Fig. 29.1
(a, b) Side-cutting burr and the external-extended corticotomy from the free mandibular border to the gonial angle. The corticotomy is interrupted as soon as the cancellous bone is visible. (b) At the lingual cortex, the bone cut is incompletely, preserving 6–7 mm of the internal cortical flayer at the site of the neurovascular bundle
Afterward, a flexible unidirectional external device (KLS-Martin, Germany) is inserted. Two titanium pins are introduce percutaneously through the whole thickness of the mandible, 4–5 mm in front and behind the corticotomy. The pins should be parallel to each other to facilitate the fixation of the distraction device. In this moment, we recommend an “intraoperative test” of accuracy: activate the device 5–6 mm and observe the changes in the corticotomy. The surgeon must obtain the opening of the corticotomy segments without difficulty and assess that the elongation system works properly. If the surgeon identifies the presence of cortical bridges, the lengthening mechanisms will not work and the corticotomy must to be revised.
The advantage of combining the use of an external corticotomy and a flexible device is the ability to obtain a 3D correction of height, length, and position of the mandible. In fact, different zones of bone resistances are encountered, minor of the angle but major resistance at the alveolar ridge, that will be elongated differently under a perpendicular distraction vector (Fig. 29.2a–c).
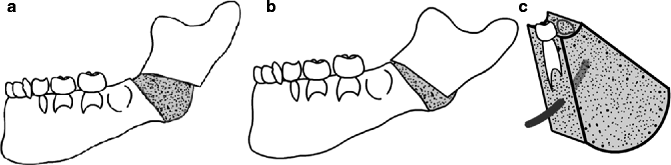

Fig. 29.2
(a) Location of the corticotomy in a grade II-A hemifacial microsomia. (b) Using an oblique vector, the new bone formation production is larger at the angle and minor at the alveolar ridge, also at the initial portion of the ascending ramus. (c) Tridimensional diagram of the regenerate bone. The new volumetric bone formation corrects the height, the length, and position of the mandible. The tooth buds and neurovascular elements have been preserved
The area of new bone formation produces a better shape of the mandibular angle and modifies the ascending ramus position with a simultaneous better relationship of the condyle and the glenoid fossae. The initial condyle lateral position moves into a more central one that is more similar with the contralateral normal one. All of these findings are different from those obtained with linear distractors and osteotomies.
The selection of the vector of distraction is also a critical decision. The corticotomy and the position of the pins determine the distraction vector. It is different in each patient depending on the grade of mandibular hypoplasia. In patients with grade I, the pins must be placed perpendicular to the corticotomy, obtaining an oblique vector that produces a larger bone elongation in the angle and a minor bone elongation in the alveolar ridge. In patients with grade II-A hypoplasia, the distraction process must remodel and elongate the angle and the initial portion of the ascending ramus (Fig. 29.3). For this reason, the pins must be inserted in an intermediate position between a vertical and oblique distraction vector. This group of patients represents the vast majority of our clinical series.
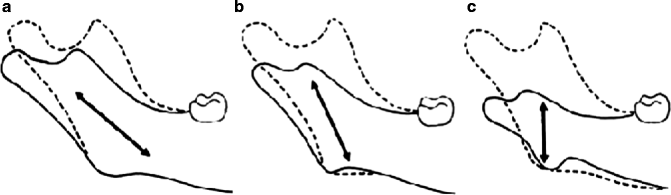

Fig. 29.3
Distraction vectors are the key to obtaining excellent results. Basically, three distraction vectors are used to correct a mandibular hypoplasia in hemifacial microsomia. The oblique vector is used for grade Pruzansky I, and the vertical vector is used to recreate the ascending ramus in the grade Pruzansky II-B
In patients with grade II-B hypoplasia, the corticotomy is placed horizontally in the base of the ramus. The pins must follow a strict vertical distraction vector in order to obtain more elongation in the hypoplastic ascending ramus.
Our distraction protocol includes a latency period of 4–5 days. Distraction commences at a rate of 1.0 mm/day (distraction period). This period is continued 4–6 weeks until we achieve the desired mandibular lengthening with the correction of the facial asymmetry, chin position, level of the oral commissure, and the changes in the dental occlusion. A very important point is to produce an overcorrection in the group of growing patients. In the preoperative period, the patients present a marked lateral deviation of the mandibular teeth to the affected side. After the distraction has been completed, the deviation of the mandibular interincisal line is reproduced in the opposite direction in the contralateral side as a result of overcorrection. Also, a posterior open bite and a crossbite are produced immediately after distraction; for these reasons, posterior bite blocks, dynamic appliances, and standard orthodontic maneuvers will easily control the occlusal changes and will produce some degree of dental occlusion stability. Bite blocks were required to maintain the posterior open bite; the blocks were gradually reduced to allow vertical descent of the maxillary dentoalveolus. We must always avoid the production of occlusal disasters as this situation will be impossible to correct later with standard orthodontic procedures.
The consolidation period is about 8 weeks or more. It depends on the age of the patient as well as the amount of bone lengthening. In an adult patient with a severe hypoplastic ramus, it can be prolonged for 16 weeks until there is radiographic evidence of mineralization. At this time, the device is removed under sedation.
Age is also a critical factor in the treatment of a hemifacial microsomia patient with mandibulardistraction. During the 1990s, the international criteria were to indicate the procedure at an age of 5–6 years, including the more severe cases. This decision was established according to the amount of mandibular bone stock and the feasibility of using intra- or extraoral distraction devices. Actually, we know that patients under 5 years of age, presenting a severe or moderate deformity, are not good candidates to elongate the mandible with intraoral devices. The procedure will result in a failure to achieve the ideal distraction vector, secondary occlusal disasters, and the need for future surgical interventions.
In our clinical series, aesthetic results were excellent. The facial symmetry was restored with descent of the buccal commissure to the level of the contralateral normal side; the menton became horizontal and was located at the midline (Fig. 29.4a–d). In all our patients, we noted an increase in the soft tissue envelope bulk. This simultaneous soft tissue expansion is the most important factor in obtaining the correction of facial asymmetry, and it is more observed during the consolidation period. At this time, the device serves as an external fixator, and the muscles of mastication produce contraction forces over the regenerate bone allowing the molding of the callus with the increase of the bigonial distance by the muscles’ pull.
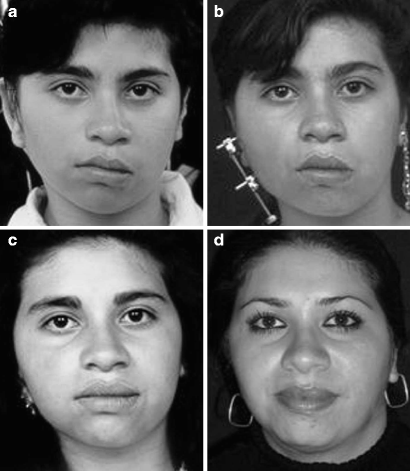

Fig. 29.4
(a) Preoperative frontal view of a 9-year-old girl with a Pruzansky II-A hemifacial microsomia showing facial asymmetry and chin deviation to the affected side. (b) During the distraction process, 2 weeks after the initial 16 mm of mandibular elongation showing an early improvement of the facial asymmetry. (c) Six months after 24 mm of mandibular distraction showing facial symmetry with descent of the buccal commissure and medialization of the chin. (d) The patient 12 years later showing stability in the clinical result. Facial symmetry: a chin position has been stable in the long-term result
Our clinical series also includes a group of patients with hypoplasia grade II-B treated between 18 months and 3 years of age. Undoubtedly this group of children has better craniofacial growth and long-term clinical stability in the soft tissues. After overcorrection, the use of dynamic orthodontic appliances and bite blocks corrected the occlusal changes and the vertical dimension of the maxilla. All of these changes occurred very fast and almost spontaneously during a period of 2–3 months, compared with children treated over age of 6 years. For this reason every day, more and more, we are indicating the procedure at early ages. It is also important to mention that permanent dental injury or neurovascular damage did not occur. Elongation was done by the parents with minimal discomfort during the night without disturbing the children’s sleep. These children represent the group of patients with the best results and better tolerance to the method.
Twelve percent of the patients with hypoplasia grades II-A and II-B treated after 6 years of age required a second distraction procedure. The main reasons for a secondary procedure were erroneous distraction vector, incomplete consolidation period, and nonsatisfactory overcorrection criteria. These patients presented an early tendency to retake the original condition of facial asymmetry and malocclusion as it was observed after 2–3 years of follow-up (Fig. 29.5a–i).
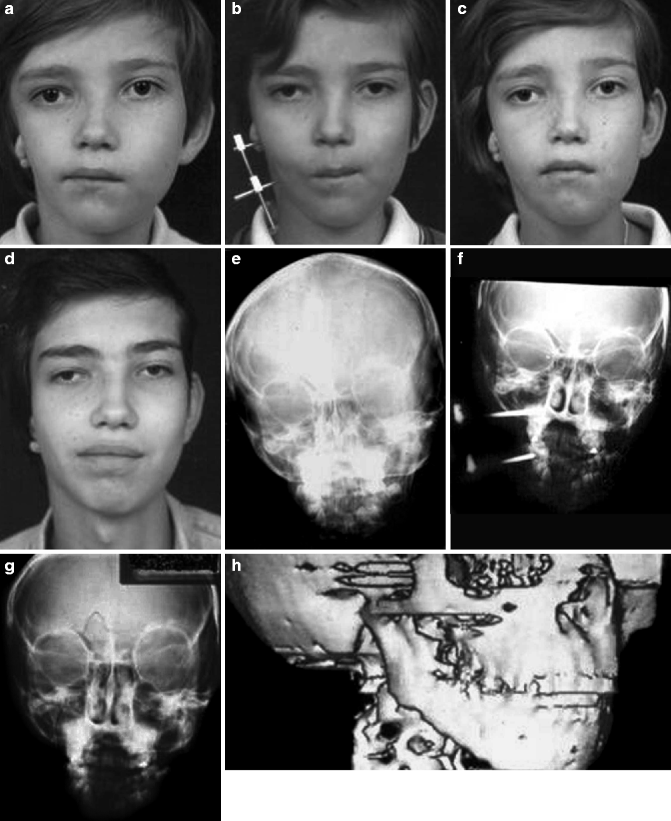
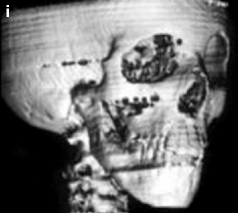


Fig. 29.5
(a) Preoperative frontal view of a 6-year-old boy with hemifacial microsomia Pruzansky II-A showing facial asymmetry with deviation of the buccal commissure and the chin. (b) During the distraction process. (c) The patient 6 months after showing facial symmetry. (d) Frontal view 10 years later. We can observe excellent growth of the mandible together with the rest of the craniofacial skeleton. (e) Preoperative PA cephalogram. (f) During the distraction process showing a low bone density area between the pins. (g) Postdistraction PA cephalogram. Notice the increase in the vertical dimension of the mandible, the condyle position, and the changes in the maxilla. (h) Preoperative CT scan showing the shortness of the ascending ramus (i) Postdistraction CT scan showing the increase of the ramus length as well as the new volumetric change of the gonion
If the patient is 12 years old or more at the time of the second bone elongation, we indicate a simultaneous maxillomandibular distraction. This technique is also indicated in the adult group of patients as a primary surgical procedure (Fig. 29.6a, b). Additional to the mandibular distraction, we include a subperiosteal dissection of the maxilla, and then a complete horizontal osteotomy is made at the level of the pyriform area in both sides. The pterygomaxillary junction is freed with a curved chisel and Rowe forceps on the affected side only. Rowe forceps may be used softly to assess the completeness of the osteotomy, but no attempt is made to mobilize the midface. The pterygomaxillary junction on the unaffected side remains intact, and it will serve as a pivot to safely produce the midface elongation-rotation movements on the affected side.
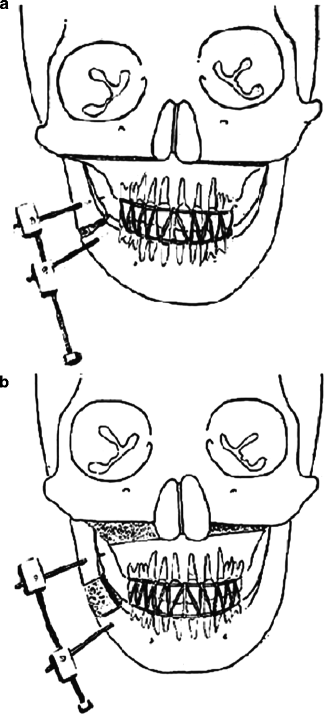

Fig. 29.6
(a) Diagram showing the mandibular corticotomy with the device in site. An additional horizontal osteotomy has been performed over the maxilla. After 5 days, an intermaxillary fixation is indicated with the aim of obtaining a simultaneous elongation of both bone structures. (b) Areas of new bone formation over the mandible and the maxillary
The result shows that with the mandibular elongation, the maxilla follows the mandible changes, achieving simultaneous elongation, medial rotation, and advancement. Preoperatively, the deviation of the occlusal plane from the horizontal varied from 12° to 18°, and after the combined distraction procedure, the clinical and orthodontic correction was obtained with a minimal slanting of 1–2° in the long-term follow-up.
Preoperatively, the vertical dimension of the maxilla was very short, and the last mandibular molar was in a very close relationship with the malar bone. Postoperatively, the vertical maxillary increases from 16 to 15 mm, representing a 90 % correction when compared with the unaffected side. All of this new bone formation results in a simultaneous correction of the oblique nasal floor, as well as the deviation of the nasal septum changing into the more normal position, increasing the volume of the nasal cavity. The preexisting dental occlusion has been preserved; after the elongation, the superior and inferior midline incisors have changed and now are positioned in the central line of the face (Fig. 29.7a–d).
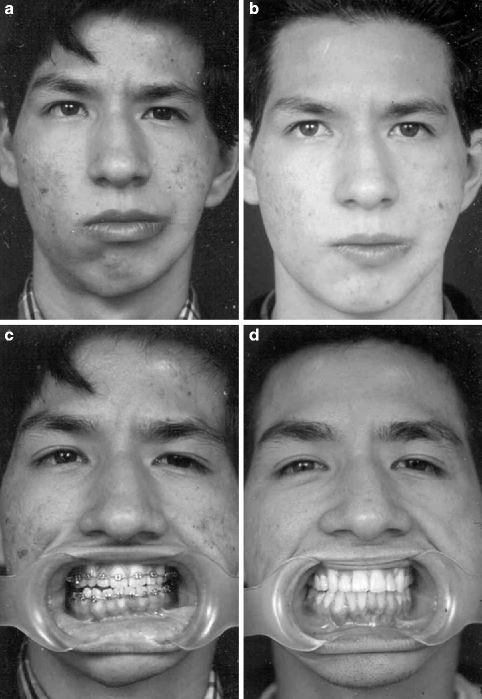

Fig. 29.7
(a) Preoperative frontal view of an adult patient with left hemifacial microsomia. (b) Six months postdistraction frontal view after a simultaneous maxillomandibular distraction. (c) The patient showing the operative occlusion. Notice the obliquity of the occlusal plane. (d) Six months after distraction, the patient shows its occlusion with the correction of the occlusal cant
The chin is always medialized by the distraction, but in adults it is not always possible to achieve a normal central position; for this reason, this procedure does not eliminate the need for a sliding genioplasty or another extrasurgical procedure, like a free dermis-fat graft, at the time of the removal of the device to improve the aesthetic final result.
29.1.2 Micrognathias
Patients with micrognathias present a different problem because of the bilateral deformity and because both the mandibular body and the ascending ramus are affected, requiring bidirectional and bilateral distraction. This concept is also true for patients with Pierre Robin, Nager, Treacher Collins, and bilateral hemifacial microsomia syndromes. In these cases, two corticotomies were done: a vertically oriented one in the mandibular body and a horizontally oriented one in the ascending ramus. The pins used are as follows: a central one is introduced at the mandibular angle between the two corticotomies, a second into the mandibular body, and a third into the central aspect of the ascending ramus. One bidirectional device is used on each side, each one with two distraction plates to allow independent and more precise elongation of each segment, using the central pin as the fixed pivot for both of them (Fig. 29.8a, b).
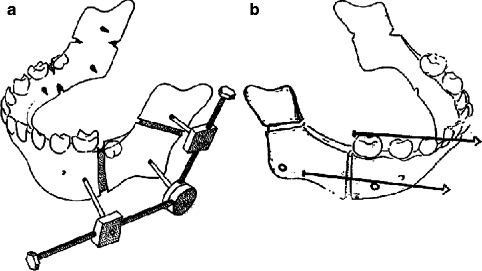

Fig. 29.8
(a) Diagram showing two corticotomies for bidirectional elongation. The central osteotomized bone fragment must be large enough to avoid fracture and back displacement. (b) The horizontal vector always has to be parallel to the occlusal plane in order to avoid the production of an anterior open bite or other occlusal disasters
Most of these patients present the typical “bird face” deformity with deficient soft tissue at the lower third of the face and at the neck, absence of the neck angle, and shortened suprahyoid muscles. With bone distraction, all the tissues from skeleton to skin are simultaneously elongated without the inconvenience of osteotomies or skin expansion (Fig. 29.9a–h). After conventional osteotomies and bone grafts, the muscles and the tight skin envelope present a limiting factor often requiring multiple procedures and seldom achieving optimal aesthetic results. Tissue expansion increases the size of the skin cover, but other soft tissues such as muscles, vessels, and nerves remain unchanged. The overall functional and aesthetic results with bidirectional mandibular distraction have been spectacular. The neck takes a normal shape with a well-defined angle. The muscles and soft tissues of the floor of the mouth together with the masticatory muscles got the expansion giving a better aspect of the neck. The chin takes a more prominent position.
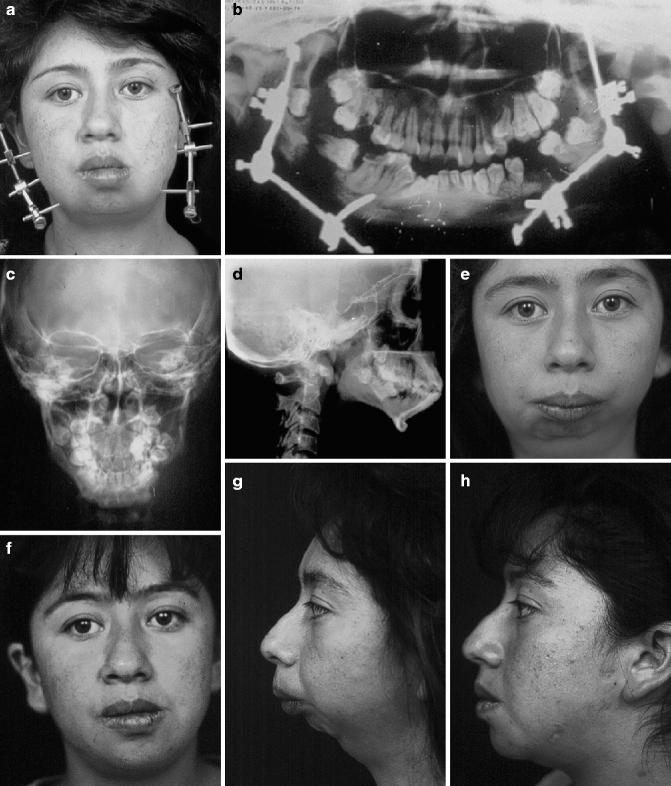

Fig. 29.9
(a) Frontal view of a 22-year-old girl during the distraction process of a bilateral and bidirectional mandibular elongation. (b) Panorex view showing the four independent vertical and horizontal distraction vectors. In asymmetrical micrognathias, one mandibular body can be elongated more than the contralateral in order to obtain symmetry. (c) Preoperative frontal view of the patient showing the asymmetrical micrognathia secondary to a condyle fracture during the early years of life. (d) Frontal view 3 years later of the mandibular distraction. Facial symmetry has been restored. (e) Preoperative lateral view showing the classic “bird face.” (f) Lateral view 3 years later showing the new mandible with a nice elongation of the soft tissues over the superior third of the neck. (g) PA cephalogram 3 years later showing a very well-defined mandibular structure. (h) Lateral cephalogram 3 years later. After mandibular elongation, the procedure has obtained a normal anatomy with an ascending ramus, gonion, mandibular body, and chin. The use of proper distraction vectors has achieved a normal occlusal relationship
29.1.3 The Temporomandibular Joint Ankylosis
Studies of the effect of mandibular distraction on the temporomandibular joint have shown that the condyle assumes a more normal anatomic size, shape, and position after distraction (McCormick et al. 1995). In fact, the process of distraction is beneficial to the condyle structure and its position in the glenoid fossae.
Regardless of the etiology of the joint ankylosis, it can be treated using the concept of bone transport and distraction to generate a neocondyle and to obtain a normal mandibular anatomy. In extra-articular ankylosis through a vestibular incision and subperiosteal dissection, an L-shaped osteotomy is made from the medial aspect of the projected condyle down to the posterior aspect of the ramus. Two pins are inserted, one in the osteotomized bone fragment and a second at the angle. The distraction vector is directed to the empty glenoid fossae (Fig. 29.10a, b). After a 5-day latency period, the osteotomized segment of bone is distracted and transported in a vertical direction until achieving the planned condyle lengthening. Usually 14–20 mm is enough to achieve a similar dimension with the contralateral side. Immediately the patients begin with open-close exercises, and during this activation period, the edge of the neocondyle is remodeled into a smooth, rounded surface. Fibrocartilaginous tissue at the leading edge of this segment acts as a pseudodisk.
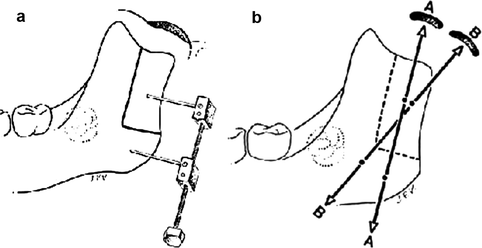

Fig. 29.10
(a) Diagram showing the “L osteotomy” over the ascending ramus with the device in place. (b) The distraction vector must be directed to the empty glenoid fossae
If the patients present an intra-articular ankylosis (true bony fusion), an arthroplasty is performed through a preauricular incision. The surgeon must release the bony fusion, and he will avoid bone resection reducing the ramus height. The abnormal bone is remodeled with a burr, and once this maneuver is completed, the opening of the mouth is accomplished with the assistance of a special forceps. Then a very fine Silastic layer (less 1.0 mm) is introduced as a cap on the top of the projected condyle and fixed to the surrounding scar tissue with two resolvable stitches. We close the incision, and then we change into the intraoral route for the L-shaped osteotomy.
This method produces a vertically elongated mandible with a functioning nonankylosing temporomandibular joint in the short term. The interincisal distance obtained ranged from 35 to 45 mm in the adult group. This technique will probably become the treatment of choice of temporomandibular joint ankylosis. Better diagnostic methods and understanding of etiology will be necessary in the near future to determine the efficacy of this process.
29.1.4 Cleft Lip and Palate Patients
The etiology of midface deficiency in cleft patients is uncertain. The absence of class III malocclusion in untreated clefts suggests that previous cheiloplasty and palate repair may be related to this condition (Ortiz-Monasterio et al. 1959). Ross (1987) in a longitudinal survey of 528 repaired cleft patients from 15 centers around the world demonstrated that approximately 25 % develop maxillary hypoplasia that did not respond to orthodontic procedures alone.
At the time of treatment, the ages of patients ranged between 6 and 12 years (mean 8 years), and all of them demonstrated clinical and radiographic evidence of moderate to severe underdevelopment of the maxilla (sagittal, vertical, and transverse). They also presented with a flattened middle third of the face and class III malocclusion, with partial or total anterior and posterior crossbite.
The severity of maxillary hypoplasia ranged from 2 to 10 mm of A-P discrepancy. Class III malocclusion with anterior and posterior crossbite, deep overbite, and in some patients, vertical skeletal open bite was observed.
Preoperative orthodontics are mandatory to obtain a minimal occlusal stability. The following orthodontic requirements were fulfilled prior to maxillary distraction: skeletal and/or dentoalveolar transverse expansion of the maxilla, alignment of permanent incisors in the cleft area in some patients, and bone grafting at 8–10 years old in other cases (Subtelny and Brodie 1954; Tindlund 1989, 1994).
Prior to surgery, a modified quad-helix fixed appliance was placed in the palate. This is made of a simple lingual arch attached to bands placed on the second deciduous molars. Anteriorly the arch maintains passive contact with the incisors through an acrylic button. In order to maintain maxillary expansion during the advancement, an extra transverse arch is fixed to both premolar bands which in turn provide the support for the vestibular hooks.
Under general anesthesia, two maxillary vestibular incisions 3–4 cm long are made, leaving a 2-cm central mucosal bridge between the incisions. Subperiosteal dissection is performed from the pyriform fossae to the lateral maxillary buttress on each side exposing the anterior and lateral aspects of the maxilla to the level of the infraorbital nerve and above the canine roots. Dissection on the nasal floor is limited to the lateral part only. The nasal septum and the maxillary cleft gap remain intact. Using a side-cutting burr, a horizontal osteotomy is performed above the roots of the canines and molar tooth buds as identified on the posteroanterior cephalogram and panorex.
Bilaterally, using a 7-mm chisel, the osteotomy is extended into the maxillary buttress, reaching the pterygomaxillary region. Disjunction with Rowe forceps is not performed, thereby avoiding unnecessary bleeding and uncontrolled fractures in the pterygomaxillary junction. At this time, the surgeon must assess maxillary mobility by applying gentle downward pressure to the Le Fort I segment. The mucosa is then approximated and closed with absorbable sutures. Following this minimally invasive technique, the hypoplastic maxilla is ready to be mobilized. As the nerve function and vascularity have been preserved, the mechanical distraction forces will stimulate the functional matrix to produce new bone formation.
Using the fixed intraoral appliance system as an anchorage for a modified “petit” facial mask supported by the forehead and chin, distraction forces are initiated on postoperative day 5. Two intraoral elastic bands on each side are linked from vestibular hooks to a bar on the mask. No other fixation is required. The initial mechanical force used for distraction is about 900 g. The facial mask is used mainly at night and at some periods during the day for a total of 16–18 h every day.
When the vertical length of the maxilla is deficient, a combination of forward and downward distraction forces can be used to simultaneously advance and lengthen the maxilla.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


