incidence of WSL. No significant differences were found in WSL incidence and prevalence between the right and left sides of the maxilla and mandible. The frequency of WSLs on the maxillary incisors, canines, and premolars in orthodontically treated patients were lateral incisors >canines >first premolars >second premolars >central incisors. These data are consistent with a previous report, except that the maxillary central incisor had a greater frequency of WSLs than did the maxillary second premolars. This study concluded that there was no difference in the incidence of WSLs relative to treatment time: 12 to 16 months vs up to 36 months for banded or bonded teeth.
The objectives of our study were to retrospectively evaluate the incidence and severity (surface area) of WSLs at the time of fixed orthodontic appliance removal with routine digital photographs, and to determine whether treatment and patient variables affect the incidence and severity of WSLs in patients treated with fixed appliances.
Material and methods
This study was approved by the Research Compliance Administration (IRB-04, study 0801-11) of Indiana University. Digital photos of patients finished during 2 consecutive years in the graduate orthodontic clinic at Indiana University were evaluated. In contrast to previous prevalence studies that determined demineralizations at the end of treatment, we studied the incidence of demineralizations during treatment because it was controlled with pretreatment photographs. A total of 332 patients were sampled in the 2006 and 2007 academic years. All consecutively finished patients were included except for those with poor quality or inadequately angled digital photographs, incomplete records, limited treatment or retreatment, lingual fixed orthodontic appliances, clear aligner treatment, missing teeth (eg, lateral incisors or canine substitutions), and facial restorations on the crowns of teeth being evaluated.
Patients applying for orthodontic treatment were required to present a signed letter from their dentist confirming periodontal health and no caries. At the initial screening examination, oral hygiene, gingival color, and response to brushing were evaluated. Patients with 1 bleeding site after brushing were assessed as having fair oral hygiene. Two or more bleeding sites were classified as poor hygiene. Patients in the fair and poor categories (inadequate oral hygiene) were informed that they must correct the deficiency before the pretreatment records appointment, or they would be dismissed. Oral hygiene was monitored and recorded at each appointment during active treatment, and oral hygiene instruction was provided when necessary. A fluoride toothpaste and mouth rinse were prescribed for all patients, but they were not provided. Hygiene instruction given as needed was the only preventive measure. At appliance removal, adhesive was removed with a carbide finishing bur, and complete removal was verified by air drying the teeth.
Routine clinical photographs were collected based on the series recommended by the American Board of Orthodontics. All examinations, scorings, and calibrations were done by 1 examiner (J.A.C.) under the direct supervision of the principal investigator (W.E.R.). Initial and final photos were compared and recorded for the presence of WSLs. Environmental and developmental alterations such as enamel hypoplasia, fluorosis, stains, and demineralization sites on teeth before orthodontic treatment were not scored. Scoring was done with the computer software program Image J (version 1.39, National Institutes of Health, Bethesda, Md) and the Wacom Intuos3 professional pen tablet (Saitama, Japan). The facial surfaces of the anterior 8 maxillary teeth (first premolar to first premolar, or to second premolars if the first premolars were missing) were evaluated for WSLs ( Fig 1 ). Photographs were assessed in random order for visually detectable WSLs. Teeth identified as having WSLs had their total facial surfaces and lesion areas outlined with the pen tablet, and the respective areas were calculated with Image J software ( Figs 2 and 3 ). The area of the WSL was divided by the area of the total facial surface of the tooth to calculate the percentage of the facial surface affected. Teeth without WSLs were recorded as a zero percentage. The percentage of WSL per total facial tooth surface provided a relative value that controlled for differences in magnification of the digital photos.
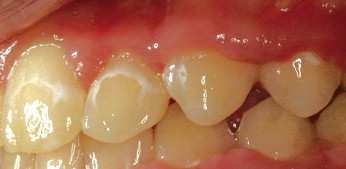
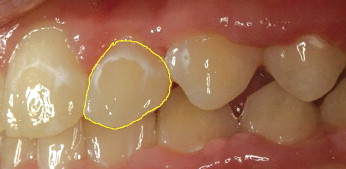

To determine the relative sensitivity of the photographic method, 10 randomly selected patients were examined clinically at their appliance removal to record the presence of WSLs. Total facial surface and WSL areas were manually outlined twice with write-on overhead transparency film for the maxillary anterior 8 teeth. The same procedure was used on the clinical photographs taken at the appliance removal appointment. The outlines of the total facial surface and WSLs were digitized. Image J software was used to calculate the percentages of the facial surface affected by WSLs by using both direct (clinical) tracings and indirect (photographic) images. To determine incidence, only WSLs occurring during the specified treatment interval were quantified. To determine repeatability, Image J software was used to calculate the percentage of the facial surface affected by WSLs on 2 occasions, a week apart. This calibration was used to assess the repeatability and agreement between digital photos for evaluation of WSLs and the gold standard, which is direct clinical examination.
A waiver of consent and authorization was obtained in accordance with the IRB-04, study 0801-11, guidelines for the clinical examinations of patients and the retrospective reviews of patient records. Patient records and treatment notes were reviewed to evaluate these categories: patient demographics, patient factors, and operator factors. Table I lists these variables by category.
| Category | Variable evaluated |
|---|---|
| Patient | Sex: male or female |
| Demographics | Ethnicity: white, black, Hispanic, Asian, or other |
| Age of patient at start (mo) | |
| Patient factors | Pretreatment oral hygiene: good, fair, or poor |
| Treatment duration (mo) | |
| Number of active treatment appointments | |
| Number of missed appointments: failed or canceled | |
| Number of repairs or emergencies | |
| Number of negative oral hygiene entries | |
| Number of negative compliance entries Early debond (premature termination): yes or no |
|
| DI score OGS score CCA score OGS and CCA combined score |
|
| Operator factors | Number of residents providing treatment |
| Type of bracket: conventional metal, self-ligating, or ceramic Number of treatment phases (1 or 2) |
|
| Number of months and percentage of treatment time in elastomeric chain: minimum of half of the teeth involved (mo) |
The American Board of Orthodontics’ occlusal grading system (OGS), the discrepancy index (DI), and the comprehensive clinical assessment (CCA) were recorded. The OGS assesses treatment outcomes by scoring posttreatment dental casts and panoramic radiographs. The CCA was developed to supplement the OGS, by evaluating compliance, records quality, facial and dental esthetics, vertical control, arch form, periodontium management, root resorption, and treatment efficiency. Elevated OGS and CCA scores indicated a poor treatment outcome, whereas lower scores indicated a more favorable treatment outcome. Pretreatment dental casts and lateral cephalometric radiographs were used to determine the DI as an assessment of malocclusion complexity. A high DI score indicates a more complex pretreatment malocclusion and vice versa.
Statistical analysis
Repeatability of the WSL area measurements was assessed by using intraclass correlation coefficients (ICC). The percentage of tooth surface area covered by a WSL was determined for each tooth. The percentages were averaged for each of the 8 teeth. The percentage of tooth surface area covered by WSLs was also categorized as zero (no WSL on any teeth), average area <10%, or average area >10%. Each predictor was examined individually for an association with WSL area, presence of any WSL, and categorized WSL area by using linear regression, logistic regression, and cumulative logistic regression, respectively. For each of the 3 outcomes, a stepwise variable selection procedure was used to develop a parsimonious multiple-variable prediction model. The significance level for entry and removal from the models was 5%.
A secondary analysis compared the teeth for differences in WSL to evaluate whether certain teeth were more likely to have WSLs or to have more area covered by WSLs. WSL areas were compared by using mixed-model analysis of variance (ANOVA) to account for the correlations among teeth from the same patient. Comparisons for the presence of any WSL were made with the generalized estimating equation methodology applied to logistic regression to account for the correlations among teeth from the same patient.
Results
The repeatability for the clinical examination had an ICC of 0.97 with an average difference between the first and second scores of 0.006% for the area of WSLs. Replication for the digital photo examination had an ICC of 0.98, with an average difference between the first and second scores of 0.004. In comparing the clinical and digital photo examinations, the ICC was 0.88, with an average difference between the clinical and digital scores of 0.003. The only discrepancies were 3 small lesions found on the digital photos that were not seen during the clinical examinations, and 2 small lesions found in the clinical examination that were not confirmed with the digital photo. A histologic examination of extracted or exfoliated teeth would be needed to determine which method was correct for these minor discrepancies.
The average WSL covered 9.8% of the total facial surface of the affected tooth ( Table II ). The central incisors had significantly less mean WSL area than the other teeth ( P <0.001), the premolars were significantly less affected than the lateral incisors and canines ( P <0.001), but the lateral incisors and canines were not significantly different ( P = 0.46).
| WSL area | Any WSL | ||||
|---|---|---|---|---|---|
| n | Minimum | Maximum | Mean (SD) | n (%) | |
| All teeth ∗ | 332 | 0 | 38 | 3.5 (6.6) | 118 (36) |
| Teeth with WSL | 118 | 1 | 38 | 9.8 (7.9) | — |
| Right-side teeth | 332 | 0 | 41 | 3.5 (6.8) | 116 (35) |
| Left-side teeth | 332 | 0 | 39 | 3.4 (6.6) | 103 (31) |
| Central incisors | 332 | 0 | 43 | 1.9 (6.0) | 56 (17) |
| Lateral incisors | 332 | 0 | 40 | 4.5 (8.2) | 113 (34) |
| Canines | 332 | 0 | 55 | 4.3 (8.7) | 103 (31) |
| Premolars | 332 | 0 | 37 | 3.2 (6.7) | 94 (28) |
The incidence of at least 1 WSL in the maxillary anterior 8 teeth was 36% ( Table II ), with 22% having WSL areas <10% and 14% having WSL >10%. The central incisors had significantly lower proportions of teeth with WSL than did the other teeth ( P = 0.0001), followed by the premolars ( P = 0.07, vs the canines, P <0.001, vs the lateral incisors), canines, and lateral incisors ( P = 0.012, canines vs the lateral incisors) ( Table II ). There was no significant difference in WSL incidence when the right and left sides were compared.
The characteristics of the 332 patients are detailed in Tables III and IV . The sample was 62% female and 73% white. Ethnicity was collapsed into white and not white for the analyses. The average starting age was 16.2 years (range, 8-56 years). Mean treatment duration was 32 months, including patients in the mixed dentition, those who were partially edentulous, and those needing multi-phase treatments. Seventeen percent of the sample had premature termination of treatment (early debond). At the pretreatment screening, 55%, 36%, and 8% had good, fair, and poor hygiene, respectively. All patients entering treatment were required to have good hygiene before the fixed appliances were placed. The sample included 87% conventional metal brackets, 8% ceramic brackets, and 5% self-ligating brackets. The conventional metal brackets were compared with the combined ceramic and self-ligating groups in the analyses.
| n | Minimum | Maximum | Mean (SD) | |
|---|---|---|---|---|
| Treatment duration (mo) | 332 | 6 | 81 | 32 (13.6) |
| Age at start (y) | 331 | 8 | 56 | 16.2 (8.7) |
| Residents providing care | 332 | 1 | 7 | 2.6 (1.2) |
| Months in elastomeric chain | 332 | 0 | 21 | 3.2 (3.1) |
| Time in elastomeric chain (%) | 332 | 0 | 71 | 10.9 (10.0) |
| Active treatment appointments | 332 | 5 | 61 | 23.8 (9.7) |
| Missed appointments | 332 | 0 | 37 | 3.7 (4.4) |
| Emergency/repair appointments | 332 | 0 | 13 | 1.8 (2.0) |
| Appointments with poor oral hygiene | 332 | 0 | 15 | 2.0 (2.7) |
| Appointments with poor compliance | 332 | 0 | 10 | 1.4 (1.9) |
| OGS score | 332 | 2 | 79 | 27.8 (10.4) |
| CCA score | 332 | 1 | 19 | 6.1 (3.3) |
| Total score | 332 | 4 | 93 | 33.9 (12.4) |
| DI score | 332 | 1 | 57 | 15.6 (8.9) |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


